2
Obesity Prevention Strategies in Concept and Practice
|
KEY MESSAGES
|
Obesity has long been viewed as an individual problem, treated primarily by individual or family-based medical and/or psychological methods. As noted in Chapter 1, the expansion of the obesity epidemic to affect diverse age groups, socioeconomic strata, and racial or ethnic groups and communities in the United States and globally has caused a paradigm shift toward preventive strategies that can reach whole communities and populations, as well as a sense of urgency in mounting these strategies (Kumanyika et al., 2002, 2008; Public Health Service, 2001; WHO, 2000). This chapter provides an overview of current thinking and practice regarding obesity prevention strategies. First, definitions and types of obesity prevention are discussed
from a population perspective. The logic of obesity prevention when undertaken by different sectors and at different levels is then examined using an overarching model developed by a prior Institute of Medicine (IOM) committee on child obesity prevention. Specific obesity prevention approaches are next identified across a spectrum that includes changes in policy and legislation, organizational practices, community and neighborhood environments, and health care settings, as well as strategies based on health communication or health education and individual counseling. Examples of how these strategies are combined in multilevel approaches are also provided. The chapter concludes by placing strategies being used to address obesity prevention in the context of those used to address other complex public health problems.
Approaches discussed in this chapter draw on accounts of current practice, policies, and programs that have been implemented or recommended as being potentially pertinent to obesity prevention. Background information on concepts and evidence for assessing the effectiveness of the approaches presented here is provided in Chapter 3.
DEFINITIONS AND TYPES OF PREVENTION
The concept of increasing obesity prevalence caused by a shift in the population distribution of BMI was shown in Figure 1-1 in Chapter 1, based on actual data for adults in the U.S. population. From a population perspective, obesity prevention means reversing this shift—lowering the mean BMI level and decreasing the incidence of obesity, that is, the rate at which people enter the upper end of the BMI distribution (Kumanyika et al., 2002; WHO, 2000). Stabilization of the BMI distribution or the incidence of new people crossing the relevant BMI threshold (30 kg/m2 for adults or the 95th sex–age percentile of the BMI reference for children) would be the first sign of success, followed by a decline in these indicators. Within the population, accomplishing this will require that adults at a healthy weight (i.e., not underweight, overweight, or obese) maintain that status and avoid the phenomenon of excess weight gain that commonly accompanies aging. For children, prevention means maintaining a healthy weight trajectory and preventing excess weight gain while growing, developing, and maturing. Prevention for individuals who are already overweight or obese can be defined as avoiding progression to a more severe level of obesity and/or preventing or delaying the onset of obesity-related medical conditions (IOM, 1995).
A 1995 IOM report on criteria for evaluating weight management programs emphasizes the importance of giving greater priority to obesity prevention in light of the increases in population weight levels and obesity prevalence (IOM, 1995). Although that report focuses primarily on setting standards for individually focused weight management programs, the committee that produced it set the stage for thinking about levels of prevention from a population perspective. Instead of the primary, secondary, and tertiary prevention terminology, based on a continuum of disease
emergence,1 that is typically used in relation to chronic diseases, the committee identified categories of prevention in terms of population segments. Thus, the 1995 committee moved toward a more general risk reduction approach to prevention.
As shown in Figure 2-1, the population-based classification in the 1995 report identifies three levels of obesity prevention interventions targeting the population at large (universal); subgroups of the population that are at high risk, such as those defined by race/ethnicity or income level (selective); or individuals at high risk (indicated). High risk may refer to individuals who are identified as having minimal but detectable signs that foreshadow obesity, who exhibit biological markers indicating a predisposition to an obesity-related condition, or who do not meet the full diagnostic criteria for the disorder itself (IOM, 1995). The key distinction is in whether the population targeted has been selected on the basis of risk characteristics. The adoption of a similar population-based conceptualization of obesity prevention by a 1997 World Health Organization (WHO) expert panel in characterizing intervention strategies to address the obesity epidemic globally (WHO, 2000) has further disseminated this way of thinking about obesity prevention strategies.
This population-based view of prevention focuses attention on key issues related to how resources are used and the relative emphasis placed on interventions aimed at directly changing individual behavior (e.g., in indicated prevention). Targeted, selective, and indicated prevention approaches differ in cost per person reached and in many other variables that determine their feasibility and ultimate impact. Fundamental to the need for the new framework proposed in this report, these strategies also differ in how one goes about evaluating their impact—by examining effect sizes, certainty of effects, and potential benefits and harms. Furthermore, a mix of strategies is needed. Individual-oriented strategies are critical, but for problems affecting whole populations, they should be used judiciously because they are often some of the most resource-intensive approaches. Such indicated prevention strategies are essentially treatment strategies directed either at adults or children who can be considered overweight (“pre-obese”) or at obese children to prevent their progression to obesity during adulthood. These strategies require case identification and intensive, long-term counseling.
Another reason to place less emphasis on individual-oriented strategies for obesity prevention relates to the nature of what constitutes prevention from an individual behavioral perspective. Although the prevention and treatment of obesity both rely on the same principle of energy balance, the challenges are quite different. Treatment relies on the creation of negative energy balance through substantial reductions in caloric intake and increases in physical activity to produce an observable reduction in body weight. Prevention strives to create caloric balance (or caloric intake that supports appropriate growth patterns in children) and to avoid a persistent, small positive
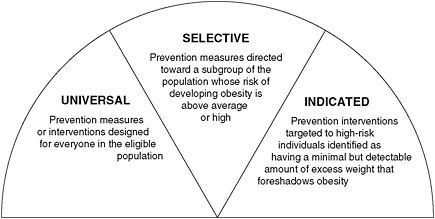
FIGURE 2-1 Types of obesity prevention interventions.
