2
Health Insurance and Children in America
This chapter compares trends in health insurance coverage across three major coverage groups of children in the United States: those with employer-based coverage (private insurance), those enrolled in the Medicaid program (public insurance), and those who have no insurance (uninsured). Trends in insurance coverage for adults are also included for purposes of comparison. The chapter reviews evidence of patterns in children's insurance coverage by age, race, ethnicity, parental income, and parental employment. The chapter also reports evidence on the duration of uninsurance and describes regional variations in the rates of uninsurance.
For ease in identifying trends that are described in the text, the figures in this chapter present data for individuals with the main sources of coverage—employer-based (private) and Medicaid (public) coverage—and for uninsured individuals. The tables in this chapter present a complete array of all sources of health insurance coverage and also give exact percentages.
Background
In the United States, the private sector provides health insurance for the majority of children and adults, primarily through employer-sponsored coverage (see Table 2.1 and Table 2.2). This is in contrast to other developed countries (e.g., Canada, United Kingdom, France, and Japan), which rely primarily on public-sector financing for health insurance (IOM, 1993; Schieber and Poullier, 1989).
In the United States, public-sector financing for children's health insurance is primarily through Medicaid, a program financed by the federal and state governments and administered by the states. In 1995, approximately one in four children (23 percent) were enrolled in Medicaid (see Table 2.1). Other sources of public insurance include military health care and Medicare; together, however, these other sources provide coverage for fewer than 5 percent of insured children.
As of 1994, approximately 14 percent of American children, or about 10 million children, did not have any insurance coverage (see Table 2.1 and Table 2.3). By 1996, this figure had grown to more than 11 million children (Weigers et al., 1998). As later sections of this chapter indicate, the majority of these uninsured children live in working families. These working parents do not have coverage through their employers, earn too little to be able to afford to buy health insurance on their own, and earn too much to be eligible for public health insurance such as Medicaid.
For uninsured children, access to health care is often unaffordable or otherwise out of reach. Unable
INSURANCE COVERAGE TRENDS (PERCENTAGES) FOR CHILDREN (TABLE 2.1) AND ADULTS (TABLE 2.2)
TABLE 2.1 Trends in Health Insurance Coverage Among Children, Ages 0-17, United States, 1987-1995 (percent)
|
Children's Health Insurance Source |
Percent |
||||||||
|
|
1987 |
1988 |
1989 |
1990 |
1991 |
1992 |
1993 |
1994 |
1995 |
|
Total private |
73.2 |
73.0 |
73.1 |
70.6 |
69.2 |
68.7 |
67.4 |
65.6 |
66.1 |
|
Employer-based |
66.7 |
66.5 |
65.8 |
64.0 |
62.7 |
62.0 |
59.5 |
58.1 |
58.6 |
|
Self-pay |
6.5 |
6.5 |
7.3 |
6.6 |
6.5 |
6.7 |
7.9 |
7.5 |
7.5 |
|
Total public |
19.3 |
19.5 |
19.5 |
22.2 |
24.2 |
25.2 |
26.8 |
26.3 |
26.4 |
|
Medicaid |
15.5 |
15.9 |
16.0 |
18.9 |
20.8 |
22.0 |
23.9 |
22.9 |
23.2 |
|
Military health carea |
4.0 |
3.8 |
3.6 |
3.6 |
3.6 |
3.5 |
3.3 |
3.8 |
3.2 |
|
Medicare |
0.2 |
0.2 |
0.1 |
0.1 |
0.1 |
0.1 |
0.1 |
0.3 |
0.4 |
|
Uninsured |
13.1 |
13.3 |
13.6 |
13.2 |
12.9 |
12.7 |
13.7 |
14.2 |
13.8 |
|
Total |
105.6 |
105.8 |
106.2 |
106.0 |
106.3 |
106.6 |
107.9 |
106.1 |
106.3 |
|
NOTES: Columns do not add to 100 percent because individuals may receive coverage from more than one source during 1 year. a Military health care also includes the Civilian Health and Medical Program of the Uniformed Services and health care through the U.S. Department of Veterans Affairs. SOURCE: EBRI, 1997. Estimates are based on data from the March 1988-1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce. |
|||||||||
TABLE 2.2 Trends in Health Insurance Coverage among Adults, Ages 18-64, United States, 1987-1995 (percent)
|
Adults' Health Insurance Source |
Percent |
||||||||
|
|
1987 |
1988 |
1989 |
1990 |
1991 |
1992 |
1993 |
1994 |
1995 |
|
Total private |
77.1 |
76.2 |
76.2 |
74.8 |
73.8 |
72.3 |
72.4 |
73.1 |
72.7 |
|
Employer-based |
70.4 |
70.1 |
69.8 |
68.3 |
67.8 |
65.9 |
65.4 |
66.1 |
66.1 |
|
Self-pay |
6.7 |
6.2 |
6.3 |
6.4 |
5.9 |
6.4 |
7.0 |
7.0 |
6.6 |
|
Total public |
10.7 |
10.6 |
10.4 |
11.1 |
11.7 |
11.9 |
12.3 |
12.8 |
12.2 |
|
Medicaid |
5.6 |
5.6 |
5.7 |
6.4 |
7.0 |
7.3 |
7.8 |
7.9 |
7.8 |
|
Military health careª |
4.6 |
4.4 |
4.1 |
4.2 |
4.0 |
3.8 |
3.8 |
4.3 |
3.7 |
|
Medicare |
2.1 |
2.0 |
2.1 |
2.2 |
2.3 |
2.4 |
2.3 |
1.8 |
2.0 |
|
Uninsured |
15.6 |
16.4 |
16.6 |
17.4 |
17.8 |
18.9 |
18.8 |
18.5 |
19.0 |
|
Total |
103.4 |
103.2 |
103.2 |
103.3 |
103.3 |
103.1 |
103.5 |
104.4 |
103.9 |
|
Table 2.2 Trends in Health Insurance Coverage among Adults, Ages 18-64, United States, 1987-1995 NOTES: Columns do not add to 100 percent because individuals may receive coverage from more than one source during 1 year. a Military health care also includes the Civilian Health and Medical Program of the Uniformed Services and health care through the U.S. Department of Veterans Affairs. SOURCE: EBRI (1997). Estimates are based on data from the March 1987-1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce. |
|||||||||
to pay for needed care, their parents may decide to delay treatment and hope that a medical problem will resolve on its own. Health problems that are minor in their early stages can escalate to serious and costly medical emergencies, and delays in access to health care can increase the burden of suffering from disease. This is especially true for children with special needs and chronic diseases.
