7
Nursing Research
Research training in nursing prepares investigators to create new scientific knowledge to guide nursing practice, assess the health care environment, improve patient, family, and community outcomes, and influence health policy.
The science of nursing is focused on the development of knowledge to: (1) build the scientific base for clinical practice; (2) prevent disease and disability; (3) manage and eliminate symptoms caused by illness; and (4) enhance end-of-life and palliative care.1 As described by Donaldson and Crowley, such research is characterized by three themes of inquiry that relate to human well-being: (1) principles and laws that govern life processes and offer maximum optimum function during illness and health; (2) patterns of human behavior in interaction with the environment in critical life situations; and (3) processes by which positive changes in health status are affected.2 Thus, nursing studies serve to integrate the full range of biobehavioral responses of human beings.
As in many health care disciplines, much of nursing practice is not currently based on high-quality evidence. The major objective of modern nursing science is to develop the knowledge base on which to plan the most effective health care. Such research may range from fundamental basic laboratory research to community-based and translational research to improve care of groups highly susceptible to a range of different diseases.
The prevention of disease or disability is a major focus of nursing research along with a strong focus on health promotion and risk reduction across a wide spectrum of individuals and disease conditions. This approach is well exemplified by the following example of a school-based program adopted by most North Carolina schools. It is a health promotion program in exercise and diet for young children at risk for cardiovascular disease. The research results from this prevention-based program are impressive; the young people’s total cholesterol levels and measurements of body fat were significantly reduced following the education and exercise interventions, and their fitness levels, physical activity, and knowledge about cardiovascular disease risk factors improved.3
Preventing the complications of chronic disease is also a major area for research in nursing. Some of this work develops ways to help individuals and families cope with long-term chronic disease. For example, a program targeting better self-management of Type 1 diabetes examined the effectiveness of specific coping skills; the results of the study showed both improved metabolic control and higher quality of life in adolescents who used the skills. The program has been adopted in more than 100 clinical programs.4
Nursing care and research have traditionally addressed strategies for the management of symptoms associated with illnesses or their treatment. For example, in a study that focused on developing a longer-acting pain medication, investigators found that gender is a major factor in whether drugs are effective. Women responded well to seldom-used kappa-opioid drugs, but men had little benefit from those drugs.5
Influencing, redesigning, and shaping the environment for patients, families, and communities is another major area of study in nursing. Many studies have shown the influence of nursing surveillance and presence on positive patient outcomes. A shortage of nurses, a critical factor in the current health care environment, has been demonstrated to increase patient mortality and morbidity. Other studies show the benefit of home visits by advanced practice nurses in improving the health and quality of life of elders being discharged from the hospital.6
Research in nursing is often referred to as “nursing science” or “nursing research,” which has led some to confuse it with the nursing profession. This terminology exists at the National
|
1 |
NINR. 2006. NINR Strategic Plan, Pub No. 06-4832. Online at http://www.ninr.nih.gov/AboutNINR/NINRMissionandStrategicPlan/. |
|
2 |
Donaldson, S.K., and D.M. Crowley. 1978. The discipline of nursing. Nursing Outlook 26(Feb):113-120. |
|
3 |
NINR Strategic Plan, 2006, p. 26. |
|
4 |
NINR Strategic Plan, 2006, p. 27. |
|
5 |
NINR Strategic Plan, 2006, p. 28. |
|
6 |
NINR Strategic Plan, 2006, p. 28. |
Institutes of Health (NIH) in the name of the National Institute for Nursing Research (NINR); however, the funding from NINR supports scientific research relevant to the science of nursing, and the investigators may be nurses or non-nurses.
The conditions needed for training in nursing research described in the 2005 NRC report hold true today:
Research training for nurses, as for other biomedical and behavioral researchers, needs to occur within strong research-intensive environments that typically will be in universities and schools of nursing. Important characteristics of these training environments include an interdisciplinary cadre of researchers and a strong group of nursing research colleagues who are senior scientists with consistent extramural review and funding of their investigative programs and obvious productivity in terms of publications and presentations. These elements are essential to the environment required for excellence in research training. (NRC, 2005, p. 73)
To encourage the development of research training in nursing, NINR devotes at least 7 percent of its funds to research training—about double what is found in other Institutes. The committee supports this priority as critical to the future of nursing research.
