Executive Summary
A COMMUNITY PERSPECTIVE
In its first three reports, the Committee has shown that the lack of health insurance is widespread and enduring in the United States and that there are adverse health, psychosocial, and economic impacts on uninsured individuals and members of families with at least one uninsured member. By removing or lowering financial barriers to access to health care, health insurance can and does make a positive difference in the lives of insured persons when they need health care. This report sets the experiences of uninsured individuals and families in the context of the communities in which they live, work, and seek health care. It considers another aspect of health insurance’s importance, namely, as a predictable and stable revenue source for health care service providers.
In A Shared Destiny: Community Effects of Uninsurance, the Committee finds that the adverse effects of uninsurance that accrue to uninsured individuals and families in a community, as well as the financial strain placed on the community’s health care system, have important spillover effects on community health care institutions and providers. In communities with higher uninsured rates, access to health services and consequent benefits are compromised for persons other than those who lack coverage. The community effects of uninsurance are often difficult to see at a national level but can be quite vivid at the local level. The great heterogeneity in the organization of health care services locally and in the ways that care for uninsured persons is financed affects how uninsurance interacts with local health services, a community’s social and economic fortunes, and may even affect the health of its members. A
Shared Destiny documents a number of these interactions and presents working hypotheses about many more.
Health care practitioners and institutions are an important part of most local communities, knitting together the lives of individual community residents as providers facilitate access to care, contribute to local economic vitality, and protect and improve the health of community members. Even for healthy community members, having a regular health care provider and more advanced medical services and resources available has real value. These health care relationships and resources enhance the quality of our lives and peace of mind.
The failure to insure all members of American communities can distort and even disrupt these relationships between health care providers and the people they serve. Uninsured persons have much more trouble finding health care providers who will see them, use health care services much less often when they need care than do insured persons, and are more likely to incur high unreimbursed costs when they do obtain care (IOM, 2001a, 2002b). As a result, the presence of a sizable or growing population of uninsured persons may impose destabilizing financial stresses on the health care providers that serve all community members and on the public and private sources that finance local health care. Lack of access to health care results in adverse economic, social, and health consequences for uninsured persons and their family members (IOM, 2001a, 2002a, 2002b). Ripple or spillover effects of these consequences on uninsured persons may be felt by their insured neighbors. For example, an uninsured breadwinner’s lack of health care can lead to disability and loss of income that necessitates public support payments.
This fourth report of the Committee on the Consequences of Uninsurance explores the ways in which many others may be affected by the lack of health insurance of some of us. The Committee hypothesizes a series of spillover effects of uninsurance, effects that extend beyond the adverse health and financial impacts on uninsured individuals and families documented in Coverage Matters, Care Without Coverage, and Health Insurance Is a Family Matter. A Shared Destiny establishes an analytic framework for thinking about the causal pathways hypothesized to lead to the more widespread impacts of uninsurance, assesses the limited empirical evidence that exists about community effects, and proposes a research agenda to better demonstrate the presence or absence of these effects.
Given the large, persisting population of uninsured persons in the United States, the current economic environment and state government fiscal situations make the problems of uninsurance even more urgent and in need of remedy. The national uninsured rate of 16.5 percent among persons under age 65 masks substantial variation in state and local uninsured rates, median durations of uninsured spells of individuals, and the sizes and concentrations of uninsured groups within different populations (Mills, 2002). Uninsured rates vary across the states from 8.7 percent in Iowa to 26 percent in Texas (see Figure ES.1).
Over the past two decades the uninsured rate and total number of uninsured nationally has grown slowly but steadily (with only a slight dip during 1999 and 2000). With the current combination of higher unemployment and rapidly rising
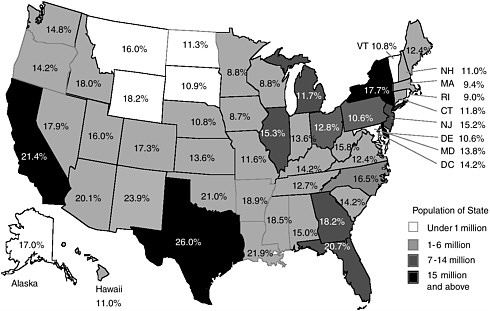
FIGURE ES.1 Probability of being uninsured for population under age 65, by state, 2001.
