Page 17
1
Introduction
Nearly 1 million people each year report taking time away from work to treat and recover from musculoskeletal pain or loss of function due to overexertion or repetitive motion either in the low back or upper extremities (Bureau of Labor Statistics, 1999a).1 Although there is a risk of long-term disability in both types of disorder, the majority of individuals return to work within 31 days. Estimated workers' compensation costs associated with these lost workdays range from $13 to $20 billion annually. However, in order to determine the total economic burden, indirect costs related to such factors as lost wages, lost productivity, and lost tax revenues must be added to the cost of compensation claims, leading to estimates as high as $45 to $54 billion annually for musculoskeletal disorders reported as work-related. These figures are conservative and represent only reported cases. Several studies suggest that many disorders that could be attributed to work are not reported and therefore are not counted in any of the existing databases. According to Praemer, Furner, and Rice (1999), data collected in 1995 show that when nonoccupationally related disorders are included, the economic burden is as high as $215 billion.
Given the national dimensions of the problem and the diverse positions of interested parties—including medical and public health professionals, behavioral researchers, ergonomists, large and small businesses, labor, and government agencies—on the strength of the evidence regarding causation, Congress requested a study of the scientific literature on the causation, diagnosis, and prevention of musculoskeletal disorders.
1The median number of days away from work for overexertion is 7; for repetitive motion, it is 18.
Page 18
CHARGE TO THE PANEL
The Panel on Musculoskeletal Disorders and the Workplace was established by the National Research Council (NRC) and the Institute of Medicine (IOM) in January 1999, to conduct a two-year study of the contribution of workplace physical and psychosocial factors to the occurrence of musculoskeletal disorders of the low back and upper extremities and to examine the effectiveness of various prevention strategies. The panel is composed of 19 experts representing the fields of biomechanics, epidemiology, hand surgery, human factors engineering, internal medicine, nursing, occupational medicine, orthopedics, physical medicine and rehabilitation, physiology, psychology, quantitative analysis, and rheumatology. The impetus for the study was a request from Congress to examine the causation, diagnosis, and prevention of musculoskeletal disorders (House Report 105-635). The congressional request was presented in the form of seven questions (see Box 1.1). The charge to the panel, prepared by the NRC and the IOM, was designed to provide a comprehensive review of the science base and to address the issues outlined in the congressional questions. The tasks specified in the charge are:
-
Assess the state of the medical and biomechanical literature
BOX 1.1 Seven Questions Posed by Congress House Report 105-6351. What are the conditions affecting humans that are considered to be work-related musculoskeletal disorders? 2. What is the status of medical science with respect to the diagnosis and classification of such conditions? 3. What is the state of scientific knowledge, characterized by the degree of certainty or lack thereof, with regard to occupational and non-occupational activities causing such conditions? 4. What is the relative contribution of any causal factors identified in the literature to the development of such conditions in (a) the general population; (b) specific industries; and (c) specific occupational groups? 5. What is the incidence of such conditions in (a) the general population; (b) specific industries; and (c) specific occupational groups? 6. Does the literature reveal any specific guidance to prevent the development of such conditions in (a) the general population; (b) specific industries; and (c) specific occupational groups? 7. What scientific questions remain unanswered, and may require further research, to determine which occupational activities in which specific industries cause or contribute to work-related musculoskeletal disorders? |
Page 19
-
Evaluate the state of the medical and behavioral science literature on the character of jobs and job tasks, the conditions surrounding task performance, and the interactions of person, job, and organizational factors and, in addition, examine the research literature on the individual and nonwork-related activities that can contribute to or help prevent or remediate musculoskeletal disorders.
-
Assess the strengths and weaknesses of core datasets that form the basis for examining the incidence and epidemiology of musculoskeletal disorders reported in the workplace.
-
Examine knowledge concerning programs and practices associated with primary, secondary, and tertiary prevention of musculoskeletal injuries, ranging from organization-wide promotion of a safety culture to modified work and a variety of clinical treatment programs.
-
Characterize the future of work, how the workforce and jobs are changing and the potential impact of these changes on the incidence of musculoskeletal disorders.
-
Identify the most important gaps in the science base and recommend needed research.
describing the models and mechanisms characterizing the load-response relationships and the consequences (adaptation, impairment, disability) for musculoskeletal structures of the neck, the upper extremities, and the low back.
The disorders of particular interest to the panel, in light of its charge, focus on the low back and the upper extremities. Some of these are clinically clear-cut, others less so. With regard to the upper extremities, these include rotator cuff injuries (lateral and medial), epicondylitis, carpal tunnel syndrome, tendinitis, tenosynovitis of the hand and wrist (including DeQuervain's stenosing tenosynovitis, trigger finger, and others), and a variety of nonspecific wrist complaints, syndromes, and regional discomforts lacking clinical specificity. With regard to the low back, there are many disabling syndromes that occur in the absence of defined radiographic abnormalities, or commonly occur in the presence of unrelated radiographic abnormalities. Thus, the most common syndrome is non-specific backache. Other disorders of interest include back pain and sciatica due to displacement and degeneration of lumbar intervertebral discs with radiculopathy, spondylolysis, spondylolisthesis, and spinal
stenosis2—
2Radiculopathy is a disease of the roots of the spinal nerves. Spondylosis is a defect in the spinal arch—the part of the vertebrae that lies behind the nerves and the spinal cord. Spondylolisthesis is the slippage of a vertebra on the vertebra below. Spinal stenosis is a narrowing of the spinal canal, usually due to osteoarthritis and sometimes with pressure on the nerve root.
Page 20
International Classification of Disease (ICD-9) categories 353-357, 722-724, and 726-729.