|
Things happen. Earaches happen. Toothaches happen. Not being in a position to be able to save up for that rainy day of emergency room visits or doctor visits, I have spent more than a few minutes wondering what would I do if something happened. It's a lot like driving a car with no brakes. You know there is a stop light ahead. You just pray for green, because you don't know what you'll do if you have to stop. Maureen Ceidro Parent and Former Participant, Caring Program of Western Pennsylvania Public Workshop, June 2, 1997 |
Profile Of Health Insurance Coverage
Who Is Insured and Who Isn't
The U.S. health care system is often described as a patchwork of funding streams, often resulting in fragmentation of the delivery of care. Depending on the methods used to collect and analyze information from these funding streams, estimates of insurance coverage vary.
For example, estimates of Medicaid coverage from the Health Care Financing Administration differ substantially from those produced by the Bureau of the Census and the Agency for Health Care Policy and Research. However, because the Current Population Survey (CPS) from the Bureau of the Census is most commonly used by governmental and nongovernmental agencies in health insurance analyses, the committee relied principally on CPS data for the estimates of insurance coverage presented in this chapter.
CPS data show that the major sources of coverage for health care for the nation's 71 million children in 1995 included the following:
- 41.7 million had employer-based coverage through their parents,
- 16.5 million were enrolled in Medicaid,
- 300,000 were Medicare beneficiaries,
- 2.3 million had military health care (primarily Civilian Health and Medical Program of the Uniformed Services, or CHAMPUS), and
- 9.8 million had no coverage.
Table 2.3 indicates the array of sources of health insurance coverage for children, and for purposes of comparison Table 2.4 indicates the same array for adults.
Trends in Coverage for Children
Figure 2.1 shows the trends in coverage for children from 1987 to 1995 as a percentage of all children (refer to Table 2.1 for the exact percentages). Employer-based coverage for children decreased 8 percent between 1987 and 1995 (see Figure 2.1). The decrease in employer-based coverage for children was
INSURANCE COVERAGE TRENDS (MILLIONS) FOR CHILDREN (TABLE 2.3) AND FOR ADULTS (TABLE 2.4)
TABLE 2.3 Trends in Health Insurance Coverage by Actual Numbers Among Children, Ages 0-17 United States, 1987-1995
|
|
Number (in millions) |
||||||||
|
Health Insurance Source |
1987 |
1988 |
1989 |
1990 |
1991 |
1992 |
1993 |
1994 |
1995 |
|
Total private |
47.3 |
47.5 |
48.1 |
46.9 |
46.6 |
47.2 |
47.0 |
46.3 |
47.0 |
|
Employer-based |
43.1 |
43.2 |
43.3 |
42.5 |
42.2 |
42.6 |
41.5 |
41.0 |
41.7 |
|
Self-pay |
4.2 |
4.2 |
4.8 |
4.4 |
4.3 |
4.6 |
5.5 |
5.3 |
5.4 |
|
Total public |
12.4 |
12.6 |
12.8 |
14.8 |
16.3 |
17.3 |
18.7 |
18.6 |
18.8 |
|
Medicaid |
10.0 |
10.3 |
10.5 |
12.5 |
14.0 |
15.1 |
16.7 |
16.1 |
16.5 |
|
Military health carea |
2.6 |
2.5 |
2.4 |
2.4 |
2.4 |
2.4 |
2.3 |
2.7 |
2.3 |
|
Medicareb |
0.1 |
0.1 |
0.0 |
0.1 |
0.1 |
0.1 |
0.0 |
0.2 |
0.3 |
|
Uninsured |
8.5 |
8.7 |
8.9 |
8.8 |
8.7 |
8.7 |
9.6 |
10.0 |
9.8 |
|
Total, children 0-17 |
64.6 |
65.0 |
65.8 |
66.4 |
67.4 |
68.7 |
69.8 |
70.5 |
71.1 |
|
NOTE: Columns may not add to totals because individuals may receive coverage from more than one source during 1 year. a Military Health Care includes the Civilian Health and Medical Program for the Uniformed Services and health care through the U.S. Department of Veterans Affairs. b For Medicare, numbers for some years round to less than 0.1 million, and are indicated by "0.0." SOURCE: EBRI (1997) Estimates are based on data from the March 1988-1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce. |
|||||||||
TABLE 2.4 Trends in Health Insurance Coverage Among Adults, Ages 18-64, United States, 1987-1995 (Millions)
|
|
Number (in millions) |
||||||||
|
Health Insurance Source |
1987 |
1988 |
1989 |
1990 |
1991 |
1992 |
1993 |
1994 |
1995 |
|
Total private |
115.6 |
115.5 |
116.3 |
115.3 |
114.8 |
113.4 |
114.6 |
116.5 |
116.9 |
|
Employer-based |
105.5 |
106.2 |
106.6 |
105.3 |
105.5 |
103.4 |
103.4 |
105.3 |
106.2 |
|
Self-pay |
10.1 |
9.3 |
9.7 |
9.9 |
9.3 |
10.0 |
11.1 |
11.2 |
10.6 |
|
Total public |
16.1 |
16.1 |
15.9 |
