3
Potential Risks Associated with Egg Retrieval
After the hormone treatment has stimulated the ovaries to produce more eggs, those eggs must be retrieved. The retrieval surgery takes place about 36 hours after the injection of human chorionic gonadotropin (hCG), which signals the follicles to prepare to ovulate. In ovulation, a follicle ruptures and expels the egg from the follicular sac, after which the egg will travel through the fallopian tube toward the uterus. Egg retrieval is timed to catch the eggs shortly before they would start this journey, at a point at which they are ready for fertilization but are still within their follicles and they can easily be found.
To retrieve the eggs, a surgeon places a device into the vagina that pushes a needle through the vagina wall and into the ovary (see Figure 3-1). All of the movements are guided by ultrasound technology. Once the needle is inside the ovary, it is maneuvered to pierce one follicle after another. When the needle is inside a follicle, suction is applied to pull the follicular fluid out through a tube and into a test tube. Floating within the fluid extracted from the follicles will be the target of the procedure: the oocytes.
The surgery, which generally lasts about 30 minutes, is done on an outpatient basis, and the woman usually goes home a few hours after the eggs are retrieved. This procedure is considered to be minor surgery. Nonetheless, it is still a surgical procedure done under anesthesia, and both the surgery and the anesthesia carry potential risks. Several speakers at the workshop described these potential risks and detailed what is known about them.
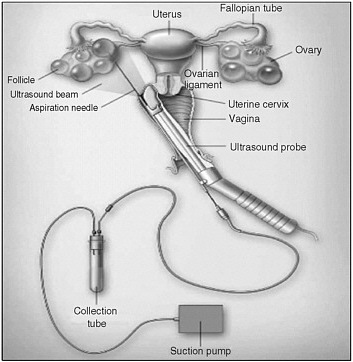
FIGURE 3-1 Oocyte retrieval.
SOURCE: Steinbrook (2006). Copyright © 2006 Massachusetts Medical Society. All rights reserved.
POTENTIAL SURGICAL RISKS
Most of the surgical complications surrounding egg retrieval stem from two basic facts about the surgery: a needle must be pushed through the vagina and into the ovary, and a number of other organs and sensitive tissues lie nearby. The hypogastric artery (also known as the internal iliac artery) runs past the ovary, for example, as does the ureter. The surgeon often finds the ureter right next to the ovary, explained Ana Murphy, chair of the Department of Obstetrics and Gynecology at the Medical College of Georgia, which might put the ureter at high risk for inadvertent damage.
It is difficult to know, however, exactly how often such complications occur, Dr. Murphy said. Although excellent statistics are kept on such things as how many viable eggs each procedure produces, the statistics are not so complete on the complications that ensue during and after
the surgery. Still, there are enough data to get a good idea of what is going on.
Dr. Murphy described the results of a study in Germany that examined the outcome of approximately 380,000 oocyte retrieval surgeries during 2000-2004. There was no information about complications for 28 percent of them, but for the procedures for which there was information, the rate of complications was very low. There was vaginal bleeding in 0.07 percent of the women, intra-abdominal bleeding in 0.05 percent, intestinal injuries in 0.001 percent, and peritonitis, or an inflammation of the peritoneum (the lining of the abdominal cavity) in 0.005 percent. Of all the women who had the procedure, only 0.002 percent—2 in every 100,000—had complications that required surgery to correct.
It is possible, Dr. Murphy said, that these numbers are far too optimistic. “There are those that say that there must be underreporting here, and that has been suggested in the literature. I don’t know.” But if the numbers are accurate, it is clear that the rate of complications was very low.
A prospective study published in 2006 showed a clearly higher rate of complications, but, again, the rate of serious complications was very low. In a study population of more than 1,000 patients, 2.8 percent experienced some vaginal bleeding, but none required suturing. Indeed, for all but one of the patients, all that was needed to stop the bleeding was the application of pressure; one patient required a tamponade, an absorbent dressing, applied to the wound. Severe pain requiring hospitalization occurred in 0.7 percent of the 1,035 women studied who had undergone oocyte retrieval, and in one case there was an injury to another organ (the ureter), and the patient recovered quickly after a stent was placed in the ureter.