SOURCE: IOM, 1995.
energy imbalance that over time results in excess weight gain. As a result, quantifying the results of prevention is difficult because the results are less apparent—no change in weight or health outcomes, as opposed to the weight loss and decrease in risk factors associated with treatment (Kumanyika et al., 2008). It is also difficult to measure or, from the individual’s perspective, to be reassured that people are making the small changes in caloric intake and physical activity that may facilitate the prevention of excess weight gain. For this reason, it is important to emphasize universal prevention strategies intended to foster aggregate behaviors along lines that will decrease the likelihood of chronic excess caloric consumption in relation to expenditure. Such approaches focus primarily on modifying social norms and social structures through changes in policies or the implementation of broad interventions that reduce exposure to obesity-promoting environments in the population at large. The same is true for targeted prevention approaches that direct universal strategies at subpopulations (e.g., children and youth, or ethnic or socioeconomic status groups with higher-than-average obesity prevalence). A focus on specific populations may be needed to ensure that interventions address disparities in social and environmental conditions related to eating or physical activity (e.g., in food availability or affordability or in options for physical activity). Universal prevention may address individuals, although not on a one-to-one basis. Examples are mass education or social marketing strategies to improve individual knowledge and skills related to weight change or to promote favorable responses to changes at the environmental or policy level.
Complementary to concepts of obesity prevention that are based on the population segment targeted, public health strategies may also be characterized as affecting macro versus micro environments: macro environments might be at the national, state, or community level, involving variables that affect individuals indirectly, while micro environments might be school, worksite, clinical, or home environments to which
individuals are directly exposed on a day-to-day basis. A distinction also is often made between “upstream” and “downstream” approaches: the former address factors far removed from the individual’s control, whereas the latter reach individuals on a one-to-one basis. Upstream approaches are also more likely than downstream approaches to reduce disparities for socially and economically disadvantaged populations because they improve access to opportunities for healthful eating and physical activity (Kumanyika et al., 2008). Upstream approaches often target sectors outside of public health and health care, such as education, agriculture, transportation, urban planning, and industry, that influence eating and activity patterns.
THE LOGIC OF OBESITY PREVENTION
To develop a framework for evaluating childhood obesity efforts, a prior IOM committee developed a series of logic models that are helpful in understanding pathways to obesity prevention at different levels and in different sectors. The overall model developed by that committee, which is relevant to obesity prevention for populations of all ages, is reproduced as Figure 2-2 to provide a conceptual basis for thinking about prevention strategies.
At the far right of this logic model, the ultimate outcomes related to obesity prevention (“Health Outcomes”) are shown to result from achievements related to four different types of intermediate outcomes—structural, institutional, systemic, and envi-
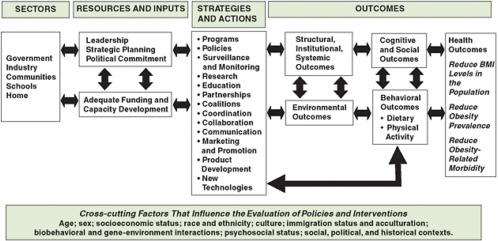
FIGURE 2-2 Evaluation framework for childhood obesity prevention policies and interventions.
SOURCE: IOM, 2007.
ronmental outcomes in society or the community—which impact cognitive, social, and behavioral outcomes in individuals. A range of potential strategies and actions can be applied to achieve the intermediate outcomes.
At the left of the model, the potential for these strategies and actions to be undertaken by various sectors (government, industry, communities, schools, and homes) is indicated. The specifics of resources and inputs, strategies and actions, and outcomes that are relevant vary by sector. How this logic plays out sector by sector is included in the prior committee’s report (IOM, 2007). The demographic, sociocultural, and economic variables shown across the bottom of the figure as “cross-cutting factors” might define considerations for when targeted prevention is needed. The individual cross-cutting factors will determine the heterogeneity of effects on individuals and, therefore, the average effects on populations.
The logic model in Figure 2-2 illustrates some key points that will be revisited throughout the remaining chapters of this report. One is that the ultimate objective of obesity prevention activities is a change in BMI levels. Another is that change in BMI outcomes is achieved through activities that have an impact on four types of intermediate outcomes. The model emphasizes that many strategies undertaken to prevent obesity will not be expected to have an impact directly on BMI, but rather on pathways that will alter the context in which eating, physical activity, and weight control occur. This point has clear implications for the evaluation of evidence from obesity prevention studies with respect to how well the outcomes assessed match the actions in question. This report does not aim to give specific guidance as to which outcomes to assess; rather, it encourages users of the framework to think broadly when choosing outcomes, considering intermediate outcomes that lead to the ultimate objective of achieving and/or maintaining appropriate BMI levels.