SOURCE: Fronstin, 2002, estimates based on March 2001 Current Population Survey.
costs of health care and insurance premiums, absent major public policy reforms, the national uninsured rate can be expected to rise more rapidly in future years (Chernew et al., 2002; Cutler, 2002).
Assessing Community Effects
For the purposes of this report, the Committee defines a community as a group of people who (1) live in a particular geographic area and (2) have access to a specific set of health resources for which information about financial and health-related outcomes exists. Geographical entities (e.g., rural counties, metropolitan statistical areas) are the units for which epidemiological, demographic, and economic data are collected most often, and they serve as rough approximations for health services market areas. The limited availability of research about community-level attributes, for example, the availability of specialty care within a neighborhood, constrains the Committee’s analysis. Findings are often based on cross-sectional comparisons among states, metropolitan areas, and rural counties with differing uninsured rates as well as on illustrative case studies and other qualitative evidence. Because of the limited data with which to characterize and monitor community effects and the challenges of distinguishing effects that stem from the extent of uninsurance from effects of related community-level characteristics (e.g., income structure), the Committee developed a research agenda as part of its work.
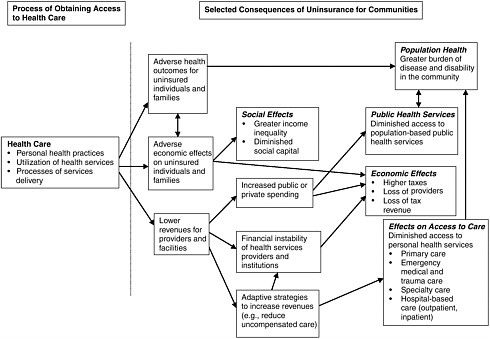
The Committee hypothesizes that the experiences of uninsured individuals and of families within a community influence the collective and aggregate effects of uninsurance on their community. The causal pathways hypothesized for community effects incorporate the experiences of uninsured individuals and families as well as the performance of health care institutions and providers. Figure ES.2 depicts the Committee’s conceptual framework for thinking about the breadth and scope of community effects and the pathways through which those effects are exerted. The framework builds on a widely used behavioral model of access to health services (Andersen, 1995; Andersen and Davidson, 2001) and focuses primarily on the economic, financial, and coverage-related factors that affect outcomes of health care services and their impact on communities. These hypothesized pathways and effects are noted in the sections that follow. Some of these effects on local health care services, local economies, and population health have been documented. Other effects are not well understood and require more extensive and systematic data collection and analysis.
CONTEXT FOR COMMUNITY EFFECTS
Financing the Delivery of Health Services
Over the past 25 years, federal and state policies to control health care costs and an increasingly competitive private market for health care services and coverage have constrained reimbursement rates for care, eroding previous levels of subsidy for uncompensated care costs associated with care delivered to uninsured persons. The effects of this erosion have been felt more strongly in communities with large or growing uninsured populations and by providers (e.g., public hospitals) that serve a high number or proportion of uninsured persons. Although the mainstream health care system provides most of the services that uninsured persons receive, the uninsured rely disproportionately on safety-net arrangements for care (Cunningham and Tu, 1997; Lewin and Altman, 2000). In urban areas, multiple tiers of providers and services tend to segregate patients by income level and coverage status, isolating insured patients from the experiences of uninsured patients. In rural areas, insured and uninsured patients may have more in common because a more limited set of providers typically serves all community members and safety-net arrangements tend to be less formal.
