Appendix E
Statistics on Emergency and Trauma Care Utilization
Emergency departments (EDs) and trauma centers see an enormous variety of patients and conditions on a daily basis. Regardless of income, insurance status, age, or race, people rely on EDs for care in the event of a serious illness or injury, and increasingly for primary care. This appendix describes some of the key utilization trends in hospital-based emergency care. It is based largely on data from the Centers for Disease Control and Prevention’s (CDC) National Hospital Ambulatory Health Care Survey for 2003, as reported by McCaig and Burt (2005), supplemented by other sources.
INJURIES AND CONDITIONS TREATED
In 2003, the most common medical diagnoses among ED patients, excluding injuries, were acute upper respiratory infections (5.7 percent), abdominal pain (3.9 percent), chest pain (3.7 percent), and spinal disorders (2.5 percent). About 40.2 million visits, or 35.3 percent of visits, were injury related. Of the visits related to injuries, 70 percent were for unintentional injuries, such as falls, being unintentionally struck by an object, motor vehicle crashes, and injuries from a piercing instrument or object. About 5 percent of injuries were intentional, including assaults and self-inflicted injuries (McCaig and Burt, 2005). Reasons for hospital ED visits are summarized in Table E-1.
There has also been a marked increase in the number of trauma visits, resulting in a significant increase in emergency workloads and contributing to the crowding problem (Reilly et al., 2005). During the 5 years between
TABLE E-1 ED Visits by 20 Leading Diagnoses
|
Principal Reason for Visit |
Percent |
|
Contusion with intact skin surface |
4.2 |
|
Acute upper respiratory infections, excluding pharyngitis |
4.0 |
|
Abdominal pain |
3.9 |
|
Chest pain |
3.7 |
|
Open wound, excluding head |
3.6 |
|
Spinal disorders |
2.5 |
|
Otitis media and eustachian tube disorders |
2.3 |
|
Sprains and strains, excluding neck and back |
2.2 |
|
Fractures, excluding lower limb |
2.1 |
|
Open wound of head |
2.0 |
|
Sprains and strains of neck and ankle and back |
2.0 |
|
Acute pharyngitis |
1.7 |
|
Urinary tract infection |
1.6 |
|
Chronic and unspecified bronchitis |
1.6 |
|
Superficial injuries |
1.6 |
|
Cellulitis and abscess |
1.6 |
|
Pyrexia of unknown origin |
1.5 |
|
Asthma |
1.5 |
|
Heart disease, excluding ischemic |
1.5 |
|
Rheumatism, excluding back |
1.5 |
|
All other |
53.1 |
|
Total |
99.7 |
|
SOURCE: McCaig and Burt, 2005. |
|
1999 and 2003, trauma visits rose by 18.1 percent. Most of this increase reflects patients who were seen by the trauma team and released rather than admitted as patients. The authors suggest that overtriage, perhaps related to malpractice and Emergency Medical Treatment and Active Labor Act (EMTALA) concerns associated with treating injured patients at nontrauma centers, may be a major factor.
Over the past several years, increasingly complex cases have been seen in the ED. Patients are presenting with higher severity of illness, and many have comorbidities and chronic diseases (Derlet and Richards, 2000; Bazzoli et al., 2003). These patients require more complex and time-consuming workups and treatments.
In 2000, 45.4 percent of Americans had a chronic condition (see Figure E-1). That number is expected to grow to 47.7 percent by 2015 (Partnership for Solutions, 2002). Specifically, the prevalence of cardiovascular disease (CVD) will increase by 18 percent as a result of the aging of the population. In 2003, 71 million Americans had CVD (AHA, 2006); by 2010, it is projected that 69 million Americans will have the disease. Simi-
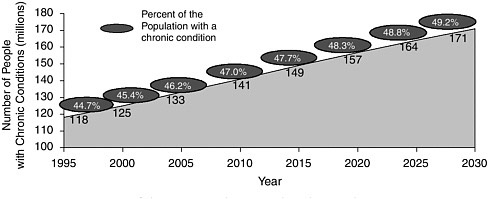
FIGURE E-1 Portion of the U.S. population with a chronic disease.
SOURCE: Partnership for Solutions, 2002.
larly, the prevalence of neurological diseases, particularly those associated with aging, such as Parkinson’s disease, stroke, and Alzheimer’s disease, will increase.
Increases in disease prevalence over the coming decade, especially of CVD and neurological disease, will also drive growth in ED use. The use of medical therapies will reduce ED visits in the near term, but those same patients will live longer, resulting in increased ED visits in the longer term. Implantable technologies for cardiac diseases will increase patient survival and the likelihood of increased ED visits later in patients’ lives. A higher prevalence of chronic diseases, such as diabetes, asthma, and obesity, will also lead to higher ED utilization. Poor patient management of chronic diseases and polypharmacy issues—the unwanted duplication of drugs—will contribute to increased ED utilization as well.
ED VISITS BY AGE
Elderly
Older Americans (75+) have a much higher rate of ED visits than other age groups (see Table E-2). Care of the elderly presents unique challenges. This pool of patients tends to come to the ED with more severe medical-related conditions, to have a higher probability of being admitted to the hospital, and to consume more resources than other patients.