Expert panels concerned both with dietary guidance generally and with the prevention of specific diseases emphasize the importance of obesity prevention (CDC, 2009; HHS, 2008; USDA/HHS, 2005; WHO, 2003, 2004; World Cancer Research Fund and American Institute for Cancer Research, 2007). For example, the 2005 Dietary Guidelines for Americans include a recommendation to “maintain body weight in a healthy range” and to “prevent gradual weight gain over time” (USDA/HHS, 2005, p. 14). The World Cancer Research Fund 2007 report (p. 373) includes a recommendation to “be as lean as possible within the normal range [defined as the appropriate ranges issued by national governments or WHO] of body weight.” These groups specify targets for obesity prevention based on population behaviors that may predispose to excess caloric intake or inadequate physical activity. These targets, supported by evidence with varying degrees of certainty, are summarized in Box 2-1. With a few exceptions, these targets apply to people of all ages and are therefore appropriate for both universal and targeted prevention strategies.
|
Box 2-1 Target Behaviors for Obesity Prevention Diet-related
Activity-related
Other
SOURCES: |
THE SPECTRUM OF OBESITY PREVENTION APPROACHES
This section describes a sampling of obesity prevention interventions, adapted along lines suggested by the Spectrum of Prevention developed by Cohen and Swift (Cohen and Swift, 1999; Rattray et al., 2002) for use in public health and health promotion. The Spectrum of Prevention is a framework for developing multifaceted approaches to address complex public health problems. It identifies multiple levels of increasing scope, from the individual level to the policy level, emphasizing that effectiveness in addressing a given issue requires integrated actions across those levels. In this sense, the spectrum is similar to ecological models used to organize objectives and intervention approaches (McLeroy et al., 1988; Stokols et al., 1996). Ecological models describe individual, interpersonal, organizational, environmental, and policy factors.
A framework conceptualizing prevention actions based on an ecological model is described in a prior IOM report about obesity (IOM, 2005). The way the ecological model has evolved to give rise to thinking about obesity on a broader systems level is discussed in Chapter 4.
Policy and Legislative Approaches
Increased recognition of obesity and especially childhood obesity as a public health crisis has spurred legislative, regulatory, and policy proposals at the national, state, county, and city levels. States and local communities have been more successful than national government agencies in passing and implementing such proposals (IOM, 2009a,b). Referring to Figure 2-2, these are examples of strategies and actions undertaken by the government sector. In the case of reducing consumption of sugar-sweetened beverages and high-calorie, energy-dense foods, policy and legislative approaches might include limiting the availability of these products in certain environments (such as schools) or programs (such as federal nutrition assistance programs), imposing taxes or price increases on them, or mandating a reduction in their standard serving sizes. In the case of increasing physical activity, examples of policy and legislative approaches are requirements and funding for bike paths, mixed land use, parks, and safe routes to school; physical activity requirements for schools and child care centers; and taxes on gasoline.
For the most part, such population-based initiatives are not “proven.” That is, they are not yet supported by a strong evidence base showing that they will bring about improved dietary habits, increased physical activity, or reduced obesity at the population level; rather, they are based on extrapolations from clinical trials, expert opinion, previous experience, or promising practices (Brownson et al., 2006; IOM, 2009a; Khan et al., 2009). Nonetheless, because obesity is epidemic, there has been demand in some communities to take immediate action.
Approaches Involving Changes in Organizational Policies, Environments, and Practices
To reach the population, strategies should be implemented across many organizational settings. Referring to Figure 2-2, these settings correspond to strategies and actions involving programs, coalitions, coordination, and collaboration. Examples of organizational settings include child care facilities for younger children, schools for older children and adolescents, colleges for young adults, worksites for other adults, and senior centers for older adults. In addition, community organizations, faith-based settings, and primary care offices are important across the age spectrum (IOM, 2009b; Story et al., 2008). Relevant policies or programs could involve regulatory (mandatory) changes that affect an organization or voluntary changes that could be implemented by an organization itself. Examples of organizational initiatives include requiring restaurants to post the calorie content of their foods on menus; increasing
the availability of fruits and vegetables in a worksite cafeteria; and limiting the availability of sugar-sweetened beverages and high-calorie, energy-dense foods in a school. The relative cost of foods served or sold in worksite cafeterias, schools, or community settings might be adjusted. Requirements for physical education and recess in schools, child care settings, and aftercare settings might be instituted and enforced at the federal or state level, but also at the organizational level. Schools might implement training programs to enable teachers to offer nutrition or physical education, provide financial support for programs and services related to weight control, or keep school recreational facilities open after hours for community use. The appeal of such setting-based approaches includes the ability to work with a “captive audience”; provide age- and developmentally appropriate activities; and influence social norms within the setting, with possible transfer to behavior outside of the setting.
Approaches Designed to Foster Changes in Communities and Neighborhoods
Many obesity prevention efforts are undertaken at the local or community level; those focusing on childhood obesity have tended to concentrate on local, district, or state school policies that impact nutrition and/or physical activity opportunities. Policy changes are often easier at the local level because they may be able to be accomplished without the same intensity of representation of vested interests, or through relatively agile regulatory bodies rather than through legislation (IOM, 2009a,b). According to testimony from the Assistant Commissioner of the New York City Department of Health at a public workshop convened by the committee (January 8, 2009), in deciding what strategies to pursue, the department targeted actions that the city could influence through regulations under its jurisdiction. A single individual, community organization, or stakeholder is also apt to have greater influence or power at the local level because opposition at the state (or national) level is likely to be more organized and better financed. Furthermore, it may be easier to achieve consensus at the local than at the state level. An individual or a few committed people can often move an agenda item forward quickly and play a greater role in ensuring its implementation because of the smaller, more manageable scale. Strategy planners at the local level are also more likely to be sensitive to context—they know what is feasible, practical, and acceptable in a particular setting. Different types of evidence—for example, more locality-specific—may be needed for smaller-scale, locally controlled policies that will not encompass a wide variety of settings. Local actions may, therefore, be less vulnerable to the greater costs and inertia entailed in larger-scale policies.