CHANGING THE CAREER TRAJECTORY FOR NURSE-SCIENTISTS
Changing the career trajectory for nurse-researchers involves three major efforts: (1) enhancing sustained productivity for nurse-scientists to promote an earlier and more rapid progression through the educational programs to doctoral and postdoctoral study; (2) responding to the shortage of nurse-investigators by increasing the number of individuals seeking doctoral education and faculty roles; and (3) emphasizing research-intensive training environments, including increased postdoctoral and career development opportunities.
ENHANCING SUSTAINED PRODUCTITY FOR NURSE-SCIENTISTS
Nurse-scientists play a critical role in the conduct of research and the generation of new knowledge that can serve as the evidence base for practice and the improvement of patient health outcomes. However, nurses enter Ph.D. programs mostly at a substantially later age than in any other biomedical or clinical science, limiting their years of potential scientific productivity. Faculty in many scientific fields starting their careers in their mid-30s may well have a research career of 30 to 40 years (to age 65-75). The average age of doctorally prepared nurse faculty, however, is 55.6 years [AACN data online]7, and the average age of retirement is 62.5 years—clearly limiting the productive years for nursing science and health practice in general. Nurse-investigators tend to have a shorter career span, thus limiting the development of nursing science and its application to nursing practice. Clearly a major driver in the short career span is the late stage at which nurse-scientists receive the Ph.D.
The fact that Ph.D. training for nurse-scientists occurs at such an advanced age (current assistant professors in nursing schools received the Ph.D. when they were 42.9 years) is a direct consequence of the traditional model for nurse-scientist training. The current path from the R.N. to the Ph.D. can be remarkably tortuous. After receiving the B.S.N. degree, nurses are encouraged to work in clinical practice, and indeed a subsequent application for admission to an M.S.N. program often requires several years of work experience. Again, after receipt of the M.S.N. degree, a period of additional clinical exposure is customary before entering a Ph.D. program. In addition, 65 percent of such doctoral students are unfunded (or only partly funded), and it is likely that these students work to cover their expenses. As a result, graduate students in nursing spend 8.3 to 15.9 years earning their doctorate after entering a master’s program,8 and the committee sees no sign that this trend is being reversed.
One way to help address this problem is to reduce the number of interruptions that nursing doctoral students experience. Once students enter undergraduate programs in nursing, students with interests in science should be identified early and encouraged to consider doctoral education and research. They should also have a chance to interact with nurse-scientists early in their undergraduate years. Several such programs have already been created.
In order to move undergraduates directly into doctoral education, nursing programs need to dispel the myth that students need clinical practice before entering graduate school. In fact, students interested in a research career may be best served by not earning a master’s degree first, as is the case in many scientific fields. In addition, certification requirements for advanced practice may add two years to master’s programs, further postponing entry into doctoral education. Funding that supports concurrent clinical and research training (similar to the MSTP) may facilitate movement into and through doctoral education.