Responsibility for financing and providing health care to uninsured persons in the United States is fragmented and ill defined. State, county, and municipal facilities are, often by default, the providers of last resort for uninsured patients. The so-called safety net is a highly diverse set of frequently ad hoc local arrangements to accommodate patients without the ability to pay for their own care. The incomplete patchwork of federal, state, and local mandates that minimal services be provided does not typically specify a scope of benefits to which a medically indigent person is entitled, nor are there guarantees that providers will be reimbursed. The particular local configuration of safety-net arrangements—for ex-
ample, whether it is centralized or dispersed—and its effectiveness in caring for the community’s uninsured residents influences the range and extent of community effects related to uninsurance.
The current amalgam of service arrangements and the mix of public and private funding sources was not designed as an integrated system; rather, it has resulted from the aggregation, over time, of initiatives and developments in both the private and the public sectors. Because the organization and delivery of care are closely linked to health insurance, the needs of persons who lack health insurance have been of secondary interest, often only as afterthoughts in the development of public policy.
Who Pays for Care for Uninsured Persons?
Public support of the health care expenses of uninsured Americans accounts for as much as 85 percent of the estimated $34–$38 billion (for 2001) in uncompensated care costs that they incur (Hadley and Holahan, 2003). To address the health needs of a relatively large low-income population, state and local jurisdictions may find themselves under considerable financial pressure, supporting health services both directly, through public hospitals and clinics, and indirectly, through public insurance programs such as Medicaid.
Federal, state, and local governments play different roles in financing care for uninsured persons. The federal government’s primary role is financing health care services through insurance mechanisms (e.g., the State Children’s Health Insurance Program [SCHIP]), grant programs for service delivery (e.g., community health centers), and programs of direct care (e.g., Department of Veterans Affairs facilities). States determine eligibility standards and provide funding for Medicaid, SCHIP, and similar state programs that serve populations that do not qualify for federal matching funds. Local governments operate public clinics and hospitals and frequently provide personal health care services directly or through contracts to uninsured residents. Physicians in solo and group practices, practicing in clinics and in hospital settings, provide an estimated $5.1 billion in free or reduced-price charity care to uninsured patients (Hadley and Holahan, 2003).
COMMUNITY EFFECTS ON ACCESS TO CARE
Insurance facilitates access to health care by removing or diminishing financial barriers faced by individuals and families. It also supports the stable operations of health care providers and institutions. The Committee hypothesizes that the burden of financing care for uninsured persons affects the health services available to all community residents, especially in urban areas where providers treat large numbers of uninsured persons and in rural areas where providers treat relatively high proportions of them. The pathway proposed is that of lower provider revenues resulting from the combination of the lower use of health services by
uninsured persons (compared with use by insured persons), as well as the uncompensated costs incurred when uninsured persons do receive health care. The Committee finds that low- to moderate-income1and uninsured residents have worse access to health care in communities with high uninsured rates than they do in communities with relatively low rates, although the causal influence of the local uninsured rate on access is unclear. Health care providers in rural and urban settings both experience financial pressures related to lower revenues but may adopt different strategies for coping with them. In an effort to avoid the burden of uncompensated care for uninsured residents or to minimize its financial impact, physician practices and hospitals may cut back services, reduce staffing, relocate or close.
Three recent studies examine the relationship between self-reported access to care and community uninsurance in urban areas (Cunningham and Kemper, 1998; Brown et al., 2000; Andersen et al., 2002). All of the studies rely on survey data about self-reported access to care, using measures such as difficulty obtaining care or not having seen a physician in the previous 12 months, and include limited analytic adjustments for the many covariates of insurance status. These studies find that, unadjusted for the major covariates of local uninsured rate, the uninsured rate in urban areas is inversely associated with the ability of uninsured and of low- to moderate-income residents to obtain needed and regular health care. Such measures of access to health services are basic markers of effective, quality care that improves health outcomes (Millman, 1993; IOM, 2002a, 2002b).