17.1 |
18.1 |
18.7 |
19.4 |
20.4 |
19.6 |
|
Medicaid |
8.4 |
8.6 |
8.7 |
9.9 |
10.8 |
11.4 |
12.3 |
12.6 |
12.5 |
|
Military health carea |
6.9 |
6.6 |
6.3 |
6.4 |
6.2 |
6.0 |
6.0 |
6.9 |
5.9 |
|
Medicareb |
3.1 |
3.1 |
3.2 |
3.4 |
3.5 |
3.8 |
3.7 |
2.9 |
3.2 |
|
Uninsured |
23.3 |
24.9 |
25.3 |
26.8 |
27.7 |
29.6 |
29.8 |
29.4 |
30.5 |
|
Total, adults 18-64 |
149.9 |
151.5 |
152.7 |
154.2 |
155.5 |
156.8 |
158.3 |
159.4 |
160.7 |
|
NOTE: Columns may not add to totals because individuals may receive coverage from more than one source during 1 year. a Military Health Care includes the Civilian Health and Medical Program for the Uniformed Services and health care through the U.S. Department of Veterans Affairs. b For Medicare, numbers for some years round to less than 0.1 million, and are indicated by "0.0." SOURCE: EBRI, 1997 Estimates are based on data from the March 1988-1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce. |
|||||||||
offset by an increase of almost 8 percent in Medicaid coverage between 1989 and 1993 (see Table 2.1 and especially Figure 2.1).
There are a variety of interpretations and substantial disagreement, however, about the relationship between the decrease in employer-based coverage and the increase in Medicaid coverage. At the heart of the issue is the concern that employers and employees might drop private health insurance to take advantage of increasing Medicaid eligibility thresholds to higher levels of income. Others maintain that shifting employment patterns, including the large scale shift from manufacturing to service sector jobs, account for the decline in employer coverage. Thus, the issue of replacement or substitution of coverage, or "crowding out," is controversial. This issue is discussed later in this chapter.
Trends in Coverage for Adults
Employer-based coverage decreased for adults as well as for children over the period from 1987 to 1995. However, the rate of decrease was faster for children, particularly in the 1990s (see Tables 2.1 and 2.2 and Figures 2.2 and 2.3).
During the same period that private coverage for adults was decreasing, the percentage of uninsured adults was increasing (Figure 2.3) and the percentage of adults with Medicaid was about the same. This suggests that adults who lose employer-based coverage are more likely to become uninsured than to enroll in Medicaid (Figure 2.3).
Demographics Of Coverage For Children
Age
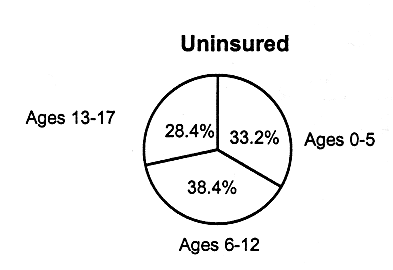
As indicated in Figures 2.4 and 2.5, the age distributions for children with employer-based coverage and uninsured children are similar. However, among children with Medicaid coverage, a disproportionate number (approximately 80 percent) are in the younger age groups (43.6 percent ages 0 to 5, 36.8 percent ages 6-12). This is true, in part, because families with young children are more likely to be poor and eligible for Medicaid compared with families with older children.
In addition, the Medicaid expansions enacted in the late 1980s are being phased in by age, with younger children gaining coverage before older children. Some policy analysts and health services researchers interpret the larger number of Medicaid-insured younger children as evidence that the Medicaid expansions have effectively reached the intended age group.
Race and Ethnicity
As indicated in Figures 2.6 and 2.7, the patterns of children's health insurance coverage among children by race and ethnicity are not uniform. In general, children of color are disproportionately more likely to be uninsured. These figures present national aggregated data; state and regional differences in distribution may be significantly different.
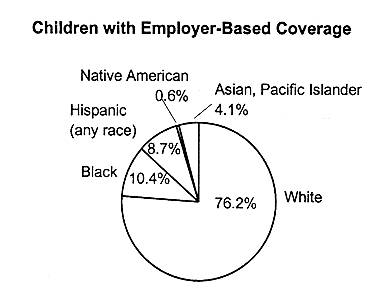
Most children with employer-based coverage (76 percent) are white; and most white children (69 percent) have employer-based coverage.
Among black children, fewer than 40 percent have employer-based coverage, close to half (45 percent) have Medicaid coverage, and about one in six (15 percent) have no insurance.
More than one in four Hispanic children (27 percent) are uninsured, whereas 35 percent have private insurance and about 37 percent have Medicaid coverage.
Among Native Americans, about one third (33 percent) have employer-based coverage, almost half (45 percent) have Medicaid, and approximately 11 percent are eligible to use the Indian Health Service.
