Chapter One
Introduction
In recent years, numerous reports have called attention to serious and widespread problems in the quality of health care provided to Americans. In 1998, a statement prepared for the National Roundtable on Health Care Quality asserts that many patients are harmed unnecessarily by the care they receive and that quality problems are not limited to any particular geographic area or type of health plan, whether managed care or fee-for-service (Chassin and Galvin, 1998). Likewise, a 1999 report of the IOM’s National Cancer Policy Board reveals that many individuals with cancer do not receive care known to be effective for their conditions (Institute of Medicine, 1999). A subsequent report by the IOM’s Committee on the Quality of Health Care in America, To Err Is Human: Building a Safer Health System, focused national attention on problems in patient safety and the need to design safer care processes and systems (Institute of Medicine, 2000).
The IOM is not alone in calling attention to health care safety and quality concerns. Almost 30 years ago, geographic variations in the delivery of health care were observed (Wennberg and Gittelsohn, 1973) and these variations persist today (Chassin et al., 1987; O’Connor et al., 1999; Welch et al., 1993). In 1998, the President’s Advisory Commission on Consumer Protection and Quality in the Health Care Industry offered major recommendations for improving the quality of care for Americans. These recommendations included establishing public-private partnerships to provide national leadership in health care quality improvement, promoting the measurement and reporting of the quality of care delivered, and investing in information technology infrastructure to support decision making and the delivery of quality care (President’s Advisory Commission on Consumer Protection and Quality in the Health Care Industry, 1998). A literature review published by the RAND Corporation in 1998 also calls for routine, mandatory tracking and reporting on the quality of care delivered to the American people (Schuster et al., 1998). And the Commonwealth Fund’s newly released Quality of Health Care in the United States: A Chartbook confirms that large gaps
persist between the care patients should and actually do receive (Leatherman and McCarthy, 2002):
-
Poor treatment of diabetes result in tens of thousands of cases of premature death, limb amputation, kidney disease and blindness (American Diabetes Association, 2002; Centers for Disease Control and Prevention, 2002).
-
Inadequate care after a heart attack results in 18,000 unnecessary deaths per year (Chassin, 1997).
-
The average Medicare beneficiary having one or more chronic conditions is seen by eight different physicians during a year (Anderson and Knickman, 2001). Results of a recent survey indicate that approximately 20 million Americans with chronic illnesses received contradictory information from different health care providers, and 17 million reported being told by their pharmacist that the drugs they were prescribed could have interactions (Harris Interactive, 2001).
-
Fewer than half of adults aged 50 and over were found to have received recommended screening tests for colorectal cancer, the second most common cause of cancer death in the United States (Centers for Disease Control and Prevention, 2001; Leatherman and McCarthy, 2002).
The 2001 IOM report Crossing the Quality Chasm: A New Health System for the 21st Century sets forth an ambitious agenda for taking the first steps in redesigning how health care is routinely delivered (Institute of Medicine, 2001a). The report recommends focusing greater attention on the development of care processes for common chronic conditions. The rationale for this emphasis is that targeting those conditions that account for the majority of health care burden and expenditures and making real changes in the care delivery processes for those conditions would benefit a sizable portion of the population. Moreover, a focus on enhancing quality for a few well-selected priority conditions would be likely to generate systems, skills, awareness, and a culture that would foster improvements in other areas as well. In addition, since many conditions are treated in more than one health care setting, a focus on priority conditions might be expected to encompass care provided in physicians’ offices, hospitals, and nursing homes, as well as home care settings. The Quality Chasm report therefore recommends that the Agency for Healthcare Research and Quality (AHRQ) within the Department of Health and Human Services (DHHS) identify no fewer than 15 priority conditions that might serve as the starting point for transforming the delivery of health care (Institute of Medicine, 2001a).
In response, DHHS contracted with the IOM to convene a committee of experts that would establish a process and develop a set of criteria for determining the priority conditions, identify candidate conditions, and recommend to DHHS a final list of priority conditions deserving of immediate attention. The IOM established a committee with broad-based representation from the following areas: public health, prevention, medicine, nursing, chronic disease management, behavioral medicine, epidemiology, quality of care, health care delivery/policy, health economics, consumer groups, geriatrics, mental health, and special populations (see Appendix A for biographies of the committee members). This report presents the results of the committee’s efforts.
