5
Expanding RECA Eligibility: Scientific Issues
The committee was charged with making recommendations to the Health Resources and Services Administration (HRSA) that are based on scientific knowledge and principles:
whether other classes of individuals or additional geographic areas should be covered under the Radiation Exposure Compensation Act (RECA) program.
The present criteria for downwinder eligibility include diagnosis of a compensable disease and proof of residence in selected counties of Arizona, Nevada, and Utah during the period of atmospheric testing at the Nevada Test site (NTS) (see Map 2.2). The committee reviewed the criteria and compared them with those of other compensation programs related to radiation exposure (Chapter 2, Table 2.4). This chapter describes a process for expanding geographic areas for coverage of people who may have been exposed to radiation from fallout from US nuclear-weapons testing that is based on diagnosis of disease and on scientific methods to determine the extent to which radiation was responsible for the disease. The objective is to suggest a process that would not take an inordinately long time to develop and implement.
In an attempt to identify an appropriate way to consider geographic areas for compensation of people who may have been exposed to radiation from fallout from US nuclear-weapons testing, the committee began evaluating the current system of eligibility on the basis of residence alone. One method that the committee used was to estimate the absorbed dose of radiation for populations living in affected areas surrounding the NTS. People can be exposed to radiation from
fallout by many pathways including external radiation as a plume or cloud passes over the region, external exposure to radioactivity deposited on the ground and remaining there for extended periods, and internal exposure to radioactivity that accumulates in the body from inhalation or ingestion of plants, meat, and milk.
A collection of data is available to map exposure rates across the United States from radioactivity deposited on the ground as a result of fallout (NCI, 1997). Analysis of the data has revealed that doses from external radiation to radiosensitive tissues are small and, in all but a few cases, not significantly greater than those from natural background radiation (CDC-NCI, 2001).
The most important pathway is the ingestion of iodine through the consumption of milk (NCI, 1997). Iodine is absorbed rapidly in the gastrointestinal tract and almost completely transferred to the blood through the small intestine. Of the iodine in the blood, about 30% is transferred to the thyroid, and the remainder is eliminated by excretion. Stable iodine in the thyroid is reduced by 50% in approximately 120 days. The isotope iodine-131 (131I) has a radioactive half-life of 8 days. Thus, more than 90% of the atoms of 131I taken up in the thyroid will decay there. Beta particles from that decay deliver a substantial dose to the thyroid.
There has therefore been an extensive effort to determine the dose to populations from 131I originating in the atmospheric weapons-testing program at the NTS. The decade-long effort has produced a dose calculator that can conveniently be used to estimate the dose to a person on the basis of age, location, and milk consumption (NCI, 1997) (http://ntsi131.nci.nih.gov/).
We have used the calculator to provide information that might be useful in identifying geographic areas in the continental United States that might be eligible for compensation through RECA. To begin the process, we created an imaginary person. The person was a male born on January 1, 1948, who remained in a single county throughout the testing period. He consistently drank one to three glasses of processed milk from local dairies. We computed the total dose to the person’s thyroid. We repeated that process for every county in Utah. Several counties with sufficient fallout data were subdivided into regions, and we performed the dose calculation for each region separately. Figure 5.1 shows the results of our calculations. Each circle represents the computed dose for a specific county or sub-county region in Utah. The counties on the X axis are arranged from the highest thyroid dose to the lowest.
The variation in dose is large, ranging from 30 mGy for the lowest value in Iron County to 210 mGy in Washington County.
We assumed that the person was diagnosed with thyroid cancer some time after the testing at the NTS stopped. We then determined whether he was eligible for compensation through RECA. The solid circles in Figure 5.1 represent counties where he would be eligible for compensation, and the open circles represent counties in which he would not. Some counties with relatively low doses are
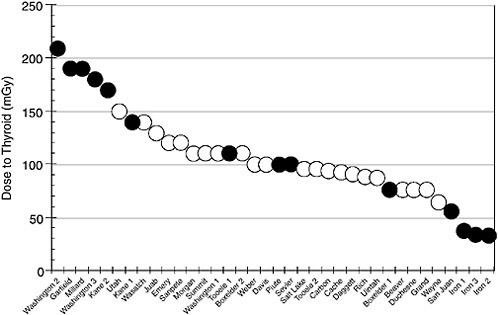
FIGURE 5.1 Calculated absorbed dose to the thyroid of a person born in 1948 who resided in same county in Utah for entire period of NTS testing.
included in RECA, and some with relatively high doses are not. That result leads to confusion and concern.
We repeated the computation with different persons of different ages and sexes. When plotted on a graph, the data were always similar to those in Figure 5.1. We then extended the computation to include counties is some states other than Utah. The results are shown in Figure 5.2. The solid circles represent counties in Utah where the person would be eligible for compensation through RECA. The open circles represent counties in the states listed.
This is not a comprehensive survey of all counties in the continental United States. It does however demonstrate that thyroid doses in other regions of the country can be greater that for counties currently eligible for compensation. We would expect similar results for other cancers, but have not made these computations because the dose calculators have not been thoroughly developed at this time.
That simple exercise does illustrate the problem one encounters when attempting to recommend extensions of RECA coverage for exposure to fallout. Doing so might well include counties throughout most of the United States. The committee also recognized that including absorbed dose in the determination of eligibility for compensation would not be sufficient because the risk of radiation-induced cancer depends on the age at exposure and age at diagnosis in addition to dose. A process based on risk would therefore use dose and the other criteria to
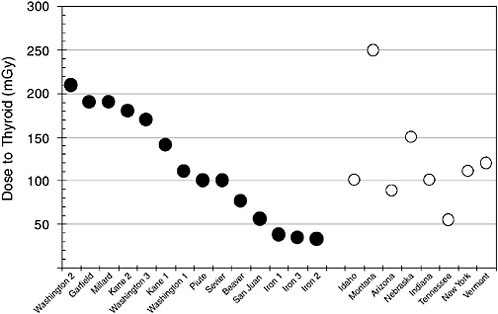
FIGURE 5.2 Calculated absorbed dose to the thyroid of a person born in 1948 who resided in same county for entire period of NTS testing. The solid circles are for counties in Utah that are currently eligible for compensation in RECA and the open circles are counties in states other than Utah.
determine the probability that an identified cancer was caused by radiation rather than by other agents.
