EXECUTIVE SUMMARY
Umbilical cord blood, like bone marrow and mobilized peripheral blood, is rich in potentially life-saving stem cells called hematopoietic progenitor cells (HPCs). When they are transplanted, HPCs are effective for the treatment of blood disorders (e.g., leukemia, selected metabolic disorders and immunodeficiencies, and sickle cell anemia) and in recent years have been transplanted to more than 25,000 people in the United States alone. Increasingly, these transplants are performed with HPCs derived from cord blood.
Recognizing the need for a national system for the collection, distribution, and use of cord blood, the U.S. Congress asked the Institute of Medicine to review the options for such a system and to make recommendations on the ideal structure of a national program.
In its considerations, the committee was guided by two overarching goals: (1) easing access to timely, complete, and accurate information on the HPCs available from cord blood donors at the time that the physician is making the decision about the transplant, and (2) ensuring the best possible quality of the cord blood units that were to be used by patients.
The committee reviewed the available data and conducted original analyses of the data collected by the National Marrow Donor Program (NMDP), The National Cord Blood Program of the New York Blood Center (NYBC), and the Cord Blood Banking and Transplantation (COBLT) study of the National Heart, Lung,
and Blood Institute. The analysis confirmed the hypothesis transplants matched with the recipient for four of six human leukocyte antigens (HLAs) is not as effective those matched at six of six antigens. The study also demonstrated that, with increased cell dose, a five of six match has survival rates almost identical to that of a six of six match.
The committee proposes the creation of a National Cord Blood Stem Cell Bank Program. The committee makes specific recommendations for the organization and administration, data management, and quality control in the national program that would best serve the needs of both the donors and the patients requiring stem cell transplants.
Stem cells, a primitive type of cell found in all animals, are capable of both self-renewal and differentiation into more specialized cells. These capacities offer great potential for regenerative medicine. This report recommends the development of an integrated system for the therapeutic use of one specific type of stem cell found in humans, the hematopoietic progenitor cell (HPC), which is a multipotent stem cell responsible for the continual production of the diverse array of normal blood cells. Because of the potential of HPCs to reconstitute bone marrow and peripheral blood, they have been used for the treatment of patients with bone marrow damage from either chemotherapy or underlying hematological failure for several decades.
HPCs can be obtained from a variety of sources including bone marrow, mobilized peripheral blood, and umbilical cord blood collected from the placentas of recently delivered infants. HPCs obtained from cord blood appear to have some advantages over HPCs obtained from bone marrow or peripheral blood. Among them, immune cells from umbilical cord blood are less mature1 than those from other sources, so their transplantation results in a lower risk of graft-versus-host disease, a common immune response to transplantation that can be fatal. In addition, cord blood is readily available, carries a low potential for infectious disease transmission, and involves minimal risk to the mother or the infant at the time of collection.
Because of these advantages over bone marrow, cord blood has the potential to be an excellent resource, opening up the possibility of transplantation to patients who either can not find a human leukocyte antigen (HLA) match within the bone marrow donor pool, or who are too ill to be able to wait for the sometimes lengthy process of searching and then har-
vesting bone marrow from living adult donors. By increasing both the size and quality of the cord blood inventory, nearly 90 percent of all patients who need a transplant should be able to find a suitable HLA match in either the marrow or the cord blood inventories.
Over the past few decades, HPCs obtained from cord blood have been shown to be a suitable alternative to adult bone marrow or peripheral blood in transplants for the treatment of leukemia, lymphoma, aplastic anemia, and inherited disorders of immunity and metabolism. Additional research is required to clarify whether cord blood is as good as or superior to other HPC sources in all of these situations. Factors already shown to influence the outcome of cord blood transplantation include the number of HPCs in the unit of blood, the body size of the transplant recipient, and the degree of HLA mismatch between the donor and the recipient, which increases the likelihood of a poor transplant outcome.