On a national basis, Asian-American children make up approximately 4 percent of the total in each
EMPLOYER-BASED COVERAGE HAS BEEN DECLINING AMONG CHILDREN (FIGURE 2.1) AND AMONG ADULTS (FIGURE 2.2)
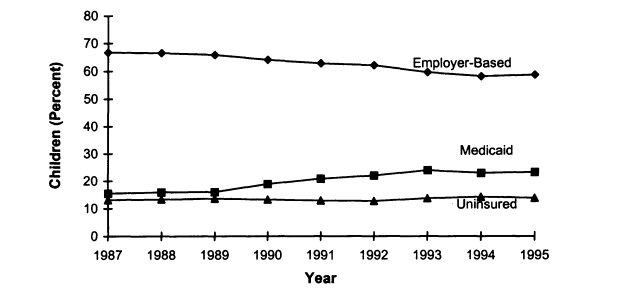
FIGURE 2.1
Trends in health insurance coverage among children, ages 0-17, United States, 19871995. SOURCE: EBRI (1997) Estimates are based on data from the March 1988-1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce.
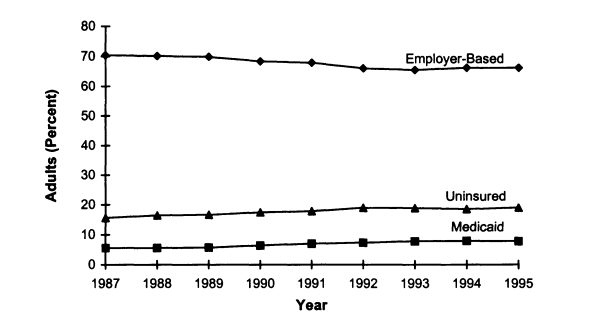
FIGURE 2.2
Trends in health insurance coverage among adults, ages 18-64, United States, 1987-1995. SOURCE: EBRI (1997) Estimates are based on data from the March 1988-1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce.
CHILDREN'S MEDICAID COVERAGE HAS INCREASED SINCE 1987
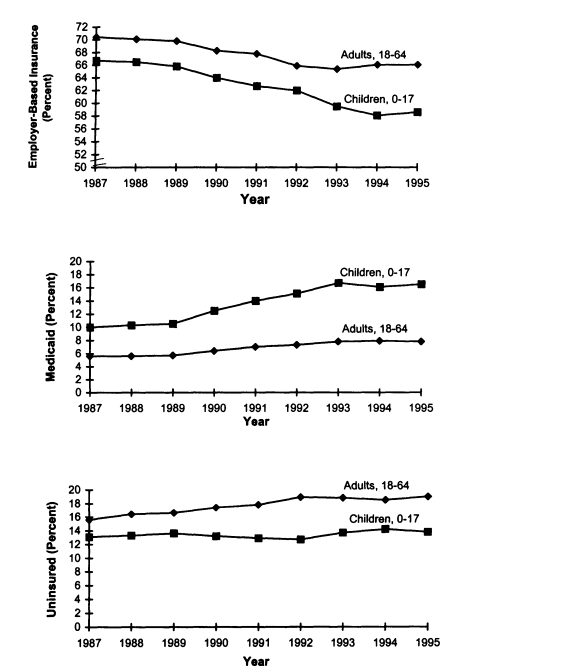
FIGURE 2.3
Comparison of trends in health insurance coverage for adults, ages 18-64, and children, ages 0-17, United States, 1987-1995. SOURCE: EBRI (1997) Estimates are based on data from the March 1988-1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce.
MEDICAID COVERS A HIGHER PROPORTION OF YOUNGER CHILDREN
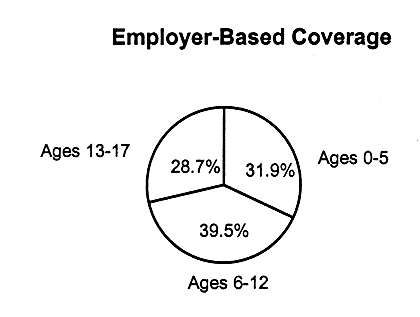
|
Employer-Based Coverage |
||
|
Age Group |
Number (in millions) |
Percent |
|
Ages 0-5 |
13.7 |
31.9 |
|
Ages 6-12 |
17.0 |
39.5 |
|
Ages 13-17 |
12.3 |
28.7 |
|
Total |
43.0 |
100.0 |
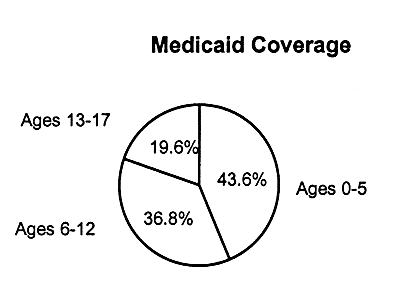
|
Medicaid Coverage |
||
|
Age Group |
Number (in millions) |
Percent |
|
Ages 0-5 |
7.2 |
43.6 |
|
Ages 6-12 |
6.1 |
36.8 |
|
Ages 13-17 |
3.2 |
19.6 |
|
Total |
16.5 |
100.0 |
|
Uninsured |
||
|
Age group |
Number (in millions) |
Percent |
|
Ages 0-5 |
3.2 |
33.2 |
|
Ages 6-12 |
3.8 |
38.4 |
|
Ages 13-17 |
2.8 |
28.4 |
|
Total |
9.8 |
100.0 |
FIGURE 2.4
Patterns of children's health insurance coverage by age, for employer-based insurance, Medicaid,and children without coverage, United States, 1995. SOURCE: EBRI, 1997, special tabulations. Estimates are based on data from the 1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce.
