The passage of the Patient Protection and Affordable Care Act of 2010 (ACA) provides the United States with an opportunity to offer an unprecedented level of population health care coverage and dramatically reduce existing health disparities. The expansion of coverage to millions of uninsured Americans and the new standards for coverage of preventive services that are included in the ACA have the potential to increase the use of preventive health care services and screenings and in turn improve the health and well-being of individuals across the United States.
The approaches to prevention and wellness offered within the Act are broad based and range from new coverage requirements and incentives to expand workplace wellness activities to new investments. Among these are prohibition of the imposition of cost-sharing requirements for recommended preventive services (an overview of the Act is provided in Box 1-1, and the preventive services are listed and described in detail in Chapter 2), the requirement to link health insurance premiums to participation in health promotion programs, public health workforce development (the ACA authorizes new training and placement programs for public health workers), and community-based prevention activities.
This report focuses on the preventive services for women specified in Section 2713 of the Public Health Service Act. These services were added by the ACA and are detailed in the last bulleted item in Box 1-1 (HHS, 2010; Federal Register, 2010).
BOX 1-1
Overview of Regulations in Section 2713
of the Public Health Service Act
Section 2713 of the Public Health Service Act, Coverage of Preventive Health Services, which was added by the Affordable Care Act, and the interim final regulations (26 CFR 54.9815–2713T, 29 CFR 2590.715–2713, 45 CFR 147.130) require that group health plans and health insurance issuers offering health insurance coverage for groups or individuals provide benefits and prohibit the imposition of cost-sharing requirements for
- Medical devices or services that are evidence based and that have, in effect, a rating of Grade A or B in the current recommendations of the United States Preventive Services Task Force (USPSTF) for the individual involved.
- Immunizations for routine use in children, adolescents, and adults that have, in effect, a recommendation from the Advisory Committee on Immunization Practices (ACIP) of the Centers for Disease Control and Prevention (CDC) for the individual involved. A recommended ACIP immunization is considered to be “in effect” after it has been adopted by the CDC director. A recommended immunization is considered to be for routine use if it appears on the immunization schedules of the Centers for Disease Control and Prevention.
- Preventive health care and screenings for infants, children, and adolescents informed by scientific evidence and provided for in the comprehensive guidelines supported by the Health Resources and Services Administration (HRSA).
- Preventive health care and screenings for women informed by scientific evidence and provided for in comprehensive guidelines supported by HRSA (not otherwise addressed by the recommendations of the USPSTF). The U.S. Department of Health and Human Services is developing these guidelines and expects to issue them no later than August 1, 2011.
The complete list of recommendations and guidelines that these interim final regulations are required to cover can be found at http://www.HealthCare.gov/center/regulations/prevention.html.
ROLE OF PREVENTION IN ADDRESSING HEALTH AND WELL-BEING
Prevention is a well-recognized, effective tool in improving health and well-being and has been shown to be cost-effective in addressing many conditions early (Maciosek et al., 2010). Prevention goes beyond the use of disease prevention measures. For example, interventions to prevent injuries and binge drinking can increase positive health outcomes and reduce harm.
Historically, the many disparate components of the U.S. health care system have relied more on responding to acute problems and the urgent
needs of patients than on prevention. Although these functions are appropriate for acute and episodic health problems, a notable disparity occurs when this model of care is applied to the prevention and management of chronic conditions. The provision of preventive health care services is thus inherently different from the treatment of acute problems, but the U.S. health care system has fallen short in the provision of such services. Compared with a system that prevents avoidable conditions early, a system that responds to the acute health care needs of patients can be inefficient and costly, and a focus on response instead of prevention is a major barrier to the achievement of optimal health and well-being by Americans.