In many cases, policy initiatives were first implemented at the local or community level before being implemented more broadly across a state. Mirroring the history of tobacco control efforts, this scaling up of implementation has been undertaken in current policy and environmental efforts to improve nutrition, increase physical activity, and reduce sedentary activities (IOM, 2009a; Khan et al., 2009). After a pioneering locality develops an intervention, tests its feasibility, and assesses public support and
opposition, and the idea becomes less novel over time, similar interventions are implemented more readily in other settings. In addition, legal challenges may have been part of the process. For example, New York City was not successful in implementing calorie posting on menus on the first try (Mello, 2009) because of a successful legal challenge. The city promulgated an amended calorie labeling law in January 2008, after which the courts ruled in its favor against the New York State Restaurant Association. After the second ruling, other New York counties copied much of the New York City language in their legislative proposals in hopes of avoiding a legal challenge.
Examples of strategies and actions that might be undertaken by communities and neighborhoods to improve dietary behaviors include advocating for zoning that limits fast food establishments, facilitating the situating of supermarkets in underserved neighborhoods (based on observational data that access to a supermarket is associated with better dietary quality and/or increased fruit and vegetable intake [Larson et al., 2009; Lovasi et al., 2009; Moore et al., 2008; Morland et al., 2002; Zenk et al., 2009]), increasing the availability of farmers’ markets, and creating and supporting community gardens. Examples of strategies and actions to increase physical activity include supporting safe routes to school, creating and maintaining a walking school bus, increasing the number of parks and bike paths, and enhancing walking infrastructure (IOM, 2009a).
Two recent reports recommend community-based policy and environmental strategies and associated measurements that local governments and communities can use to plan, implement, and monitor population-level initiatives designed to prevent obesity (IOM, 2009a; Khan et al., 2009). For most of the strategies, the evidence is insufficient to determine effectiveness in changing caloric intake, physical activity, and/or obesity prevalence; for some of the strategies, there is no evidence, only theoretical projections. One of the reports (IOM, 2009a) summarizes the strength of the evidence (from intervention or observational studies to related nonresearch sources) and recommends a number of “promising” policy strategies, apart from school-based interventions, based on their anticipated effect and projected reach. Both reports are notable in that the majority of the strategies recommended are not evidence-based because, for the most part, strong evidence that they will achieve the desired outcomes is not available. Nonetheless, these reports, which recommend a number of the same strategies, are a useful starting point for local governments, communities, and organizations seeking guidance on where to focus their efforts. Although not intended as such, they may also be useful guides for federal agencies and/or legislators in their strategic thinking about policies to control obesity.
Health Communication and Social Marketing Approaches
Strategies and actions to prevent obesity can be enhanced through communication, marketing and promotion, and new technologies, as shown in Figure 2-2. Documentaries and television specials have captured the attention of the public and
the broader media in pointing out some of the marketing tactics used by the food industry to increase consumption of certain foods. Increased awareness of the health and societal costs associated with excess caloric intake from sugar-sweetened beverages and high-calorie, energy-dense foods has led to social pressure to decrease efforts to encourage overeating and supersizing of meals at some fast food establishments. In addition, government organizations such as CDC and the Produce for Better Health Foundation have developed a campaign promoting fruits and vegetables (Foerster et al., 1995), while CDC sponsored the VERB™ campaign to increase and maintain physical activity among youth (Wong et al., 2004).
Interventions in Health Care Settings
While there is little conclusive evidence that health care interventions can prevent obesity, screening to ensure early detection of diseases/conditions and anticipatory guidance and health promotion counseling are hallmarks of any preventive health care program. For children aged 2-20, annual screening for obesity using sex-specific BMI-for-age percentiles, accompanied by preventive counseling about diet and physical activity, is recommended by professional organizations including the National Institutes of Health (NIH), Centers for Disease Control and Prevention (CDC), the American Academy of Pediatrics, and the American Academy of Family Physicians.
National surveillance of objective measures of obesity (based on measured height and weight) is limited to the National Health and Nutrition Examination Survey (NHANES), which does not provide state-, county-, or local-level estimates of obesity. Some states have worked through health care providers for surveillance purposes, while other states and cities have mandated screening of students for obesity or assessment of weight status based on BMI percentiles. In New York State, managed care programs have been required since 2005 to report as a quality indicator the percentage of adolescents who were screened for obesity (based on sex-specific BMI-forage percentiles), counseled about nutrition, and counseled about physical activity or exercise as part of their annual preventive visit. Beginning in 2006, these data were publicly reported. In 2006, screening for obesity among adolescent patients during preventive visits was 29, 26, and 23 percent for patients enrolled in Commercial, Medicaid, and Child Health Plus managed care programs, respectively (New York State Department of Health, 2006). By 2008, these percentages were 53, 61, and 59 percent, respectively (New York State Department of Health, 2008a,b,c). Other states or health plans could expand and/or further define those criteria to include more specific or detailed counseling. In addition, insurance coverage could be expanded to cover behavioral and nutritional counseling. Whether increased screening for obesity and increased preventive counseling about diet and physical activity will lead to reduced obesity is not yet known.
Multilevel, Multisector Obesity Prevention Approaches
Repeated calls for multilevel, multisector efforts to prevent obesity have been sounded by governments, scientific and professional societies, advocacy groups, and funding agencies at the local, state, and national and international levels (IOM, 2005; Sallis et al., 2006; Story et al., 2008). Because multilevel prevention approaches are less targeted than treatment practices and reach a broader audience, they are often seen as more equitable than single-level approaches (IOM, 2005). Most obesity treatment programs are limited in both reach and long-term success. For example, while obesity prevalence, and thus the need for treatment, is higher among low-income and ethnic minority children (see Chapter 1), these populations often have inadequate access to preventive and clinical health care services (Kumanyika et al., 2008). Furthermore, ethnic minority populations tend to be underrepresented in the obesity treatment literature, reflecting their limited access to (because of both location and eligibility requirements) and/or participation in research studies (Kumanyika, 2008).