Estimates of the frequency of these disorders may be gleaned from the fact that Americans make some 70 million physician office visits annually for musculoskeletal disorders. Of these, nearly 20 million are for back complaints and 2.7 million are for complaints related to the wrist. Comparative estimates of the incidence of these disorders in the non-working general population are not available, since more than 80 percent of American adults are in the workforce. In addition, low back pain is a common complaint and mechanical stressors are not confined to the workplace. Defining the proportion of musculoskeletal disorders due to workplace injuries is therefore a complex undertaking.
BACKGROUND
In the workplace, the multiplicity of factors that may affect reported cases—including work procedures, equipment, and environment; organizational and social factors; physical and psychological characteristics of the individual; and workplace reporting practices—has led to an ongoing debate about causes, nature, severity, and degrees of work-relatedness.3 In response, the National Institute for Occupational Safety and Health published an extensive review of the literature describing the epidemiology of musculoskeletal disorders of the back and upper extremities (Bernard, 1997b). This review focused on the results of research projects designed to examine the causal link between physical activities in the workplace and musculoskeletal disorders; in addition, one section was devoted to the assessment of the research on psychosocial factors, such as workload, social support, job control, and activities outside the workplace. The authors reported strong evidence for the combined effects of repetitive motion, force, and posture on elbow and hand/wrist disorders as causative factors, although the evidence was weaker for each factor individually.
3Work-related illnesses or diseases may be caused by, aggravated, accelerated, or exacerbated by workplace exposures, and they may impair working capacity. Personal characteristics and other environmental and sociocultural factors usually play a role as ri work-related illnesses and diseases. These are more common than occupational diseases, which are at one end of the work-relatedness spectrum, whereby the relationship to specific causal factors at work has been fully established and the factors concerned can be identified, measured, and eventually controlled. At the other end of the spectrum are diseases with a weak, inconsistent, unclear relationship to working conditions, although the strength and magnitude of the relationship may vary. This definition also includes conditions that are not caused by work but are aggravated by it (World Health Organization, 1985).
Page 21
In summer 1998, the National Academy of Sciences/National Research Council convened a workshop to review the scientific literature regarding the effects of a wide range of potential contributing factors and their interactions. The report of the workshop's organizing committee found that although the strength of the evidence varied, some broad conclusions could be drawn (National Research Council, 1999b:27):
-
“There is a higher incidence of reported pain, injury, loss of work, and disability among individuals who are employed in occupations where there is a high level of exposure to physical loading than for those employed in occupations with lower levels of exposure.
-
There is a strong biological plausibility to the relationship between the incidence of musculoskeletal disorders and the causative exposure factors in high-exposure occupational settings.
-
Research clearly demonstrates that specific interventions can reduce the rate of reported musculoskeletal disorders for workers who perform high-risk tasks. No known single intervention is universally effective. Successful interventions require attention to individual, organizational, and job characteristics, tailoring the corrective actions to those characteristics.”
Other researchers have developed different interpretations of the available data. These researchers contend that there is insufficient evidence to establish a causal relationship between workplace activities and the occurrence of musculoskeletal disorders (see, for example, Hadler, in press; Nathan et al., 1992). Their argument hinges on the proposition that the methodology for most studies is inadequate and thus uncertain results are obtained. The panel shares the view that sound conclusions must be based on valid data, and accordingly developed rigorous criteria for the inclusion of studies in the present effort. These criteria are detailed later in this chapter.
APPROACH TO THE PROBLEM
In responding to its charge, the panel conducted a comprehensive review of the scientific literature describing the biological responses to load on tissue; biomechanical models of static, dynamic, and repetitive motion and the effects of various forces and loads on the body; the relationships among the occurrence of musculoskeletal disorders and physical work, social and organizational factors, activities outside the workplace, and individual differences; changes in the workplace or the addition of workplace programs designed to reduce the risks for the occurrence of musculoskeletal disorders; and trends in workplace charac-
Page 22
teristics and their implications for musculoskeletal disorders in the future.
Several screening criteria were used by the panel in selecting the research literature for review. Criteria that applied to all areas included:
1. Focused on low back and upper extremity musculoskeletal disorders
2. Conducted within the last 20 years
3. Published in peer-reviewed publications
4. Published in English
Because the scientific literature has various purposes; includes both empirical and theoretical approaches; and covers a wide variety of research designs, measurement instruments, and methods of analysis, the selection criteria necessarily varied among disciplines. Reviews in tissue mechanobiology and biomechanics were further limited to controlled studies measuring physical and physiological responses using cadavers, animal models, and human subjects. The review of the biomechanical literature focused on studies that assessed the basic load-tolerance construct, had quantifiable exposure metrics, had outcome measures that were quantifiable on a continuous measurement scale, did not rely solely on self-reports, and were designed as prospective, case-controlled, or randomized controlled trial studies. The criteria used in screening literature for the epidemiology review were: a participation rate of 70 percent or more, well-defined exposure and referent populations, and well-defined criteria for measuring health outcomes determined before the study. Finally, the review of the intervention literature was restricted to studies with control groups that examined the effects of primary and secondary interventions in the workplace. The intervention review was supplemented by an evaluation of reports from industry describing best practices in the workplace.