Nearly half of all deaths in the United States are caused by modifiable health behaviors (McGinnis and Foege, 1993). Maciosek and colleagues found that an increase in the use of clinical preventive services in the United States could result in the saving of more than 2 million life-years annually (Maciosek et al., 2010). Because of the numbers of diseases and conditions that are preventable, inclusion of support for prevention has become more routine during clinical health care visits (Sussman et al., 2006). When patients are systematically provided with the tools and information that they need to reduce their health risks, the likelihood that they will take steps to, for example, reduce substance use, stop using tobacco products, practice safe sex, eat healthful foods, and engage in physical activity increases (WHO, 2002). Therefore, physicians who routinely educate patients on risk-reducing behaviors may reduce the long-term burden and health care demands of chronic conditions. Stimulating the commitment and action of patients, families, and health care teams is also necessary to promote prevention and improve overall population well-being.
Evidence-based testing, diagnosis, and relief of symptoms are also hallmarks of contemporary health care, but these services are often underutilized. A well-cited reason for this underutilization is, for example, the high cost of prescription copayments, with the result being that patients do not fill their prescribed medications, resulting in the loss of lives and dollars (Shrank et al., 2010). Moreover, a recent study by The Commonwealth Fund that analyzed the responses of U.S. adults to a questionnaire indicated that U.S. adults were significantly less likely than adults in all other countries studied to have confidence in their ability to afford health care (Schoen et al., 2009).
About 51 million Americans lacked health insurance in 2009 (DeNavas-Walt et al., 2010). This is in addition to the millions of under-insured Americans who lack access to the appropriate screenings and services needed to detect and address preventable health conditions and diseases. Furthermore, health care workers have often failed to seize patient interactions as opportunities to promote health and well-being and to inform patients about disease prevention strategies (WHO, 2002). This failure to
inform patients has been found to be due to time constraints in the clinical setting, a lack of reimbursement for provision of these services, and a lack of consensus and provider knowledge about what services to prioritize for their patients. The ACA intends to mitigate these issues.
The ACA has the potential to transform the way in which the U.S. health care system addresses women’s health issues in many ways. It expands access to coverage to millions of uninsured women, ends discriminatory practices such as gender rating in the insurance market, eliminates exclusions for preexisting conditions, and improves women’s access to affordable, necessary care. The Women’s Health Amendment (Federal Register, 2010), which was introduced by Senator Barbara Mikulski and which was added to the ACA, expands on these improvements by requiring that all private health plans cover—with no cost-sharing requirements—a newly identified set of preventive health care services for women. Defining appropriate preventive services for women and ensuring that those services can be accessed without cost sharing are important strategies to improve women’s health and well-being (Bernstein et al., 2010; Blustein, 1995).
Many reasons exist for expanding the list of preventive care and screening services for women beyond those included in the guidelines of the United States Preventive Services Task Force (USPSTF) Grade A and B guidelines, the Advisory Committee on Immunization Practices (ACIP), and Bright Futures (for adolescents) stipulated in the ACA (USPSTF, ACIP, and Bright Futures and their guidelines are described in detail in Chapter 2). Even though women have longer life expectancies than men, women suffer from chronic disease and disability at rates disproportionate to those of men, with consequences for their own health and the health of their families (Wood et al., 2010). Furthermore, mounting evidence suggests that women not only have different health care needs than men (because of reproductive differences) but also manifest different symptoms and responses to treatment modalities (IOM, 2010). Behavioral factors that are shown to contribute to morbidity and mortality in women, include smoking, eating habits, physical activity, sexual risk-taking, and alcohol use (IOM, 2010). Pregnancy and childbirth also carry risks to women’s health including maternal mortality (CDC, 2008). Figure 1-1 illustrates preventable mortality in women.
Health outcomes occur because of multiple factors including biology, behavior, and the social, cultural, and environmental contexts in which women live. Smoking, eating habits, physical activity, and other health-related behaviors are shaped by cultural and social contexts, including factors associated with social disadvantage. The marked differences in
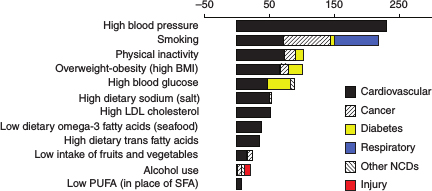
FIGURE 1-1 Deaths in women attributable to total effects of individual risk factors (in thousands), by disease.