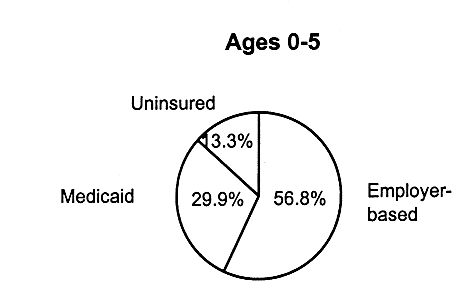
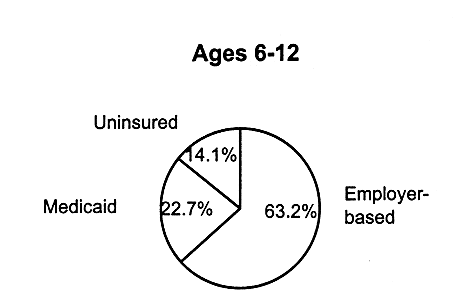
SOURCES OF CHILDREN'S HEALTH INSURANCE COVERAGE VARY WITHIN AGE GROUPS
|
Ages 0-5 |
||
|
Insurance Status |
Number (in millions) |
Percent |
|
Employer-based |
13.7 |
56.8 |
|
Medicaid |
7.2 |
29.9 |
|
Uninsured |
3.2 |
13.3 |
|
Total |
24.1 |
100.0 |
|
Ages 6-12 |
||
|
Insurance Status |
Number (in millions) |
Percent |
|
Employer-based |
17.0 |
63.2 |
|
Medicaid |
6.1 |
22.7 |
|
Uninsured |
3.8 |
14.1 |
|
Total |
26.9 |
100.0 |
|
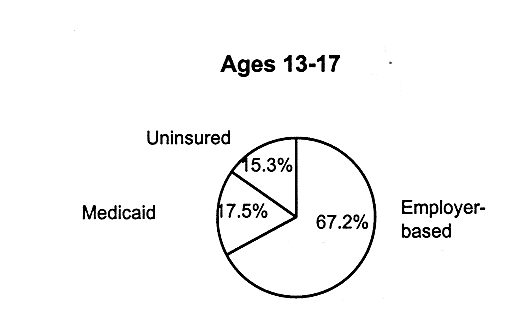
Ages 13-17 |
||
|
Insurance Status |
Number (in millions) |
Percent |
|
Employer-based |
12.3 |
67.2 |
|
Medicaid |
3.2 |
17.5 |
|
Uninsured |
2.8 |
15.3 |
|
Total |
18.3 |
100.0 |
FIGURE 2.5
Children's health insurance coverage within age groups, for employer-based insurance, Medicaid, and uninsured children, United States, 1995. SOURCE: EBRI (1997). Estimates are based on data from the 1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce.
CHILDREN OF COLOR ARE MORE LIKELY TO BE ON MEDICAID OR UNINSURED
|
Employer-Based Coverage |
||
|
Race/Ethnicity |
Number (in millions) |
Percent |
|
White |
31.8 |
76.2 |
|
Black |
4.3 |
10.4 |
|
Hispanic (any race) |
3.6 |
|
|
Native American, Eskimo, Aleut |
0.3 |
|
|
Asian, Pacific Islander |
1.7 |
|
|
Total |
41.7 |
|
|
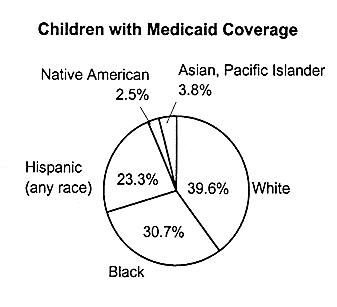
Medicaid Coverage |
||
|
Race/Ethnicity |
Number (in millions) |
Percent |
|
White |
6.5 |
39.6 |
|
Black |
5.1 |
30.7 |
|
Hispanic (any race) |
3.8 |
23.3 |
|
Native American, Eskimo, Aleut |
0.4 |
2.5 |
|
Asian, Pacific Islander |
0.6 |
3.8 |
|
Total |
16.5 |
100.0 |
|
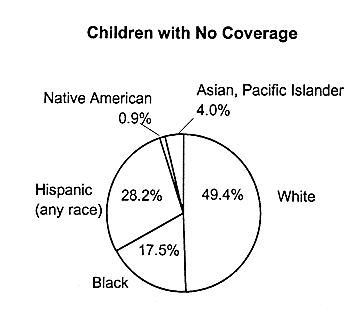
No Coverage |
||
|
Race/Ethnicity |
Number (in millions) |
Percent |
|
White |
4.8 |
49.4 |
|
Black |
1.7 |
17.5 |
|
Hispanic (any race) |
2.8 |
28.2 |
|
Native American, Eskimo, Aleut |
0.1 |
0.9 |
|
Asian, Pacific Islander |
0.4 |
4.0 |
|
Total |
9.8 |
100.0 |
FIGURE 2.6
Health insurance coverage among children by race and ethnicity, United States, 1995. SOURCE: EBRI (1997) Estimates are based on data from the 1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce.