IN SEARCH OF A MATCH
An appropriate HLA match is important for all types of HPC transplantation, regardless of the graft source. The number of patient candidates for an HPC transplant is estimated to be 11,700 annually; of those, only a small percentage have an HLA-identical living sibling donor, generally considered the best HPC source. In an attempt to make HPCs more widely available to the large number of patients who do not have an HLA-identical sibling, large international volunteer adult (bone marrow and peripheral blood) donor registries were created in the 1980s. Today, more than 9 million registered adult donors are listed in more than 40 registries worldwide. However, despite the large numbers of adult donors recruited over the past two decades, registries and transplant physicians still face several challenges, including:
-
an inability to identify fully or closely matched HLA donors for a significant proportion of transplant candidates, particularly non-Caucasian individuals;
-
permanent or transient unavailability of some potential donors, even if that individual was identified in a registry on the basis of HLA match;
-
the prolonged interval between the time of a search request and the time of HPC acquisition (the currently reported median time is greater than 4 months); and
-
risks associated with bone marrow and peripheral blood donation.
Several groups have recognized that larger and more accessible cord blood collections could resolve several of these issues, in part, because of the relative ease and safety of acquisition of cord blood and the potential to
obtain cells from a broad cross-section of the population and the ability to have successful transplant outcomes with a somewhat greater degree of HLA mismatch than with adult HPCs. As a result, at least 40 cord blood banks exist at present in the United States. Of these, approximately half store donations for use for transplantation between unrelated donors. These cord blood units are typed and stored anonymously for use by any patient who might have a medical need for them. The remaining banks are private banks, meaning that they store cord blood at the expense of the donor’s family for potential future use only by the donor or a member of the donor’s family. Such use could be allogeneic (i.e., for someone else), to treat a sibling of the donor, for example, or it could be autologous, meaning that the cord blood cells would later be used to treat a condition in the child from whom the cord blood originally was obtained.
THE CHALLENGES OF A FRAGMENTED SYSTEM
The proliferation of cord blood banks has raised questions related to accessibility; the adequacies of the cord blood inventories; the standardization of cord blood collection, processing, and storage methods and documentation; and quality control. Although independence can lead to innovation, it can also lead to inconsistency in cord blood quality from bank to bank, and the need for transplant centers to use different methods of accessing, thawing, and processing units received from different banks. In addition, most banks have developed practices and procedures independent of any consistent quality assurance or regulatory oversight, although many banks are accredited by independent organizations.
The lack of a single outcomes database has thwarted the scientific community’s ability to determine best practice guidelines. Currently, outcomes are tracked by individual cord blood banks with varying degrees of success, dependent on resources and transplant center compliance. Furthermore, absence of a standard search format, differences in levels of HLA typing from bank to bank and between cord blood and adult donor registries, and the requirement for multiple searches to independent cord blood banks or consortia of cord blood banks at least in part reflects the fragmentation of the system. Reflecting the desires of the end user transplant centers, some aspects of the search process have become more uniform over time. However, other hindrances still exist—most notably, the lack of access to all transplant data.
Recognizing the potential contributions of umbilical cord blood transplantation and the need for a system that better serves patients, in the 2004 appropriations bill for the U.S. Department of Health and Human Services (DHHS), the U.S. Congress provided $10 million for the establishment of a National Cord Blood Stem Cell Bank Program under the leadership of the
Health Resources and Services Administration (HRSA). Although there is agreement on the need for a national program, there are major differences in perspectives as to how this goal might be accomplished with regard to governance, database management, unit selection processes, sources of material, financing and competition, standards, and other issues.
BACKGROUND OF THIS STUDY
The Congress’s 2004 $10 million appropriation for the establishment of a National Cord Blood Stem Cell Bank Program recognized the different views on how such a program might be established. A portion of that appropriation was allocated to the Institute of Medicine (IOM) to provide HRSA with an assessment of existing cord blood programs and inventories and to make recommendations on the ideal structure, function, and utility of a National Cord Blood Stem Cell Bank Program. The charge to the IOM committee is as follows:
In response to Conference Report on H.R. 2673, Consolidated Appropriation Act 2004 (H. Rept. 108-401), IOM will assemble a committee of experts to conduct a study that will consider relevant issues related to the establishment of a National Cord Blood Stem Cell Bank Program within HRSA. The IOM study will make recommendations for the optimal structure for the cord blood program and address pertinent issues related to maximizing the potential of this technology (e.g., collection, storage, standard setting, information sharing, distribution, reimbursement, and research and outcome measures).
The following are among the more specific issues that the committee was asked to consider:
-
What is the role of cord blood in HPC transplantation in the context of other sources of HPCs?
-
What is the current status of the cord blood banks already in existence?
-
What is the optimal structure for the cord blood program?
-
What is the current use and utility of cord blood for stem cell transplants?
