1
Introduction
On October 1 and 2, 2009, a group of human factors and other experts met to consider a diverse range of behavioral and human factors issues associated with the increasing migration of medical devices, technologies, and care practices into the home. The Committee on the Role of Human Factors in Home Health Care organized the event to gather information on a topic on which relatively little has been established empirically, although it is increasingly clear that more and more health care is being delivered in homes. Part I of this volume is a summary of the presentations and discussions that took place at the Workshop on the Role of Human Factors in Home Health Care.
THE ROLE OF HUMAN FACTORS IN HOME HEALTH CARE1
A standard textbook definition characterizes the field of human factors research as “the discipline that takes into account human strengths and limitations in the design of interactive systems that involve people, tools and technology, and environments to ensure their safety, effectiveness, and ease of use.” This definition can easily be modified to apply to human factors in home health care said Kerm Henriksen during his opening remarks at the workshop:
The field of human factors in home health care takes into account provider and recipient capabilities in the design of interactive home care systems of people, devices and technology, and environments to ensure their safety, effectiveness, and ease of delivering care.
Figure 1-1 provides a more detailed characterization of the role of human factors in home health care. From the perspective of the care recipient, the ultimate goal is to ensure the delivery of high-quality care in the home and to avoid preventable adverse events, as shown at the bottom of the figure. A host of factors must come together for this objective to be achieved, Henriksen observed. The factors closest to the recipient that can cause adverse events are the characteristics of the provider and the recipient. (These are labeled as “active errors” in the figure.) Factors more distant from the recipient (labeled “latent conditions”) can also result in deficiencies in care. These factors include the nature of home health care tasks and the characteristics of the physical environment, of medical devices and technologies, and of the social or community environment. Exerting an even broader influence are factors in the external environment, including demographic, economic, and political factors. Thus, recipients and providers “inherit the sins of omission and commission of everybody else who has played a role in the design of the greater sociotechnical system,” said Henriksen.
Human factors research has a long track record of addressing challenging issues in demanding environments, particularly when it is able to address issues in the context of integrated systems. But systems thinking has not come easily to home health care, Henriksen said. Homes are not designed for health care, and considerable variation exists in what constitutes a home. Recipients and providers, whether formal or informal, have considerable variation in knowledge and skills. Many lay providers are themselves care recipients, as the provider workforce ages. Hazards in the home are often unrecognized, and home health care providers have limited experience with medical devices and medical information technologies. Home and community culture and environments are extremely variable. And health care reform often tends to mean doing more with less.
A comprehensive study of the role of human factors in home health care faces a challenging set of goals:
-
Achieve an in-depth understanding of the human factors challenges underlying safe and high-quality home health care.
-
Specify critical gaps in understanding.
-
Develop an integrated framework to guide research across the major components and disciplines relevant to safe delivery of care in the home.
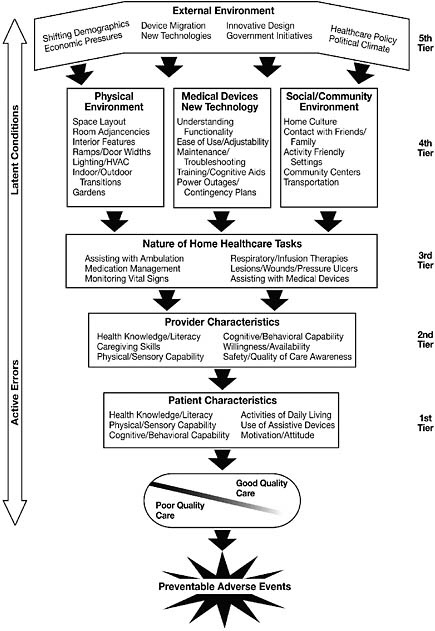
FIGURE 1-1 Factors that influence the safety, quality, and effectiveness of home health care range from the immediate characteristics of recipients and providers (Tiers 1 and 2) to aspects of home health care tasks, technologies, and environments (Tiers 3, 4, and 5).
SOURCE: K. Henriksen, Anjali, J., and Zayas-Caban, T. (2009). The human factors of home health care: A conceptual model for examining safety and quality concerns. Journal of Patient Safety, 5(4), 229-236. Reprinted with permission of Wolters Kluwer Health.
-
Develop guidelines for those involved in the design, development, and implementation of health information technology in the home.
-
Provide a roadmap for needed research.
Given the rapid increases in home health care that have already occurred and will continue to occur, the overall goal, said Henriksen, must be to “provide a wake-up call for home health care policy.”
WORKSHOP THEMES
Nine presentations, given in three half-day sessions, summarized the main conclusions of the background papers prepared for the workshop by experts in human factors and home health care. The first session covered the people who receive and provide home health care. The second session looked at the tools and technologies involved in the delivery of home health care, and the third session focused on the physical and social environments in which home health care occurs. At the end of each session, a discussant highlighted important points, fielded questions, and moderated an exchange among the presenters, committee members, and workshop participants on the topics covered during the session. At the end of the workshop, the committee chair, David Wegman, moderated a final discussion of the most important observations and conclusions to emerge from the workshop as a whole.
ORGANIZATION OF THE REPORT
Part I is a summary of the workshop event. This chapter gives the context in which the workshop took place. Chapters 2, 3, and 4 summarize the presentations and discussions that occurred during each of the three sessions. Chapter 5 describes the main points made in the final wrap-up session.
Part II contains individually authored papers written for the workshop and consists of Chapters 6 through 12. The Appendix presents the workshop agenda and list of participants.
It is important to be specific about the nature of the workshop summary (Part I), which documents the information presented in the workshop presentations and discussions. Its purpose is to lay out the key ideas that emerged from the workshop, and it should be viewed as an initial step in examining the research and applying it in specific policy circumstances. The report is confined to the material presented by the workshop speakers and participants. Neither the workshop nor this summary is intended as a comprehensive review of what is known about human factors in home health care, although it is a general reflection of the literature. The presentations and discussions were limited by the time available for the workshop. A
more comprehensive review and synthesis of relevant research knowledge will have to await the committee’s consensus report.
This report was prepared by a rapporteur and does not represent findings or recommendations that can be attributed to the planning committee. Indeed, the report summarizes views expressed by workshop participants, and the committee is responsible only for its overall quality and accuracy as a record of what transpired at the workshop. Also, the workshop was not designed to generate consensus conclusions or recommendations but focused instead on the identification of ideas, themes, and considerations that contribute to understanding of human factors in home health care. The insights of the presenters and workshop participants constitute extremely useful input for the committee’s continuing work.