Like tobacco control initiatives, multilevel, multisector approaches combining programmatic and policy interventions with strategic, culturally appropriate, high-impact messages can change the social norms around eating, physical activity, and life-style behaviors. But unlike tobacco control, obesity prevention does not have a single, easily defined “villain” devoid of redemptive qualities. Food is complex—it has associations with cultural and religious traditions and provides emotional comfort, essential nutrients, and sustenance. The art of food preparation, its presentation, and feeding behaviors can also be nurturing. Food cannot be dichotomized into good and bad. It is truly essential—just not in the quantity and proportions consumed by many people in the United States and other countries where obesity is prevalent. Obesity prevention approaches that combine strategies and actions at multiple levels of the spectrum of prevention are essential; the need for such approaches and their targeted behaviors and settings are discussed below.
The Need for a Multilevel Approach
Two essential tenets of the Dietary Guidelines for Americans, which are based on the best available evidence (and when necessary, expert opinion) and form the nation’s blueprint for a healthful diet, are that nutritional needs should be met through foods and beverages and that energy consumed must balance energy expended. Reducing the consumption of excess discretionary calories is a strategy that is both evidence-based and supported by expert opinion (USDA/HHS, 2005). Four of the six principal target areas identified by CDC to prevent and control obesity address specific dietary behaviors: decrease the consumption of sugar-sweetened beverages; reduce the consumption of high-calorie, energy-dense foods; increase the consumption of fruits and vegetables; and increase the initiation, duration, and exclusivity of breastfeeding.2 For
|
2 |
Available online: http://www.cdc.gov/obesity/stateprograms/index.html (accessed September 3, 2009). |
each behavioral target, the evidence base supporting its impact on caloric intake and/or obesity differs (Khan et al., 2009).
Because many factors influence these food and beverage consumption behaviors, an intervention in a single sector or setting will be of limited value. Target behaviors are affected by federal, state, and local policies, regulations, and/or legislation; organizational practices and policies; educational campaigns; and individual knowledge and skills. For example, the significant profit factor associated with sugar-sweetened beverages and highly processed high-calorie, energy-dense foods greatly impacts the promotion of these products. A large number of factors that may mediate, enable, or amplify the intake of sugar-sweetened beverages, highly processed high-calorie, energy-dense foods, and fruits and vegetables act at multiple levels and in a variety of sectors and settings. For example, food is accessible throughout the day in multiple settings; more processed foods are available in large portion sizes and at relatively low prices; an increasing number of calories are being consumed from foods away from home; energy-dense, nutrient-poor foods are readily available in the school food environment and in the fast food and convenience store outlets in low-income urban areas; and food marketing to children has increased over the past 30 years (IOM, 2005, 2006).
Example of a Multilevel Approach: Childhood Obesity Prevention in Texas
Table 2-1 shows the efforts of an array of individuals, organizations, lawmakers, public officials, community leaders, and organizations to develop, implement, and evaluate strategies to prevent and reverse childhood obesity in Texas. A summary of a workshop convened by the IOM explains these efforts in more detail (IOM, 2009c). Texas has one of the highest obesity rates in the nation. It is home to three of the five cities with the highest obesity rates nationwide, and in 2007 two-thirds of its adult population was obese. The state’s efforts target youth, with the aim of instilling healthful behaviors and lifestyles to last a lifetime. A guiding principle is that these efforts should be “evidence based, community specific, sustainable, cost-effective, and supported by effective partnerships.” A goal is for the “responsibility to be broadly shared by individuals, families, communities, and the public and private sectors” (IOM, 2009c, p. 2).
The state’s notable achievements have included mandating nutrition standards for school meals and vending machines in schools and enacting three bills (championed by Texas State Senator Jane Nelson) that reinstated and mandated minimum physical education requirements for elementary and middle school students in public schools and required physical fitness testing of youth in grades 3-12. It is worth noting how this was accomplished, which illustrates the importance of jurisdictional oversight in accomplishing such goals. After proposed legislation to implement school nutrition standards was unsuccessful in 2003, jurisdictional control of the nutritional environment in the public schools was shifted from the Texas Education Agency to the Texas Department of Agriculture (under the leadership of Susan Combs). This allowed the state to issue the Texas Public School Nutrition Policy, which banned foods of
TABLE 2-1 Multilevel, Multisector Approach to Childhood Obesity Prevention in Texas
|
Theme |
Strategy |
Rationale |
Examples |
|
Garnering support |
|
|
|
|
• Buy-in from the public |
Focus on children and schools |
Engage community members |
Business leaders, parents, educators on committees |
|
• Buy-in from legislators |
Public education |
Legislation, Senate Bills 19, 42, 530; Texas public school nutrition policy |
Minimum physical education standards, fitness testing; nutrition standards for meals, vending machines |
|
Modeling healthful behaviors in the community |
Extend efforts beyond schools to worksites |
Improve the fiscal bottom line; reduce health care costs |
Workplace wellness programs; state employees |
|
Leveraging the power of partnerships |
Collaborative efforts; community-based solutions |
Generate greater momentum, resources, and influence |
Elected officials, state agencies, schools, worksites, higher education, urban planners, parents |
|
Implementing comprehensive approaches |
Multilevel and multisector: schools, communities, media, treatment, law enforcement |
More effective than single-level interventions |
Modeled after Texas Tobacco Prevention Initiative |
|
Using social marketing |
Think and act like marketers |
Promote positive behaviors |
Promote a healthful lifestyle, not obesity prevention |