-
What is the best way to advance the use of cord blood units for HPC transplantation (i.e., setting storage standards, collection procedures, information sharing, distribution, and outcome measures)?
-
What is the best way to make cord blood units available for research?
-
What consent procedures should be followed to obtain informed consent for both research and transplantation use?
-
Should the cord blood program set practice guidelines for all banks
-
or just the public banks (e.g., what kind of HLA-typing would need to be done before blood goes into the cord blood bank, and how are the databases advertised)?
The IOM formed the Committee on Establishing a National Cord Blood Stem Cell Bank Program, which consists of experts in the fields of economics, HPC transplantation, outcomes analysis, biostatistics, stem cell biology, cord blood quality and standards, public health, health technology assessment, patient advocacy, ethics, and obstetrics and gynecology.
RECOMMMENDATIONS
A national program should have as its primary mission the goal to maximize access to high-quality HPC sources for patient care and research in the most efficient, cost-effective, and ethical manner possible. All committee findings and recommendations were weighed against this core mission and were developed after careful consideration of current experience with cord blood banking, the lessons learned from other organ and tissue transplant programs, and the current and potential uses of HPCs derived from cord blood. In the course of its work, the committee made extensive efforts to consider all points of view on the establishment of a national program. In the committee’s view, the major parties interested in a successful cord blood program agreed on several key goals for a national program, including:
-
Simplicity. A national program needs to avoid duplication of effort in terms of both the services provided and the steps necessary for a transplant center to access appropriate graft sources.
-
Quality. The ultimate goal of a program should be to promote the best possible chance of patient recovery by establishing an inventory of high-quality, HLA-diverse, cord blood units.
-
Patient, physician, and donor support. Support and education for all individuals involved in the program is an integral and necessary part of the program.
With these goals in mind, the committee developed recommendations to improve the operations of cord blood banks and banking procedures, ensure adherence to ethical standards, move toward an optimal inventory of cord blood units for a national program, create the structure and organization for a national program, and facilitate research in this area. In addition, oversight will be an important component of the functioning of a national program. In its recommendations on the structure and organization of a national program, the committee recommends that the Secretary
of DHHS establish a National Cord Blood Policy Board to set policy and advise the Secretary of DHHS and HRSA on policy regarding the donation, collection, and uses of cord blood, as well as on the research needed to improve and augment the uses of HPCs. Thus, several of the recommendations rely on the establishment of the structure proposed in Recommendations 7.1 to 7.6 (see below).2
Banks and Banking
Centers that collect, process, and store cord blood differ in their organization and governance as well as in their processing methods. When physicians attempt to access units for patients, they confront different search algorithms and informatics systems, depending on which bank or network of banks they search. Likewise, HLA typing requests might come to banks in different formats on the basis of different transplant center preferences.
Some federal and state laws and regulations govern the operation of cord blood banks, and many are accredited through one organization or another. Yet these rules and regulations are not standardized, and a more consistently applied set of standards would benefit both the cord blood banks and the end users. In addition, Food and Drug Administration (FDA) licensure of cord blood units will go a long way toward providing another layer of safety and quality assurance in the system and has the added benefit of creating requirements that are enforceable by law.
In addition, a single, uniform accreditation system for the evaluation and inspection of cord blood banking facilities is needed to ensure the safe and effective collection and storage of cord blood units for transplantation. Centers performing cord blood transplants should also be accredited to ensure the proper selection and thawing of cord blood units. FDA licensure of cord blood units is another means by which uniformity and high standards can be met. The committee believes that the interests of all parties would best be served if all banks, whether they are public or private, were to be licensed and were to adhere by these standards.
Finally, a particularly important barrier to the fundamental goal of unimpeded access to treatment is the fact that units in existing cord blood collections lack sufficient ethnic and racial diversity. This limits the availability of HLA types for some groups of potential recipients and indicates a need for even greater outreach to underrepresented populations to donate cord blood and for the development of innovative approaches to donor recruitment, recognizing that a deficiency in the representation of certain
ethnic populations within cord blood inventories is due to many factors and not just recruitment.
Recommendation 4.1: Identify a Cord Blood Accrediting Organization. The Health Resources and Services Administration should identify a Cord Blood Accrediting Organization by means of an open, competitive request for proposal process. This organization should be charged with the delineation of standards for any cord blood bank, collection center, or transplant center desiring to participate in the National Cord Blood Stem Cell Bank Program.