The next step will be to work with various stakeholders in the health care community to develop and implement strategies for improving the quality of care for each priority condition within the next 5 years. To encourage action by other stakeholders, DHSS intends to review the committee’s recommendations; select priorities; and begin incorporating them into the National Health Care Quality Report, to be released for the first time in 2003 (Institute of Medicine, 2001b). That congressionally mandated report is intended to track the progress of the six national quality aims delineated in the Quality Chasm report: safety, effectiveness, patient-centeredness, timeliness, efficiency, and equity (Institute of Medicine, 2001a).
Study Approach
The committee developed its recommendations using an evidence-based approach whenever possible. While such evidence is essential, however, it cannot do justice to the avoidable harm that occurs in the current health care system. The priority areas recommended in this report encompass conditions for which patients are often receiving substandard care. This poor-quality care is due not to a lack of effective treatments, but to disjointed health care delivery systems that are unable to put these treatments into practice. Hence, the committee’s focus was on identifying the greatest opportunities for closing the gap between known best practice and usual practice and for reducing unwarranted variation in practice, with an emphasis on changes that must be made in the health care system to exploit those opportunities. The committee also dealt with quality as a systems property—not just the responsibility of overtaxed health care workers, but flowing naturally from the improved structure of redesigned systems of care.
The committee’s charge did not encompass evaluating the prospects for improving existing best-practice treatments through biomedical research or technological innovations. Rather, the committee focused on means of enhancing the delivery of those treatments. As affirmed in the Quality Chasm report (Institute of Medicine, 2001a:4): “The current care systems cannot do the job. Trying harder will not work. Changing systems of care will.” Improving the delivery of care in the 20 specific priority areas recommended by the committee by changing systems of care would provide a way for stakeholders at the national, state, and local levels to begin setting the course toward quality health care, along with reducing unacceptable disparities among Americans (Institute of Medicine, 2002a; Institute of Medicine, 2002c).
This study was designed as a “fast-track” effort. The committee met three times over a 3-month period. A public workshop also was held to provide an opportunity for the committee to hear from experts in the areas of mental health, child/adolescent health, long-term care, disability, end of life, and preventive care and to receive input from special-interest groups, the business community, and others (see Appendix B for the workshop agenda). Between meetings, the committee also made extensive use of subgroups. Immediately following the first meeting, three subgroups were formed to refine a set of preliminary criteria for the selection of priority areas, to craft a process for identifying the priority areas in a systematic and thoughtful manner, and to examine measurement issues involved in determining the final list of areas. Between the second and third meetings, two subgroups were formed to filter the initial slate of priority areas through a process agreed upon by the committee. The third and final meeting was spent deliberating the priority areas and formulating recommendations for this report.
It was originally envisioned that the priority areas would consist of common clinical conditions, most of which would be chronic in nature (Institute of Medicine, 2001a). The charge from AHRQ to the committee reflected this view. For several decades, the health care needs of the American people have been shifting from predominately acute care to chronic care. Today, chronic conditions are the leading cause of illness, disability, and death in the United States. In the year 2000, nearly half of the U.S. population, or approximately 125 million people, had such a condition. This figure is projected to increase to 157 million by 2020. In addition, 60 million Americans have two or more chronic conditions. Such chronic conditions also account for the majority of health care expenditures. In the year 2000, the direct costs of care for chronic conditions totaled $510 billion, and this figure is estimated to double to $1.07 trillion by 2020 (Partnership for Solutions, 2001).
The nation’s health care delivery systems have not significantly evolved to meet these changing demands. It has become increasingly clear that existing health care systems are designed to provide acute and emergency care and must be redesigned to deliver the type of
planned, proactive care needed to prevent and manage chronic disease. Although some patients receive well-orchestrated quality care, far too many others must navigate through a tangled web of health professionals and medical facilities. The result is often profound frustration and confusion on behalf of patients, families, and health care providers, which in turn increases the risk that health care needs will not be adequately met and contributes to disparities in care among social, ethnic, and socioeconomic groups (Anderson and Knickman, 2001; Hoffman et al., 1996; Institute of Medicine, 2002c; Wagner et al., 1996).