CHILDREN'S HEALTH INSURANCE COVERAGE VARIES AMONG RACIAL AND ETHNIC GROUPS
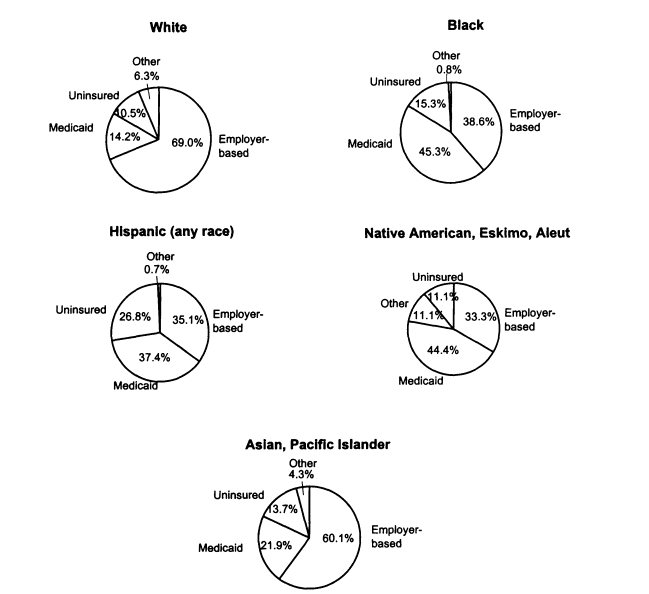
FIGURE 2.7
Patterns of health insurance coverage among children by race andethnicity, United States, 1995. SOURCE: EBRI (1997). Data are based on estimates from the 1996 CurrentPopulation Survey, Bureau of the Census, U.S. Department of Commerce.
of the three major coverage groups: private coverage, Medicaid, and uninsured. However, in California, Asian-Americans comprise approximately 20 percent of the population and approximately 12 percent of the uninsured children (Children Now, 1997).
Many, but not all, of these differences by race and ethnicity correspond to differences in parental employment and thus relate to family income. An analysis of the data from the National Medical Expenditure Survey found that poverty, minority status, and absence of insurance each had independent effects on access to and the use of primary care, but that there was overlap among the groups: among children in at least one of these at-risk groups, 40 percent also had another risk factor. In other words, children who are uninsured are more likely to be poor and to be from a racial or ethnic minority (Newacheck et al., 1996).
Along with the growing diversity of the American population throughout all regions of the country, the availability of culturally appropriate health care services also varies. However, in designing new children's insurance expansions, it will be important to have current information on the racial and ethnic distributions of children by insurance status at the state level and local levels. Without such information, it will be more difficult to focus appropriate outreach and enrollment efforts on the communities with the highest concentrations of uninsured children.
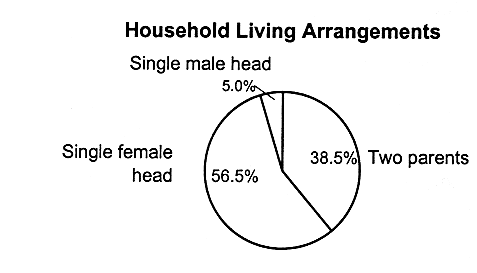
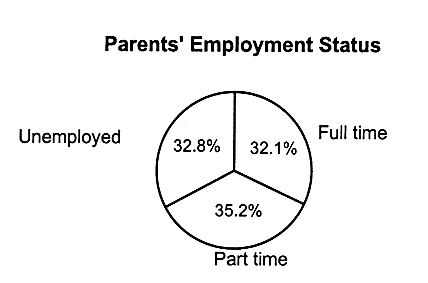
Family Structure and Parental Employment
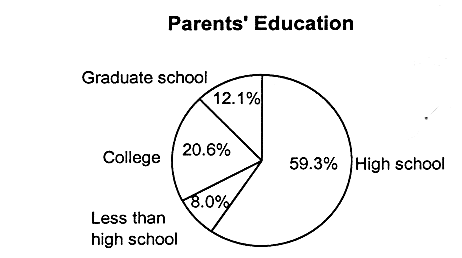
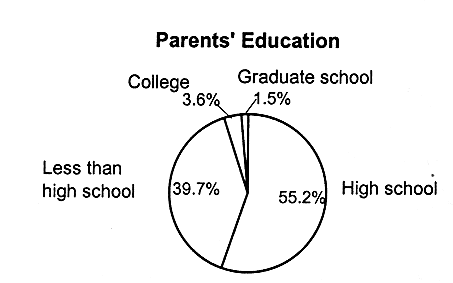
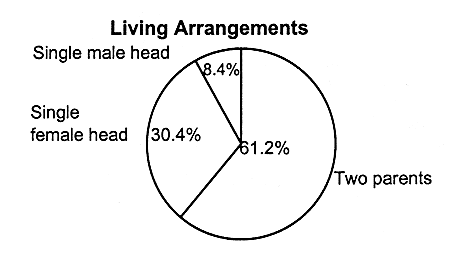
Figures 2.8, 2.9, and 2.10 present the breakdowns of household living arrangements, parents' employment status, family income, and parents' education status for children who have employer-based coverage and Medicaid, and for those who are uninsured, respectively.
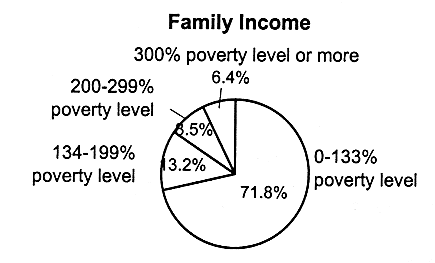
Not surprisingly, the majority of children with employer-based coverage live in two-parent, working families (see Figure 2.8). More than half (54 percent) live in families with incomes that are 300 percent of the federal poverty level or higher. Children with Medicaid coverage are more likely to live in single-parent families (61.5 percent) in which the family income is 133 percent of the federal poverty level or less (71.8 percent) (see Figure 2.9 for Medicaid breakdowns, and see also Table 2.5 for breakdowns of federal poverty thresholds by family size).