ABBREVIATIONS: BMI, body-mass index; LDL, low-density lipoproteins; NCD, non-communicable disease; PUFA, polyunsaturated fatty acid; SFA, saturated fatty acid.
SOURCE: Danaei et al. (2009).
condition prevalence and mortality in women who experience social disadvantage are associated with minority race/ethnicity, lower education, low income, and differential exposure to stressors such as domestic violence. Such exposures are related to outcomes as varied as injury and trauma, depression, asthma, heart disease, human immunodeficiency virus (HIV) infection, and other sexually transmitted infections (Campbell et al., 2002; Coker et al., 2000; Ozer and Weinstein, 2004; Tjaden and Thoennes, 1998).
On average, women need to use more preventive care than men (Asch et al., 2006; HHS, 2001), owing to reproductive and gender-specific conditions, causing significant out-of-pocket expenditures for women (Bertakis et al., 2000; Kjerulff et al., 2007). This creates a particular challenge to women, who typically earn less than men and who disproportionately have low incomes. Indeed, women are consistently more likely than men to report a wide range of cost-related barriers to receiving or delaying medical tests and treatments and to filling prescriptions for themselves and their families (KFF, 2010). For example, women have been shown to be more likely than men to forgo preventive services such as cancer screenings and dental examinations because of cost (Rustgi et al., 2009). Studies have also shown that even moderate copayments for preventive services such as mammograms and Pap smears deter patients from receiving those services (Solanki et al., 2000; Trivedi et al., 2010). A 2010 Commonwealth Fund
survey found that 44 percent of adult women (compared with 35 percent of adult men) either reported that they had a problem paying medical bills or indicated that they were paying off medical debt over time, an increase from 38 percent in 2005 (Robertson and Collins, 2011). The same survey indicated that less than half of women are up to date with recommended preventive care screenings and services (Robertson and Collins, 2011).
Most women and men in the United States are covered by insurance obtained through the workplace. However, women with employer-based insurance are almost twice as likely as men to be covered as dependents, increasing their vulnerability to losing their insurance if they divorce, their partners lose their jobs, or they become widowed (KFF, 2010). Even though results of studies indicate that evidence-based preventive care services lower the burden of disease, are often cost-effective, increase the efficiency of health care spending, and contribute to the creation of a more productive and prosperous America, many financial barriers exist that prevent women from achieving health and well-being for themselves and their families.
Preventive services for women are services that prevent conditions harmful to women’s health and well-being. “Conditions” are considered diseases, disabilities, injuries, behaviors, and functional states that have direct implications for women’s health and well-being. These conditions may be specific to women, such as gynecologic infections and unintended pregnancy; they may be more common or more serious in women, such as autoimmune diseases and depression; they may have distinct causes or manifestations in women, such as alcohol abuse, obesity, and interpersonal violence-related posttraumatic stress disorder; or they may have different outcomes in women or different treatments, such as cardiovascular disease and diabetes (IOM, 2010). To “prevent” is to forestall the onset of a condition; detect a condition at an early stage, when it is more treatable; or slow the progress of a condition that may worsen or result in additional harm. Preventive services may therefore include the provision of immunizations, screening tests, counseling and education, Food and Drug Administration-approved medications and devices, procedures, and over-the-counter medications and devices.
COMMITTEE ON PREVENTIVE SERVICES FOR WOMEN
The Office of the Assistant Secretary for Planning and Evaluation (ASPE) of the U.S. Department of Health and Human Services (HHS) asked the Institute of Medicine to convene a diverse committee of experts in disease prevention, women’s health issues, adolescent health issues, and
evidence-based guidelines to review existing guidelines, identify existing coverage gaps, and recommend services and screenings for HHS to consider in order to fill those gaps (Box 1-2). A 16-member committee was selected to complete the statement of task.
In subsequent guidance to the committee, HHS sponsors at ASPE directed the committee to limit its focus to females between the ages of 10 and 65 years.