As part of its information gathering activities, the panel commissioned 12 literature reviews including: (1) five on biological responses to load on nerves, tendons, ligaments, muscle, and bone; (2) two on the biomechanics of the back and upper extremities; (3) four on epidemiologic research on the contribution of physical and psychosocial factors to musculoskeletal disorders of the back and upper extremities; and (4) one on economic and cultural context factors that influence the reporting and duration of these disorders. In addition, the panel was given the opportunity to observe work performed at two Ford Motor Company automobile plants and to hold discussions with union representatives, plant managers, and members of ergonomics teams. The panel also heard a presentation describing the Bureau of Labor Statistics database on musculoskeletal dis-
Page 23
orders and others outlining the experiences of various industries with these disorders, including trends in reported cases and the effectiveness of various intervention strategies. Finally, the panel held an open forum in which representatives from orthopedics, occupational medicine, industry, and labor offered their views on the weight of the scientific evidence. The information gathered in the site visit to Ford Motor Company and in the presentations enriched the panel's discussions of workplace activities and the effectiveness of various intervention strategies in selected work environments.
THE WHOLE PERSON: INJURY, ILLNESS, AND DISEASE
We begin the discussion with some basic concepts that guided the panel's analysis of the scientific literature. These include the concept of physical injury, including the response of the whole person and the challenges of diagnosis based on symptoms (e.g., pain), objective, measurable biological change, or both.
In the most immediate sense, injury is a biological event representing the impact of an environmental alteration on the individual. Such alterations are of numerous types and intensities and may range from invasion by biological agents, such as viruses or bacteria, through exposure to toxic substances or various forms of radiant energy, to physical forces, including those capable of damaging musculoskeletal structures. The extent of physical injury after such exposure varies widely depending on the intensity of the adverse event, the duration of exposure to it, and the characteristics of the injured individual.
Just as there is wide variability in the nature of the inciting event, there is wide variability among individuals in response to pain and functional limitation, including a variety of individual coping mechanisms, the effectiveness, extent, and adequacy of personal support systems at home and at work, and the individual's broader adjustment to the work context. These factors mean that injury is a psychosocial event as well as a biological or physical one. In addition, physical activities outside the workplace, including, for example, those deriving from domestic responsibilities in the home, physical fitness programs, and others are also capable on one hand of inducing musculoskeletal injury and on the other of affecting the course of such injuries incurred at the workplace. Because injury and its impact on the individual are inextricably bound, the panel approached its charge by considering the context of the whole person as the injured and reacting entity, rather than focusing on the low back or upper extremities in isolation.
Among individuals who have the same level of physiological impairment, there is wide variation with regard to symptom intensity, associ-
Page 24
ated interference with activity, and contributing and comorbid factors in the individual's health status and in the wider social context of his or her life. Important diagnostic issues are involved in workplace injuries, just as they are in most situations in which individuals look to physicians or others in the health care system for diagnosis and management of symptoms. Furthermore, in the case of many clinical disorders, it is common for complete and unambiguous objective support of the diagnostic formulation to be lacking. Thus, clinicians are accustomed to the concept of diagnostic thresholds; that is, acceptable levels of evidence on the basis of which treatment and other management decisions are made. Such evidence may include the extent to which the patient's symptoms are characteristic of the disorder under consideration, the degree to which the findings on physical examination are consonant with it, the presence of predisposing factors and precipitating events sufficient to lend support to the diagnosis, and the level of confirmation available from objective studies, such as laboratory tests, electrocardiograms, and X-rays. Assessments lacking such objective medical evidence can sometimes achieve high degrees of diagnostic reliability, as is the case in some pain syndromes in other areas, for example, classic migraine headache, angina pectoris, and premenstrual syndrome, although in may instances presenting syndromes are less specific.
Several studies of varying design (chart review, clinic questionnaire, community surveys) have examined how often patients with common physical complaints have symptoms only, in the absence of correlated measurable change (Kroenke and Mangelsdorff, 1989; Kroenke and Price, 1993; Kroenke et al., 1994; Marple et al., 1997; Kahn, Kahn, and Kroenke, 2000). It appears that at least one of every three patients who present with physical complaints in the primary care setting fall into this category, regardless of the specific symptoms or complaints. In these studies, the proportion of individuals with back pain who had symptoms only ranged from 16 to 90 percent. The widely ranging estimates arise from substantial differences in study methodology. Those studies relying on retrospective review of medical records (Kroenke and Mangelsdorff, 1989; Khan et al., 2000) for back pain diagnosis only yielded higher estimates (70 to 90 percent), while those using directed inquiry of physicians (Kroenke et al., 1994; Marple et al., 1997) provided lower estimates (16 to 30 percent). These data do not mean that such symptoms are trivial, but rather that patients presenting for care frequently experience symptomatic illness in the absence of abnormalities on physical examination and available diagnostic tests. The predominance of a symptom-only diagnosis is not restricted to musculoskeletal disorders but has been demonstrated also for other symptoms, including chest pain and abdominal pain (Wasson, Sox, and Sox, 1981; Martina et al., 1997).
Page 25
These factors point to an important distinction that obtains widely throughout clinical medicine: the distinction between illness and disease or, framed in an alternative manner, the distinction between the experience of being ill or sick (symptoms, other discomforts, dysfunctionality, fear, and social impacts) on the one hand, and disease, a biological event characterized usually but not invariably by definable and objective change (for example, abnormalities in X-rays, blood tests, or on examination of the heart) on the other. Disease and illness are usually present together and in related fashion, but this is not inevitably the case. Thus, it is possible to be ill in the absence of objective change (migraine headache is a good example), and it is possible to have objective disease without being ill (for example, a small lung tumor evident on a chest X-ray that has not yet produced any symptoms). The important derivative of these considerations for the purposes of the deliberations of the panel is that symptomatic injury of the low back or upper extremity may or may not be accompanied by definitive objective change, for example, on X-ray examinations, and, conversely, abnormalities of a variety of types may be found on X-rays or other studies that do not bear on and have no relation to the symptoms with which the patient may be presenting to the care system. Clinical judgment, that is, the weighing of all of the evidence by the physician, is thus an important factor in arriving at a diagnostic conclusion.