The origins of the current educational structure in nursing and the hurdles it creates are summarized in the 2005 report:
Nursing developed both its Ph.D. and its D.N.Sc.9 programs to build on the master’s degree in nursing as well as to accommodate breaks between degrees for clinical practice. Early
|
7 |
AACN. Special Survey of Vacant Faculty Positions for Academic Year 2009-2020. Available at http://www/aacn.nche.edu/ids/pdf/vacancy09.pdf. |
|
8 |
National Opinion Research Center. 2001. Survey of Earned Doctorates. Unpublished special reports generated for the American Association of Colleges of Nursing. Chicago, IL: AACN. |
|
9 |
McEwen, M., and G. Bechtel. 2000. Characteristics of nursing doctoral programs in the United States. Journal of Professional Nursing. 16:282-292. |
reliance on the master’s degree is understandable in that it was nursing’s highest degree for many years before the establishment of a significant number of research doctoral programs. As doctoral programs were developed, they built on the master’s content, which at the time was predominantly research and theory focused. Over time the master’s programs have changed to become primarily preparation for advanced clinical practice, yet nursing continues to require the master’s degree for entry into doctoral study in most programs. Currently, very few doctoral programs in nursing admit baccalaureate graduates directly into the program, and for those that do, the master’s degree is usually required as a progression step. This requirement for entry into the Ph.D. program makes the group of advanced nurse-practitioners, rather than baccalaureate students, the major pool from which applicants are recruited into research. This is problematic in that this practitioner pool has the same demographic characteristics as the profession and thus is older in average age and more limited in diversity compared to applicants for science Ph.D. programs in general. Incorporation of the clinical/professional content from the master’s degree as foundational to the Ph.D. in nursing also encourages faculty to recruit and teach only nurses. Currently there are only a few doctorate programs in nursing that admit non-nurses.
Even though there are other fields that require a master’s degree as a requirement for earning the professional research doctorate, such as the M.P.H. for the Dr.P.H., the master’s degree has a completely different meaning relative to the science Ph.D. degree. The master’s degree is usually awarded as a “consolation prize” for students who are unable to complete the requirements for the science Ph.D. By making the master’s degree a requirement for its Ph.D. program, nursing has created confusion as to the meaning of the degree outside the nursing profession. (NRC, 2005, p. 74)
Nursing is both a practice profession that requires practitioners with clinical expertise and an academic discipline and science that requires independent researchers and scientists to build the body of knowledge. Each has a separate set of educational needs and goals. To improve the productivity and research focus of the Ph.D. in nursing, doctoral programs need to be structured to admit students directly from baccalaureate programs, to admit non-nurses, to decrease the number of years from high school to Ph.D. graduation, and to expand the interdisciplinary scope of their programs and research topics.
As outlined above, there is no consistent research career trajectory evident among practicing scientists in nursing today. The common thread is that they entered their doctoral programs later than most other scientists, and the majority have not benefited from postdoctoral education. As such, they bring with them rich clinical experiences that may help shape the focus of their inquiry. In addition, when nurses complete their doctoral education, most move directly into an academic career. There they frequently encounter a setting in which the demands for teaching and lack of pervasive research programs, socialization, and further mentoring make continuing progress as a scientist difficult.
RESPONDING TO THE SHORTAGE OF NURSE-INVESTIGATORS
It has been well established that not only is there both a current shortage but also there is a projected continued shortage of nursing faculty, especially those who are scientists and researchers. At this time, approximately 50 percent of the faculty teaching in nursing baccalaureate programs are doctorally prepared [AACN].10 This represents a marked increase from the 15 percent in the late 1970s. This 50 percent level was reached by 1999, but it has not increased since then despite a large increase in the number of doctoral degree programs available to nurses during the same time period. This is a reflection of two factors: (1) other than a modest increase in the number of doctoral degrees earned in 2007 and 2008, the yield of Ph.D. degrees has been largely static (even though the number of programs has increased, as shown in Table 7-1), and (2) the older age of graduates. The combination of these two factors suggests that an increasing number of doctorally prepared faculty will retire in the next few years, but there will not be an adequate number of new Ph.D.s to replace them. Nursing programs will be left with too few faculty members to conduct research and educate the next generation of scientists.
A 2009-2010 Special Survey of Vacant Faculty Positions conducted by the American Association of Colleges of Nursing (AACN) indicated that 90.6 percent of the vacancies require an earned doctoral degree [AACN],11 yet graduation rates from nursing doctoral programs are relatively flat. If there is any hope of filling a significant number of these faculty positions, both the NIH and nursing schools will need to provide incentives to increase the number of nurses who select a research career, and to do so early in their professional development.