BOX 1-2
Statement of Task to the Committee on
Preventive Services for Women
The Institute of Medicine will convene an expert committee to review what preventive services are necessary for women’s health and well-being and should be considered in the development of comprehensive guidelines for preventive services for women. The committee will also provide guidance on a process for regularly updating the preventive screenings and services to be considered. In conducting its work, the committee will: conduct a series of meetings to examine existing prevention guidelines, obtain input from stakeholders, identify gaps that may exist in recommended preventive services for USPSTF Grade A and B preventive services guidelines for women and in Bright Futures and USPSTF Grade A and B guidelines for adolescents, and highlight specific services and screenings that could supplement currently recommended preventive services for women. Specifically, the committee will consider the following questions:
- What is the scope of preventive services for women not included in those graded A and B by the USPSTF?
- What additional screenings and preventive services have been shown to be effective for women? Consideration may be given to those services shown to be effective but not well utilized among women disproportionately affected by preventable chronic illnesses.
- What services and screenings are needed to fill gaps in recommended preventive services for women?
- What models could HHS and its agencies use to coordinate regular updates of the comprehensive guidelines for preventive services and screenings for women and adolescent girls?
The Office of the Assistant Secretary for Planning and Evaluation (ASPE) on behalf of the U.S. Department of Health and Human Services (HHS) has been charged to examine recommendations for women’s preventive services. ASPE will use the information and recommendations from the committee’s report to guide policy and program development related to provisions in the Affordable Care Act addressing preventive services for women.
The ACA defines the current USPSTF recommendations regarding breast cancer screening, mammography, and breast cancer prevention to be “the most current other than those issued in or around November 2009.” Thus, coverage for screening mammography is guided by the 2002 USPSTF guideline, which specifies that such screenings be performed every one to two years for women aged 40 years and older.
Furthermore, for consistency in approach with the other three guidelines used by the ACA and given the time limitations for this study, the committee was restricted from considering cost-effectiveness in its process for identifying gaps in current recommendations. Finally, despite the potential health and well-being benefits to some women, abortion services were considered to be outside of the project’s scope, given the restrictions contained in the ACA.
The committee received clarification from ASPE that its work was not intended to duplicate the processes used by the USPSTF or Bright Futures. Thus, the committee interpreted this guidance to indicate that evidence ranging from systematic reviews of the evidence to other bodies of evidence could be considered. This appears to be consistent with the process that led to the current preventive services within the ACA.
The committee was also directed to limit its work to identifying clinical preventive service coverage gaps and not to make recommendations regarding community-based prevention activities.
The committee recognizes that many factors that shape the health and well-being of women fall outside the realm of clinical services. These include, for example, changes to the environment and the workplace to promote health, changes in women’s concept of self-efficacy to promote health, and changes in women’s self-empowerment to address their own health and wellness. These factors and determinants of health are elements of models such as the Whitehead and Dahlgren (1991) determinants-of-health model and encompass biological, behavioral, and social factors. Nevertheless, evaluation of these factors and determinants of health were outside of the committee’s purview.
HHS will consider the committee’s recommendations as it develops guidelines to support the delivery of effective preventive services for women. If they are enacted, the recommendations from this study, along with the other coverage requirements in the ACA, will provide a comprehensive package of clinical preventive services for women.
To meet its charge, the committee held three information-gathering meetings on preventive services for women and reviewed the relevant literature. Before the first meeting and throughout the committee’s delibera-
tions, the committee gathered extensive information on numerous topics related to health and health care services for women, including chronic and mental health conditions, cancers, sexually transmitted infections, bone diseases, breastfeeding, interpersonal violence, unintended pregnancy, and a variety of behavioral health issues. During the public forums, representatives from women’s health organizations, national health interest groups, health coverage providers, employer interest groups, and other experts presented statements to the committee on the latest status and developments in their respective fields (see Appendix B for the meeting agendas). Committee members questioned the speakers to address additional concerns that they did not cover in their statements. The committee also invited comments (both written and oral) from the general public and representatives from numerous organizations with interest in women’s preventive services.