|
Identifying a champion |
Advance a specific cause (local level), lead by example (state level) |
Energize others, spread enthusiasm, communicate, unite people toward a common goal, leverage resources |
Implement a program or project, pass legislation, obtain funding, incentivize change |
|
Recognizing the power of community data |
Collect local, community data; culturally adapt; collect state data |
All politics are local; mobilize a call to action among decision makers |
Measure outcome of interventions, compare local and state performance |
|
Implementing federal policy change |
Advocate federal policy change |
Develop a foundation for states to build upon; create support for change at the community and state levels |
Support federal school nutrition, physical education and fitness standards |
|
Securing funding |
Needed to launch and sustain programs; innovation important, often overlooked |
Projects should be scalable, adaptable, and sustainable; funders tend to be risk-averse |
Government (federal, state, local), private foundations, universities, colleges, business community |
|
SOURCE: IOM, 2009c. |
|||
minimal nutritional value in elementary schools. After the laws requiring physical education in schools were passed, not all schools implemented physical education programs, illustrating the importance of ensuring that such laws are implemented and enforced. Nelson and Combs worked to gain public support and to gather and present data that would make a compelling case for the need for efforts to prevent obesity. When Combs became Texas State Comptroller, she was able to leverage her role in controlling the state finances to institute a grant program that covers the costs
of providing physical education for middle schools attended by at least 75 percent educationally and economically disadvantaged students. It should also be noted that researchers helped develop, implement, and evaluate the Coordinated Approach to Child Health program, which has been implemented in 2,500 schools in the state. The physical fitness test that is used, the Fitnessgram, was also developed in Texas (by the Cooper Institute).
While Texas has made significant progress in changing state policies, improving the school nutrition environment, increasing students’ opportunities for regular high-quality physical education, and putting evaluation systems in place, the work is not done. The state will be guided in developing best practices for the prevention and control of obesity by ensuring that these coordinated school nutrition, physical education, and health initiatives are implemented in all Texas schools; continuing to improve nutrition education and access to healthful foods; promoting worksite wellness programs; supporting comprehensive evidence-based community initiatives; and monitoring the impact of these efforts. A starting point for policy adoption, the Texas Obesity Policy Portfolio, was created by the Texas State Health Services Department to provide a basis for a comprehensive approach to decision making (Texas Department of State Health Services, 2006). This report is a compilation of current and proposed evidence-based obesity policy options along with their respective levels of effectiveness (untested, promising, effective), as described by the Washington State Department of Health (2005).
Conclusion
Many approaches to obesity prevention supported by varying degrees of evidence could be and are being implemented in multiple settings, cities, local communities, and states. Yet identifying where, how, and what is being done is challenging. Evaluating the process, implementation, and/or outcome of an approach is even more difficult and often is not being done at all. To address this gap, CDC has conducted a systematic review of the published literature and sought expert opinion to identify and recommend means of achieving some uniformity in approach and outcome measures (Khan et al., 2009). The results of this effort will potentially allow pooling of findings (see Chapter 8), making it easier to assess the implementation of an approach and its effectiveness and public health impact. Finally, obesity prevention initiatives need to be viewed in a broader health context and should encompass long-term, multigenerational goals, and obesity prevention policies need to be applied in a broad range of settings to achieve long-term movement toward better health.
OBESITY PREVENTION STRATEGIES IN THE BROADER CONTEXT OF OTHER PUBLIC HEALTH INITIATIVES
Strategies used to address other public health epidemics and crises, including the significant progress made in tobacco control, may be applicable in addressing the obe-
sity epidemic (see Table 2-2) (Economos et al., 2001; Mercer et al., 2003). When the Report of the U.S. Surgeon General on smoking and health (Public Health Service, 1964) first concluded that cigarette smoking was a health hazard of sufficient importance to warrant appropriate remedial action, the evidence base regarding which strategies would be most cost-effective and/or efficacious was limited. Some 30 years later, the most promising approaches and strategies were collected and published as Best Practices for Comprehensive Tobacco Control Programs (CDC, 1999), later revised to include the accumulated evidence and strengthened science base (CDC, 2007). According to that report, the most successful efforts combined (1) comprehensive
TABLE 2-2 Strategies to Address Other Public Health Problems: Lessons for Obesity Prevention
|
Strategy |
Other Public Health Problems |
Obesity Prevention |
|
Promote health (media) |
|
|
|
Provide information |
|
|
|
Use pricing |
|
|
|
Limit advertising |
|
|
|
Restrict access to products |
|
|
|
Protect public from second-hand exposure |
|
|
|
Require insurance coverage for treatment or prevention |
|
|
|
Frame as public health problem; change social norms and expectations |
|
|
and coordinated programmatic and policy interventions designed to influence social norms, systems, and networks; and (2) effective, sustained, and adequately funded health communication campaigns that delivered strategic, culturally appropriate, high-impact messages (CDC, 2007). Policy changes to reduce tobacco use included increasing the unit price (taxation), protecting the public from tobacco smoke (clean indoor air legislation), limiting minors’ access to tobacco products, and providing insurance coverage for tobacco cessation/treatment programs (CDC, 2007). Because it is presumed that sustainable changes occur through shifts in the social environment, the report advocates interventions that influence the societal organizations, systems, and networks that facilitate desired behavior changes.
