10
Conclusions
Over the past 25 years, life expectancy has been rising in the United States at a slower pace than has been achieved in many other high-income countries. Consequently, the United States has been falling steadily in the world rankings for level of life expectancy, and the gap between the United States and countries with the highest achieved life expectancies has been widening. Life expectancy at birth in the United States for both sexes combined now ranks 28th in the world, just behind the United Kingdom, Korea, and Malta and more than 2 years behind Australia, Canada, France, Iceland, Italy, Japan, and Switzerland (United Nations, 2009). International comparisons of various measures of self-reported health and biological markers of disease reveal similar patterns of U.S. disadvantage. What are the reasons for the relatively poor performance of the United States? Are these factors visibly at work in two other underachieving countries—Denmark and the Netherlands?
PATTERNS OF MORTALITY AT OLDER AGES
It is not surprising that differences in levels of life expectancy exist among various high-income countries. What is perhaps more surprising is that large differences did not exist among many high-income countries around 1950, that the divergence discussed in this report began relatively abruptly around 1980, and that it has taken so long for this divergence to be recognized and analyzed. If one examines trends in life expectancy at various ages across countries, it becomes clear that the divergence has occurred for both men and women and at ages above and below 50. Nev
ertheless, the largest divergence among countries appears to have been for women aged 50 and over, and this segment of the population has been the primary focus of this report.
Descriptive analysis can be a powerful tool in demography. In this case, the panel undertook a careful examination of cause-of-death statistics to ascertain whether specific causes of death could account for the relatively low level of life expectancy in the United States and were associated with improvements in life expectancy in vanguard countries. Comparative analysis of causes of death is complicated by issues of variation in coding practices across countries and over time. Nevertheless, it does appear that higher mortality rates for lung cancer and respiratory diseases in the United States, Denmark, and the Netherlands are an important part of the story. Such a finding is clearly consistent with the hypothesis that smoking was an important factor accounting for the slowing of mortality decline among women in these three countries.
Other conditions that account for the poor performance of U.S. women include cerebrovascular conditions (primarily stroke), diabetes, and mental disorders. Stroke is another cause of death for which smoking is a risk factor. Obesity is a risk factor for both stroke and diabetes. With respect to mental disorders, the increase in such disorders is difficult to interpret, and the idea that this increase is attributable to differences in coding cannot be rejected. It should be noted, however, that the risk factors for heart disease, diabetes, and stroke overlap with those for Alzheimer’s disease, and it is possible that the trend in deaths due to mental disorders is related to some of the same underlying factors. Although mortality from heart disease played little role in the divergent trends in life expectancy—because even 50 years ago the United States already had much higher levels of mortality from heart disease than the other countries examined for this study—it accounts for about half the current gap between the United States and the countries with highest life expectancies; therefore, this condition should be a focus of efforts to bring U.S. life expectancy in line with that of the exemplar countries.
While descriptive analysis of causes of death is certainly informative, this report has begun the process of moving from description to identifying the underlying determinants of the observed differences, a necessary first step toward ultimately developing an integrated model of causal processes. More specifically, the panel examined a number of possible risk factors and considered how differences among countries in exposure to these risk factors might account for observed disparities in improvement in life expectancy. Such an approach is not without its limitations. For some factors, comparable cross-country data exist on the current levels of risk, while for others, surprisingly little direct evidence can be brought to bear. Few countries are conducting systematic surveillance of health risk factors, so that directly comparable data even for the present often are not available for a large
number of countries, and for a substantial number of countries, data are available for almost no risk factors for the 50-year period examined for this study. Much is known about current international differences in smoking patterns and levels of obesity, but far less about international differences in stress, physical exercise, or social networks.1 Very little is known, moreover, about changes over time and across countries in lifetime exposures and behaviors for most risk factors.
The fluid nature of the relationship between mortality and some of the major risk factors also complicated the panel’s work. For example, the epidemiological literature still reflects considerable differences of opinion with respect to the magnitude of the relationship between obesity and mortality. As the obesity epidemic has spread, the number of people at risk of obesity-related health problems has risen. At the same time, however, management of some of the more serious obesity-related health problems, such as heart disease and type 2 diabetes, has improved. Thus, the net effect of rising obesity on mortality is difficult to estimate.