Not infrequently, pain syndromes related to the low back or upper extremities do not satisfy rigorous diagnostic criteria for well-defined clinical entities. Thus, most instances of acute or chronic low back pain are not accompanied by classical radiation of the pain in the distribution of the sciatic nerve, a syndrome that usually indicates herniation of a lumbar intervertebral disc with impingement on nerve roots. In such instances, the poor fit of the symptom pattern in the particular patient with diagnostic criteria for well-defined disorders is not an indication that the patient's symptoms are trivial or unrelated to identifiable risk factors. Indeed, the lack of such a fit with clearly defined disorders is more often the case than not.
Pain is the most common symptom for which patients see physicians, and chronic pain is a particularly difficult problem in clinical management. Pain can have no precise definition because only the suffering individual perceives it. Pain receptors are widely distributed in the tissues of the body and appear to be stimulated either by strong mechanical deformation, by extremes of hot or cold, or by various chemical substances liberated by inflammation or other processes. Pain is transmitted through peripheral nerves to the spinal cord and to the brain. Various responses are elicited, through a variety of neural connections involving the spinal cord as well as descending pathways from the brain. Some of these are reflex in nature and others involve complex reactions that vary widely
Page 26
from individual to individual, based on pain intensity, the implications of the pain to the individual, the extent to which the pain interferes with physical or social function, and many other factors. ( Chapter 5 contains a more detailed discussion.)
Somatization is a clinical phenomenon that requires consideration in the context of understanding the perception of pain. It is generally defined as the experiencing and reporting of bodily symptoms lacking a plausible physical explanation and the attribution by the symptomatic individual of such symptoms to disease. Medical attention is frequently sought for such symptoms. Somatization must be distinguished from malingering. Malingering is the intentional production of false or grossly exaggerated physical or psychological symptoms prompted by a conscious desire to obtain tangible external rewards. Somatization, which is both unintentional and involuntary, shares neither of these characteristics (Sadock and Sadock, 1999).
Medically explained symptoms that occur in somatizing patients can sometimes persist for long periods of time. Cognitive processes (e.g., increased attention to normal bodily sensations or excessive worry about a serious cause) as well as psychological factors both contribute to somatization. Among the psychological factors, depression and anxiety are particularly important influences in the experience of pain related to Somatization. These factors are present in 30 to 60 percent of somatized patients (Kroenke et al., 1994, 1997; Simon et al., 1996). Both pharmacological and nonpharmacological treatments may lead to symptom reduction in somatizing patients (O'Malley et al., 1999; Kroenke and Swindle, 2000). A small subset of somatizing individuals have a history of chronic multiple, unexplained symptoms and are classified as having a somatoform disorder. Early recognition of the role Somatization may play in some patients with musculoskeletal disorders or other persistent symptoms is essential to avoid excessive diagnostic testing as well as inappropriate medical and surgical interventions. The evaluation and management of Somatization are reviewed by Barsky and Borus (1995, 1999).
A particular challenge in the treatment of musculoskeletal disorders in the worker in whom Somatization is a causative or aggravating factor is the potential stigma related to experiencing or reporting a concomitant psychological problem, such as depression or anxiety. Such stigmatization may preclude access to appropriate management of the psychological distress that accompanies these problems. Although denial of requests for behavioral health evaluations may be based on claims adjusters' fears of adding a secondary “mental claim” to a primary “physical claim,” related to a belief among claims adjusters that such an addition drives up the cost of the claim significantly, an analysis of detailed medical costs for back pain by private workers' compensation carriers indicates that psy-
Page 27
chiatric or psychological care accounts for a very small percentage of health care costs, despite the high prevalence of idiopathic low back pain and co-occurrence of anxiety and depression in this diagnostic group. Only 0.4 percent of the cost of the care delivered for low back pain was allocated to psychiatric or psychological evaluation and treatment in one study (Williams et al., 1998). A similarly low percentage of health care costs was allocated to behavioral health services in a large group of federal workers diagnosed with carpal tunnel syndrome or tendinitis of the elbow managed within the federal workers' compensation system (Feuerstein et al., 1998).
Workplace and individual psychosocial factors can interact with ergonomic factors to affect clinical and functional outcomes even in those workers not receiving workers' compensation and actively working with pain. The practical implication is the importance of early evaluation of injured workers to determine if there are psychosocial issues that might influence the outcome. If such problems are detected, intervention should be aggressively targeted at these areas early.
LEVELS OF ANALYSIS: INDIVIDUALS AND POPULATIONS
Analysis of musculoskeletal disorders and the workplace must take place on two levels. The first of these addresses the individual, and the second addresses populations at risk in the aggregate. Individual considerations in workplace injury include elements of individual exposure to risk, the characteristics of the injuring event, the responses of the individual to the injury, diagnostic issues, and case management, including both clinical and nonclinical aspects. Aggregate or population approaches to workplace injury allow the accumulation of epidemiologic information, which in turn permits the analysis of patterns of injury, patterns of responses, and the design of potential preventive measures. There is a broad scientific literature in each of these areas—that is, at the level of both the individual and the population at risk—and the panel has analyzed both in the process of its examination of the evidence bearing on workplace injury.