Elderly patients may not receive appropriate care, particularly when there is cognitive impairment (Sanders, 2002). Their problems tend to be
TABLE E-2 Visits and Visits per 100 by Age, 2003
|
Age |
Number of Visits in Thousands |
Visits per 100 Persons |
|
Under 15 |
24,733 |
40.8 |
|
15–24 |
17,731 |
44.2 |
|
25–44 |
32,906 |
40.0 |
|
45–64 |
20,992 |
30.8 |
|
65–74 |
7,153 |
39.5 |
|
75 and older |
10,389 |
64.2 |
|
SOURCE: McCaig and Burt, 2005. |
||
complex and time-consuming, and therefore have a disproportionate impact on emergency care services (Sanders, 2001). For older patients, workups are more difficult, and lengths of stay in the ED are greater; nearly half of older patients (65 and older) are admitted to the hospital, compared with 11 percent of younger adults (McNamara et al., 1992; Singal et al., 1992). More patients aged 75 and older arrive by emergency medical transport (40.9 percent, versus 4.2 percent of all patients), and patients 65 and older are most likely to be classified as emergent (25.5 percent, versus 15.2 percent of all patients) (McCaig and Burt, 2005). Utilization of the ED by elderly patients is likely to increase as the population ages over the next two decades; by 2050, individuals aged 65+ are expected to make up over 20 percent of the total U.S. population (U.S. Census Bureau, 2004).
Children
In 2003, children under age 15 made over 24 million visits to EDs, representing 22 percent of all ED visits. This equates to almost 4 visits for every 10 children under age 15 (McCaig and Burt, 2005). Despite the frequent use of emergency services by children, the training, equipment, medications, and technology of emergency care often fail to address their needs (Glaser et al., 1997; Moreland et al., 1998; Tamariz et al., 2000; Middleton and Burt, 2006). Children are different from adults in a wide range of clinically significant ways. For example, they have different metabolic and respiratory rates, different blood pressure levels, smaller airways, greater surface-to-body weight ratios, higher emotional sensitivity, and limited communication skills. The services, drugs, and equipment developed for use by adult patients in an emergency situation are often inappropriate for pediatric patients. The limited availability of pediatric equipment and supplies in ambulances and EDs has been well documented in several reports (IOM, 1993; Hamilton et al., 2003). One survey of EDs found that the average hospital in the
United States had about 80 percent of the American Academy of Pediatrics’ (AAP) recommended pediatric supplies, and only 6 percent of hospitals had all of the recommended equipment (Middleton and Burt, 2006). And while children’s hospitals are a unique resource for pediatric patients, most such patients are treated in general rather than children’s hospitals (Gausche-Hill et al., 2004). Pediatric emergency care is dealt with comprehensively in the companion IOM report in this series titled Emergency Care for Children: Growing Pains.
ED VISITS BY RACIAL AND ETHNIC COMPOSITION
The 2002 utilization rate for African Americans was 71 percent higher than that for whites. In addition, African Americans had some of the largest increases in ED utilization rates during the 1990s. Particularly among those over 65, African Americans increased their ED utilization by 59 percent during that decade, while utilization among whites in the same age bracket remained relatively unchanged (McCaig and Ly, 2002).
Other minority populations, including Hispanic and non-English-speaking populations, also utilize the ED at higher rates than whites. The proportion of the population that said they spoke English less than “very well” grew from 4.8 percent in 1980 to 6.1 percent in 1990 and 8.1 percent in 2000 (U.S. Census Bureau, 2004). Language barriers can result in higher rates of resource utilization for diagnostic studies, increased ED visit times (Hampers et al., 1999), and lower satisfaction with care (Carrasquillo et al., 1999). In addition, non-English-speaking people may be less likely to trust the emergency system and more likely to be unfamiliar with 9-1-1 and to fail to understand which services are available to them and at what cost.
While racial disparities in health care have been well documented (IOM, 2002; AHRQ, 2003), the evidence for disparities in emergency services is limited. Studies have shown differences in wait times for Hispanic patients, insurer authorization for ED visits by African Americans (Lowe and Bindman, 1994), and administration of pain medication for African Americans (Todd et al., 2000).
FREQUENT USERS
One particularly challenging group of ED patients is those who make repeated visits. Estimates from different data sources indicate that 5 to 7 percent of the U.S. population will make two or more ED visits in a given year (Zuckerman and Shen, 2004). A smaller group of individuals, often referred to as “frequent flyers,” visit the ED for care even more frequently. Frequent users tend to be in poor health, suffering from high rates of chronic illness, drug disorders, and mental illness (Sun et al., 2003; Washington
State Department of Social and Health Services, 2004). Many also suffer from socioeconomic distress (Sun et al., 2003). Frequent users are a challenge to ED staff because they require intensive resources, such as mental health, substance-abuse, and case management services, that often are not available at EDs.
REFERENCES
AHA (American Heart Association). 2006. Heart Disease and Stroke Statistics—2006 Update. Dallas, TX: AHA.