Although chronic conditions are clearly central candidates for quality improvement, the committee was charged and purposely constituted to adopt a more comprehensive approach. Thus, the scope of the study was broadened from the original focus on “priority conditions” as suggested in the Quality Chasm
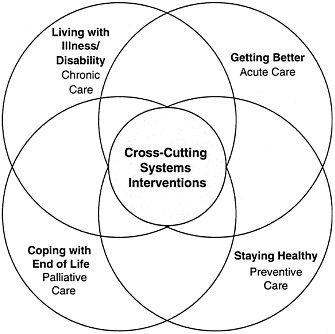
FIGURE 1–1 The committee’s initial framework for determining priority areas.
report to include other essential “priority areas” of health care, such as preventive care and behavioral health. Indeed, one of the committee’s main conclusions was that a purely disease-based approach to health care would not accomplish the needed transformation that is the intent of the recommended list of priority areas.
The committee decided a framework would be useful in the initial identification of candidate priority areas. Consistent with its charge, it built upon a framework originally formulated by the Foundation for Accountability that is to be incorporated into the National Health Care Quality Report (Foundation for Accountability, 1997a; 1997b; Institute of Medicine, 2001b). This consumer-oriented framework encompasses four domains of care: staying healthy (preventive care), getting better (acute care), living with illness/ disability (chronic care), and coping with end of life (palliative care).1 The committee also
recognized that a number of areas, such as the need for better coordination of care and support for self-management, cut across specific conditions and domains. The committee included these areas to emphasize the notion that changing the health system will require breaking down boundaries between diseases as well as classes of diseases. Thus, the committee supplemented the above four categories with a fifth—cross-cutting systems interventions—to ensure that improvement efforts will benefit all Americans, including those without specific priority conditions. Figure 1–1 presents the committee’s initial framework. The overlapping circles represent the interrelatedness of the five categories.
Recommendation 1: The committee recommends that the priority areas collectively:
-
Represent the U.S. population’s health care needs across the lifespan, in multiple health care settings involving many types of health care professionals.
-
Extend across the full spectrum of health care, from keeping people well and maximizing overall health; to providing treatment to cure people of disease and health problems as often as possible; to assisting people who become chronically ill to live longer, more productive and comfortable lives; to providing dignified care at the end of life that is respectful of the values and preferences of individuals and their families.
How Might the List of Priority Areas be Used?
The committee was acutely aware that report after report has been issued on the quality of health care and that government agencies and commissions have issued numerous “priority” recommendations. Another such report and list of priorities would not necessarily be helpful. The question is how this report is different and whether it might be a more practical guide to action.
Although it is impossible to predict all the activities that might be undertaken by various stakeholders to improve care in the priority areas identified by the committee, some uses of the list of areas presented in this report can be anticipated. These applications are likely to include the full range of health care system improvements and policy changes outlined in the Quality Chasm report, including applying evidence to health care, redesigning care processes around patient needs, making better use of information technology in the area of decision support, promoting accountability through measurement and performance feedback, and realigning payment incentives with quality care (Institute of Medicine, 2001a).
Building on the framework set forth in the Quality Chasm report, Berwick’s (Berwick, 2002) User’s Guide for the IOM Quality Chasm Report delineates four levels within the health care system at which quality improvement can take place (see Figure 1–2). Each priority area identified by the committee has aspects at each of these levels:
-
Level A—the experience of patients
-
Level B—the functioning of small units of care delivery, or micro-systems
-
Level C—the functioning of organizations that support micro-systems
-
Level D—the environment of policy, payment, regulation, accreditation, and other factors
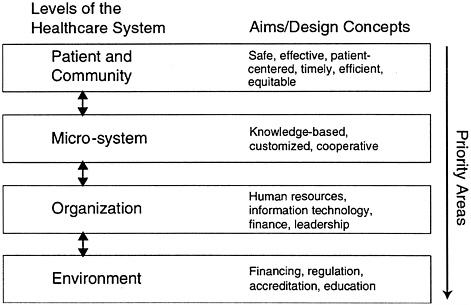
SOURCE: Reprinted with permission from Donald M.Berwick, M.D. (2002) (adapted from a slide used at the IOM Health Professions Education Summit held June 17–18, 2002 in Washington, D.C.).