The mandate before the committee involved scientific justification. One approach that is being used in other compensation programs, both in the United States and in the UK, is referred to as probability of causation (PC) or assigned share (AS). That approach has been reviewed extensively in the literature and has been used for tort litigation in many situations related to exposure to ionizing radiation. This chapter presents the history and implementation of PC in issues related to ionizing radiation. It defines PC in the context of compensation and presents examples that illustrate the process. Chapter 6 applies the PC process specifically to the task of expanding RECA eligibility.
PROBABILITY OF CAUSATION
Litigation for damages from ionizing radiation first became an issue after reports documented the hazards experienced by radium-dial painters (Martland, 1929). Many cases have since been adjudicated in the United States for medical, industrial, and environmental exposures to radiation. The problem faced by the legal system is that no specific form of cancer is caused only by radiation. Fur-
thermore, features of a cancer caused by radiation cannot be distinguished from those of the same cancer caused by other mechanisms. Legal decisions were often based on the opinions of experts who determined whether radiation was likely to be the cause of cancer in a particular person. That combination of circumstances created considerable controversy. In 1983, Congress instructed the National Institutes of Health (NIH) to develop data that would provide a scientific basis for determining whether a cancer diagnosed in a person was caused by a documented dose of radiation. The data were ultimately published in the form of tables that were entitled the probability of causation.1
The tables were based on information from epidemiologic studies of many groups of people. Technically, PC is the fraction of a group of identical persons in whom a radiation-induced cancer would be expected to occur at some specified time after a dose of radiation was received. In that sense, PC is a prospective concept applied to a population. In practice, however, PC is applied to a single exposed person in whom cancer has already been diagnosed; that is, it is used retrospectively. It has been suggested that the term “assigned share” is more appropriate for that situation because the value of PC for a group has been “assigned” to an individual. It is therefore the individual’s “share” of the total cancer risk due to radiation (NIH, 1985). PC and AS are numerically the same. The committee has adopted the nomenclature PC/AS for the purposes of this report. PC/AS is now widely used for claims against the government or its contractors in compensation programs such as Radiation-Exposed Veterans Compensation Act (REVCA) and Energy Employees Occupational Illness Compensation Program Act (EEOICPA).
Much of the information used to generate PC/AS for leukemias and solid tumors has been obtained from long-term followup of Japanese atomic-bomb survivors. Data on lung cancer resulting from exposure to radon decay products are obtained from studies of underground uranium miners. Estimates of the risk of thyroid cancer used for existing values of PC have been obtained, in part, from patients receiving diagnostic medical examinations involving the thyroid.
Risk-projection models are often required when information on specific doses is unavailable. In particular, that occurs for low doses of radiation when the spontaneous risk of cancer is at least as large as the risk of cancer from radiation. The models generally agree with a linear nonthreshold (LNT) hypothesis for radiation effects. They predict that there is some chance that a cancer will occur at any dose. The probability of occurrence is proportional to dose and does not reach zero until the dose is zero. Cigarette-smoking is the only other risk factor that is considered in the PC tables for radiation; it is applied only to the calculations for lung cancer.
A significant issue that needs to be addressed is how to choose a value of PC/AS that is accepted as “proof” that radiation was responsible for the diagnosed cancer in an individual. If the PC/AS has a value of exactly 0.5, it implies that it is as likely as not that the cancer was caused by radiation. For a PC/AS greater than 0.5, it is assumed that it is more likely than not that the cancer was caused by radiation. Most tort cases are based on a decision value of PC/AS equal to or greater than 0.5 (at least as likely as not that the cancer was caused by radiation). That criterion is discussed below, as are uncertainty in determining PC/AS and how uncertainty is incorporated into the decision-making process.
Definitions of PC/AS
If a person is exposed to radiation, the risk that a specific radiation-induced cancer will develop at a given age is referred to as Rrad. It depends on the absorbed dose to the organ, sex, age at the time of exposure, and age at the time of diagnosis. The risk that a specific cancer from all other causes will develop at the same age at diagnosis can be referred to as Rbaseline. Probability of causation, PC/AS, is defined as
(1)
In most cases, the risks posed by radiation must be obtained from risk-projection models based on epidemiology. For example, when a relative-risk (RR) model is used,
(2)
(3)
(4)
where RR is relative risk factor and ERR is excess relative risk factor (see Chapter 3).2 Useful relationships among PC/AS, RR, and ERR are
(5)
(6)
The relationship between PC/AS and ERR is plotted in Figure 5.3.
|
2 |
ERR is sometimes used only for a linear risk model. In this case, however, the committee is using it in its more general form, ERR = RR − 1, as discussed in Chapter 4. |
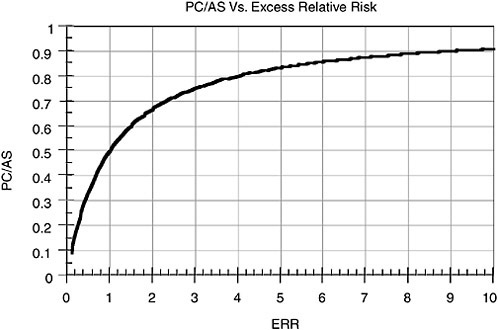
FIGURE 5.3 PC/AS as function of ERR. If excess risk from dose of radiation is 10 times baseline risk, PC is 0.91 (that is, 10/(10+1).
For example, suppose that a person receives an absorbed dose to the thyroid and is later diagnosed with thyroid cancer. Presume that the risk of developing thyroid cancer from that absorbed dose and the person’s age at exposure is found to be twice the baseline risk of thyroid cancer. Then
(7)
(8)
(9)
(10)
That leads to the intuitive result that if the risk added by radiation exposure is just equal to the baseline risk (ERR = 1), then there is an equal chance (PC/AS = 0.5) that the diagnosed cancer was caused by the absorbed dose from radiation in comparison with all other factors.