Primary Care
Aside from the studies of access to care described above, there are few studies of uninsurance’s effects on primary care. Shortages of physicians in rural and urban areas with relatively high uninsured rates can mean less access to primary care for all residents. Over the 1990s, the proportion of physicians who have provided charity care (whether to uninsured or insured persons) has declined, a decrease that is explained as a response to declining provider revenues (Reed et al., 2001; Cunningham, 2002). In rural areas, physicians are more likely to treat Medicaid and uninsured patients and have higher proportions of Medicare patients. Reimbursement levels in rural areas are lower than in urban areas and safety net arrangements tend to be less formal and not supported with public funds (Taylor et al., 2001; Coburn, 2002).
In urban areas, public clinics play a key role. One survey of primary care access at four types of ambulatory care sites in New York City in 1997 finds that public sites provide the most comprehensive care for low-income patients and
concludes that serving increasing numbers of uninsured persons may weaken ambulatory sites’ capacity to provide primary care to all members of the community (Weiss et al., 2001).
Community health centers (CHCs) face financial pressures on a number of fronts: from reduced income from Medicaid patients, from reduced public subsidies, and from an increased proportion of their patient mix that is uninsured (Lewin and Altman, 2000). These pressures have adversely affected CHCs’ capacity to serve all of their patients (Shi et al., 2001; Rosenbaum et al., 2002). A longitudinal study of 588 CHCs between 1996 and 1999 finds that reductions in capacity appear to be concentrated among subsets of health centers with a sizable number or share of uninsured patients or those that have experienced a recent increase in uninsured patients (McAlearney, 2002).
Reduced access to primary care may increase demand for services in already overcrowded hospital emergency departments. In turn this may reduce access to care and the quality of care received, regardless of insurance status.
Emergency Medical Services and Trauma Care
Emergency departments and trauma centers are key examples of how market pressures and public policies interact in ways that create incentives for hospitals to reduce their exposure to financial losses associated with serving uninsured patients. For example, the federal Emergency Medical Treatment and Labor Act (EMTALA) requires that emergency deparments (EDs) maintain an “open door” policy, serving all comers without regard to their ability to pay. The service areas of highly specialized and resource-intensive trauma centers extend across populous metropolitan areas and multicounty regions in rural areas, transcending local neighborhood boundaries that often separate wealthier, insured groups from less wealthy, uninsured ones. In many urban and rural areas, hospital emergency departments are often filled beyond capacity, affecting all who rely on them (Richards et al., 2000; Derlet et al., 2001; Lewin Group, 2002).
ED overcrowding is primarily caused by an insufficient number of staffed inpatient beds into which ED patients can be admitted (Brewster et al., 2001). This bed shortage is in part a result of market and related financing pressures on hospital operating margins, pressures that include the relative amount of uncompensated care provided by the hospital, some of which is delivered to uninsured patients. Overcrowding adversely affects the quality of care for all emergency department patients (Bindman et al., 1991; Kellermann, 1991; Rask et al., 1994). Members of medically underserved groups are particularly likely to suffer because they have fewer options to obtain primary care outside EDs, compared with insured persons, although they use EDs less frequently than do insured persons (Felt-Lisk et al., 2001; IOM, 2002a; Weinick et al., 2002).
Specialty Care
Evidence about the relationship between the uninsured rate and access to specialty services other than emergency medical care is limited. A consequence of the on-call obligations that hospitals may require of affiliated specialists, under EMTALA, is the relocation of orthopedists, neurosurgeons, and other specialists out of the area, leading to local shortages of particular specialty services (Bitterman, 2002). In addition, in rural areas, all residents may experience lessened access to specialty care (as with primary care) if providers leave the community because of financially unviable practice conditions (Ormond et al., 2000a). Rural areas tend to have shortages of specialty physicians, and referrals are often to specialists in urban areas, which may deter some patients from obtaining care or result in their seeking it later than advisable. The inability of primary care providers to make specialty referrals for their patients may be an effect of a relatively high local uninsured rate.