Recommendation 4.2: Establish Uniform Standards for Cord Blood Collection. Uniform standards for the collection of cord blood units without alteration of safe obstetrical practice should be established by the Cord Blood Accrediting Organization suggested in Recommendation 4.1 and should be required of all banks participating in the National Cord Blood Stem Cell Bank Program.
Recommendation 4.3: Establish Uniform Quality Assurance Systems. Uniform quality assurance standards and criteria should be established by the proposed Cord Blood Accrediting Organization for the collection, processing, and storage of cord blood, and adherence to these standards should be required of all banks participating in the National Cord Blood Stem Cell Bank Program. In addition, a system for the frequent performance of compliance reviews should be established
Recommendation 4.4: Establish FDA Licensure of Cord Blood Units. The Food and Drug Administration should move promptly to establish a system of licensure of cord blood units intended for clinical transplantation. As an interim measure until a licensure process is established, all banks participating in the National Cord Blood Stem Cell Bank Program should operate under an investigational new drug application.
Recommendation 4.5: Apply Quality Standards to All Banks. The committee strongly recommends that all cord blood banks, regardless of public or private status or participation in the national program, adhere to the established quality standards.
Ethical and Legal Issues
The issues associated with the collection, storage, and use of tissue for transplantation are technical and medical, as well as ethical and legal. Donors of cord blood are not just depositing leftover byproducts of the birth process with interested researchers and physicians; rather, they are making a choice to do something that may potentially benefit another person. Some major questions the donor must fully comprehend before she
consents to donate cord blood include who has access to the cord blood unit once donated, where it will be stored, how it will be stored, how her privacy will be protected, and whether the donor stands to gain from the donation (e.g., by a future transplantation for herself or members of her family), or be harmed by the donation (e.g., subsequent discovery of information relevant to the health of the woman or her child).
Pregnant women receive a great deal of information—sometimes conflicting—about the donation process and the consequences of different types of banking. It is crucial to disclose several kinds of information to the potential donor, including who has access to the cord blood once it is donated, where it is stored, how it is stored, and how the donor’s privacy is protected.
Recommendation 5.1: Cord Blood Centers Need Policies Regarding Who Must Provide Consent. Cord blood collection centers should have clear policies about who must provide consent for donation and a plan to address paternal objections to the donation of cord blood.
Recommendation 5.2: Informed Consent Should be Obtained Prior to Labor and Delivery. Informed consent for the collection, storage, and use of cord blood should be obtained before labor and delivery, and after the adequate disclosure of information.
Recommendation 5.3: Donors Must Be Provided with Clear Information about their Options. The information provided to a donor must include a balanced perspective on the different options for banking. The information disclosed for allogeneic donation should not include language that gives the donor an impression that the unit will be available to the family after donation.
Recommendation 5.4: Promote the Security of Medical Information. Secure links between the medical records of the donor and the banked cord blood unit must be established to ensure the safety of transplantable products and the patients receiving the transplants. These records must be kept confidential and afforded the full protection of the law. If an abnormality is discovered during testing, the results must be delivered to the donor in a manner that is appropriate in relation to the severity of the abnormality.
Recommendation 5.5: Cord Blood Donors Must Understand the Limitation of their Rights. Those who collect cord blood for public banks should disclose to potential donors all possible clinical and research uses of the cord blood, and furthermore, that donation will terminate a prospective donor’s ability to direct the use of the cells.
Establishing a National Inventory
One of the largest unresolved issues in the establishment of a national cord blood program is determining how many units are needed at the national level and establishing a mechanism for projecting or estimating the need for cord blood on a continuing basis. On the basis of preliminary analyses of all existing outcome data and an economic analysis of the costs and benefits of various inventory sizes, the committee made preliminary estimates of an efficient inventory size. The committee estimates that at least an additional 100,000 new, high-quality cord blood units are needed in the national inventory. As more data are collected and as HLA match probabilities and relationships between HLA mismatch and cell dose and outcomes are reevaluated, the final inventory size will need to be determined by the proposed national oversight board (see Recommendation 7.1 below.) It is important that the determination of the final inventory size take into account clinical, policy, and economic interests.