Acknowledging these limitations, the panel’s strategy was to try to establish the strength of the evidence for a number of the most commonly proffered explanations for differences in life expectancy between the United States and other high-income countries—for example, that these differences are the result of a particularly inefficient U.S. health care system or that they are a function of poor health behaviors in the United States, particularly with respect to smoking, overeating, and failing to exercise sufficiently. The panel also considered differences among countries in levels of social integration and in socioeconomic inequality. Ultimately, all of these potential risk factors will need to be examined in an integrated framework across the entire life course, taking account of the effects of differences in socioeconomic status, behavioral risk factors, and social policy, as well as effects across particular cohorts and periods.
Smoking appears to be responsible for a good deal of the divergence in female life expectancy. Other factors, such as obesity, diet, exercise, and economic inequality, also have likely played a role in explaining the current gap between the United States and other countries, but evidence of their importance to the divergence is not as firm. The case against smoking, by contrast, is quite strong. Fifty years ago, smoking was much more widespread in the United States than in Europe or Japan: a greater proportion of Americans smoked and smoked more intensively than was the case in other
countries. The health consequences of this behavior are still playing out in today’s mortality rates. Over the period 1950–2003, the gain in life expectancy at age 50 was 2.1 years lower among U.S. women compared with the average of nine other high-income countries (5.7 vs. 7.8 years gained, respectively). The damage caused by smoking was estimated to account for 78 percent of the gap in life expectancy for women and 41 percent of the gap for men between the United States and other high-income countries in 2003 (Chapter 5). Smoking also has caused significant reductions in life expectancy in the Netherlands and Denmark, which as noted are two other countries with relatively poor life expectancy trends. It has had a major negative effect as well on life expectancy in Canada, where life expectancy trends have been much more favorable.
While smoking appears to be an important part of the story, it is by no means the entire story. Other factors, particularly the rising level of obesity in the United States, also appear to have played a significant part, although as noted, there is a good deal of uncertainty in the literature regarding the mortality consequences of obesity and possible trends therein. Several peer-reviewed articles appearing recently suggest effects of quite different orders of magnitude. Preston and Stokes (2010) conclude that, even using relatively low estimates of associated risk, obesity accounts for a fifth to a third of the shortfall in life expectancy in the United States relative to other high-income countries.
Other specific risk factors also are surely important, but their effects are even more difficult to quantify. The panel found some evidence to suggest that adults aged 50 and over in the United States are somewhat more sedentary than those in Europe, but the research base is insufficient even to identify a reasonable range of uncertainty in estimates of the contribution of physical activity to international differences or trends in mortality.
In other cases, the panel determined that certain risk factors are unlikely to have played a major role in the divergence of life expectancy in various countries over the past 25 years. A large body of work shows a causal relationship between social ties and social integration and mortality. Yet there is little basis for concluding that levels or trends in the quality of social networks have played a role in the divergent life expectancies studied. Similarly, little evidence supports the hypothesis that postmenopausal hormone therapy played a part in an emergent longevity shortfall for American women.
Finally, the panel examined whether differences in health care systems across countries might help explain the divergence in life expectancy over the past 25 years. The health care system in the United States differs from those in other high-income countries in a number of ways that conceivably could lead to differences in life expectancy. Certainly, the lack of universal access to health care in the United States has increased mortality and re-
duced life expectancy. However, this is a smaller factor above age 65 than at younger ages because of Medicare entitlements. For the main causes of death at older ages—cancer and cardiovascular disease—available indicators do not suggest that the U.S. health care system is failing to prevent deaths that would elsewhere be averted. In fact, cancer detection and survival appear better in the United States than in most other high-income countries. Survival rates following heart attack are also favorable in the United States.
Most of the comparative data the panel reviewed relate to the performance of the U.S. health care system relative to those of other high-income countries after a disease has already developed. A separate concern is that the U.S. health care system does a particularly poor job at prevention, an observation that may be especially relevant in the midst of a nationwide obesity epidemic. The panel reviewed scattered evidence on the performance of the United States with respect to preventive medicine relative to European countries and found the evidence to be inconclusive. Certainly the high prevalence of certain health conditions in the United States is consistent with a failure of preventive medicine. But it could also be consistent with a higher prevalence of smoking, obesity, and physical inactivity among Americans, or with a medical system that may be unusually effective at identifying certain diseases.