Other public health initiatives and social changes that require intervention targeting diverse groups at multiple levels may be analogous to obesity prevention (Economos et al., 2001).3 Lessons from a range of successful attempts at social change, including increasing breastfeeding rates, seat belt use, and recycling, reveal similar keys to success. These include recognition that there was a crisis; major economic implications associated with the crisis; a science base including research, data, and evidence; leaders who could work for their cause through their knowledge, competence, talents, skills, and even cunning and charisma; coalitions to move the agenda forward and a strategic, integrated media advocacy campaign; involvement of the government at the state level to write and implement legislation and at the local level to implement change; mass communication that included consistent positive messages supported by scientific consensus and was repeated in a variety of venues; policy and environmental changes that promoted healthful behaviors; and a plan that included many components that worked synergistically (Economos et al., 2001).
Such approaches characterize the multilevel, multisector obesity prevention strategies that have been called for by governments, scientific and professional societies, advocacy groups, and funding agencies at the local, state, and national and international levels. Because many factors influence obesity-related behaviors, such strategies are believed to offer the best chances for success in obesity prevention.
REFERENCES
Brownson, R. C., D. Haire-Joshu, and D. A. Luke. 2006. Shaping the context of health: A review of environmental and policy approaches in the prevention of chronic diseases. Annual Review of Public Health 27:341-370.
CDC (Centers for Disease Control and Prevention). 1999. Best practices for comprehensive tobacco control programs—April 1999. Atlanta, GA: U.S. Department of Health and Human Services, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health.
CDC. 2007. Best practices for comprehensive tobacco control programs—October 2007. Atlanta, GA: Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health.
|
3 |
Available online at http://www.preventioninstitute.org/tool_spectrum.html (accessed September 3, 2009). |
CDC. 2009. Division of nutrition, physical activity, and obesity. http://www.cdc.gov/nccdphp/dnpao/aboutus/index.html (accessed November 30, 2009).
Cohen, L., and S. Swift. 1999. The spectrum of prevention: Developing a comprehensive approach to injury prevention. Injury Prevention 5(3):203-207.
Economos, C. D., R. C. Brownson, M. A. DeAngelis, S. B. Foerster, C. Tucker Foreman, J. Gregson, S. K. Kumanyika, and R. R. Pate. 2001. What lessons have been learned from other attempts to guide social change? Nutrition Reviews 59(3, Supplement 2):S40-S46.
Foerster, S. B., K. W. Kizer, L. K. DiSogra, D. G. Bal, B. F. Krieg, and K. L. Bunch. 1995. California’s ‘5 a day—for better health!’ campaign: An innovative population-based effort to effect large-scale dietary change. American Journal of Preventive Medicine 11(2):124-131.
HHS (U.S. Department of Health and Human Services). 2008. 2008 physical activity guidelines for Americans. Office of Disease Prevention and Health Promotion Publication No. U0036. Washington, DC: U.S. Department of Health and Human Services.
IOM (Institute of Medicine). 1995. Weighing the options: Criteria for evaluating weight-management programs. Edited by P. R. Thomas. Washington, DC: National Academy Press.
IOM. 2005. Preventing childhood obesity: Health in the balance. Edited by J. Koplan, C. T. Liverman, and V. I. Kraak. Washington, DC: The National Academies Press.
IOM. 2006. Food marketing to children and youth: Threat or opportunity? Edited by J. M. McGinnis, J. Gootman and V. I. Kraak. Washington, DC: The National Academies Press.
IOM. 2007. Progress in preventing childhood obesity: How do we measure up? Edited by J. Koplan, C. T. Liverman, V. I. Kraak, and S. L. Wisham. Washington, DC: The National Academies Press.
IOM. 2009a. Local government actions to prevent childhood obesity. Edited by L. Parker, A. C. Burns, and E. Sanchez. Washington, DC: The National Academies Press.
IOM. 2009b. Community perspectives on obesity prevention in children: Workshop summaries. Edited by P. T. Whitacre and A. C. Burns. Washington, DC: The National Academies Press.
IOM. 2009c. Childhood obesity prevention in Texas: Workshop summary. Edited by K. Nyberg, A. C. Burns and L. Parker. Washington, DC: The National Academies Press.
Khan, L. K., K. Sobush, D. Keener, K. Goodman, A. Lowry, J. Kakietek, and S. Zaro. 2009. Recommended community strategies and measurements to prevent obesity in the United States. Morbidity and Mortality Weekly Report 58(RR-7):1-26.
Kumanyika, S. 2008. Ethnic minorities and weight control research priorities: Where are we now and where do we need to be? Preventive Medicine 47(6):583-586.
Kumanyika, S., R. W. Jeffery, A. Morabia, C. Ritenbaugh, and V. J. Antipatis. 2002. Obesity prevention: The case for action. International Journal of Obesity 26(3):425-436.
Kumanyika, S. K., E. Obarzanek, N. Stettler, R. Bell, A. E. Field, S. P. Fortmann, B. A. Franklin, M. W. Gillman, C. E. Lewis, W. C. Poston II, J. Stevens, and Y. Hong. 2008. Population-based prevention of obesity: The need for comprehensive promotion of healthful eating, physical activity, and energy balance: A scientific statement from American Heart Association Council on Epidemiology and Prevention, Interdisciplinary Committee for Prevention (formerly the Expert Panel on Population and Prevention Science). Circulation 118(4):428-464.
Larson, N. I., M. T. Story, and M. C. Nelson. 2009. Neighborhood environments: Disparities in access to healthy foods in the U.S. American Journal of Preventive Medicine 36(1):74-81.e10.