Analysis at the aggregate level provides a useful structure for considering a wide range of strategies for reducing the risk factors for the occurrence of musculoskeletal disorders. One intervention strategy, for example, might be redesigning elements of the physical workplace; others might be creating a more supportive organizational culture or introducing an exercise program for strengthening workers both physically and psychologically. In introducing any intervention strategy, it is important to take into account the whole person and his or her interactions with the environment. Hence, many of those working in this area have used
Page 28
multifactorial approaches based on programs that include, for example, changes in workplace design, exercise regimens, training in pain control techniques, and efforts to affect other aspects of the workplace environment, such as equipment design.
Modifications of workplace infrastructure are intended to be enduring and appropriate for a population of workers. Although the potential effects of workplace activities on the body occur in workers as individuals, employer remedies and preventive strategies are more logically and economically directed toward a workplace system in which the aggregation of workers is characterized by a range of human physical and psychological features. The goal is to create workplace conditions that are robust to changes in the workforce over time and adaptable to changes in the nature of the work being performed.
CONTEXTUAL FACTORS
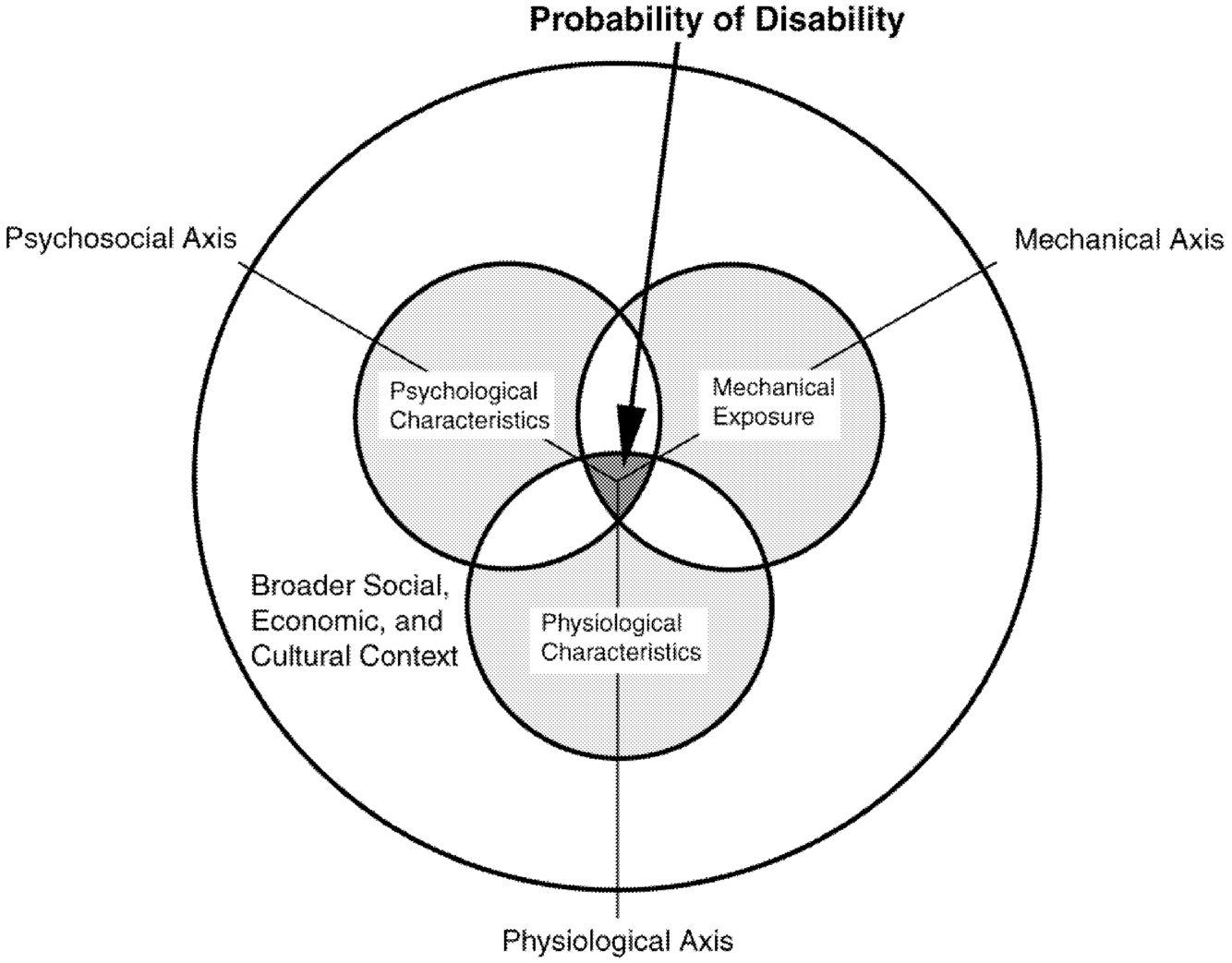
Figure 1.1 provides an overview of the risk factors for injury, impairment, and disability attributed to musculoskeletal disorders in the individual. It shows that the association between physical exposure and the development of a musculoskeletal disorder occurs in a broad context of economic and cultural factors and reflects the interaction of elements intrinsic to, as well as extrinsic to, the individual. Most research on musculoskeletal disorders in the workplace has focused on physical exposures and psychosocial factors, and indeed these factors are treated in greatest detail in this report. Here we briefly discuss the potential impact of economic incentives, workplace organizational policies, and research, because in our view these are important to any interpretation of the basic scientific data on the relationship between exposure and rates of worker disability. In this regard, there is convincing evidence to support the hypothesis that compensation wage replacement rates, local unemployment rates, and cultural differences can influence the reporting of musculoskeletal pain or disability—even though assessment of the direction and magnitude of these factors is quite complex.