Urban safety-net hospitals and academic health centers (AHCs), major sites for specialty care in their communities, are also likely to be affected by high levels of uninsured patients (Gaskin, 1999). A study of 125 public and private academic health centers between 1991 and 1996 finds that in local markets with high managed care penetration, care for uninsured persons had been increasingly concentrated at a subset of AHCs, resulting in less aggregate revenue for the AHCs. For private AHCs, particularly those that are not located in neighborhoods with high uninsured rates (e.g., central city), one strategic response of hospitals to such cost pressures has been to eliminate specialty services with relatively poor rates of reimbursement, such as burn units, trauma care, pediatric and neonatal intensive care, emergency psychiatric inpatient services, and HIV/AIDS (Gaskin, 1999; Commonwealth Fund, 2001).
Hospital-Based Care
Hospitals treating uninsured patients must contend with the cumulative effects of inadequate care for chronic conditions, exacerbated acute illnesses, and delayed treatment (IOM, 2002a). In addition, hospital outpatient departments and their satellite clinics are an important source of both primary and specialty care for medically underserved populations, including uninsured persons and their families. As discussed above, one way that hospitals have responded to increasing financial pressures is to reduce the availability of certain services known to attract persons who are more likely than average to be uninsured (Gaskin, 1999). The reduced availability or complete loss of these services (e.g., trauma, burn care, care for HIV/AIDs) may be expected to affect everyone in the health services market who needs them. In urban areas, this community effect is likely to affect access for low-income residents, who have few options for care other than their local public or private safety net hospitals. In contrast, in rural areas, where health services are
less segmented, adverse effects on hospital operating margins are more likely to affect the care of residents across income levels (Sutton et al., 2001).
Financial pressures may also motivate a local hospital’s governing body to merge, to convert from public to private ownership status, or from private non-profit to for-profit status, or to close (Meyer et al., 1999; Needleman, 1999). Local uninsured rates and the burden of uncompensated care costs to local and state government have contributed to the conversions of some large urban public hospitals (Bovbjerg et al., 2000b). The conversion, merger, or closing of a hospital may lead to improved and less costly health services locally. However, the loss of a physical plant and with it the relatively automatic support that a bricks-and-mortar institution commands may also result in a net loss of public dollars for indigent health care, and the proposed closing of a public hospital may be perceived by other local providers as threatening the financial stability of their own institutions by spreading the burden of uncompensated care more broadly.
New Analysis of Hospital Services and Financial Margins
The Committee commissioned analyses of hospital services and financial margins across the 85 largest metropolitan statistical areas and across nonmetropolitan (rural) counties in seven states in the 1990s. Compared to urban areas with relatively low uninsured rates, the analyses show that hospitals in urban areas with relatively high uninsured rates:
-
have fewer beds per capita (except for intensive care unit beds);
-
offer fewer services for vulnerable populations, including psychiatric, alcohol and chemical dependence, and AIDS care; and
-
are less likely to offer trauma and burn care (Gaskin and Needleman, 2002).
In comparison to rural areas with relatively low uninsured rates, hospitals in rural areas with relatively high uninsured rates:
-
have lower financial margins,
-
have fewer intensive care unit beds, and
-
offer fewer psychiatric inpatient services (Needleman and Gaskin, 2002).
ECONOMIC AND SOCIAL IMPLICATIONS OF UNINSURANCE WITHIN COMMUNITIES
Over the past two decades the uninsured rate nationally has grown slowly but steadily, despite an increasingly tight labor market that expanded employment-based coverage and yielded tax revenues to expand public coverage. Present economic trends have changed from boom to economic recession and, absent major policy interventions, indicate a continuing rise in this rate. Health care cost
and health insurance premium increases are projected to add to the ranks of the uninsured (Chernew et al., 2002; Cutler, 2002).
Health insurance is not the solution to all communal ills; nevertheless, the Committee hypothesizes that its presence or absence can make a substantial difference for a community’s economic fortunes. The costs of care for uninsured Americans are passed down to taxpayers and consumers of health care in the forms of higher taxes and higher prices for services and insurance. Locally, residents are likely to subsidize care for their uninsured neighbors through taxes and higher prices for health services and health insurance in their community. The tax burdens of funding care for uninsured residents is more concentrated locally than is the burden of Medicaid finance or other insurance-based public programs in which the federal government participates.