The committee first met in November 2010 and held its last meeting in May 2011. Within that time frame, it should be noted that the committee did not have adequate time or resources to conduct its own meta-analyses or comprehensive systematic review for each preventive service or for every special population group that may have different health needs or benefit from different preventive services, such as minority populations, disabled women, recent immigrants, lesbians, prisoners, and those employed in high-risk environments.
Box 1-3 details the committee’s definition of preventive health services, which was used as a starting point for the study.
This definition of preventive health services is primarily derived from a blend of definitions from multiple health care organizations and agencies, including the USPSTF and the World Health Organization, with the text regarding well-being possessing the most original phrasing by the committee and stems from the statement of task. In addition, other key definitions are included in Box 1-4. These definitions were adapted from the Five Major Steps to Intervention of the Agency for Healthcare Research
BOX 1-3
Definition of Preventive Health Services
For the purposes of this study, the Committee on Preventive Services for Women defines preventive health services to be measures—including medications, procedures, devices, tests, education, and counseling—shown to improve well-being and/or decrease the likelihood or delay the onset of a targeted disease or condition.
BOX 1-4
Key Definitions: Preventive Interventions
Preventive interventions come in several forms: screening, testing, counseling, immunization, preventive medication, and preventive treatment.
- Screening is best described as tests that assess the likelihood of the presence of a disease or condition in an apparently healthy individual. Screening methods use, for example, laboratory analyses and X rays and similar technologies. Screening also includes questions from clinicians. Screening may be targeted to people at increased risk because of age, gender, family or personal history, and other factors. Each screening tool is different in design and method, affecting the sensitivity (ability to correctly identify those with the disease), specificity (ability to correctly identify those without the disease), and positive and negative predictive values of the tool. Ideally, screening tests are rapid, simple, and safe. Screening is not a definitive diagnostic test, and a positive result on a screening test merely indicates that the screened individual has a higher likelihood of having the disease or condition for which the individual is being screened. Individuals who screen positive on such tests should have confirmatory diagnostic tests to ensure an accurate diagnosis.
-
Testing refers to any process used to determine whether a condition is present or to assess the status of a condition. Testing may involve questioning patients (e.g., asking a patient about tobacco use), physical examination (e.g., mammography screening to detect potential breast cancers), or examining blood, body fluids, or tissues (e.g., to see if a cancer is present in a biopsy sample). Testing may also require the use of sophisticated technology, such as computed tomography and magnetic resonance imaging scans and other X rays, or invasive procedures, such as heart catheterization to detect blockage of coronary arteries. Tests may be used to
- Screen individuals who have risk factors but no indication of having the condition,
- Diagnose a disease or condition in individuals who have symptoms and signs but for whom a test will add certainty about the diagnosis, or
- Monitor the progress of an individual who is being treated or being considered for treatment, such as monitoring blood pressure over time.
- Counseling refers to a discussion between a clinician and patient about ways that changes in personal behavior can reduce the risk of illness or injury. The goal of counseling is for clinicians to educate patients about their health risks as well as to provide them with the skills, motivation, and knowledge that they need to address their risk behaviors (e.g., the “5 A” framework for tobacco cessation: ask, advise, assess, assist, arrange). A special kind of counseling, informed decision making, recognizes that different people will make different decisions, even though their situations may seem to be similar. Informed decision making is structured to give an individual all the information needed
to choose from among different clinical options, such as whether to undergo genetic testing.
- Immunization protects an individual from a specific communicable disease (e.g., hepatitis) by exposing the individual to an antigen or a trace amount of an inactivated disease-causing agent, spurring the development of natural immunity.
- Preventive medications are used to prevent the onset of a disease or a condition (e.g., aspirin therapy to prevent cardiovascular events).
- Preventive treatment involves a procedure intended to prevent the occurrence of a disease or condition or to prevent the progression of a disease from one stage to another. Preventive treatments usually refer to the use of prescription or nonprescription (over-the-counter) medications, but they may also involve the use of prescriptions for lifestyle changes (e.g., exercise or diet change) or other interventions. Some surgical procedures may be considered preventive treatment, such as removal of polyps in the colon identified during a screening colonoscopy to prevent their progression to cancer lesions.