To more clearly assess the relationship between HLA matching and the inventory size, the committee conducted its own outcomes analysis using data available from NMDP, the New York Blood Center, and the Cord Blood Banking and Transplantation study conducted by the National Heart, Lung, and Blood Institute. The committee found that a strong relationship between outcomes and both the degree of matching and the cell dose3 in a cord blood unit, and that with a cell dose greater than 2.5 × 107 nucleated cells per kilogram of body weight needed to ameliorate the negative effects of transplanting units with one or two HLA mismatches.
Recommendation 6.1: Establish a National Inventory Policy. Forecasts of the required size of a national inventory of cord blood should be based on the principles of efficiency and equity for identifiable groups of patients. The program should regularly examine data on:
-
ways in which increases in cord blood inventory would benefit the length and the quality of life among potential transplant recipients;
-
the benefits and costs per unit for identifiable groups of patients; and
-
the effects of inventory policy on the financial viabilities of hematopoietic progenitor cell collection, storage, and distribution systems for HPCs.
These assessments should be used by the National Board to respond to changes in need, indications, and technology for hematopoietic progenitor cell transplantation and future applications for cord blood cellular therapy.
Recommendation 6.2: Continue to Conduct Outcomes Research. The Health Resources and Services Administration and the National Institutes of Health should support further research directed toward understanding the relationships among inventory size, human leukocyte antigen match quality, cell dose, multiple-unit transplants, and the benefits of hematopoietic progenitor cell transplantation to the length and quality of life.
Recommendation 6.3: Expand the Current Inventory. Because an increased inventory size would increase the potential benefits of transplantation, the Health Resources and Services Administration should support inventory growth while it assesses the current inventory and establishes the optimal size of a cord blood unit inventory.
The characteristics of existing units must be re-evaluated for their acceptability for transplantation by simultaneously considering both the cell dose and the degree of HLA match. The quality of the existing inventory should thus be reviewed in the context of the newly developed standards. As a result, it is likely that many existing units will be found unsuitable for clinical use based on low cell count or inadequate evaluation and storage. Resulting inventory policy should be flexible enough to support changes in the understanding of the HLA and cell-dose factors as well as evolving clinical practices (such as dual cord transplants), and should be re-evaluated on a regular basis. Finally, the current inventory should be assessed in the context of the global inventory; the harmonization of international standards will facilitate such an assessment.
Recommended Structure of a National Program
The committee’s central charge was to advise HRSA on how a National Cord Blood Stem Cell Bank Program should be structured. The committee believes that the primary goal of any structure that is created should be to provide transplant physicians the assurance that when they determine that an HPC transplant from an unrelated donor is appropriate, the process for locating the best available cells is accurate and timely; that the procured cells are of high quality; and that information on the clinical experience of the transplant recipient is subsequently collected for ongoing research, quality assurance, and clinical improvement purposes. It is clear to the committee that at present, cord blood banks operate under various standards, that the outcomes of a significant proportion of cord blood transplants are not reported either to the bank from which the unit was obtained or to the transplant community generally, and that the economic status of cord blood banking is fragile. The structure that is ultimately identified should address all three of these critical issues.
The committee was aware that current participants in cord blood collection, banking, and transplantation hold strong views about the ideal structure of a national program. In addition, the committee recognized that some activities or components of a comprehensive structure already exist (e.g., a good patient education and advocacy system). However, what is in place is not sufficient for either present or future needs, and the NMDP as currently structured would not be able to fulfill that role. While many aspects to be performed by the proposed National Cord Blood Stem Cell Bank Network have analogs in the NMDP not all U.S. and few non-U.S. cord blood banks participate in the NMDP network, and the procurement and banking of donated cord blood are processes very different from those used to recruit and track potential adult donors.
Finally, any structure identified now needs to be responsive to emerging knowledge about HPC transplantation and should have the capacity to adjust its procedures and structure as necessary and appropriate to incorporate that emerging knowledge.
From many perspectives, a single national system for all sources of HPC (whether they be adult bone marrow, adult peripheral blood, or cord blood) would simplify many aspects of the transplantation process, including search efforts, outcomes data collection and analysis, research, and policy making. There are, however, substantial differences in adult and cord blood registries, and unifying them in a single database requires much better understanding of the science behind the two graft sources.