The process of obtaining PC/AS is in effect a process of determining the ERR for a person exposed to radiation and diagnosed with cancer. The determination of ERR for a particular person must rely on dosimetry to determine dose
and how the ERR depends on dose. Very often, the dose is not measured directly but is estimated through a dose-reconstruction process that relies on many assumptions. In addition, risk is modified by factors that depend on the type of radiation, the dose rate, age at time of exposure, and age when disease is diagnosed. Variations in baseline risk also depend on life style and socioeconomic factors.
All components used to estimate ERR have uncertainty. They are combined to form a probability distribution for ERR that reflects the combined uncertainty of all the components used to obtain ERR. Figure 5.4 is an example of a distribution of ERR.
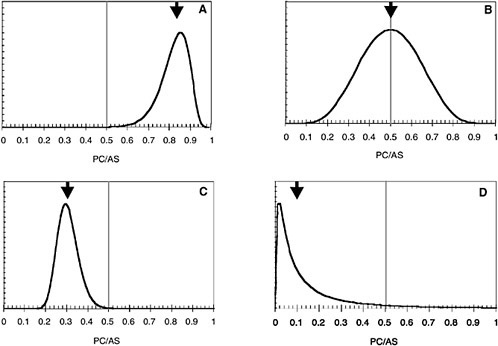
On Figure 5.4, the median value of ERR is 1.0 (half the estimates of ERR are smaller than 1.0, and half are greater than 1.0). The average value of ERR is 1.8, and there is a small chance that the ERR could be as high as 10. That distribution can be converted to a probability distribution of PC/AS by using the relationship shown in Equation 6. For illustration, several examples of the combined uncertainty (credibility) of PC/AS are shown in Figure 5.5. Each plot, A-D, is the resulting distribution of PC/AS obtained from different hypothetical situations for dose and risk.
Figures 5.5 shows that for any given case, the range of possible values can be very large. The arrow represents the median, or central, value of PC/AS (half the
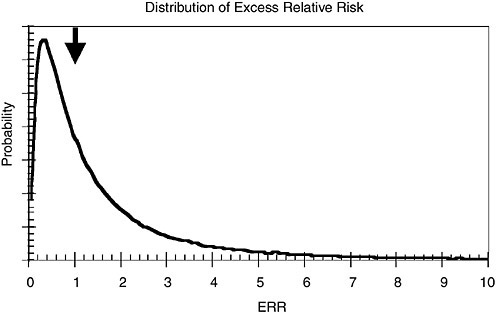
FIGURE 5.4 A probability distribution of excess relative risk, ERR resulting from uncertainties in estimates of the absorbed dose and associated cancer risks. Arrow indicates median value.
estimates are larger than this value, and half are smaller). The vertical line corresponds to a PC/AS of 0.5. If the true value of PC is greater than 0.5, it is more likely than not that the diagnosed cancer for this person was caused by radiation. The true value is not known exactly, so the graphs, including all the uncertainties, must be used to determine eligibility for compensation.
One possible criterion for awarding compensation under RECA is if the median value of the PC/AS distribution is equal to or greater than 0.5, that is, odds are at least 1 to 1 that the cancer was caused by radiation. For such a case, the persons represented by A and B in Figure 5.5 would be eligible, but the persons represented by C and D would not be eligible. Another possible criterion is a median value of the PC/AS distribution is equal to or greater than 0.2, that is, odds are at least 1 to 4 that the cancer was caused by radiation. For such a case, the persons represented by A, B, and C would be eligible, but the person represented by D would not be eligible.
A third possible criterion is whether some portion of the distribution exceeds 0.5. EEOICPA and the Department of Veterans Affairs (VA) award compensation if at least 1% of the distribution is greater than 0.5. In effect, only a small fraction of the right-hand tail of the distribution needs to exceed 0.5. In that case, the persons represented by A, B, and D would be eligible, but the person represented by C would not be eligible.
At first, one could conclude that using the 1% rule always gives the benefit of the doubt to the claimant. There are circumstances, as in D, where the average and the median values of PC/AS are small, but compensation is awarded because the uncertainty (the spread of the distribution) is very large. That often happens in the case of cancers where the association with radiation is not well established and the corresponding risk factors have large uncertainties. However, even though person C has a median value of PC/AS that is higher than person D, C would not receive compensation, because of the confidence that the true value of PC/AS is less than 0.5.
TOOLS FOR DETERMINING PC/AS
NIH Radioepidemiological Tables
The original radioepidemiological tables that ultimately served as a basis for determining PC/AS were mandated under Public Law 97-414, the Orphan Drug Act (NIH, 1985). A section of that law, pertaining to the development of radioepidemiological tables, was originally introduced by Senator Orrin Hatch (R-Utah) as a part of Senate bill S 1483, which became the Radiation Exposure Compensation Act. The tables were intended to provide a means for estimating the likelihood that a person who has or had any of several radiogenic cancers developed it as a result of exposure to ionizing radiation from the nuclear-weapons tests in Nevada.
The term radiogenic means that credible research has established a connection between exposure to radiation and an increased risk of the disease in human populations. In general, a radiation-induced cancer cannot be distinguished from the large number of similar cancers that are related to other causes. Public Law 97-414 required the US Public Health Service to develop radioepidemiological tables that set forth the relationships between PC/AS and radiation dose for various cancers. The main purpose of the tables has been to provide a mechanism for making decisions for compensation after exposure to ionizing radiation.
A committee of the National Research Council was formed to review the development of the radioepidemiological tables (NRC, 1984). The committee objected to the use of the term probability of causation and recommended the use of assigned share.3
An ad hoc working group of NIH developed the first radioepidemiological tables for estimating PC/AS in 1985. Its report (NIH, 1985) identified 13 different cancer sites that had statistical evidence of an association between absorbed dose and cancer in human populations.4
The final NIH report was issued in 1985 and has been used by VA as a guide to adjudicating compensation claims, through the Veterans Dioxin and Radiation Exposure Compensation Act, for cancers diagnosed in persons who were exposed during military service.