For communities as for individuals and families, uninsurance can be associated with a loss of income and increased expenditures that weaken shared economic and social foundations. Increased public sector support for or reimbursement of providers for uncompensated care delivered to uninsured persons requires that additional public revenues be raised, resources be diverted from other public purposes, or budget cuts be imposed, adversely affecting all members of the community and potentially increasing the number of uninsured persons.
State and local governments’ capacity to finance health care for uninsured persons tends to be weakest at times when the demand for such care is likely to be highest, namely, during economic recessions. While health insurance programs such as Medicaid also make claims on state tax revenues, the incidence of the tax burden for federal or shared federal–state financing programs falls more broadly upon American taxpayers and can alleviate some of the financial demands that uninsurance places on disproportionately affected communities. As a result, the communities most in need of tax-subsidized assistance to health services institutions and providers may be the least likely to be able to afford to finance care for uninsured and underserved persons (Lewin and Altman, 2000).
Budget Implications for States and Localities
During the 1990s, the fiscal capacity and resources of the states for spending on health programs grew. Starting in 1999, states have increasingly been experiencing hard times, with economic recession, federal cuts to Medicare and Medicaid, and public resistance to raising taxes (Dixon and Cox, 2002; Lutzky et al., 2002). Many states plan to cut Medicaid spending in the coming years (Smith et al., 2002). The consequences of these responses are likely to result simultaneously in lower public funding for health insurance, fewer public funds available for other purposes, and higher taxes. States’ ability to levy taxes and their tax structures constrain revenue increases to support care for uninsured persons. The federal-state financing structure of Medicaid places great demands on state budgets even as it provides federal monies to the states. Medicaid’s federal match is designed to provide relatively greater federal support to those states with lower average per-
sonal income; however, it only imperfectly reflects relative state needs (Miller, 2002b).
Economic Base and the Potential for Development
How health care contributes to the economic vitality of communities and how uninsurance within a community affects the local economy overall are poorly documented (Doeksen et al., 1997). A high uninsured rate may both indicate and contribute to an area’s economic challenges as it reflects the relative availability of employment-based coverage. Coverage is less likely to be available in areas with a lower-waged labor force.
A high uninsured rate and the corresponding burden of uncompensated care on the local health care system may threaten the survival of individual providers or hospitals, reducing the viability of the economic base of the community. These hypothesized effects are easier to measure in rural than in urban areas because of the smaller scale and simpler scope of rural economies and the influential economic role of local hospitals in rural areas (Doeksen et al., 1997; Cordes et al., 1999; Colgan, 2002). Public financing, particularly through Medicare and Medicaid, is especially important for the rural health services infrastructure (Cordes, 1998). These dollars, spent locally, can be a source of new jobs, population growth, and tax revenues, making hospitals a form of economic development that brings outside dollars into the community (Cordes et al., 1999). Rural hospital closings are also associated with the loss of community physicians, and the jobs and tax revenues that private practices generate (Hartley et al., 1994; Doeksen et al., 1997).
UNINSURANCE AND COMMUNITY HEALTH
The health of the community itself, including its insured as well as uninsured residents, may be compromised by high levels of uninsurance. The sheer number of uninsured persons in an area contributes disproportionately to the community’s burden of disease and disability, because of the poorer health of uninsured community members and from spillover effects on other residents. The mechanisms for this can be as diverse as the spread of communicable diseases and the paucity or loss of primary care service capacity as a result of physicians’ location decisions, cutbacks in clinic staffing and hours, or outright closures.
Area-wide rates of potentially avoidable hospitalizations serve not only as indicators of access to care but also as measures of the acuity of illness experienced within a population and the efficiency with which health care is provided overall. Uninsured patients are more likely to experience avoidable hospitalizations than are privately insured patients when measured as the proportion of all hospitalizations, and studies consistently report substantially higher rates of these hospitalizations in lower-income areas (Billings et al., 1993, 1996; Millman, 1993; Bindman
et al., 1995; Pappas et al., 1997). Uninsurance is likely to contribute to these higher rates.