CHARACTERISTICS OF NURSING PROGRAM FROM THE RESEARCH-DOCTORATE STUDY
The data in this section come from the NRC Research-Doctorate Study. The data from the study are valuable, because they provide unique information on program, faculty, and student characteristics. Although not time series data, they do provide a snapshot of nursing programs in 2006. Data were collected from 55 of the 85 programs that awarded Ph.D.s in nursing in 2006. Not all Ph.D.-granting institutions agreed to participate in the study, and only programs that averaged one Ph.D. or more per year submitted data. But these 55 programs educate a large proportion of the Ph.D.s in nursing, and their characteristics are generally representative of nursing programs. The data support the
|
10 |
AACN. 2009. American Association of Colleges of Nursing. 2008-2009 Enrollment and Graduations in Baccalaureate and Graduate Programs in Nursing. Washington, DC: AACN. Pub. no. 08-09-1. |
|
11 |
AACN. Special Survey of Vacant Faculty Positions for Academic Year 2009-2020. Available at http://www/aacn.nche.edu/ids/pdf/vacancy09.pdf. |
TABLE 7-1 Nursing Doctorates from U.S. Institutions, 1997-2008
|
|
1997 |
1998 |
1999 |
2000 |
2001 |
2002 |
2003 |
2004 |
2005 |
2006 |
2007 |
2008 |
|
Number of Doctorates |
420 |
399 |
353 |
414 |
363 |
437 |
413 |
394 |
422 |
415 |
483 |
505 |
|
Number of Males |
13 |
17 |
14 |
15 |
24 |
23 |
35 |
18 |
35 |
33 |
35 |
43 |
|
Number of Females |
406 |
380 |
337 |
399 |
335 |
414 |
378 |
376 |
387 |
382 |
448 |
462 |
|
Minorities |
24 |
22 |
29 |
21 |
31 |
30 |
38 |
42 |
35 |
42 |
43 |
51 |
|
Citizenship |
|
|
|
|
|
|
|
|
|
|
|
|
|
U.S. Citizen |
356 |
336 |
296 |
344 |
290 |
350 |
337 |
316 |
320 |
339 |
392 |
412 |
|
Permanent Resident |
11 |
11 |
8 |
9 |
10 |
7 |
7 |
11 |
9 |
11 |
11 |
14 |
|
Temporary Resident |
40 |
33 |
36 |
45 |
48 |
49 |
50 |
51 |
55 |
52 |
53 |
49 |
|
Unknown Status |
13 |
19 |
13 |
16 |
13 |
2 |
5 |
5 |
10 |
4 |
6 |
6 |
|
Postdoctoral Plans |
|
|
|
|
|
|
|
|
|
|
|
|
|
Postdoctoral Fellow |
12 |
12 |
7 |
20 |
23 |
29 |
21 |
23 |
21 |
37 |
22 |
33 |
|
Postdoctoral Research |
2 |
3 |
3 |
5 |
8 |
9 |
8 |
6 |
8 |
6 |
5 |
8 |
|
Postdoctoral Trainee |
0 |
0 |
0 |
1 |
0 |
1 |
2 |
0 |
2 |
1 |
2 |
2 |
|
Other Study |
0 |
3 |
6 |
4 |
5 |
5 |
2 |
4 |
2 |
9 |
2 |
2 |
|
Employment |
242 |
211 |
195 |
218 |
189 |
225 |
203 |
193 |
199 |
212 |
255 |
251 |
|
Other Plans |
5 |
11 |
4 |
8 |
5 |
10 |
5 |
4 |
2 |
8 |
3 |
7 |
|
Unknown Plans |
39 |
45 |
24 |
19 |
26 |
46 |
28 |
21 |
24 |
26 |
30 |
30 |
|
SOURCE: NSF. 2008. Survey of Earned Doctorates, 2008. Washington, DC: NSF. |
||||||||||||
finding elsewhere in this chapter concerning the aging of the faculty, the late age at which students receive a doctorate, and the need for additional training support at the doctoral and postdoctoral levels.