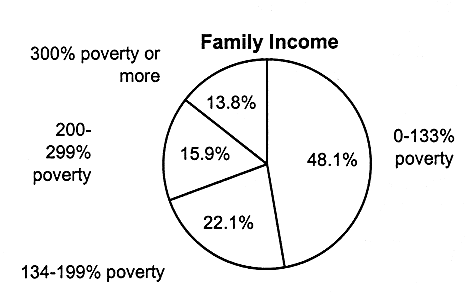
The majority of uninsured children live in two-parent, working families (see Figure 2.10). Thus, parents of most uninsured children have been described as being among the ''working poor." Almost half of uninsured children (48 percent) live in families whose incomes are below the 133 percent of the federal poverty level ($20,706.77 for a family of four in 1995).
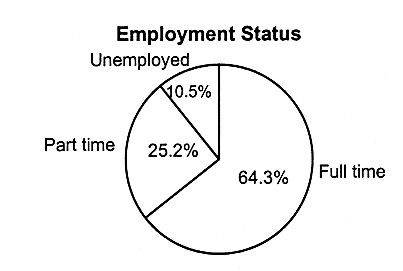
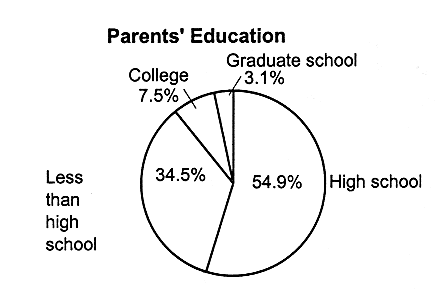
More than half (55 percent) of the uninsured children have parents who finished high school. The majority of children who are uninsured (64 percent) live in families in which someone works full time year-round, typically in service industries, seasonal work, or other low-wage jobs in small businesses.
Evidence suggests that the majority of workers who are offered insurance coverage through their employer will enroll (Nichols et al., 1997). Small employers are less likely to offer health insurance to their workers than are large employers, and small employers tend to provide less-comprehensive benefits than do large employers (Nichols et al., 1997). However, the available evidence shows no clear relationship between firm size and the size of employees' contributions for dependent coverage (Nichols et al., 1997), suggesting that employers consider more than just the number of their employees in designing their benefits and cost-sharing requirements.
Duration Of Lack Of Coverage
According to data from the Census Bureau's Survey of Income and Program Participation, millions of children spent several months without coverage between 1992 and 1994. Only 12 percent of uninsured children lacked coverage for 3 months or less. Nearly 40 percent were without coverage for 4 to 9 months, and half (50 percent) were without coverage for 10 months or more (see Figure 2.11).
MOST CHILDREN WITH PRIVATE INSURANCE LIVE IN TWO-PARENT, WORKING FAMILIES
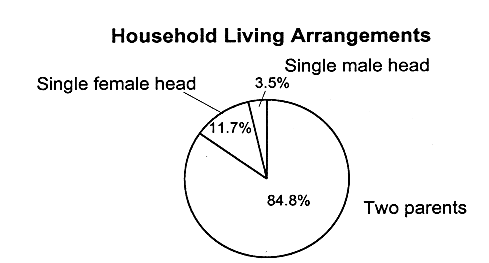
|
Living Arrangements |
Number (in millions) |
Percent |
|
Two parents |
35.3 |
84.8 |
|
Single female head |
4.9 |
11.7 |
|
Single male head |
1.5 |
3.5 |
|
Total |
41.7 |
100.0 |
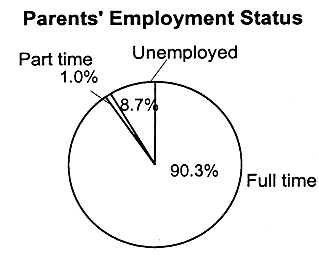
|
Parents' Employment Status |
Number (in millions) |
Percent |
|
Full time employee |
37.4 |
90.3 |
|
Part time employee |
0.4 |
0.9 |
|
Unemployed |
3.6 |
8.7 |
|
Totala |
41.4 |
100.0 |
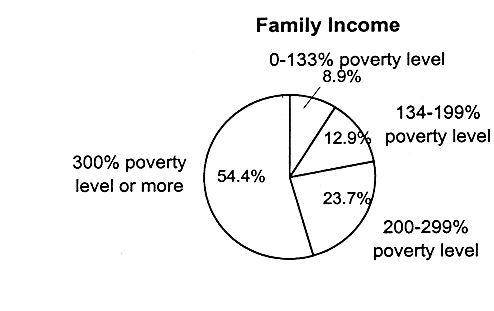
|
Family Income |
Number (in millions) |
Percent |
|
0-133% poverty level |
3.7 |
8.8 |
|
134-199% poverty level |
5.4 |
12.9 |
|
200-299% poverty level |
9.9 |
23.9 |
|
300% poverty level or more |
22.7 |
54.4 |
|
Total |
41.7 |
100.0 |
|
Parents' Education |
Number (in millions) |
Percent |
|
High school |
24.5 |
59.3 |
|
Less than high school |
3.3 |
8.0 |
|
College |
8.5 |
20.8 |
|
Graduate school |
5.0 |
12.1 |
|
Totalb |
41.3 |
100.0 |
FIGURE 2.8
Characteristics of families of children with employer-based insurance coverage, ages 0-17, United States, 1995.
SOURCE: EBRI (1997). Estimates are based on data from the 1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce. a.b The total number does not equal the number of children with employer-based insurance (41.7 million), because some children do not live with a parent; that is, they may live in foster care or with other relatives.