Disability Benefits
Virtually every study that addresses workers' compensation disability benefits shows that the nature of these benefits has a significant effect on the timing of return to work after a work-related injury. The probability of return to work decreases and duration of work absence increases as benefit levels increase (Loeser, Henderlite, and Conrad, 1995). The causal direction of the reimbursement effect, however, may not always be clear. While higher reimbursement rates may indeed prompt some workers
Page 29
~ enlarge ~
who would otherwise return to work to remain absent longer, lower rates may prompt others to return to work too early, while still symptomatic, and with significant functional limitations. Separate from benefits, an association between attorney representation and the frequency and duration of claims has been documented. This linkage has prompted policy recommendations to remove disincentives to return to work (Johnson, Baldwin, and Butler, 1998). The direction of this “attorney effect,” however, is difficult to establish. It is not obvious that representation by an attorney is the cause of a claim's being filed or prolonged. For example, patients with the most severe functional limitations are most likely to seek assistance from attorneys. It may also be that the legal proceedings prolong the period until a claim is settled and the worker returns to work.
Page 30
Organizational Policies and Practices
The rise of direct and indirect costs of work-associated injuries during the 1980s prompted employers and researchers to examine the ways in which workplace policies and practices may influence work disability. Hunt and Habeck (1993) studied the role of organizational policies and practices on the frequency and duration of worker disability among employees of 220 companies in Michigan in 1991. Firms that reported maintaining safe equipment, investigating risks and accidents promptly, enforcing safety policies, and emphasizing safety in all aspects of operations had fewer lost workdays. Firms that reported active involvement of the injured worker and supervisor in the return-to-work process, creative strategies to accommodate injured workers, and cooperation and coordination of workers also had fewer lost workdays and fewer claims.
Shannon and colleagues (1996) surveyed employers and workers at 435 manufacturing workplaces across six industries in Ontario. Several factors were associated with lower rates of lost-time injuries, including greater experience (seniority) of the workforce, greater involvement of the workers in decision making, and greater commitment of the company to workers' career development. Profitability and unionization were not associated with lost-time frequency rates in this study, nor were the structure or functioning of the joint health and safety committees. Union membership has been shown to delay return to work in the United States but not in Canada, perhaps because in the United States unions often provide workers with attorneys and legal representation, which may prolong work absence (Johnson, Baldwin, and Butler, 1998; Baldwin, 2000).
There is consistent evidence that providing injured employees with modified work (typically modified tasks and schedules) increases the rate of successful return to work twofold and reduces the length of work absence following injury by half (Krause, Dasinger, and Neuhauser, 1998). Furthermore, the employer's attitude toward injured workers may have important effects on return to work (Strunin and Boden, 2000).
These findings indicate that organizational policies and practices in the workplace influence rates of worker disability. In particular, companies that make a greater commitment to worker health, safety, involvement in decision making, and availability of modified work appear to have lower rates of lost-time injuries. Of note is the observation that structural elements such as health and safety committees appear not to lead to lower lost-time rates unless they are coupled with a commitment to worker well-being.
Page 31
Culture
There is also some evidence that cultural factors influence reporting. Although this literature is difficult to interpret due to the elusive definition of such factors, there is work on low back pain and whiplash injury suggesting that cultural differences may affect musculoskeletal epidemiology. Specifically, Westernization, industrialization, and social security systems may be associated with a greater willingness of workers to report low back pain (Volinn, 1997). With regard to whiplash injury, investigators have speculated that insurance for personal injury drives rates upward in some countries and the lack of insurance depresses rates in others (Obelieniene et al., 1999; Partheni et al., 1999). The conversion in Saskatchewan from tort-based compensation, including payments for pain and suffering, to a no-fault system that did not provide such payments was accompanied by substantial decreases in the incidence of claims (Cassidy et al., 2000). The effect of the change in compensation system on whiplash symptoms was not evaluated in this study.
MECHANICAL, PHYSIOLOGICAL, AND PSYCHOLOGICAL FACTORS
Every clinical disorder represents a complex interaction between the affected individual and a variety of determinants of the response of the particular individual to injury. Thus, the “dose” of the injuring agent or circumstance may vary widely from person to person, interacting with relevant characteristics of the individual that determine vulnerability or resistance. In addition, symptoms, disease, injury, and disability have varying meaning among individuals, reflecting a wide array of psychological and social responses. The spheres in Figure 1.1 represent individual risk factors for musculoskeletal disorders and their potential interaction with mechanical stressors—one sphere contains the mix of the individual's psychological characteristics, such as coping strategies, and his or her social context; the second includes physiological characteristics of the individual, including tissue response to load, age, and the presence of medical comorbidities; and the third includes mechanical exposures, such as physical job demands resulting in external loading. The importance of each sphere, and hence its contribution to the risk of disorder, varies among individuals and work environments. At the center, the three spheres overlap to define a region of risk for disorder, emphasizing the principle that the risk is multifactorial and reflects the varying contribution of each set of factors. In addition to their specific contributions, the extent to which the spheres interact is influenced by social, medical, orga-
Page 32
nizational, and other factors, and the probability of disorder varies accordingly.
The psychological characteristics sphere represents the nature of the individual's psychological response to extrinsic stressors, largely reflecting social context and its implications for the individual. The relative importance of this sphere is determined by such psychological characteristics as attitudes, values, and a variety of coping mechanisms. The psychosocial axis represents the psychosocial factors to which the individual is exposed.
The physiological characteristics sphere represents the individual's biology/physiology: the structure and function of the body. This sphere reflects how individual physical factors contribute to risk of disability. These factors include age, body mass index, gender, and general physical condition, including the presence of comorbidities. Medical interventions, such as clinical treatments and surgery, can influence the individual's physical state and thus the position of the physiological sphere along the physiological axis.