There is no question that high mortality rates among those of low socioeconomic status are one reason the United States has a lower level of life expectancy than it might otherwise. A useful proxy for socioeconomic status is educational level (Avendano et al., 2010). Death rates at particular levels of educational attainment tend to be higher in the United States than in other countries, and the differences are generally greatest at the lowest levels of education. On the other hand, lifetime socioeconomic status has generally been higher for these cohorts of Americans than for the comparable cohorts of Europeans. Because educational levels in the United States have been relatively high, the low-education group is quite small in the United States, while the high-education group is quite large. As a result, measures of inequality in mortality that combine distributions with rates indicate that the United States is not unusual in the size of its mortality differentials by educational attainment.
Determining the role of socioeconomic inequality in the divergence in life expectancy among high-income countries is more difficult than determining its role in mortality levels, although it appears to have played some role. Data from the period after 1980 do suggest, however, that growing inequality in mortality in the United States is attributable to a slowdown in mortality improvement among white women, particularly those with low levels of education.
Finally, with respect to racial differentials, high mortality rates among blacks clearly help explain why the level of life expectancy in the United
States is lower than it might otherwise be. However, racial differences in mortality are unlikely to contribute significantly to explanations for the divergence in life expectancy between the United States and other highincome countries since 1980. Neither the relative size of the white and black populations nor the mortality differential between the two has changed dramatically enough since that time for that differential to hold much explanatory power.
LOOKING TO THE FUTURE
What will happen to life expectancy in the United States and other countries in the coming decades? Although it is impossible to answer that question with any certainty, the analyses described in this volume do point to some likely patterns for the future. Because there appears to be a lag of several decades between smoking and its peak effects on mortality, there is some opportunity to predict how smoking will affect life expectancy in various countries over the next 20 to 30 years.
Smoking has been shown to affect both levels and trends in life expectancy. High levels of smoking in the United States have produced an increase in smoking-related mortality and a reduction in the pace of improvement in life expectancy at age 50. As a result, the level of life expectancy at age 50 in the United States has fallen below that of countries with lower levels of smoking. However, the imprint of smoking has started to recede in the United States among males, contributing to a more rapid reduction in mortality than would have occurred had its imprint been constant or rising (Wang and Preston, 2009). Thus, life expectancy for U.S. men is likely to improve relatively rapidly in the coming decades in response to changes that have occurred in smoking patterns over the past 20 years (Wang and Preston, 2009). For U.S. women, on the other hand, smoking peaked among cohorts born in the 1940s, and these cohorts are just entering the prime ages for dying. Thus the impact of smoking on the mortality of U.S. women may not have become fully manifest, and relatively slow mortality declines among this population might be anticipated over the next decade or two. Similarly, life expectancy in Japan can be expected to improve less rapidly than it otherwise would because of the rapid increase in the prevalence of smoking in that country.
The mechanics of how obesity is likely to influence life expectancy at age 50 are broadly similar to those described above for smoking. The United States has been in the vanguard of a global obesity epidemic, and obesity also appears to be an important contributor to the shortfall in life expectancy in the United States. In line with Olshansky and colleagues (2005), Stewart and colleagues (2009) conclude that, if the obesity trend in the United States continues, it will more than offset the longevity improvements
expected from reductions in smoking. However, recent data on obesity in the United States suggest that its prevalence has leveled off, and some studies indicate that the mortality risk associated with obesity has declined (Flegal et al., 2010; Mehta and Chang, 2010). Yet regardless of whether the prevalence of obesity continues to rise in cross-sectional data, the number of years the average individual will have spent in the obese state is likely to rise because of past increases in prevalence. The interplay between obesity levels and obesity risks bears watching as an important factor in future longevity trends in the United States.
LIMITS TO LIFE EXPECTANCY
Smoking and obesity are only two of many influences on mortality, and the future of longevity in the United States or elsewhere is beyond the scope of this study (see National Research Council, 2000b). However, one exercise that follows directly from this report’s consideration of international longevity trends is to compare the current level of life expectancy with the future rate of improvement. If we are approaching a biological limit to the length of life, future gains will become more difficult to achieve, and one might expect to observe an inverse association between the current level of life expectancy and the rate of improvement in the following decade.
Figures 10-1a and 10-1b show the relationship between these two variables for males and females for 22 countries over the past five decades, using life expectancy at age 80 as the basic mortality indicator. For both men and women, little association between the two variables is evident. The correlation coefficient (R2) for women is 0.03 and for men is 0.01. This simple exercise extends earlier demonstrations by Kannisto and colleagues (1994) and Vaupel (1997), and continues to suggest that if a limit exists, it is probably much higher than 85 years.