SOURCES: AHRQ, 2011; NBGH, 2005.
and Quality (AHRQ, 2011) and the National Business Group on Health’s Purchaser’s Guide to Clinical Preventive Services: Moving Science into Coverage (NBGH, 2005).
The report that follows is organized into seven chapters, summarized below.
- In Chapter 2, the report reviews the three existing guidelines used in the ACA to determine coverage.
- Chapter 3 details the existing practices of national, state, and selected private health plans.
- In Chapter 4, the committee discusses its framework for identifying gaps in existing preventive services and its process for selecting how to fill those gaps.
- Chapter 5 provides a description of the gaps identified through the committee’s work.
- The committee’s recommendations for updating guidelines for preventive services are proposed in Chapter 6.
- Chapter 7 includes committee conclusions and summarizes committee recommendations while identifying the limitations under which the committee performed its work.
- Appendix A includes a review of the conditions that the committee considered as part of its deliberations. Although no new recommendations were developed, the committee made clarifying statements or suggestions of ways to use preventive services to address these conditions.
- Appendix B provides agendas for the committee’s three public meetings.
- Appendix C includes condensed biographies of committee members.
- Appendix D contains one committee member’s statement of dissent and a response from all other committee members.
AHRQ (Agency for Healthcare Research and Quality). 2011. Five major steps to intervention (the “5A’s”). Rockville, MD: Agency for Healthcare Research and Quality, U.S. Public Health Service. http://www.ahrq.gov/clinic/tobacco/5steps.htm (accessed June 3, 2011).
Asch, S. M., E. A. Kerr, J. Keesey, J. L. Adams, C. M. Setodji, S. Malik, and E. A. McGlynn. 2006. Who is at greatest risk for receiving poor-quality health care? New England Journal of Medicine 354(11):1147–1156.
Bernstein, J. L., D. Chollet, and G. G. Peterson. 2010. Issue brief: Encouraging appropriate use of preventive health services. Princeton, NJ: Mathematica Policy Research.
Bertakis, K. D., R. Azari, L. J. Helms, E. J. Callahan, and J. A. Robbins. 2000. Gender differences in the utilization of health care services. Journal of Family Practice 49(2):147–152.
Blustein, J. 1995. Medicare coverage, supplemental insurance, and the use of mammography by older women. New England Journal of Medicine 332(17):1138–1143.
Campbell, J., A. S. Jones, J. Dienemann, J. Kub, J. Schollenberger, P. O’Campo, A. C. Gielen, and C. Wynne. 2002. Intimate partner violence and physical health consequences. Archives of Internal Medicine 162(10):1157–1163.
CDC (Centers for Disease Control and Prevention). 2008. Safe motherhood: Promoting health for women before, during, and after pregnancy 2008. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, Coordinating Center for Health Promotion.
Coker, A. L., P. H. Smith, L. Bethea, M. R. King, and R. E. McKeown. 2000. Physical health consequences of physical and psychological intimate partner violence. Archives of Family Medicine 9(5):451–457.
Danaei, G., E. L. Ding, D. Mozaffarian, B. Taylor, J. Rehm, C. J. Murray, and M. Ezzati. 2009. The preventable causes of death in the United States: Comparative risk assessment of dietary, lifestyle, and metabolic risk factors. PLoS Med 6(4):e1000058.
DeNavas-Walt, C., B. D. Proctor, and J. C. Smith. 2010. Income, poverty, and health insurance coverage in the United States: 2009. Washington, DC: Bureau of the Census.
Federal Register. 2010. Interim final rules for group health plans and health insurance issuers relating to coverage of preventive services under the Patient Protection and Affordable Care Act. Federal Register 75(137):41726–41756.
HHS (U.S. Department of Health and Human Services). 2001. Utilization of ambulatory medical care by women: United States, 1997–98. In Vital and health statistics. Atlanta, GA: National Center for Health Statistics, Centers for Disease Control and Prevention, U.S. Department of Health and Human Services.
HHS. 2010. Preventive regulations. http://www.healthcare.gov/center/regulations/prevention/regs.html (accessed April 13, 2011).