Fewer studies are available that look at the question of infectious complications, and Dr. Murphy described two. In one, published in 1993, 9 patients out of 1,000 had pelvic abscesses after surgery that had to be treated. In a second, published in 2006, there were no abscesses at all. “I was curious as to how there could be such a huge difference,” Dr. Murphy said, “so I looked at the materials and methods [in the earlier study]. And what I found was that aseptic technique was not the norm, at least in this institution, and that they cleaned it with saline. They did not do anything other than keep the end of the needle sterile. And so some of this may actually be what happens when you drag in infectious agents with your needle.” The implication would seem to be that infectious complications are rare as long as aseptic techniques are used.
Another complication that appeared on occasion was ovarian torsion, which occurs when the ovary twists around on itself, cutting off its blood supply. In a study of 1,500 women who underwent in vitro fertilization (IVF), torsion occurred in 0.13 percent of the cycles. The torsion occurred late, 6 to 13 weeks after the oocyte retrieval, and since the risk of torsion increases with the softening of the ligaments that appears in pregnancy, it seems that torsion is a complication that is mainly associated with women who get pregnant with IVF, according to Dr. Murphy. Later in the workshop, Dr. Zev Rosenwaks, director of the Center for Reproductive Medicine and Infertility at Cornell University, said that torsion can also occur with hyperstimulation in the absence of pregnancy.
Various things can be expected to increase the potential risk of complications for women undergoing oocyte retrieval, Dr. Murphy said. Previous surgeries make complications more likely, for example, because the surgeon finds structures where they’re not supposed to be, or else the structures don't move the way they’re supposed to move. A history of pelvic inflammatory disease (PID) is also an important risk factor, as are endometriosis and pelvic adhesions. Generally speaking, all of these things are much more likely to be found in women undergoing in vitro fertilization—because of their history of infertility and various efforts to get pregnant—than in women serving as egg donors.
In conclusion, Dr. Murphy said, the data indicate that the potential risks of surgical complications from oocyte retrieval are generally very small. There are very few data that are specific to egg donors—as opposed to infertile women undergoing oocyte retrieval and, later, the implantation of embryos—but all of the evidence implies that the potential surgical risks should be much lower in oocyte donors.
POTENTIAL RISKS OF ANESTHESIA
Besides the potential risks associated with the surgical retrieval, women undergoing oocyte retrieval also face certain potential risks from the anesthesia used to handle their pain during the surgery. Lawrence Tsen, associate professor in anesthesia at the Harvard Medical School, spoke at the workshop about these potential risks.
When discussing the use of anesthesia, Dr. Tsen said, there are three basic subjects to cover: whether anesthesia is needed for a particular pro-
cedure, what form of anesthesia should be used, and what the potential risks are.
To the question of whether anesthesia is necessary for oocyte retrieval, he said, “I would have to answer an emphatic yes.” And the reasons for this, he said, come from a consideration of the sorts of pain that a patient faces during oocyte removal.
Three things cause pain during oocyte removal, Dr. Tsen said: the stretching of the perineum when the retrieval tool is inserted, the push of the needle through the vaginal wall, and the insertion of the needle into the ovary. Because of where these pain signals enter the spine, a paracervical block—a type of anesthesia sometimes used during childbirth that involves injecting a local anesthetic on either side of the cervix—would not block all of the pain. Thus an anesthesiologist would need to use something in addition to the paracervical block or else would have to use a spinal anesthetic or some intravenous form of anesthesia or sedation.
Furthermore, Dr. Tsen said, women going through oocyte retrieval have a factor that may make them particularly sensitive to pain. He tested a group of women who were going through in vitro fertilization to see if the higher estrogen levels that they experience made a difference to how their bodies process pain signals. He did this by testing how sensitive they were to two stimuli, cold and pressure, that are processed by the same nociceptors, or sensory receptors, that process pain. He tested the women before they began the IVF process and then again at the time of oocyte retrieval. What he found was that, although the women showed no difference in how they responded to pressure, they were much more sensitive to cold stimuli, and their reaction time to those stimuli was significantly altered. The implication, Dr. Tsen said, was that there is clearly some pain modulation among women undergoing IVF cycles, and it is probably caused by the high estrogen levels.