FIGURE 1–2 Levels within the health care system for quality improvement.
Level A: The Experience of Patients
The overarching goal of quality improvement is to enhance the experience of patients. Achieving this goal entails improvement in the six national quality aims enumerated earlier: safety, effectiveness, patient-centeredness, timeliness, efficiency, and equity (Institute of Medicine, 2001a). While quality improvement generally involves reorganization at the levels of micro-systems, organizations, and environment, as described below, these efforts must ultimately be geared toward and judged by their ability to improve the direct experience of patients. Accordingly, one basis upon which the committee chose the priority areas was the degree to which broader changes in the way systems function in an area could improve the day-to-day care and quality of life for patients.
Level B: Micro-systems
Micro-systems are small work units that administer care to patients (Quinn, 1992). This “front-line” interaction is the basis on which patients judge their experience with the health care system. Examples of micro-systems include a physician’ office, an intensive care unit, and an outpatient surgery center. This is the level that is closest to the direct needs of patients.
The Chronic Care Model provides one example of a multidimensional solution to the often chaotic structure found at the microsystem level (Improving Chronic Illness Care, 2002; Wagner, 2001; Wagner et al., 2001; Wagner et al., 1996). Developed at Group Health Cooperative of Puget Sound in the mid-1990s under the Improving Chronic Illness Care program of The Robert Wood Johnson Foundation, this model is focused on the care
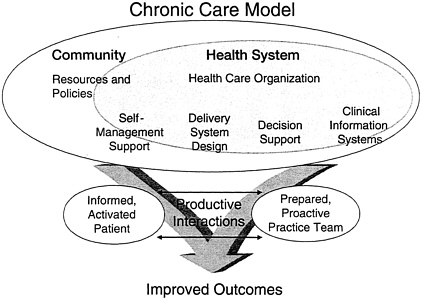
SOURCE: Reprinted with permission from Brian Austin (2002).
FIGURE 1–3 Chronic Care Model.
provided by primary care teams to patients with chronic illness and their families. Patients are expected to be active participants in their overall care plan and are acknowledged to be the principal managers of their condition(s). “Productive interactions” between an informed patient and a prepared practice team are the bedrock of the model. Patient preferences are emphasized, along with an evidence-based approach to effectively managing the course of the condition. Persistent planned follow-up completes the model. There are six key elements to this model, four of them implemented at the micro-system level (see Figure 1–3):
-
Self-management support—recognition of the patient and family as the source of control, with the practice team collaborating and providing expertise and tools.
-
Delivery system design—creation of a care delivery structure appropriate to the planned management of patients with chronic illness, with clear roles for all staff.
-
Decision support—integration of evidence-based guidelines into daily practice.
-
Clinical information systems—reminder and feedback systems for clinicians and the tools to plan care for both individuals and whole populations of patients.
An example of the Chronic Care Model in action is the Health Disparities Collaboratives, spearheaded by the Bureau of Primary Health Care within DHHS (Health Disparities Collaboratives, 2002). The goal of these initiatives is to develop programs that expand access to high-quality, culturally and linguistically competent health care—both primary and preventive—for underserved, uninsured, and underinsured Americans, as well as those in traditionally underserved minority,
ethnic, and racial groups. To meet this goal, the collaboratives focus on a subgroup of the entire population and then, if successful, spread to the rest of the patients in a community. The first collaborative, focused on diabetes, started in January 2000. Many of the priority conditions identified in this report could benefit from application of the Chronic Care Model. In addition to chronic care, the model’s concepts could be applied in preventive (Glasgow et al., 2001), acute, and palliative care.