The lack of a complete, coordinated network for accessing banked cord blood units, assessing the characteristics of those units, and evaluating the outcomes of transplants with units from various banks made it difficult for the committee to accurately assess the status and quality of the cord blood units available at present and their current use for transplantation. Given these considerations, the following are goals that the committee has sought to incorporate into the final structure of the network:
-
ensured clinical access to cord blood through substantial increases in the current inventory,
-
maximal efficiency of processes,
-
minimal redundancy of systems and investment,
-
guaranteed cord blood unit quality,
-
protected patient and donor confidentiality,
-
timely data collection and outcomes reporting,
-
transparent policies and procedures,
-
long-term financial viability of banks,
-
enhanced communication among all parties, and
-
adherence to ethical standards.
In moving toward the structure recommended by the committee (see below) and in meeting the associated goals of quality assurance, information exchange, and transparency, DHHS is urged to make transparent to the transplant community, banks, patients, and the public the process for establishing, implementing, and evaluating a national program. Table ES-1 illustrates the main functions of the cord blood program and the way in which the committee envisions that they will be fulfilled. More specific recommendations follow.
TABLE ES-1 Key Functions of a National Cord Blood Program
|
Governance |
A National Cord Blood Policy Board (the National Board) should establish policies and regularly monitor all issues related to cord blood uses. Day-to-day management should be done by a National Cord Blood Center, identified by HRSA through a competitive process. |
|
Database |
Data on both cord blood units available for transplantation and patient outcomes after the transplant are needed. As these two types of data serve different purposes, it is not necessary for them to be available in a single integrated database. |
|
Unit Selection |
The National Cord Blood Center should facilitate coordinated searches while allowing transplant centers to customize reports according to local selection practices and to work directly with cord blood banks. Search support should provide guidance or information on the selection of adult donor versus cord blood graft sources. |
|
Source of Transplanted Material |
The choice of the source for HPCs must be driven by the patients’ needs and the best available evidence about the different sources of material for transplantation. This evidence about uses of all sources of material for transplantation must be regularly updated and made available. |
|
Finances |
Federal funds for support of cord blood banking should be allocated to the expansion of the inventory of banked units with some funds reserved for the national infrastructure that will be needed. |
|
Cord Blood Bank Selection |
Banks wishing to participate in the National Cord Blood Program should meet the standards to be established by the National Board and must meet all data requirements of the national program. |
|
Standards |
Quality standards for banks, donor centers, and transplant centers will be set by an accrediting agency that is independent of the National Cord Blood Center. The accrediting agency will be chosen by a competitive mechanism. |
|
Outcomes Data |
The National Board should have ready access to comprehensive data that allow for analysis of all transplants in which HPCs are used and that can be used to establish the desired inventory size and readily update the policies of the National Cord Blood Program. |
Recommendation 7.1: Establish a National Cord Blood Policy Board. The Secretary of U.S. Department of Health and Human Services (DHHS) should establish a National Cord Blood Policy Board (National Board) to set policy and advise the secretary of DHHS and the Health Resources and Services Administration on policy regarding the donation, collection, and uses of umbilical cord blood, as well as on research needed to improve and augment the uses of the cells in cord blood. The National Board should routinely review outcomes data for all clinical uses of umbilical cord blood and develop policy on changes in inventory size, procedures, and standards, as experience and emerging science indicate. The National Board should ensure active interactions among the various organizations involved in adult donor peripheral blood and bone marrow transplantation and umbilical cord blood transplantation.
This new National Board should be established at the level of the secretary of DHHS to provide appropriate distance from the day-to-day concerns of HRSA, which is the agency directly responsible for managing the relationships between DHHS and adult donor and cord blood programs as well as allocating funding. The proposed board should be established as a chartered body subject to the requirements of the Federal Advisory Committee Act, such that the charter and all appointments would be publicly announced in the Federal Register and the meetings of the board would be open to the public. The National Board should include experts in cord blood transplantation; HPC collection, storage, and distribution; clinical transplantation; ethics; epidemiology; histocompatibility; statistics; informatics; health care services; and other relevant areas. In addition, the National Board should have representation from the public. Members of the board should, at a minimum, be free of financial conflicts of interest. The committee urges the board to play an active role in ensuring that the lessons learned during the development and growth of NMDP, the COBLT study, and the solid-organ transplant program are appropriately applied to all funding and policy decisions about the National Cord Blood Stem Cell Bank Program.