Given that some form of anesthesia is needed in oocyte retrieval, the next question is what form of anesthesia should be used. Surveys of doctors in the United States, the United Kingdom, and Germany indicate that at least 99 percent of cases of oocyte retrieval rely on intravenous anesthesia or intravenous conscious sedation. Some individuals have tried such alternatives as acupuncture or hypnosis, Dr. Tsen said, but the results have generally not been satisfactory, and often those patients fall back on intravenous conscious sedation. He also said that he has spoken with doctors in other countries, including Canada and France, who report very similar situations, so it would seem that a broad consensus exists as to what sort of anesthesia should be used in oocyte retrieval.
The third question is what potential risks these sorts of anesthesia pose for the patient. There are no statistics that look specifically at the potential risk of anesthesia for patients undergoing oocyte retrieval, Dr. Tsen said, but it is possible to look at the overall risks of anesthesia, see what sorts of factors increase or decrease those risks, and then, by considering what sorts of individuals become egg donors, get a good idea of what the potential anesthesia risks would be for them.
Anesthesia has become very safe over the past couple of decades, Dr. Tsen said. Two of the biggest advances were the development in the 1980s of pulse oximetry and capnography, which allow health care providers to monitor a patient’s blood oxygen level and, indirectly, the level of carbon dioxide in the blood as well. Today, thanks in part to such technology but also thanks to better training and guidelines, deaths attributable to anesthesia occur only about once in 200,000 to 300,000 cases. This is comparable to the risk of flying, Dr. Tsen noted, as a person has about one chance in 250,000 of dying each time he or she boards a plane.
Examining the statistics more carefully, it is possible to pick out characteristics that put a person at higher risk from anesthesia, Dr. Tsen said. Those characteristics include being male, being older, being obese, being scheduled for inpatient rather than outpatient surgery, having surgery in an emergency setting, and having a high ASA (American Society of Anesthesiologists) classification. The ASA scheme rates how healthy a patient is on a scale from 1 for a normal healthy patient to 5 for a moribund patient who is not expected to survive 24 hours. Of the characteristics that increase the risk of anesthesia, Dr. Tsen noted, the only ones that might apply to women undergoing in vitro fertilization would be obesity and a higher ASA rating, such as might be the case for a woman who is about to undergo whole-body irradiation to treat cancer and who wants to preserve her fertility by preserving some of her eggs. But for women donating their eggs for research, it seems likely that the only characteristic that would increase the risk of anesthesia would be obesity. “So,” Dr. Tsen said, “it suggests to us that anesthetic intervention for this sort of procedure is a very safe intervention.”
There are other risks of anesthesia besides death. Some of the major morbidities associated with anesthesia are heart attacks, stroke, pulmonary emboli, and respiratory failure, but, again, they rarely occur. And there are complications that are less threatening, such as difficulty in breathing, that can require the patient to be intubated. When Dr. Tsen performed a study of IVF patients at Harvard Medical School undergoing
anesthesia during oocyte retrieval, he found that such complications as intubation or desaturation—a lowering of the blood oxygen content—were infrequent, but they were more likely in obese patients. Approximately 8 percent of the obese patients experienced desaturation, compared with less than 1 percent of those of normal weight. And 1.7 percent of obese patients required intubation versus 0.1 percent of patients of normal weight.
The bottom line, Dr. Tsen said, is that the potential risks of anesthesia for oocyte retrieval are very low—rare mortality, rare major morbidity, and rare minor morbidity. The one potential risk factor that applies to egg donors and that might put them at more risk during anesthesia is if they are obese, but even then the potential risks remain very small.
POTENTIAL LONG-TERM EFFECTS ON FERTILITY
The final question concerning the potential risks of oocyte retrieval is the surgery’s implications for a woman’s future fertility. Is her ability to have children in the future threatened in any way by having had this surgery? Nicholas Cataldo, formerly an assistant professor of obstetrics and gynecology at Stanford University, reviewed the evidence bearing on this question for the workshop.
Dr. Cataldo examined two possible pathways by which oocyte retrieval might conceivably affect future fertility. The first pathway begins with the infection and bleeding that, as described above, are occasional side effects of retrieval surgery. These side effects sometimes lead to the need for surgery or to the formation of adhesions, the sticking-together of two adjacent tissues. Both of these results, Dr. Cataldo said, could theoretically lead to fertility problems.