In the realm of pediatrics, a parallel model, referred to as the Medical Home, has been developed for children with special health care needs. In this model, the family, the physician, and other health professionals in the community constitute a team that is intimately involved in the management and facilitation of all aspects of pediatric care. The American Academy of Pediatrics defines the Medical Home as being accessible, continuous, comprehensive, family-centered, coordinated, compassionate, and culturally effective (The Medical Home, 2002). The basic principles behind the Chronic Care Model and the Medical Home offer unprecedented direction for transforming health care micro-systems.
Level C: Organizations
Care can also be improved at the level of the health care organization. Techniques for improving care within these broader systems include compiling a disease registry, facilitating access to evidence-based practice guidelines, ensuring that best practices are incorporated into daily procedures, and measuring outcomes and providing feedback on performance. The Veterans Administration’s (VA) Quality Enhancement Research Initiative (QUERI) is an example of how a focus on priority areas can be used to change a health system by means of a data-driven, integrated quality improvement program. QUERI’S underlying goals are to identify best practices, to incorporate them into daily use, and to provide a feedback mechanism to ensure continuous quality improvement. The program functions to translate findings in the research setting into improved patient care and system redesign (Demakis et al., 2000; Feussner et al., 2000; Kizer et al., 2000). A six-step process is employed to ensure systematic adherence to quality improvement efforts:
-
Identify high-risk/volume diseases among veterans.
-
Identify best practices.
-
Determine existing practice patterns and outcomes across VA and any current variation from best practices.
-
Identify and implement interventions to promote best practices.
-
Document the best practices that improve outcomes.
-
Document that outcomes are associated with improved health-related quality of life.
A first step in developing the program was to identify target conditions. Criteria used to determine this group of conditions included the number of veterans affected, the burden of illness, and known health risks within the veteran population. The conditions chosen for the initial efforts were chronic heart failure, diabetes, HIV/AIDS, ischemic heart disease, mental health (depression and schizophrenia), spinal cord injury, and stroke. The priority areas recommended in this report might similarly be used to guide organizational improvement efforts within other private and public health care organizations.
Level D: Environment
Health organizations operate within a broader financial and social environment that creates both incentives and constraints on how they operate. Even the best-intentioned and best-planned changes developed for patients and organizations will fail to be translated into real-world settings unless they are implemented in an environment containing the appropriate regulations and financial incentives. It is essential to consider these incentives when developing interventions to improve care in
each of the priority areas. For example, payments might be bundled for management of some chronic conditions, or fee-for-service payments might be enhanced or tied to the achievement of certain performance goals for priority areas. Correspondingly, the priority areas identified in this report may represent particularly important focal points for the development and testing of models for better aligning these incentives with high-quality care.
Another important environmental influence is the educational system. Coordinating care and working cooperatively in interdisciplinary teams are not routinely emphasized in the training of health care professionals (Glick and Moore, 2001). As a result, clinicians often lack the necessary skills to effectively manage patients with chronic conditions. The priority areas can help drive the development of competency-based curricula that more closely mirror the demands of the practice environment.
What Can Be Expected from Those in the Field?
The committee readily acknowledges that there are organizations that have assumed leadership positions in many of the recommended priority areas. As part of its decision-making processes, the committee intentionally looked to the work of these groups. For example, as further discussed in chapter 4 and illustrated in Table 4–1, the committee selected seven chronic conditions that had already been targeted by other priority-setting initiatives.2 The intent of the committee’s list of priority areas is not to duplicate these efforts, but rather to promote synergy. The next step is to coordinate efforts and develop strategies for these shared conditions. Such collective action will provide the necessary leverage for improvement in the priority areas to take hold. As noted earlier, to detect whether there has been a shift in the quality of the health care routinely received by Americans, AHRQ will monitor progress in these areas through the National Health Care Quality Report. The changes effected could be even more dramatic if groups already active in these areas, as well as those who have yet to become involved, were to join forces around the priority areas.
The selected priority areas also share common elements with other national efforts. For example, four of the leading health indicators3 and ten of the focus areas4 identified in Healthy People 2010 (HP2010) link directly to the priority areas (United States Department of Health and Human Services, 2000). Although this report supports the goals of HP2010— increasing quality and years of life and eliminating health disparities—the priority areas emphasize improving the health care delivery system, whereas HP2010 focuses on public health concerns.