Lovasi, G. S., M. A. Hutson, M. Guerra, and K. M. Neckerman. 2009. Built environments and obesity in disadvantaged populations. Epidemiologic Reviews 31:7-20.
McLeroy, K. R., D. Bibeau, A. Steckler, and K. Glanz. 1988. An ecological perspective on health promotion programs. Health Education Quarterly 15(4):351-377.
Mello, M. M. 2009. New York City’s war on fat. New England Journal of Medicine 360(19):2015-2020.
Mercer, S. L., L. W. Green, A. C. Rosenthal, C. G. Husten, L. K. Khan, and W. H. Dietz. 2003. Possible lessons from the tobacco experience for obesity control. The American Journal of Clinical Nutrition 77(4, Supplement):1073S-1082S.
Moore, L. V., A. V. Diez Roux, J. A. Nettleton, and D. R. Jacobs, Jr. 2008. Associations of the local food environment with diet quality—a comparison of assessments based on surveys and geographic information systems: The multi-ethnic study of atherosclerosis. American Journal of Epidemiology 167(8):917-924.
Morland, K., S. Wing, and A. Diez Roux. 2002. The contextual effect of the local food environment on residents’ diets: The atherosclerosis risk in communities study. American Journal of Public Health 92(11):1761-1767.
New York City Department of Health and Mental Hygiene. 2009. New campaign asks New Yorkers if they’re “pouring on the pounds”. http://www.nyc.gov/html/doh/html/pr2009/pr057-09.shtml (accessed March 8, 2010).
New York State Department of Health. 2006. 2006 New York State managed care plan performance: A report on quality, access to care, and customer satisfaction. http://www.health.state.ny.us/health_care/managed_care/qarrfull/qarr_2006/qarr2006.pdf (accessed April 5, 2010).
New York State Department of Health. 2008a. Adolescent preventive care—statewide— commercial managed care. http://www.health.state.ny.us/health_care/managed_care/reports/eqarr/2008/statewide/commercial/adolescent_preventive_care.htm (accessed April 6, 2010).
New York State Department of Health. 2008b. Adolescent preventive care—statewide— Medicaid managed care. http://www.health.state.ny.us/health_care/managed_care/reports/eqarr/2008/statewide/medicaid/adolescent_preventive_care.htm (accessed April 6, 2010).
New York State Department of Health. 2008c. Adolescent preventive care—statewide—child health plus managed care. http://www.health.state.ny.us/health_care/managed_care/reports/eqarr/2008/statewide/child_health_plus/adolescent_preventive_care.htm (accessed April 6, 2010).
Public Health Service. 1964. Smoking and health: Report of the Advisory Committee to the Surgeon General of the Public Health Service. Public Health Service Publication No. 1103. Washington, DC: U.S. Department of Health, Education, and Welfare.
Public Health Service. 2001. The Surgeon General’s call to action to prevent and decrease overweight and obesity. Rockville, MD: U.S. Department of Health and Human Services.
Rattray, T., W. Brunner, and J. Freestone. 2002. The new spectrum of prevention: A model for public health practice. Martinez, CA: Contra Costa Health Services.
Sallis, J. F., R. B. Cervero, W. Ascher, K. A. Henderson, M. K. Kraft, and J. Kerr. 2006. An ecological approach to creating active living communities. Annual Review of Public Health 27:297-322.
Stokols, D., J. Allen, and R. L. Bellingham. 1996. The social ecology of health promotion: Implications for research and practice. American Journal of Health Promotion 10(4):247-251.
Story, M., K. M. Kaphingst, R. Robinson-O’Brien, and K. Glanz. 2008. Creating healthy food and eating environments: Policy and environmental approaches. Annual Review of Public Health 29:253-272.
Texas Department of State Health Services. 2006. Texas obesity policy portfolio. Austin, TX: Center for Policy and Innovation.
USDA (U.S. Department of Agriculture)/HHS. 2005. Dietary guidelines for Americans, 6th ed. Home and Garden Bulletin No. 232. Washington, DC: U.S. Government Printing Office.
Washington State Department of Health. 2005. Nutrition and physical activity: A policy resource guide. http://www.dshs.state.tx.us/obesity/pdf/WAnutritionphysicalactivityguide.pdf (accessed December 1, 2009).
WHO (World Health Organization). 2000. Obesity: Preventing and managing the global epidemic. Report of a WHO consultation. WHO Technical Report Series 864. Geneva: World Health Organization. http://www.who.int/nutrition/publications/obesity/en/index.html.
WHO. 2003. Diet, nutrition, and the prevention of chronic diseases. Report of a joint WHO/ FAO expert consultation. WHO Technical Report Series 916. Geneva: World Health Organization.
WHO. 2004. Global strategy on diet, physical activity, and health. Geneva: World Health Organization.
Wong, F., M. Huhman, C. Heitzler, L. Asbury, R. Bretthauer-Mueller, S. McCarthy, and P. Londe. 2004. VERB™——a social marketing campaign to increase physical activity among youth. Preventing Chronic Disease 1(3):1-7.
World Cancer Research Fund and American Institute for Cancer Research. 2007. Food, nutrition, physical activity, and the prevention of cancer: a global perspective. Washington, DC: American Institute for Cancer Research.
Zenk, S. N., L. L. Lachance, A. J. Schulz, G. Mentz, S. Kannan, and W. Ridella. 2009. Neighborhood retail food environment and fruit and vegetable intake in a multiethnic urban population. American Journal of Health Promotion 23(4):255-264.




