Tables Created by the Committee on Interagency Radiation Research and Policy Coordination
In 1988, the Committee on Interagency Radiation Research and Policy Coordination (CIRRPC) developed tables to be used in screening claims of radiation-induced cancer. The tables made extensive use of uncertainties in the values of PC/AS listed in the 1985 NIH report. A person passed the screening test when there was at least 1% probability that the estimated PC/AS exceeds 0.5. The CIRRPC report noted that
this procedure is designed to insure that cases which have even a small chance of a true PC that is 0.5 (50%) or greater (i.e., that meet the “at least as likely as not” criterion), are developed for assessment of causality, yet will avoid detailed development of those cases for which there is virtually no chance that the true PC would be as large as 50%.
Revision of the Radioepidemiological Tables
In 2003, a working group of the National Cancer Institute (NCI) and the Centers for Disease Control and Prevention (CDC) reviewed and updated the 1985 NIH radioepidemiological tables (NCI-CDC, 2003, available at http://dceg.cancer.gov/docs/Report03.pdf, accessed February 22, 2005.). Rather than publish a new set of tables, the working group developed the computer program Interactive Radio-Epidemiological Program (IREP 5.3), which can be used to estimate PC/AS with the revised radioepidemiological tables. The program incorporates the following revisions for the process of estimating PC/AS:
-
New incidence and mortality risk data.
-
Calculation of risk and AS for all ages at exposure starting at birth.
-
New cancer sites including some less strongly associated with radiation exposure.
-
New analytic approaches and ways to summarize data.
-
More attention to uncertainty and presentation of risk.
-
Use of organ-specific equivalent dose, in sievert (Sv).
The 2003 revision is based on two working assumptions: most types of cancer can, in principle, be induced by radiation; and the most important question is the magnitude of the risk associated with a particular exposure. In all, more than 25 cancers and groups of cancers are considered, including several cancer types not strongly associated with an absorbed dose of ionizing radiation. A list is shown in Table 5.1. The revised treatment of uncertainty included information from the original report and a more recent information (NCRP, 1996, 1997). Essentially, the method involves the calculation of a distribution of ERR similar to that shown in Figure 5.2 for a person in whom cancer has been diagnosed and who had been exposed to ionizing radiation.
The 2003 working group had access to expanded cancer-incidence data from atomic-bomb survivors participating in the Life Span Study being conducted by the Radiation Effects Research Foundation (RERF). Those data are not only more recent but based on more timely and accurate diagnoses of disease than were previously available from death certificates. Incidence data are also more relevant than mortality to compensation claims for cancers of delayed or low fatality. Direct access to RERF data allowed the working group to conduct its own analyses directed at the needs of that report, including modeling of dose-response modifiers, such as age at exposure, and including cancer types not strongly associated with radiation exposure.
The 2003 report is based on linear dose-response models for all solid cancers, which included dose and dose-rate reduction effectiveness factors (DDREFs) to allow for the possibility that risk per unit dose decreases with decreasing dose and dose rate. The 2003 report also treats the relative biological effectiveness
TABLE 5.1 Cancer Sites Covered by 2003 Radioepidemiological Program
|
Solid-cancer sites |
|||
|
|
1. |
Oral cavity and pharynx |
|
|
|
2. |
Digestive system |
|
|
|
|
• |
Esophagus |
|
|
|
• |
Stomach |
|
|
|
• |
Colon |
|
|
|
• |
Rectum |
|
|
|
• |
Liver |
|
|
|
• |
Gallbladder |
|
|
|
• |
Pancreas |
|
|
|
• |
Other digestive |
|
|
3. |
Respiratory system |
|
|
|
|
• |
Trachea, bronchus, and lung |
|
|
|
• |
Other respiratory cancers |
|
|
4. |
Bone |
|
|
|
5. |
Skin |
|
|
|
|
• |
Basal cell carcinoma |
|
|
|
• |
Other non-melanoma skin cancer |
|
|
6. |
Female breast |
|
|
|
7. |
Female genital |
|
|
|
|
• |
Ovary |
|
|
|
• |
Other female genital |
|
|
8. |
Male genital |
|
|
|
|
• |
Prostate gland |
|
|
|
• |
Other male genital |
|
|
9. |
Urinary system |
|
|
|
|
• |
Bladder |
|
|
|
• |
Kidney and residual urinary organs |
|
|
10. |
Nervous system |
|
|
|
11. |
Thyroid gland |
|
|
|
12. |
Other and ill-defined sites (residual solid cancers) |
|
|
Hematopoietic cancers |
|||
|
|
1. |
Leukemia, all types (except chronic lymphocytic leukemia) |
|
|
|
2. |
Acute myelogenous leukemia |
|
|
|
3. |
Acute lymphocytic leukemia |
|
|
|
4. |
Chronic myelogenous leukemia |
|
|
|
5. |
Lymphoma and multiple myeloma |
|
(RBE) of densely compared with sparsely ionizing radiation as an uncertain quantity. The 2003 report does not include chronic lymphocytic leukemia (CLL) as a radiogenic disease, because data at the time were insufficient to formulate a relationship. And it does not address the health consequences of in utero exposure to ionizing radiation.
The PC/AS for lung cancer associated with radon exposure is given separately from lung cancer associated with other types of exposure. The estimates of risk for radon-related exposures are based on an analysis of data from a report to the US Department of Justice in 1996 (DOJ, 1996). A more comprehensive analysis based on risk estimates published by the National Research Council (BEIR VI), was available at the time (NRC, 1999), but implementation of BEIR VI into a PC/AS framework would have required more computational and staff resources than had been available to the NCI-CDC working group.
Interactive Radio-Epidemiological Program (IREP version 5.3)
The 2003 NCI-CDC working group replaced the tabular format for probability of causation with IREP version 5.3. That program eliminates nearly all the computational labor of estimating PC/AS values and their uncertainties, but permits a more detailed and comprehensive expression of the various components of the calculation and their uncertainties.