The priority areas also coincide with many of the performance measures already in place to monitor health care quality. For example, the National Committee for Quality Assurance’s (NCQA) Health Plan Employer Data and Information Set (HEDIS®), used to compare performance among managed care plans, contains measures relevant to 10 of the priority areas5 (National Committee for Quality Assurance, 2002). The Joint Committee on Accreditation of Healthcare Organization’s performance measurement initiative, ORYX, incorporates standardized performance measures into the accreditation process of
hospitals. ORYX encompasses four core measurement areas on which hospitals must collect data for all patient discharges, all of which are applicable to the selected priority areas6 (Joint Commission on Accreditation of Healthcare Organizations, 2002). As a final example, The Centers for Medicare and Medicaid Services (CMS) has implemented quality improvement organizations (QIOs) at the state and regional levels as a mechanism for improving the quality of care provided to Medicare beneficiaries (Centers for Medicare and Medicaid Services, 2002). The QIOs target six clinical topics, five of which overlap with the committee’s priority areas.7
Even though there are many groups that implement performance measures, a common conceptual framework, such as the priority areas, is needed. At present there exists a patchwork of measures that often do not send consistent signals. Gains could be made in the standardization of these measures so that more meaningful and comparable quality-of-care information could be generated, thus reducing burden and contributing to greater improvements. The recently released IOM report Leadership by Example: Coordinating Government Roles in Improving Health Care Quality calls for the government to take the lead in promulgating standardized performance measures and points to the priority areas as the springboard for this effort (Institute of Medicine, 2002b).
In addition, it is the committee’s hope that this report will be seen as a strong plea to physicians, nurses, pharmacists and other health care professionals, as well as health care organizations, to actively support and foster quality improvement in the priority areas identified herein. Each individual is encouraged to ask what he/she can do today, this month, this year to accelerate quality improvement in the priority areas in which he/she provides care.
First, everyone involved should recognize that the health care system will be changed only through the individual and organized actions of patients, families, doctors, nurses, and administrators. All these groups must hold themselves accountable for making changes to improve the quality of the care they deliver or accept. And while it is recommended later in this report that AHRQ convene national experts to develop action plans for improvement in the priority areas, nobody involved should wait.
Second, the recommended priority areas deliberately encompass a wide range of health care issues in which improvement is necessary for overall system change. However, the priorities have been recommended, in part, so that most individuals and organizations can have a logical and much narrower focus. For example, patients and family members can focus on particular conditions that concern them. Patient-centered care requires engaged patients and families who understand the appropriate care recommendations and are willing and able to educate and challenge their providers if they are not receiving these services. Consumer and patient groups can and should focus on their particular conditions of interest, developing appropriate educational materials that support the most appropriate care; educating patients, providers, employers, policy makers, and the media about that care; and asking hard questions when it is not provided.
Likewise, providers, especially specialists, will usually regard one or more areas—whether it be diabetes or cancer screening or immunizations—as particular priorities. They can work to ensure that they are providing the best evidence-based care and that their colleagues are encouraged to do the same.
Health care organizations may deal with a broader array of issues, but again they can focus on certain priorities. For example, hospitals might start by addressing nosocomial infections, implementing the guidelines of the Centers for Disease Control and Prevention and ensuring through their associations and regulatory bodies that all hospitals implement those guidelines.
Hospitals might also work to ensure that appropriate systems are in place to help doctors and nurses avoid pharmocolgical errors in the hospital and support clinicians in pain management.
Purchasers for both government and private programs should determine whether their coverage, payment, and information systems support and encourage health professionals in providing the clinically appropriate care at all times. Public- and private-sector policy makers should also work to identify data sources that clearly identify whether and where the appropriate care is and is not provided. The priority areas recommended by the committee may be a useful starting point for such efforts.