Recommendation 7.2: Establish a National Cord Blood Coordinating Center. The Health Resources and Services Administration should use an open, competitive process to establish and fund a National Cord Blood Coordinating Center (the Cord Blood Center). The Cord Blood Center would have day-to-day responsibility for carrying out the policies promulgated by the National Board, including:
-
managing a national network linking participating transplant centers with participating cord blood banks;
-
collecting data on the outcomes of subsequent cord blood transplants; and
-
ensuring that data regarding banked cord blood units and the outcomes of cord blood transplants are available to policy makers (including the National Board) for decision making, the participating banks and transplant centers for quality assurance purposes, and researchers seeking to better understand and expand the uses of cord blood.
In soliciting proposals for the Cord Blood Center, there should be no requirement that all of the program components be centrally managed, provided that satisfactory mechanisms for coordination are proposed, nor should the central management of all program components be prohibited. Some members of the committee are concerned that a requirement to force all aspects of cord blood transplantation into a single, central organization might slow the matching process and might stifle the creativity of the participating banks and transplant centers and their ability to search for improved practices. Proposals, whether for a central organization or not, should provide mechanisms for fostering meaningful links between and among transplant centers and banks, some degree of standardization, and providing access to the information needed for clinical decision making.
Figure ES-1 illustrates the relationships that the committee envisions under the governance structure described in these recommendations. The shaded portions of the diagram illustrate components that will have to be newly created, whereas the other portions represent existing components of the structure.
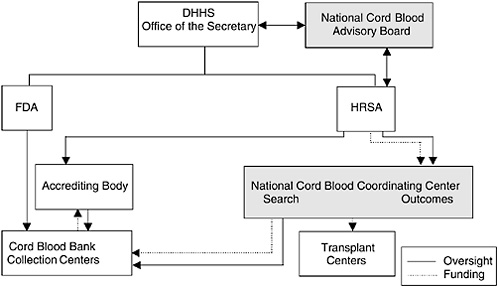
FIGURE ES-1 Proposed structure of a national program.
The National Board should set policy and the Cord Blood Center should perform its functions with the full recognition that cord blood, peripheral blood, and bone marrow are complementary alternative sources for HPCs. The source chosen must be driven by patients’ needs and anticipated outcomes on the basis of the best available evidence rather than on a priori selection of the source. Thus, every effort should be made to collaborate, as appropriate, with NMDP. The National Board must be vigilant to ensure that the Cord Blood Center operations are transparent to all involved and that cord blood is allowed to mature as a therapy complementary to adult sources of HPC.
Inventory Database and Unit Selection
The Cord Blood Center should work to facilitate the best possible methods for database searches, confirmatory HLA typing, and the reservation and selection of units on the basis of the best available evidence. These methods should include a format for the reporting of search results that provides a coherent summary of all units available through the national program and that incorporates flexibility to allow transplant centers to customize reports to meet the needs of local selection practices. For clinical purposes, a central database of all available units is not essential (but also is not precluded), as long as information on the total inventory available in all participating banks is accessible at the time of a search. The data system and policies should allow for individual participating transplant centers to work directly with participating banks, if they so desire. In addition, the Cord Blood Center should work to facilitate efficient access to units collected internationally so long as they fulfill the quality requirements set by the national system.
Outcomes Data
Recommendation 7.3: Develop an Outcomes Database for all Sources of HPCs. The National Board should support the development of an outcomes database that can guide decisions on inventory size and track cord blood bank quality and other policies as well as assist with the assessment of outcomes from all sources of hematopoietic progenitor cells.
Collection of outcomes data by the Cord Blood Center should follow a standardized format and capture the appropriate clinical information that is required by cord blood banks to meet their quality assurance, accreditation, and regulatory requirements. This might be achieved internally by the new Cord Blood Center or, perhaps more economically, by contracting with an existing organization having appropriate capacity. Any transplant center desiring to participate in the national program should agree to supply timely data on the immediate and long-term outcomes for patients
receiving cord blood units supplied by the national program. The format for this data-reporting process should be consistent with that used for adult donor transplantation and, to foster the development of an algorithm to allow for single source searching, a single outcomes database for adult and cord blood HPC transplants should be considered, building on existing efforts if possible. This information would not only ensure that complete data on the clinical outcomes following transplantation are collected, but it would also provide data to qualified researchers as well as policy makers and clinicians interested in overall analysis of both national adult donor and cord blood resources. Because these data requirements will impose a burden on the participating organizations, and because the collection and submission of high-quality data are time-consuming activities, some financial support will be needed to assist transplant centers with their data collection and data transfer activities.