IREP version 5.3 includes the updates in the 2003 NCI-CDC report. That version is accessible at the NCI Web site at http://irep.nci.nih.gov (accessed February 22, 2005). It enables the user to calculate the PC/AS for a particular cancer in a person exposed to a given dose of radiation and certain modifying factors such as the person’s age and sex. The PC/AS calculations are based on cancer-incidence data from the study of the Japanese atomic-bomb survivors and radon-induced lung cancer. The computer code allows consideration of uncertainty in an estimated dose and uncertainties in all the other items that enter into a calculation of PC/AS. The code computes the median (central estimate) of PC/AS value for a specified dose and the upper 95% and 99% percentiles of PC/AS, taking into account all uncertainties.
Implementation of IREP in Compensation Programs
The National Institute for Occupational Safety and Health (NIOSH) had adopted the 1985 NIH tables and added a few cancers to the original cancers, and it was using the results of earlier versions of IREP. It has now adopted the results of the 2003 NCI-CDC working group and is using the program NIOSH-IREP version 5.3, a modified version of the NCI-CDC code.
EEOICPA is using the modified version of the program prepared by NIOSH. The NIOSH version is accessible on the internet at http://www.niosh-irep.com/irep_niosh/, accessed
February 22, 2005. The original NCI-CDC version is maintained at http://irep.nci.nih.gov for archival and research purposes.
USE OF PC/AS IN ADJUDICATION
PC or AS has been used to adjudicate claims in the United States and the UK. The following sections summarize some of the situations in which it is used.
United Kingdom
In 1982, British Nuclear Fuels Ltd. (BNFL) and trade unions representing employees initiated a compensation program based on PC and cancer mortality. In 1987, the program was extended to cancer incidence. The program, which is voluntary and offered as an alternative to litigation, is now known as the Compensation Scheme for Radiation-Linked Diseases (CSRLD) and has been extended to UK nuclear electricity generators, the Ministry of Defense, and the Atomic Weapons Establishment (Wakeford et al., 1998).
Values of PC for the CSRLD are adapted from risk-projection models developed by BEIR V (NRC, 1990), which are based principally on the Life Span Study of the Japanese atomic-bomb survivors. The CSRLD covers all cancers except CLL, malignant melanoma of the skin, and Hodgkin’s lymphoma. Those cancers are excluded because there was no evidence of an association with radiation exposure. The CSRLD also excludes mesothelioma because it is associated almost exclusively with exposure to asbestos rather than radiation. Breast cancer and cancer of the digestive tract are included but are treated separately. There was a concern related to transferring risk estimates between populations in Japan and the UK for cancers that have different background rates in the two countries.
The CSRLD uses a sliding scale for compensation. Cancer victims with estimated values of PC/AS that are 0.5 or higher receive full awards. Persons whose estimates are between 0.2 and 0.5 receive graduated partial awards. The sliding scale is shown in Figure 5.6. Information posted on the CSRLD indicates that over 1,000 claims have been assessed. Compensation has been awarded to 97 claimants. Over half of the awards were for a PC/AS less than 0.5 (http://www.csrld.org.uk/html/scheme_history.php, accessed February 22, 2005).
Department of Veterans Affairs
In 1988, Congress passed PL 100-321, the Radiation-Exposed Veterans Compensation Act. Under that law, it is presumed that a veteran’s disease was caused by radiation if the veteran was present during a nuclear detonation regardless of the dose received. Thirteen radiogenic cancers were included in the list of presumptive diseases. A second regulation (38 CFR 3.311) governs diseases that are
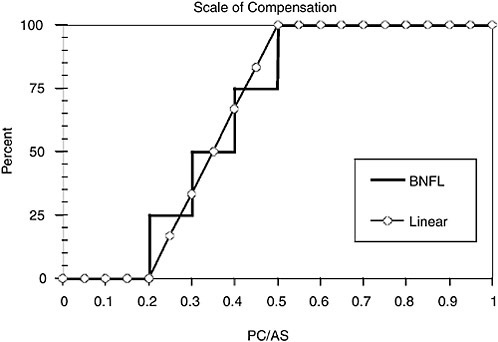
FIGURE 5.6 Percentage of full compensation based on PC/AS, (a) as used in the BNFL Compensation Scheme for Radiation-Linked Diseases (solid line) and (b) for a smooth linear scale (circles).
not presumed to be caused by radiation but could be associated with radiation if the dose was large enough.
VA has used the process developed by CIRRPC to evaluate claims (NRC, 2003b). CIRRPC produced tables that give the dose that would produce a PC/AS of 0.5 for various organs. To give the benefit of the doubt to the veteran, VA has chosen to use a threshold dose associated with a 99% credibility limit. At that dose, there is 99% confidence that the true PC is not greater than 0.5.
The PC/AS process is one of several tools in the medical decision process. It is not the only factor used in deciding whether a veteran with a nonpresumptive radiogenic disease receives compensation for service-connected exposures to radiation. However, the VA does not deny a claim if the PC/AS criterion is satisfied as long as all the other necessary conditions are fulfilled.
Department of Labor
Congress passed the EEOICPA in 2000 for persons who have worked for the Department of Energy or at any other facility involved in the development of nuclear weapons. In May 2002, the Department of Health and Human Services published its final rule on the guidelines to be used by the Department of Labor
(DOL) for determining whether a cancer included in an EEOICPA claim was caused by occupational exposure to radiation during nuclear-weapons production. DOL was advised to make such a determination by using a dose reconstruction provided by NIOSH and an estimate of PC/AS based on it. A person is eligible for compensation if DOL determines that the PC/AS was at least 0.5 (that is, at least as likely as not). Compensation is denied when there is a 99% chance that the estimate of PC/AS is less than 0.5 (that is, there is less than a 1% chance that PC/AS is at least 0.5).