There is little evidence to support this possibility, however. According to one large study, the rate of infection after oocyte retrieval was about 1 in every 200 IVF cycles, and surgery is needed to treat pelvic abscesses in less than 1 in 1,000 IVF cycles. Furthermore, since women have a set of two ovaries and two fallopian tubes, they can remain fertile even if one set is damaged, and there is no evidence that both might be threatened simultaneously by the side effects of retrieval surgery. In one study that examined this particular issue, Dr. Cataldo said, none of the women who had surgery to treat abscesses had them on both sides or lost both fallopian tubes or ovaries. As for adhesions, research has not found a higher rate of adhesions among women who have undergone oocyte
retrieval surgery. Finally, Dr. Cataldo said, since the data involve mainly women who have had fertility problems, it can be expected that the rate of infection among egg donors will be lower than has been seen in the published studies. All of this implies that there is little potential risk of future fertility being threatened in egg donors by infection or bleeding accompanying the retrieval surgery.
The second potential pathway to fertility risk begins with the trauma applied to the ovary by having a needle thrust through its surface. It has been suggested that this trauma could lead to the development of anti-ovary antibodies, and, indeed, several studies have found that women who have undergone oocyte retrievals have a greater prevalence of antibodies to ovarian tissue than those who have not undergone the surgery.
Furthermore, antibodies to ovarian antigens have been shown to be associated with IVF failures and with women having multiple attempts at IVF—a situation that, again, implies that they have had previous failures. It is possible, Dr. Cataldo said, that somehow these antibodies may interfere with sperm binding with or penetrating the oocyte and thus make it harder to fertilize the egg, but there is no evidence that this actually happens. It is difficult to know whether antibodies formed in one IVF cycle have anything to do with the failure of subsequent IVF attempts, or even if the antibodies play any role at all in infertility.
“So both of these potential avenues for risk related to oocyte retrieval have question marks associated with every step of the way,” Dr. Cataldo concluded. And whatever risk there may be for women undergoing IVF, the risk would be expected to be somewhat lower in healthy women donating eggs for research.
SUMMARY: WHAT WE KNOW ABOUT THE RISKS OF EGG RETRIEVAL
Once hormone treatment has led the ovaries to create a large number of antral follicles ready to ovulate, a surgeon must retrieve the eggs from the follicles by putting a needle through the wall of the vagina into the ovary and using the needle to aspirate the individual follicles. This surgery must be done with anesthesia, and there are a number of health risks that accompany the surgery and the anesthesia.
The statistics on egg retrieval surgery indicate that the risks of complication are relatively low. One study of several hundred thousand surgeries found, for example, that vaginal bleeding occurred in 0.07 percent
of the women, intestinal injuries in 0.001 percent, and peritonitis in 0.005 percent. Only 0.002—or 2 in every 100,000—had complications that required surgery to correct.
Complications due to infection are rare as well. Although a 1993 study found 9 patients out of 1,000 had pelvic abscesses that needed to be treated, that seems to have been due to a failure to consistently use aseptic techniques. A later study in which aseptic techniques were used found no abscesses that required treatment.
Ovarian torsion is another rare complication in women undergoing IVF—about 0.13 percent of the time, according to one study. According to Dr. Cataldo, this complication seems mainly due to the softening of the ligaments that occurs during pregnancy. Dr. Rosenwaks added that it can also occur due to hyperstimulation, even in the absence of pregnancy.
Various factors increase the risk of complications from retrieval surgery, including previous surgeries, a history of pelvic inflammatory disease, endometriosis, and pelvic adhesions. All these factors are more likely to be found in women undergoing in vitro fertilization than in the general population, which implies that egg donors should have much lower surgical risks than women undergoing IVF.
Patients undergoing egg retrieval surgery generally rely on either intravenous anesthesia or intravenous conscious sedation. In general, anesthesia is safe, with deaths occurring only once every 200,000 to 300,000 cases. Because egg donors have few of the factors that increase the risks of anesthesia, including being male, being older, being obese, having inpatient rather than outpatient surgery, having surgery in an emergency setting, and having a high ASA classification, anesthesia should be even safer for egg donors than it is for surgical patients in general.
There are two main ways that surgery may affect a woman’s future fertility—either by bleeding and infection from the surgery leading to adhesions and the need for further surgeries, or else by the trauma to the ovaries causing the creation of antibodies that may make fertilization of an oocyte more difficult—but there is no data supporting either of these possibilities.