AHRQ (Agency for Healthcare Research and Quality). 2003. National Healthcare Disparities Report. Rockville, MD: U.S. Department of Health and Human Services.
Bazzoli GJ, Brewster LR, Liu G, Kuo S. 2003. Does U.S. hospital capacity need to be expanded? Health Affairs 22(6):40–54.
Carrasquillo O, Orav E, Brennan T, Burstin H. 1999. Impact of language barriers on patient satisfaction in an emergency department [Abstract]. Journal of General Internal Medicine 14(2):82–87.
Derlet RW, Richards JR. 2000. Overcrowding in the nation’s emergency departments: Complex causes and disturbing effects. Annals of Emergency Medicine 35(1):63–68.
Gausche-Hill M, Lewis R, Schmitz C. 2004. Survey of US Emergency Departments for Pediatric Preparedness—Implementation and Evaluation of Care of Children in the Emergency Department: Guidelines for Preparedness. [unpublished].
Glaser NS, Kuppermann N, Yee CK, Schwartz DL, Styne DM. 1997. Variation in the management of pediatric diabetic ketoacidosis by specialty training. Archives of Pediatrics & Adolescent Medicine 151(11):1125–1132.
Hamilton S, Adler M, Walker A. 2003. Pediatric calls: Lessons learned from pediatric research. JEMS: Journal of Emergency Medical Services 28(7):56–63.
Hampers LC, Cha S, Gutglass DJ, Binns HJ, Krug SE. 1999. Language barriers and resource utilization in a pediatric emergency department. Pediatrics 103(6 Pt. 1):1253–1256.
IOM (Institute of Medicine). 1993. Emergency Medical Services for Children. Washington, DC: National Academy Press.
IOM. 2002. Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care. Washington, DC: The National Academies Press.
Lowe RA, Bindman AB. 1994. The ED and triage of nonurgent patients. Annals of Emergency Medicine 24(5):990–992.
McCaig LF, Burt CW. 2005. National Hospital Ambulatory Medical Care Survey: 2003 Emergency Department Summary. Hyattsville, MD: National Center for Health Statistics.
McCaig LF, Ly N. 2002. National Hospital Ambulatory Medical Care Survey: 2000 Emergency Department Summary (Advance Data from Vital and Health Statistics No. 326). Hyattsville, MD: National Center for Health Statistics.
McNamara RM, Rousseau E, Sanders AB. 1992. Geriatric emergency medicine: A survey of practicing emergency physicians. Annals of Emergency Medicine 21(7):796–801.
Middleton KR, Burt CW. 2006. Availability of Pediatric Services and Equipment in Emergency Departments: United States, 2002–03. Hyattsville, MD: National Center for Health Statistics.
Moreland JE, Sanddal ND, Sanddal TL, Pickert CB. 1998. Pediatric equipment in ambulances. Pediatric Emergency Care 14(1):84.
Partnership for Solutions. 2002. Chronic Conditions: Making the Case for Ongoing Care. Baltimore, MD: Johns Hopkins University.
Reilly PM, Schwab CW, Kauder DR, Dabrowski GP, Gracias V, Gupta R, Pryor JP, Braslow
BM, Kim P, Wiebe DJ. 2005. The invisible trauma patient: Emergency department discharges. Journal of Trauma-Injury Infection & Critical Care 58(4):675–683; discussion 683–685.
Sanders AB. 2001. Older persons in the emergency medical care system. Journal of the American Geriatrics Society 49(10):1390–1392.
Sanders AB. 2002. Quality in emergency medicine: An introduction. Academic Emergency Medicine 9:1064–1066.
Singal BM, Hedges JR, Rousseau EW, Sanders AB, Berstein E, McNamara RM, Hogan TM. 1992. Geriatric patient emergency visits. Part I: Comparison of visits by geriatric and younger patients. Annals of Emergency Medicine 21(7):802–807.
Sun BC, Burstin HR, Brennan TA. 2003. Predictors and outcomes of frequent emergency department users. Academic Emergency Medicine 10(4):320–328.
Tamariz VP, Fuchs S, Baren JM, Pollack ES, Kim J, Seidel JS. 2000. Pediatric emergency medicine education in emergency medicine training programs. SAEM pediatric education training task force. Academic Emergency Medicine 7(7):774–778.
Todd K, Deaton C, D’Adamo A, Goe L. 2000. Ethnicity and analgesic practice. Annals of Emergency Medicine 35(1):11–16.
U.S. Census Bureau. 2004. The Face of Our Population. [Online]. Available: http://factfinder.census.gov/jsp/saff/SAFFInfo.jsp?_pageId=tp9_race_ethnicity [accessed March 22,2005].
Washington State Department of Social and Health Services. 2004. Frequent Emergency Room Visits Signal Substance Abuse and Mental Illness DSHS Research and Data Analysis Division. Olympia, WA: Washington State Department of Social and Health Services.
Zuckerman S, Shen Y-C. 2004. Characteristics of occasional and frequent emergency department users. Medical Care 42(2):176–182.