APPLICATION OF PC/AS FOR FALLOUT FROM ATMOSPHERIC WEAPONS TESTING
This section presents a hypothetical example to illustrate the capabilities for determining PC/AS with existing tools and methods for a situation related to RECA. It involves thyroid cancer diagnosed in a person who was exposed to 131I from fallout. It shows how PC/AS is determined with user-friendly computer programs available on the Internet and developed by NCI. The process consists of two steps. The first step is a computation of the absorbed dose to the thyroid, and the second step is estimation of PC/AS on the basis of the dose and a diagnosis of cancer. The next section shows a sample calculation with Monte Carlo methods that demonstrate the procedures embedded in IREP.
For the hypothetical example, we consider a male born on January 1, 1951, in an area that received little fallout. On January 1, 1952, he moved to and lived in a location that received a large amount of fallout. He then returned to the original area on January 1, 1953. While in the high-fallout area, he consumed 1-3 glasses of milk a day.5 Thyroid cancer was diagnosed in 2004.
NCI Dose Calculator
The NCI calculator was used to estimate the absorbed dose to the thyroid from 131I (http://ntsi131.nci.nih.gov/, accessed February 22, 2005). The result was 0.32 Gy (32 rad), with a range of 0.032-5.2 Gy (3.2-520 rad). That 95% confidence interval can be approximated using a lognormal distribution with a geometric mean of 0.32 Gy (32 rad) and a geometric standard deviation of 4.0.
The next step was to determine PC/AS with IREP Version 5.3 at http://www.irep.nci.nih.gov/, accessed February 22, 2005. For simplicity, the small radiation doses incurred during residence at the location where the fallout was low have been ignored. Other input values supplied to the program are
-
An exposure in 1952.
-
Chronic exposure rate.
-
Radiation type—electrons with energy greater than 15 keV.
-
Organ dose lognormally distributed with a mean dose of 0.32 Gy (32 rad) and geometric standard deviation of 4.0.
The median value of PC/AS was 0.67, and this was assigned to the person. That value indicates that it is more probable than not that the thyroid cancer was due to radiation exposure.
Age at exposure is important in determining both the dose to the thyroid and the PC/AS of thyroid cancer from radiation exposure. In the above example, if the person had been born in 1931 rather than 1951 and all other information were the same (residence during 1952 and milk consumption of 1-3 glasses per day), the NCI dose calculator would yield a dose of 0.036 Gy (3.6 rad) with a range of 0.0037-0.65 Gy (0.37-65 rad). That result was considered to be a lognormal distribution of dose with a geometric mean of 0.036 Gy (3.6 rad) and a geometric standard deviation of 4.2. IREP would compute a median value of PC/AS of 0.04; it would be very unlikely that the thyroid cancer was related to the dose received from 131I in 1952.
We have also made an independent computation of PC/AS for the first scenario. We used data obtained directly from the NCI-CDC working group to compute ERR and used a Monte Carlo process to estimate the uncertainty (credibility limits). Details of the computation are presented in an annex to this chapter.
CONCERNS WITH USING PC/AS IN COMPENSATION PROGRAMS
Several authors, including those of the National Research Council 1984 committee and 2000 subcommittee reports, have pointed out various inequities that can arise in a compensation scheme that provides full payment to claimants with an estimated PC/AS greater than 0.5 but no payment to those with PC/AS less than 0.5 (NRC, 1984; NRC, 2000). For example, two people with cancer could have almost identical likelihood that their cancer was caused by exposure to radiation, but one applicant might have a PC/AS of 0.51 and the other a PC/AS of 0.49. If 0.5 were used as a bright line cut point, the first person would receive full compensation and the second none. A large difference in compensation at a single cut point does not recognize the large degree of uncertainty in the determination of PC/AS, and it assumes differences in PC/AS where statistically none exists.
Figure 5.5-D illustrates a situation where the estimated PC/AS has a wide credibility interval because of large uncertainties in estimated dose and the corresponding risk for a particular organ. For these situations, the true PC/AS might be very low, but the upper tail of the distribution could exceed established eligibility criteria.
A compensation scheme based on a sliding scale avoids that problem to some extent, in that people with PC/AS slightly below the value for full compensation would receive at least partial compensation. The 1984 National Research Council committee reviewed several alternative compensation schemes, including one in which compensation is proportional to PC/AS and another scheme in which full compensation would be received for PC/AS at least 0.5, no compensation for PC/AS is less than 0.1, and compensation scaled to PC/AS for values between 0.1 and 0.5 (NRC, 1984).
As noted above, the UK CSRLD has used a sliding compensation scale since 1982. That scale is not related linearly to PC/AS but has discontinuities at 0.2, 0.3, 0.4, and 0.5 (see Figure 5.6).
Robins and Greenland (1991) examined compensation procedures in which compensation is paid in proportion to PC/AS and compared them with a procedure in which compensation is proportional to years of life lost (YLL). They found shortcomings in both methods, but the YLL procedure had the advantages of being “robust” to model misspecification and “economically rational.” Payment schemes can be “potentially optimal,” and a scheme based on actual but unknown, biologic mechanisms and population heterogeneity is “truly optimal.” They define a payment scheme as robust if the average payment to a worker harmed by a radiation exposure equals the average payment under a truly optimal scheme. Schemes are economically rational if the total damages that a defendant pays equal the total damages assessed under a truly optimal scheme. Robins and Greenland (1991) concluded, however, that “in certain settings, payments in proportion to probability of causation might be preferred to payments in proportion to years of life lost for social, ethical and/or legal reasons.”
Robins re-emphasized several issues about PC/AS in a recent paper (Robins, 2004):
-
The PC/AS cannot be unambiguously calculated with epidemiologic data, because of the lack of knowledge of the underlying biological mechanisms of cancer.
-
PC/AS compensates only for the occurrence of a cancer; it does not completely account for the harm done to a person. For example, a person who dies from a compensable cancer at the age of 45 years suffers a greater loss than an individual dying from the same cancer at 70, but both would receive the same compensation.
-
PC/AS encourages counterproductive public-health practices. In the example of radiation workers, if the radiation dose and resulting risk is spread out over many people rather than over just a few, PC/AS values could be kept small, and no one would receive compensation. The collective dose to a group of workers could remain the same and in many cases increase. With a linear risk model, the total number of cancers may be the same or larger, even though none are compensable.