The mechanical exposure sphere represents factors associated with physical load arising in the environment—physical work procedures and equipment as well as physical activity outside the workplace. Physical work procedures include activities such as lifting, reaching, bending, twisting, and repetitive motion, all of which affect the physical load experienced by body tissues. Examples of relevant physical activities outside the workplace include exercise regimens, sports, and lifting and bending in the course of household or other daily activities. Many of these activities of daily living may involve physical stresses similar to those present in the workplace. The mechanical axis implies variation of work and organizational factors that may contribute to risk. For example, putting time pressure on the worker may result in poor execution of prescribed procedures and lack of attention to safety considerations.
Interaction among physiological, psychological, and mechanical load levels is reflected in the figure by sphere overlap. The interplay of psychological characteristics and mechanical exposure represents the intersection between imposed physical load and the individual's psychological response to the workload. The overlap between psychological and physiological characteristics represents the interaction among tissue vulnerability to load, the experience of pain, and the effect of pain on the individual. Finally, the overlap between the physiological and mechanical spheres symbolizes the relationship between physical stressors and the response of body tissue. Figure 1.1 is intended to describe variation from person to person and in the individual over time, as well as the capacity of any of its subelements to diminish or expand. There is also a
Page 33
capacity implied for adaptation on the part of the individual, as well as for alteration in mechanical factors, social and cultural context, etc.
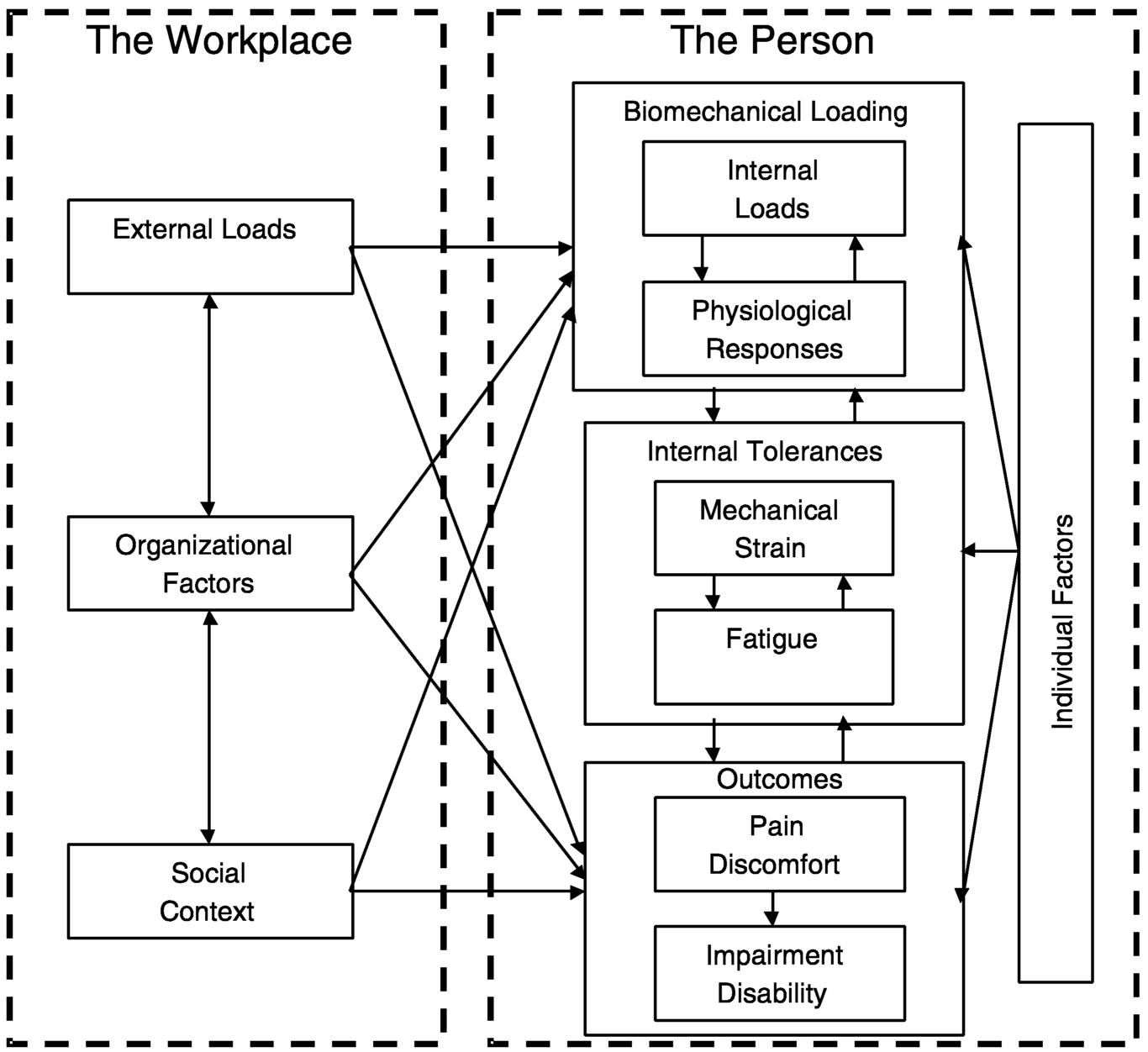
Figure 1.2 provides an elaboration of these factors and their interrelationships as a basis for the panel's review and analysis of the scientific literature. This figure is central to the panel's assessment, and provides a framework for organizing and structuring the research reviewed in this volume. Here the factors are organized into two broad categories: workplace factors and characteristics of the person that may affect the development of musculoskeletal disorders. Workplace factors include the external physical loads associated with job performance, as well as organizational factors, and social context variables. The person is identified as the central biological entity subject to biomechanical loading with the various physical, psychological, and social features associated with the individual that may influence the biological, clinical, and disability response. These individual factors are represented in the physiological and psychological spheres shown in Figure 1.1 and include age, gender, smoking habits, comorbidities, and perhaps genetically determined predispositions, as well as participation in physical activities away from the workplace (e.g., physical exercise, household work, etc.).