For the most part, this report has focused on the potential for improvements in health behaviors to produce longer and more active lives. The report does not address whether dramatic future increases in life expectancy might result from fundamental improvements in our understanding of the basic biology of aging and its genetic and environment modifiers. For example, the concept of Mendelian randomization, a method of using measured variation in genes of known function to estimate the causal effect of a modifiable exposure on disease in nonexperimental studies, provides new opportunities to test causality (Davey Smith and Ebrahim, 2003). It appears plausible that greater understanding of the basic principles governing the progressive deterioration of the body and mind could translate into interventions that would extend life to lengths not yet experienced in existing populations, and that such interventions could be adopted more rapidly in one country than another.
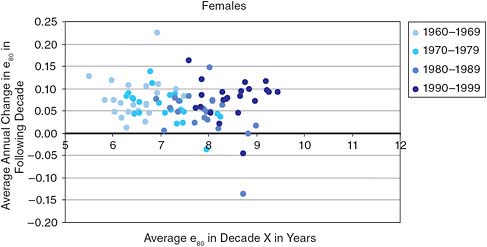
FIGURE 10-1a Male average life expectancy at age 80 (e80) plotted against average annual future change in e80 the following decade (R2 = 0.01) for selected countries.
SOURCE: Data from the Human Mortality Database, see http://www.mortality.org/ [accessed January 12, 2011].
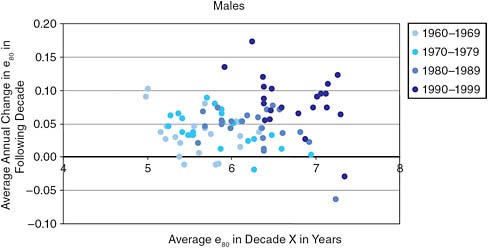
FIGURE 10-1b Female average life expectancy at age 80 (e80) plotted against average annual future change in e80 the following decade (R2 = 0.03) for selected counries.
SOURCE: Data from the Human Mortality Database, see http://www.mortality.org/ [accessed January 12, 2011].
POLICY AND RESEARCH IMPLICATIONS
The question of why U.S. longevity has fallen behind that of many other wealthy countries has proven productive in stimulating research on population health (see the background papers in National Research Council, 2010). Such research is focused on the factors that drive health conditions in large aggregates, providing a valuable complement to studies of health hazards for individuals. The factors that differentiate nations on health measures must not only affect the health of individuals but also vary in their intensity across populations. Moreover, the factors that promote change in population health must themselves be changing. To be convincing, studies attributing variation in population health outcomes to particular health risks must be consistent in the presumed magnitude of risk across levels of aggregation, from individuals to nations.
While the panel believes it made progress in identifying some of the main factors that have been driving differences in life expectancy among wealthy countries, it also identified many research gaps. The main focus of the report has been on a limited set of potential explanations—obesity, physical activity, smoking, social contacts and integration, health care, hormone replacement therapy, and socioeconomic and geographic inequality—the factors that the panel identified initially as most promising. The panel addressed some other hypotheses, such as the role of alcohol, in part in its analysis of specific causes of death, but was unable to examine other possible explanations, such as the role of the nutritional content of the diet.2
With respect to the behavioral risk factors that were investigated, a reliable marker of the damage from smoking exists—mortality rates from lung cancer. No such clear-cut and widely available marker has been identified for obesity, physical inactivity, stress, a lack of social relations, or the other risks considered in this report. Evaluation of the importance of these risks is based primarily on observational studies that follow forward people with differing levels of exposure. These studies are subject to many biases, especially those associated with omitted variables, self-selection into categories, and reverse causation. Reverse causation is such a threat in the case of physical activity that it is not clear whether much can be learned about this factor from observational studies. In the case of obesity, observational studies of
risk have left a great deal of uncertainty about the magnitude of the risk, which is important in attributing cross-sectional variation to obesity. Yet in view of the rapid increase in the population at risk, knowledge of the hazards of obesity may be especially important for projecting mortality trends in the United States.
A needed improvement in observational studies is the introduction of more information on individual histories, both prospective and retrospective. Studies that relate mortality and health only to levels of exposure at baseline miss the impact of exposures earlier in life, which are typically correlated with current exposure but may carry their own set of risks. Failure to update exposure categories after baseline is a form of measurement error and biases the estimated hazard associated with a particular risk factor (Stringhini et al., 2010; Taylor et al., 2002).