Robins suggested a two-step compensation scheme based on the total YLL of the group, which is independent of the actual distribution of YLL among the
people in the group. The program would first determine the total YLL of the group and set the compensation amount in proportion to that number. Then the distribution of compensation among the members of the group would be negotiated in some manner because it is not possible to determine the YLL for each member. That proposal could address the second and third issues noted above and optimize the response to the first one.
Other programs, as noted in previous sections, award compensation when there is at least a 1% chance (99% credibility limit) that PC/AS is greater than 0.5. That takes into account the uncertainty associated with PC/AS. The 2000 National Research Council subcommittee report criticized such an approach as favoring compensation for cancers whose connection with radiation is not well established (where the estimates of PC/AS have large uncertainties) over compensation for cancers that are clearly associated with radiation (NRC, 2000).
A similar concern could be applied to the estimation of dose. The absorbed dose to a person living far from a fallout monitoring station would typically have greater uncertainty than that of a person living closer to a station (NCI, 1997). If they contracted the same cancer and all risk factors were equal, the PC/AS of one might be 0.4 with 99% credibility limits of (0.35, 0.45), and that of the other might be 0.4 with 99% credibility limits of (0.25, 0.55). The first person would not be compensated, and the second would be because the 99% credibility limits included 0.5.
The National Research Council 2000 subcommittee recommended that the full probability distribution be taken into account. Although it did not recommend any particular compensation scheme, it suggested as an example consideration of schemes in which compensation is scaled according to the probability that PC/AS exceeds 0.5 or according to a direct function of the central value of PC/AS. The subcommittee also noted that the PC/AS method does not take degree of harm into account, in contrast with such a method as compensating according to YLL. It recognized, however, “that the current policy is grounded on the notion of AS, and we do not wish to discredit the efforts of the working group by implying that its estimates are not useful as a basis for resolving such claims, even in the face of fundamental problems of interpretation” (NRC, 2000).
CONCLUSION
The development of PC/AS was mandated by Congress to provide a more scientific basis for awarding compensation to persons who have been exposed to radiation and later have a diagnosed radiogenic disease. The concept is used in many compensation programs that involve radiation exposure. There is a well-documented infrastructure of tools and methods that has taken many years to develop.
The National Council on Radiation Protection and Measurements (NCRP) statement The Probability That a Particular Malignancy May Have Been Caused
by a Specific Irradiation (NCRP, 1992) concluded that PC/AS provided a logical procedure for addressing the issue of radiation-induced malignancy that had no other scientific or medical solution. It had the advantage that the process could be cast into a formula that would yield a figure of merit for the presumption of causation. A recognized limitation of the PC/AS approach was that population-based data were applied to individuals. That implies that a person has average susceptibility to cancer. PC/AS thus provides a probability, rather than proof of causation. It can, however, be tailored to individuals by using dose, sex, age at exposure, age at diagnosis, and type of malignancy.
The committee does not make specific recommendations on establishing a threshold value of PC/AS for compensation. However, we have compared several approaches to determine compensation on the basis of both point estimates of PC/AS and the entire distribution of PC/AS as illustrated in Figure 5.5 (see Table 5.2).
The first five schemes base compensation on point estimates of PC/AS. The term, PC/ASmed, represents the median, or central, value of the distribution. PC/ AS0.99 represents the upper tail of the distribution where there is a 1% chance that PC/AS exceeds this value. PC/ASdist represents the entire distribution estimated for a person. The last scheme uses the linear scale shown in Figure 5.6 weighted by PC/ASdist. That is to say, you compute the fraction of compensation for each value of PC/AS multiplied the probability that the person’s PC/AS might be this value and then sum up over all possible values of PC/AS from 0 to 1. This avoids the problem of selecting a single payment threshold value of PC/AS (vertical line in Figure 5.5) and eliminates the need to base the decision on a single point estimate of PC/AS for a person.
The committee has considered criticisms of the PC/AS approach. Alternative schemes also have serious shortcomings. They would require time and resources to develop for RECA. Implementation could lead to confusion and
TABLE 5.2 Examples of Compensation on the Basis of PC/AS Using Several Criteria with Distributions Illustrated in Figure 5.5
|
|
A (0.83) |
B (0.5) |
C (0.26) |
D (0.10) |
|
PC/ASmeda ≥ 0.5 |
100%b |
100% |
0 |
0 |
|
PC/ASmed ≥ 0.2 |
100% |
100% |
100% |
0 |
|
PC/AS0.99 ≥ 0.5 (EEOICPA) |
100% |
100% |
0 |
100% |
|
PC/ASmed with BNFL scale (Figure 5.6) |
100% |
100% |
25% |
0 |
|
PC/ASmed with linear scale (Figure 5.6) |
100% |
100% |
20% |
0 |
|
Fraction of PCdist ≥ 0.5 |
100% |
50% |
0 |
2% |
|
Integrate PC/ASdist with linear scale |
100% |
81% |
23% |
8% |
|
aPC/Asmed refers to the median value for each distribution, shown in parentheses at the head of each column. bThe numbers represent a percent of the maximum award for each scheme. |
||||
possible conflicts with the other compensations programs. It is not obvious that the alternative schemes would be more favorable or equitable to claimants. A compensation scheme based on PC/AS has sufficient flexibility to provide a scientifically based process for including persons who are not in geographic areas that are now eligible for compensation under RECA.
ANNEX
Calculation of PC/AS for Thyroid Cancer with Monte Carlo Method
To understand the process of determining PC/AS in more detail, the estimate of risk posed by exposure to 131I was obtained with an independent calculation. A Monte Carlo calculation was performed with the computer code Crystal Ball® 2000.2, which was developed and distributed by Decisioneering (2001).
The NCI-CDC working group (2003) used the following expression to determine the ERR of solid tumors caused by low-dose low-dose-rate radiation exposure:
(11)
where
REFL is the radiation effectiveness factor for the radiation type and cancer type,
Rγ,H is the ERR per Gy at high doses and high dose rates of the reference high-energy gamma radiation,
L and H refer to low and high doses and dose rates,
DDREFγ is the dose and dose-rate effectiveness factor, and
D is the estimated absorbed dose (Gy).