External loads resulting from work are transmitted through biomechanical forces of the limbs and trunk to create internal loads on the tissues and anatomical structures. Relevant biomechanical factors include body position, exertions, and motions. Biomechanical loading is also affected by individual factors such as anthropometry, strength, agility, dexterity, and other factors mediating the transmission of external loads to internal loads on anatomical structures. When the load exceeds mechanical tolerance or the ability of the structure to withstand the load, tissue damage occurs. The outcomes of pain, discomfort, impairment, and disability are the result of the interaction of the three categories of workplace factors portrayed and the physical and psychological characteristics of the individual.
Organizational and social context factors may affect the external demands of work and the individual's response to these demands. Organizational factors influence external loads in terms of the organization of tasks, work pace, characteristics of interpersonal interactions, and the utilization of ergonomic principles to modify tasks so as not to exceed the physical capacity of the worker. Social context factors may influence both organizational procedures and worker expectations and motivations. The impacts of the organizational and social factors on the individual are mediated through cognitive and perceptual mechanisms (represented by individual factors in Figure 1.2). These mechanisms vary from one individual to another; thus, the threshold at which external stimuli evoke psychological stress and mobilize coping mechanisms varies due to indi-
Page 34
~ enlarge ~
Page 35
vidual factors. Furthermore, responses to stress may affect the manifestations of musculoskeletal disorders by influencing pain perception and tolerance, altering cognitive function and behavior, and altering the physical and/or psychological state of readiness for the performance of physical tasks. The arrows between workplace factors, the individual factors and the biomechanical loading mechanism provide a roadmap for the panel's analysis of the relationships that have been examined in the scientific literature. This framework is used throughout the book to structure the presentation and assessment of the evidence. In addition, there are a number of key terms used throughout this volume that may be interpreted variously depending on the reader's orientation. Definitions of these terms as used in this report appear in Box 1.2.
GUIDE TO THE REPORT
Part I provides general introductory and contextual material. It includes the introduction (Chapter 1) and a chapter on the prevalence, incidence, and costs associated with musculoskeletal disorders and the economic and social factors that influence their reporting (Chapter 2). An overview of the methodological issues and approaches used in the research on musculoskeletal disorders is provided (Chapter 3).
Part II contains a review of the evidence. Presented are detailed descriptions of the evidence from epidemiologic studies of physical and psychosocial variables (Chapter 4), tissue mechanobiology (Chapter 5), biomechanics (Chapter 6), physical and behavioral responses to stress (Chapter 7), workplace interventions (Chapter 8), and general characteristics of the workplace now and in the future.
Part III presents an integration of the evidence and the panel's conclusions and recommendations, including suggestions for future research directions.
There are five appendixes. Appendix A presents the panel's response to congressional questions. Appendix B is the dissent statement by Robert Szabo. Appendix C is the panel's response to the dissent signed by the other 18 panel members. Appendix D lists the contributors to the report, and Appendix E contains the biographical sketches of panel members and staff.
Page 36
BOX 1.2 DefinitionsCompensability: Qualifying under the law for payment for medical expenses and/ or loss of earning capacity because of partial or total loss of function or capacity (impairment) as the result of an injury or illness. Disability: A social definition indicating inability or limitation in performing socially defined activities and roles expected of individuals within a social and physical environment. Examples are inability to perform a job or inability to swim recreationally (Institute of Medicine, 1997:6). Disease: An objective pathologic condition, involving interruption or interference with normal body structures or function (adapted from the definition of “pathology” in Institute of Medicine, 1997:5). Disorder: Is variously defined as an alteration in an individual's usual sense of wellness or ability to function. A disorder may or may not interfere with usual activities of daily living or work activities. A disorder may or may not be associated with well-recognized anatomic, physiologic, or psychiatric pathology. Exposure: Proximity or contact with a putative risk factor in such a manner that an injury, disease, or illness may occur (from Last, 1988). The concept carries with it the dose of the causative risk factor. Illness: A clinical definition indicating the subjective state of the person who feels aware of not being well (from M.W. Susser, cited in Last, 1988). This subjective experience may or may not be associated with objective signs of disease. Impairment: A functional definition indicating a loss and/or abnormality of mental, emotional, physiological, biomechanical, or anatomical structure or function. This includes, for example, losses or abnormalities due to pain and/or gait abnormality or at the extreme, invalidism, and may refer to organs and organ systems function or to the intact individual. (derived from Institute of Medicine, 1997:6). Injury: Any damage to the individual (anatomic, physiologic, or psychiatric) resulting from exposure to thermal, mechanical, electrical, or chemical energy or other stessors or from absence of such essentials as heat or oxygen (adapted from National Committee for Injury Prevention and Control, 1989). Outcome: All the possible results that may stem from exposure to a causal factor or from preventive or therapeutic interventions: all identified changes in health status arising as a consequence of the management of a health problem. (from Last, 1988). Work: The act of expending human labor or effort, usually for financial remuneration, to create a product or to produce goods or services. The expenditure of effort to create, transform, or process goods, services, or intellectual models. |
Page 37
BOX 1.2 Definitions
|





