Public Health and Community Uninsurance
The intentional dispersal of anthrax through the U.S. mail in late 2001 exposed yet another way in which uninsurance could threaten community health, when the impaired access to care of uninsured persons means delays in detecting, treating, and monitoring the transmission of infectious diseases linked to bioterrorism (Wynia and Gostin, 2002; IOM, forthcoming 2003). As public and policy attention turned to the country’s emergency preparedness, the weaknesses of the highly fragmented public and private health care systems became apparent. This fragmentation and minimal capacity for communication across systems and types of care hamper the ability of a community to respond rapidly and effectively to an unfamiliar threat to the public’s health.
Public health includes the key functions of assessing population health, developing policy solutions for problems identified, and ensuring that problems are addressed by the solutions devised (IOM, 1988). Many health departments also care for uninsured residents who have difficulty gaining access to care in other settings. In many parts of the country, health department officials have expressed their perceptions of being caught between the increasing demand and need for care of growing numbers of uninsured persons and diminished budgets (IOM, 1988, forthcoming 2003; Lewin and Altman, 2000).
Efforts to meet the personal health care needs of uninsured residents place considerable demands upon local health department resources and may divert funds from population-based public health activities. This diversion of resources undermines communities’ capacity to prepare for emergencies and bioterrorist threats. National planning for the vaccination of some or all of the U.S. population against smallpox is coming up against the capacity limitations of public health departments, unless there is an infusion of new federal funds.
Communicable disease control is a core function of public health departments. The Committee hypothesizes that the presence of sizable uninsured populations without reliable access to care means that both population immunization levels and communicable disease rates are likely to be worse than they otherwise would be if everyone in the United States had health insurance. For example, underimmunization of children increases the vulnerability of entire communities to outbreaks of diseases such as measles, whooping cough, and rubella (IOM, 2000). Because uninsured families and children tend to live in neighborhoods with higher-than-average uninsured rates and are likely to go without immunizations, all who live in these communities are at greater risk.
Another consequence of community uninsurance may be a greater risk of the transmission of the virus that causes HIV/AIDS especially for members of groups that are already at greater risk for becoming infected. Almost 20 percent of all persons with HIV infection are uninsured and they tend to experience greater
difficulties in obtaining access to timely and appropriate care (Sorvillo et al., 1999; Kates and Sorian, 2000; IOM, 2002a). Persons who are HIV positive and uninsured are also more likely to be unaware of their infectious state than are seropositive persons with health insurance, either public or private (Bozzette et al., 1998).
SUMMARY
The Committee draws two conclusions based on its expert judgement and the sufficiency of the evidence base.
-
A community’s high uninsured rate has adverse consequences for the community’s health care institutions and providers. These consequences reduce access to clinic-based primary care, specialty services, and hospital-based care, particularly emergency medical services and trauma care.
-
Research is needed to more clearly define the size, strength, and scope of adverse community effects that are plausible consequences of uninsurance. These include potentially deleterious effects on access to primary and preventive health care, specialty care, the underlying social and economic vitality of communities, public health capacity, and overall population health.
What we don’t know can hurt us. There is much that is not understood about the relationships between health services delivery and financing mechanisms and even less about how the current structure and performance of the American health care enterprise affect communities’ economies and the quality of social and political life in this country. Because policy makers and researchers have not asked or examined these questions through comprehensive and systematic research and analysis, there is a limited body of evidence of mixed quality on community effects.
The Committee believes, however, that it is both mistaken and dangerous to assume that the prevalence of uninsurance in the United States harms only those who are uninsured. It calls for further research to examine the effects of uninsurance at the community level but nonetheless believes there is sufficient evidence to justify the adoption of policies to address the lack of health insurance in the nation (Corrigan et al., 2002). Rather, the call for more research is to say that, as long as we as a nation tolerate the status quo, we should more fully understand the implications and consequences of our stalemated national health policy.