Rγ,H must be modified for the exposure scenario being considered. In this example, for low-dose low-dose-rate (chronic) radiation primarily from electrons (beta particles from the 131I decay), that was done by using REFL and DDREFγ. For clarity, the committee followed the NCI-CDC working group and used the terminology “Rγ,H” for the uncorrected ERR per Gy, and “ERR per Gy” for the ERR per Gy properly adjusted for the dose, dose rate, and radiation effectiveness factor. Then
(12)
Values for the four terms in Equation 11 all have associated uncertainties. In practice, a distribution of values is assigned to each term, depending on support-
ing scientific evidence, and the ERR is calculated by choosing values for each of the four terms that depend on the assigned distribution. Typically, the ERR is then calculated a number of times using a Monte Carlo sampling method, and the PC computed from each calculated value of the ERR. This process then determines the distribution of the PC.
The four terms in Equation 11 are as follows:
REFL = 1 (NCI-CDC, 2003, p. 65) for electrons with energies greater than 15 keV.
Rγ,H is the ERR per rad at high doses and high dose rates for high-energy gamma radiation. The NCI-CDC working group based its risk estimates for thyroid cancer on an analysis of seven studies by Ron et al. (1995). The resulting risk values depend on age at exposure, taken to be lognormally distributed, and are shown in Table 5.3 and Figure 5.7.
DDREFγ, the dose and dose-rate effectiveness factor for gamma radiation, for this example of chronic exposure, is a discrete probability distribution given in Table 5.4. In this context, chronic exposure to radiation occurs when the dose rate is less than 6 mGy/h (600 mrad/h) averaged over the first few hours (NCI-CDC, 2003, p. 32). The 6 mGy/hr dose rate is higher than what would occur for the 131I thyroid doses considered here as long as the total dose from one exposure is less than about 150 rad.
D, the absorbed dose, is the result of the NCI dose calculator, which is lognormally distributed with a geometric mean of 0.32 Gy (32 rad) and geometric standard deviation (GSD) of 4.
TABLE 5.3 Excess Relative Risk per Absorbed Dose (Gy) for Thyroid Cancer, High-Dose and High-Dose-Rate Gamma Radiationa
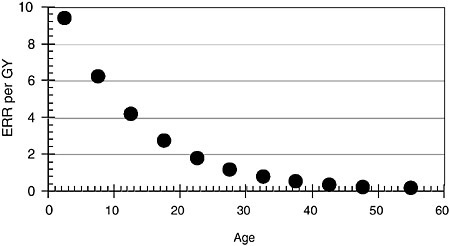
FIGURE 5.7 Excess relative risk per absorbed dose for thyroid cancer at high doses and high dose rates for gamma radiation (from NCI-CDC, 2003, p. 55).
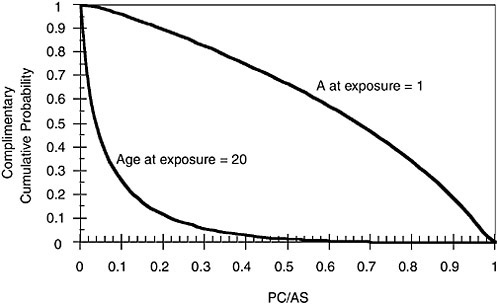
The calculation was repeated 500,000 times for this person, each time with a different value of each of the four terms in Equation 11, randomly chosen according to its statistical distribution. Results of the Monte Carlo calculation are shown in Figures 5.8a, 5.8b, and 5.8c. The computations were repeated for the case in which the person was born in 1931 and was thus 20 years old at the time of exposure. The PC/AS for that scenario is also shown in Figure 5.8c.
Figure 5.8c displays the results as a complementary cumulative distribution. The vertical axis represents the probability that PC/AS is greater than the value on the horizontal axis. For example, the median value of PC/AS (the point where the probability is 0.5 on the vertical axis) for exposure at the age of 20 is 0.04, compared with 0.67 at the age of 1 year. Drawing a vertical line that intersects the horizontal axis at 0.5 shows that there is a 1% chance that PC/AS is greater than 0.5 at the age of 20 years and a 65% chance that PC/AS is greater than 0.5 at the age of 1 year.
TABLE 5.4 Probability Distribution for the Dose and Dose-Rate Effectiveness Factora
|
DDREFγ |
Probability |
|
0.5 |
0.01 |
|
0.7 |
0.04 |
|
1.0 |
0.35 |
|
1.5 |
0.23 |
|
2.0 |
0.23 |
|
3.0 |
0.10 |
|
4.0 |
0.04 |
|
aSOURCE: NCI-CDC, 2003, p. 60. |
|
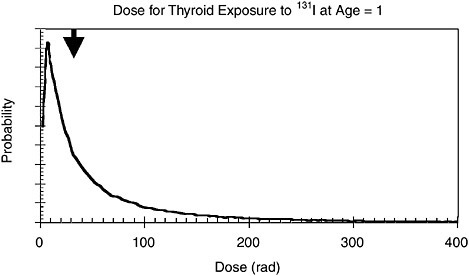
FIGURE 5.8a Distribution of absorbed dose to thyroid from exposure to 131I in fallout at age of 1. Median value of distribution is 32 rad, as indicated by arrow.
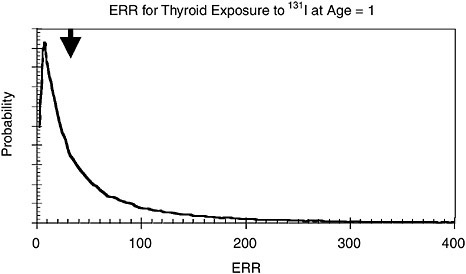
FIGURE 5.8b Distribution of excess relative risk of thyroid cancer from exposure to 131I in fallout at age of 1. Median value of distribution is 2.0 as shown by arrow.