Finances
Recommendation 7.4: Fund Banks to Promote Inventory Growth. The national program should provide the participating banks with the financial support that they need to achieve an inventory sufficient to provide as many potential recipients as possible with a high probability of a therapeutically effective cord blood unit when one is clinically indicated.
Expansion of the current inventory with units that meet established standards should receive the highest priority in the near future. The National Board should offer support to participating banks that are designing expansion plans for their inventories to include cord blood units from racially and ethnically diverse populations, thus enhancing access to cord blood for individuals who are members of racial and ethnic minority groups. Participating banks should be reimbursed for the units supplied for transplant through health care payment systems in a manner that allows them to be self-sufficient.
Recommendation 7.5: Provide Financial Support for Infrastructure Development. Some portion of the funds dedicated to the establishment of the national program should be reserved to support the infrastructure described in this chapter.
The national program will require an infrastructure that includes quality assurance and accreditation systems, as well as the Cord Blood Center and the National Board. The ongoing program of accreditation of participating centers should be supported through participant fees. To ensure that the available cord blood units are used to the greatest advantage for patient care, federal funds should be provided for start-up and ongoing costs for the development of mechanisms for the sharing and publication of out-
comes data; verification that the participating banks and transplant centers meet quality assurance standards; and the encouragement of innovation and improvement in banking, matching, and related processes.
Cord Blood Bank Selection
Recommendation 7.6: Establish Criteria for Data Sharing. The National Board should establish minimum criteria for quality standards and data sharing for banks participating in the national program. The Cord Blood Center should monitor and manage the implementation of those standards and coordinate a competitive process for the distribution of funds to qualifying banks for inventory growth.
Banks should be selected on the basis of published criteria and demonstration of the quality of their operations (e.g., accreditation and licensure). Although international banks should not be eligible to receive federal funds for inventory expansion, they should be encouraged to participate in other aspects of the program including data sharing and the provision of clinician and patient support.
Standards
Quality standards for participating banks, collection sites and centers, and transplant centers should be established and overseen by an accreditation body, which should be independent of the Cord Blood Coordinating Center and should be identified through a competitive process open to the several existing groups as well as any other group(s) that may emerge and that may be chosen by an expert panel. Only accredited banks and transplant centers should be able to participate in the National Cord Blood Stem Cell Bank Program. As recommended above (Recommendation 4.4), Food and Drug Administration licensure of units should be required of any bank participating in the national program.
Research
Recommendation 3.1: Develop a Mechanism to Make Nonclinical Units Available for Research Use. Federally funded umbilical cord blood banks should have a mechanism by which they can make available for research use units not appropriate for clinical use according to the priority standards developed by the National Cord Blood Policy Board proposed by the committee.
Further research is needed to better understand the therapeutic potential of cord blood.
|
BOX ES-1 Research Develop a mechanism to make nonclinical units available for research use (Recommendation 3.1). Umbilical Cord Blood Banks and Banking Establish a cord blood accrediting organization (Recommendation 4.1). Establish uniform standards for cord blood collection (Recommendation 4.2). Establish uniform quality assurance systems (Recommendation 4.3). Establish FDA Licensure of Cord Blood Units (Recommendation 4.4). Quality standards should apply to both public and private banks (Recommendation 4.5). Ethical and Legal Issues Cord blood centers need policies regarding who must provide consent (Recommendation 5.1). Informed consent should be obtained prior to labor and delivery (Recommendation 5.2). Donors Must Be Provided with Clear Information about their Options (Recommendation 5.3). Promote the security of medical information (Recommendation 5.4). Cord blood donors must understand the limitation of their rights (Recommendation 5.5). Inventory of a National Cord Blood Stem Cell Bank Program Establish a national inventory policy (Recommendation 6.1). Continue to conduct outcomes research (Recommendation 6.2). Expand the current inventory (Recommendation 6.3). Recommended Structure of a National Program Establish a National Cord Blood Policy Board (Recommendation 7.1). Establish a National Cord Blood Coordinating Center (Recommendation 7.2). Develop an outcomes database for all sources of hematopoietic progenitor cells (Recommendation 7.3). Fund banks to promote inventory growth (Recommendation 7.4). Financially support infrastructure development (Recommendation 7.5). Establish criteria for data sharing (Recommendation 7.6). |



