The Faculty
There are 1,471 faculty members in these 55 programs and the average size is 26, varying from a minimum of 8 to a maximum of 110. As is true of the profession in general, the faculty members are primarily female (7 percent male), and 14 of the programs have an all female faculty. Only 10 of the faculty with known citizenship were temporary residents. Most of the nursing faculty (88 percent) had an appointment in the nursing department or school, and only 12 percent were neither tenured nor on the tenure track (see Table 7-2). The percentage of assistant professors in other sciences ranges from 15 percent to 21 percent, and in nursing 31 percent of the tenure-track faculty are in that rank. This would suggest that either assistant professors in nursing are staying longer in this rank than in other sciences, or they tend to move out of the assistant professor faculty role into clinical positions at a significant rate, to be replaced by new Ph.D.s. A final possibility is that in 2006 the number of assistant professors of nursing increased rapidly by absorbing many of the newly minted Ph.D.s, although viewed historically this seems unlikely.
The average age of the faculty is 54, and 26 percent of the faculty are 60 years old or older. The age at time of degree for new assistant professors is 42.9 years, and for associate professors it is 39.9 years. The professors who received their degree even earlier were on average 35.9 years old when they completed their doctorate. Again this is consistent with the trend noted earlier in this chapter. Of the faculty who provided information about postdoctoral training, 30.1 percent had at least one postdoctoral appointment and 7.4 percent had more than one appointment. As would be expected, faculty members with more recent doctorates were more likely to have
TABLE 7-2 Tenure and Rank Status of Nursing Faculty
|
Rank |
Non-Tenured Non-Tenure Track |
Non-Tenured Tenure Track |
Tenured |
Total |
|
Assistant Professor |
84 |
310 |
8 |
402 |
|
Associate Professor |
40 |
49 |
343 |
432 |
|
Professor |
40 |
4 |
535 |
579 |
|
Emeritus |
2 |
|
15 |
17 |
|
Other |
14 |
1 |
3 |
18 |
|
Total |
180 |
364 |
904 |
1448 |
|
SOURCE: Dataset for the NRC Research-Doctorate Study. |
||||
postdoctoral training with 31 percent receiving their degree in the period 1997 to 2006. This also is likely contributing to the increasing age of assistant professors on nursing faculties.
A majority, 64 percent or 801 of the nursing faculty, have extramural funding, and these grants support 810 students either totally or partially. The average number of publications per faculty per year during the period 2000 to 2006 was about 0.5 in nursing, which is much lower than seen in other fields in the biomedical sciences, where the range is between 1.3 and 1.9.
The Trainees
In the fall of 2005, 2,176 students were enrolled in 55 doctoral programs, and the first-year enrollment was 442 students. As is the case with the profession, 94 percent of the doctoral students were female. In addition 12 percent were underrepresented minorities, and 10 percent were temporary residents. The enrollment status of the students is very different from other fields, with 1,294 (59 percent) full-time and 882 part-time. For full time-students the time to degree was 3.8 years. One of the 55 programs had an M.D./Ph.D. program with an enrollment of 3 students.
The level of full financial support for nursing students in 2006 was only 35 percent, and 27 percent of the students received no support. Presumably many of these graduate students worked to offset all, or part, of the cost of their education. A total of 37 of the 55 programs had externally funded training grants, and 17 percent of the students were supported on these grants. A small percentage, 9 percent and 7 percent, respectively, were supported on research assistant-ships and teaching assistantships. In addition to predoctoral training activities, 24 of the 55 nursing programs in the fall of 2005 supported 99 postdoctoral trainees.
Emphasizing Research Intensive Training Environments
Typically funded by the NINR, research training for nurse scientists has uses a variety of National Research Service Awards (NRSAs) and Career Development K awards. Individual predoctoral awards (F31) have been slowly increasing, but there are very limited numbers of individual postdoctoral awards (F32). In contrast, the institutional NRSAs (T32) initially grew considerably over time, but since 2003 there have been no steady increases in the number of slots supported (see Figure 7-1). There were 245 trainees supported in 2009 (156 predoctorates and 62 postdoctorates), which represents a decline from 2003.