In addition to improvements in observational studies, more studies are needed that randomly assign individuals to exposure categories, although in reality there are limited ethical opportunities to use randomized controlled trials to study the questions at issue here. Yet while it is sometimes difficult, expensive, and ethically challenging to alter individual behavior, there is no perfect substitute for such trials. Where such studies are possible, they largely overcome the problem of omitted variables and reverse causation that plague observational studies. Studies that take advantage of natural experiments, such as increased cigarette taxes, changes in the use of hormone therapy, or the introduction of health care reform, can sometimes serve as valuable supplements to randomized controlled trials.
In addition to studying individual behavioral risks, this study has examined the role of broader, systemic factors, including health care systems, levels of inequality, and the quality of social relations. Such variables and conditions are more difficult to study than individual behavioral risks. If there existed a “score” for each nation on a particular factor, one could study the association between that score and national outcomes. Such an approach would be unlikely to yield important results with a sample of 10 countries, however, a condition the panel imposed for this study, or even with a sample size of 20. Moreover, no single score exists for any of these factors, which are complex concepts that defy simple characterization.
The panel’s approach to investigating these factors was eclectic. Indicators of their importance were sought in a variety of places. In the case of medical systems, the panel relied on reasonably complete and reliable international data on cancer screening, identification, and survival. However, there is nothing remotely equivalent to the cancer registries for cardiovascular disease, a more important cause of death. The incidence, prevalence, and case fatality outcomes of heart disease and stroke are not being tracked in national data systems, representing a major gap in those systems. With regard to inequality, the panel investigated how U.S. mortality
fared for different socioeconomic and geographic strata. But with so few national observations, it was impossible to investigate how national levels of inequality may have affected the health of all groups, which remains a challenging and important topic.
To make the study tractable, the panel focused on only one part of the life course—age 50 and above. According to the latest life table published by the National Center for Health Statistics, 92.6 percent of males and 95.8 percent of females in the United States survive to at least age 50 (Arias, 2010). Doubtless focusing on a different dependent variable would have resulted in certain underlying factors being emphasized more heavily. For example, smoking and obesity play a relatively small role in explaining the poor ranking of U.S. mortality in the age interval 40–65 (Ho and Preston, 2010; Muennig and Glied, 2010). Life expectancy at birth or age 50 gives weight to the conditions that prevail at a much wider span of ages.
In addition, the panel acknowledges that this report addresses only minimally differentials before age 50 that may have implications for later life, which could range from differentials in utero to those in middle age. Observational studies have found associations between early-life nutrition and the risk of adult chronic disease, for example. Likewise, Barker (1998) has assembled evidence showing that intrauterine growth retardation, low birth weight, and premature birth have a causal relationship with the origins of hypertension, coronary heart disease, and noninsulin-dependent diabetes in later life. To the extent that early-life conditions varied across countries 70–80 years ago, then, early-life metabolic adaptations may be associated with differential prevalence of a number of chronic conditions later in life. Thus further study of cohorts exposed to harsh conditions at early-life stages might provide valuable insights as to the early-life factors that affect later-life health and mortality. Indeed, effects on a population’s longevity may be transgenerational and even precede fetal development (Bygren et al., 2001; Gluckman et al., 2008; Kaati et al., 2002).
More generally, a key limitation of this study is that its approach is based on exploring individual risk factors, one at a time. Much work remains to be done on disentangling the possible synergies and connections among different risk factors as they play themselves out at the population level. Limited progress toward a fuller understanding of the practical or policy implications of the findings presented in this report can be expected without a clearer understanding of both the theoretical and empirical associations among the various pathways of influence.
The panel concluded that a history of heavy smoking and current levels of obesity are playing a substantial role in the poor longevity performance of the United States. This conclusion poses major issues for the nation. Such behaviors, while carried out individually, are products of a broad social and economic context encompassing, for example, a level of affluence that sup
ports large numbers of automobiles, low taxes on gasoline, and dispersed residences and workplaces that encourage driving; a climate and soil in part of the country that are conducive to growing tobacco; and a productive agricultural sector that produces inexpensive foods. From a cross-national perspective, the United States is often noted for high income inequality and weak social safety nets, labor policies, and child support policies.
Some of the relevant context is political. The panel undertook no analysis of the cost-effectiveness of public interventions designed to change personal health-related behaviors; therefore, recommendations as to what might be undertaken in this regard are not appropriate. It is clear, however, that failures to prevent unhealthy behaviors are costing Americans years of life compared with their counterparts in other wealthy countries.