IOM (Institute of Medicine). 2010. Women’s health research: Progress, pitfalls, and promise. Washington, DC: The National Academies Press.
KFF (Henry J. Kaiser Family Foundation). 2010. Impact of health reform on women’s access to coverage and care. Focus on Health Reform. Washington, DC: Henry J. Kaiser Family Foundation. http://www.kff.org/womenshealth/upload/7987.pdf. (accessed April 13, 2011).
Kjerulff, K. H., K. D. Frick, J. A. Rhoades, and C. S. Hollenbeak. 2007. The cost of being a woman—a national study of health care utilization and expenditures for female-specific conditions. Womens Health Issues 17(1):13–21.
Maciosek, M. V., A. B. Coffield, T. J. Flottemesch, N. M. Edwards, and L. I. Solberg. 2010. Greater use of preventive services in U.S. health care could save lives at little or no cost. Health Affairs 29(9):1656–1660.
McGinnis, J. M., and W. H. Foege. 1993. Actual causes of death in the United States. Journal of the American Medical Association 270(18):2207–2212.
NBGH (National Business Group on Health). 2005. A purchaser’s guide to clinical preventive services: moving science into coverage. Washington, DC: National Business Group on Health.
Ozer, E. J., and R. S. Weinstein. 2004. Urban adolescents’ exposure to community violence: The role of support, school safety, and social constraints in a school-based sample of boys and girls. Journal of Clinical Child and Adolescent Psychology 33(3):463–476.
Robertson, R., and S. R. Collins. 2011. Women at risk: Why increasing numbers of women are failing to get the health care they need and how the Affordable Care Act will help. In Realizing Health Reform’s Potential. New York: The Commonwealth Fund.
Rustgi, S. D., M. M. Doty, and S. R. Collins. 2009. Women at risk: Why many women are forgoing needed health care. New York: The Commonwealth Fund.
Schoen, C., R. Osborn, M. M. Doty, D. Squires, J. Peugh, and S. Applebaum. 2009. A survey of primary care physicians in eleven countries, 2009: Perspectives on care, costs, and experiences. Health Affairs 28(6):W1171–W1183.
Shrank, W. H., N. K. Choudhry, M. A. Fischer, J. Avorn, M. Powell, S. Schneeweiss, J. N. Liberman, T. Dollear, T. A. Brennan, and M. A. Brookhart. 2010. The epidemiology of prescriptions abandoned at the pharmacy. Annals of Internal Medicine 153(10):633–640.
Solanki, G., H. H. Schauffler, and L. S. Miller. 2000. The direct and indirect effects of cost-sharing on the use of preventive services. Health Services Research 34(6):1331–1350.
Sussman, A. L., R. L. Williams, R. Leverence, P. W. Gloyd, Jr., and B. F. Crabtree. 2006. The art and complexity of primary care clinicians’ preventive counseling decisions: Obesity as a case study. Annals of Family Medicine 4(4):327–333.
Tjaden, P. G., and N. Thoennes. 1998. Prevalence, incidence, and consequences of violence against women: Findings from the national violence against women survey, research in brief. Washington, DC: US Department of Justice, Office of Justice Programs, National Institute of Justice.
Trivedi, A. N., H. Moloo, and V. Mor. 2010. Increased ambulatory care copayments and hospitalizations among the elderly. New England Journal of Medicine 362(4):320–328.
Whitehead, M., and G. Dahlgren. 1991. What can be done about inequalities in health? Lancet 338(8774):1059–1063.
WHO (World Health Organization). 2002. Integrating prevention into health care. Geneva, Switzerland: World Health Organization. http://www.who.int/mediacentre/factsheets/fs172/en/index.html. (accessed April 13, 2011).
Wood, S. F., A. Dor, R. E. Gee, A. Harms, R. Maurery, and S. Rosenbaum. 2010. Women’s health and health reform: The economic burden of disease in women. Washington, DC: The Jacob’s Institute of Women’s Health, The George Washington University School of Public Health and Health Services.