The institutional and individual research training awards under the NRSA program both serve an extremely valuable purpose in nursing research and should continue to be funded. Individual awards build scientific capability, and T32 institutional awards build a cadre of strong senior researchers. The individual predoctoral awards (F31), if allocated for up to 5 years per award, will support full-time, consistent progression for research training.
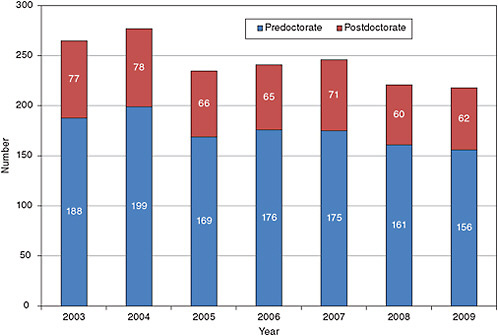
FIGURE 7-1 Training positions at the postdoctoral and predoctoral levels.
SOURCE: National Institutes of Health.
As outlined in the 2005 report, several changes to the T32 awards would strengthen them:
-
T32 awards should be placed only in research-intensive universities with strong interdisciplinary opportunities and research funding, and interdisciplinary activities should be a critical aspect of the initial NRSA application and annual reports.
-
T32 awards should be allocated only to schools with research-intensive environments including a cadre of senior investigators with extramurally funded research and research infrastructures that support research and research training.
-
The application process for T32 positions as predoctoral trainees or postdoctoral fellows should be more formalized, with specific proposals submitted in relationship to their research and the match with faculty at the institution made explicit.
-
Criteria for selection of T32 fellows and trainees should be based on a consistent, full-time plan for research training and long-term potential for contribution to science and nursing.
-
The monitoring and tracking of trainees and fellows should be formalized with changes in research plans or mentor(s) filed as part of the annual report.
A growing number of nurse-investigators are receiving K awards from NINR through the following mechanisms: K01 Mentored Research Scientist Development Award; Minority K01, Mentored Research Scientist Development Award for Minority Investigators; K22, Career Transition Award and K23, Mentored Patient Oriented-Research Career Development Award; and K24, Mid-Career Investigator Award in Patient Oriented Research. In addition, other NIH institutes and centers support nursing research through the K mechanisms, because elements of nursing research are intrinsic to other fields.
Recently, NINR staff have been advising potential K awardees to apply instead for small R-series awards. To compete in an era of limited research dollars, the availability of these early and mid-career awards needs to be increased and encouraged. There is little systematic information on the outcomes of these awards, e.g., successful research grants and publications by awardees. Based on the success in other fields, however, and the need for strongly research-prepared faculty to concentrate on the science necessary for practice, the committee believes that expanding such awards would benefit the field.
RECOMMENDATIONS
In addition to the recommendations which cross disciplines, the committee recognizes that the graying of the professoriate and need for nurse-scientists is particularly acute in nursing.
Recommendation 7–1: T32 programs in nursing should emphasize the rapid progression into research careers. Criteria should include identification of predoctoral trainees who are within 8 years of high school graduation, streamlining the master’s degree in passing to the Ph.D., and postdoctoral training within 2 years of completion of the Ph.D.
Recommendation 7–2: T32 awards should focus on programs where students and fellows have the opportunity to work with senior scientists, and applications to slots should require applicants a specific research and mentoring plan.
Recommendation 7–3: NINR should increase the number of mid- and senior career awards to enhance the number of scientists capable of sustaining programs of research and should increase the length of support for K awards to 5 years to be consistent with other institutes and centers.
Recommendation 7–4: Given the size of the NINR budget and the acute need for nursing faculty, the NIH should consider an infusion of support to allow NINR to more closely meet the needs.
Recommendation 7–5: To enhance the rapid progression for clinical scientist training, NINR should develop and pilot-test an MSTP-like program to support clinical training at the M.S.N. or D.N.P. level for those wishing to be clinician-scientists.