If quality improvement in the priority areas is to succeed, the collective efforts of all the aforementioned individuals and groups will need to be channeled into the effort. The Quality Chasm report recommends identification of the priority areas under the heading “Taking the First Steps” (Institute of Medicine, 2001a). The task is to take those first steps, and then continue the journey until we are confident that the quality chasm has been crossed.
Organization of the Report
Chapter 2 presents the rationale for the criteria used by the committee as a basis for selecting the priority areas. Chapter 3 identifies and describes the priority areas, including how they emerged from the selection process, the evidence base for their selection, and examples of how improving the quality of health care in these areas could have transformative impact on the quality of health care. Finally, Chapter 4 provides a detailed summary of the process developed and employed by the committee to identify candidate priority areas and narrow them down to the final list of 20 recommended in this report.
References
American Diabetes Association. “Facts & Figures: The Impact of Diabetes.” Online. Available at http://www.diabetes.org/main/application/commercewf;JSESSIONID_WLCS_DEFAULT http://www.diabetes.org/main/info/facts/impact/default2.jsp [accessed Aug. 6, 2002].
Anderson, G., and J.R.Knickman. 2001. Changing the chronic care system to meet people’s needs. Health Aff (Millwood)20 (6): 146–60.
Berwick, D.M.2002. A User’s Guide for the IOM’s ‘Quality Chasm’ Report. Health Aff (Millwood) 21 (3):80–90.
Centers for Disease Control and Prevention. 2001. Trends in screening for colorectal cancer— United States, 1997 and 1999. Morbidity and Mortality Weekly Report50:161–66.
——. 2002. The Burden of Chronic Diseases and Their Risk Factors.Atlanta, GA: CDC, National Center for Chronic Disease Prevention and Health Promotion.
Centers for Medicare and Medicaid Services. 2002. “Statement of Work, QIOs: 7th Round, February 2002 Version.” Online. Available at http://www.hcfa.gov/qio/2b.pdf [accessed May 13, 2002].
Chassin, M.R.1997. Assessing strategies for quality improvement. Health Aff (Millwood)16 (3):151–61.
Chassin, M.R., and R.W.Galvin. 1998. The urgent need to improve health care quality. Institute of Medicine National Roundtable on Health Care Quality. JAMA280 (11): 1000–5.
Chassin, M.R., J.Kosecoff, R.E.Park, C.M. Winslow, K.L.Kahn, N.J.Merrick, J.Keesey, A.Fink, D.H.Solomon, and R.H.Brook. 1987. Does inappropriate use explain geographic variations in the use of health care services? A study of three procedures. JAMA 258(18):2533–7.
Demakis, J.G., L.McQueen, K.W.Kizer, and J.R. Feussner. 2000. Quality Enhancement Research Initiative (QUERI): A collaboration between research and clinical practice. Med Care38 (6 Suppl 1):I17–25 .
Feussner, J.R., K.W.Kizer, and J.G.Demakis. 2000. The Quality Enhancement Research Initiative (QUERI): From evidence to action. Med Care38 (6 Suppl 1):I1–6.
Foundation for Accountability. 1997a.“The FACCT Consumer Information Framework: Comparative Information for Better Health Care Decisions.” Online. Available at http://www.facct.org/information.html [accessed June 4, 2002a].
——. 1997b. Reporting Quality Information to Consumers.Portland, OR: FACCT.
Glasgow, R.E., C.T.Orleans, and E.H.Wagner. 2001. Does the Chronic Care Model serve also as a template for improving prevention? Milbank Q79 (4):579–612, iv-v.
Glick, T.H., and G.T.Moore. 2001. Time to learn: The outlook for renewal of patient-centred education in the digital age. Med Educ35 (5):505–9.
Harris Interactive. 2001. Survey on Chronic Illness and Caregiving.New York: Harris Interactive.
Health Disparities Collaboratives. 2002. “Health Disparities Collaboratives.” Online. Available at http://www.healthdisparities.net/ [accessed June 4, 2002].
Hoffman, C., D.Rice, and H.Y.Sung. 1996. Persons with chronic conditions: Their prevalence and costs. JAMA276 (18):1473–9.
Improving Chronic Illness Care. 2002. “Overview of the Chronic Care Model.” Online. Available at http://www.improvingchroniccare.org/change/model/components.html [accessed June 4, 2002].
Institute of Medicine. 1999. Ensuring Quality Cancer Care.M Hewitt and J.V.Simone, eds. Washington, D.C.: National Academy Press.
——. 2000. To Err Is Human: Building a Safer Health System.L.T.Kohn, J.M.Corrigan, and M.S.Donaldson, eds. Washington, D.C: National Academy Press.
——. 2001a. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, D.C.: National Academy Press.
——. 2001b. Envisioning the National Health Care Quality ReportM.P.Hurtado, E.K. Swift, and J.M.Corrigan, eds. Washington, D. C.: National Academy Press.
——. 2002a. Care Without Coverage: Too Little, Too Late.Washington, D.C.: National Academy Press.
——. 2002b. Leadership by Example: Coordinating Government Roles in Improving Health Care Quality.Washington, D.C.: National Academy Press.
——. 2002c. Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care.B. S.Smedley, A.Y.Stith, and B.D.Nelson, Eds. Washington, D.C.: National Academy Press.
Joint Commission on Accreditation of Healthcare Organizations. 2002. “ORYX: The Next Evolution in Accreditation; Questions and Answers about the Joint Commission’s Planned Integration of Performance Measures into the Accreditation Process.” Online. Available at hhtp://www.jcaho.org/perfmeas/oryx_qa.html [accessed May 13, 2002].
Kizer, K.W., J.G.Demakis, and J.R.Feussner. 2000. Reinventing VA health care: Systematizing quality improvement and quality innovation. Med Care38 (6 Suppl 1):I7–16.
Leatherman, S. and D.McCarthy. 2002. Quality of Health Care in the United States: A Chartbook. New York, NY: The Commonwealth Fund.
National Committee for Quality Assurance. 2002. State of Health Care Quality Report. Washington, DC: NCQA.
O’Connor, G.T., H.B.Quinton, N.D.Traven, L.D. Ramunno, T.A.Dodds, T.A.Marciniak, and J. E.Wennberg. 1999 . Geographic variation in the treatment of acute myocardial infarction: The Cooperative Cardiovascular Project. JAMA 281 (7):627–33.
Partnership for Solutions, The Johns Hopkins University. 2001. “Partnership for Solutions: A National Program of The Robert Wood Johnson Foundation.” Online. Available at http://www.partnershipforsolutions.org/statistics/prevalence.htm [accessed Dec. 12, 2002].
President’s Advisory Commission on Consumer Protection and Quality in the Health Care Industry. 1998. Quality First: Better Health Care for All Americans—Final Report to the President of the United States.Washington DC: U.S. Government Printing Office.
Quinn, J.B.1992. Intelligent Enterprise: A Knowledge and Service Based Paradigm for Industry.New York, N.Y.: New York Free Press.
Schuster, M.A., E.A.McGlynn, and R.H.Brook. 1998. How good is the quality of health care in the United States?Milbank Q76 (4): 517–63, 509.
The Medical Home. 2002. Pediatrics 110 (1 Pt United States Department of Health and Human Services. 2000. Healthy People 2010.In two volumes, conference edition. Washington, DC: U.S. Government Printing Office.
Wagner, E.H.2001. Meeting the needs of chronically ill people. BMJ323 (7319):945–6.
Wagner, E.H., B.T.Austin, C.Davis, M. Hindmarsh, J.Schaefer, and A.Bonomi. 2001. Improving chronic illness care: Translating evidence into action. Health Aff (Millwood)20 (6):64–78.
Wagner, E.H., B.T.Austin, and M.Von Korff. 1996. Organizing care for patients with chronic illness. Milbank Q74 (4):511–44.
Welch, W.P., M.E.Miller, H.G.Welch, E.S. Fisher, and J.E.Wennberg. 1993. Geographic variation in expenditures for physicians’ services in the United States. N Engl J Med328 (9):621–7.
Wennberg, J., and A.M.Gittelsohn. 1973. Small area variations in health care delivery. Science 182 (117): 1102–8.