MOST CHILDREN WITH MEDICAID LIVE IN SINGLE-PARENT, WORKING FAMILIES
|
Living Arrangements |
Number (in millions) |
Percent |
|
Two parents |
6.4 |
38.5 |
|
Single female head |
9.3 |
56.5 |
|
Single male head |
0.8 |
5.0 |
|
Total |
16.5 |
100.0 |
|
Parents' Employment Status |
Number (in millions) |
Percent |
|
Full time employee |
5.1 |
32.1 |
|
Part time employee |
5.6 |
35.2 |
|
Unemployed |
5.2 |
32.8 |
|
Totala |
15.9 |
100.0 |
|
Family Income |
Number (in millions) |
Percent |
|
0-133% poverty level |
11.9 |
71.8 |
|
134-199% poverty level |
2.2 |
13.2 |
|
200-299% poverty level |
1.4 |
8.5 |
|
300% poverty level or more |
1.2 |
6.4 |
|
Total |
16.5 |
100.0 |
|
Parents' Education |
Number (in millions) |
Percent |
|
High school |
8.8 |
55.2 |
|
Less than high school |
6.3 |
39.7 |
|
College |
0.6 |
3.6 |
|
Graduate school |
0.2 |
1.5 |
|
Totalb |
15.9 |
100.0 |
FIGURE 2.9
Characteristics of families of children with Medicaid coverage, ages 0-17, United States, 1995.
SOURCE: EBRI (1997). Estimates are based on data from the March 1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce. a,b The total number does not equal the number of children with Medicaid (16.5 million), because some children do not live with a parent; that is, they may live in foster care or with other relatives.
MOST UNINSURED CHILDREN LIVE IN TWO-PARENT, WORKING FAMILIES
|
Living Arrangements |
Number (in millions) |
Percent |
|
Two parents |
6.0 |
61.2 |
|
Single female head |
3.0 |
30.4 |
|
Single male head |
0.8 |
8.4 |
|
Total |
9.8 |
100.0 |
|
Parents' Employment Status |
Number (in millions) |
Percent |
|
Full time employee |
6.0 |
64.3 |
|
Part time employee |
2.3 |
25.2 |
|
Unemployed |
1.0 |
10.5 |
|
Totala |
9.3 |
100.0 |
|
Family Income |
Number (in millions) |
Percent |
|
0-133% poverty |
4.7 |
48.1 |
|
134-199% poverty |
2.2 |
22.1 |
|
200-299% poverty |
1.6 |
15.9 |
|
300% poverty or more |
1.43 |
13.8 |
|
Total |
9.8 |
99.9 |
|
Parents' Education |
Number (in millions) |
Percent |
|
High school |
5.1 |
54.9 |
|
Less than high school |
3.2 |
34.5 |
|
College |
0.7 |
7.5 |
|
Graduate school |
0.3 |
3.1 |
|
Total |
9.3 |
100.0 |
FIGURE 2.10
Characteristics of families of uninsured children, ages 0-17, United States, 1995. a,b The totals in these categories do not equal the number of uninsured (9.8 million), because some children do not live with a parent; that is, they may live in foster care or with other relatives.
SOURCE: EBRI (1997). Estimates are based on data from the March 1996 Current Population Survey, Bureau of the Census, U.S. Department of Commerce.
TABLE 2.5 Federal Poverty Thresholds, by Size of Family, United States, 1995
|
|
|
Annual Income (in dollars) for the Following Poverty Level: |
||
|
Size of Family |
Poverty Level Threshold ($) |
133% |
200% |
300% |
|
One person |
7,763.00 |
10,324.79 |
15,526.00 |
23,289.00 |
|
Under 65 years |
7,929.00 |
10,545.57 |
15,858.00 |
23,787.00 |
|
65 years and over |
7,309.00 |
9,720.97 |
14,618.00 |
21,927.00 |
|
Two persons |
9,933.00 |
13,210.89 |
19,866.00 |
29,799.00 |
|
Householders under 65 years |
10,529.00 |
14,003.57 |
21,058.00 |
31,587.00 |
|
Householders 65 years and over 9,219.00 |
12,261.27 |
18,438.00 |
27,657.00 |
|
|
Three persons |
12,158.00 |
16,170.14 |
24,316.00 |
36,474.00 |
|
Four persons |
15,569.00 |
20,706.77 |
31,138.00 |
46,707.00 |
|
Five persons |
18,408.00 |
24,482.64 |
36,816.00 |
55,224.00 |
|
Six persons |
20,804.00 |
27,669.32 |
41,608.00 |
62,412.00 |
|
Seven persons |
23,552.00 |
31,324.16 |
47,104.00 |
70,656.00 |
|
Eight persons |
26,237.00 |
34,895.21 |
52,474.00 |
78,711.00 |
|
Nine persons or more |
31,280.00 |
41,602.40 |
62,560.00 |
93,840.00 |
|
SOURCE: Bureau of the Census (1995), Current Population Survey [www document]. (http://www.census.gov/hhes/poverty/threshld/thresh95.html) |
||||
Taken as a whole, these data suggest that spells without coverage can be substantial and widespread and can involve millions of children. Indeed, some 20 million children experienced at least one spell when they were uninsured during the 1992-1994 period (Table 2.6).
If children's episodes without coverage coincide with any major illnesses or injuries, their families face large out-of-pocket expenses for medical treatment. If families choose to forego treatment initially because of the cost, untreated illnesses and injuries can escalate in severity and can become much more costly to treat later on.
Much of the care provided to uninsured families becomes bad debt and is thus described by providers as "uncompensated care." As discussed in Chapter 4 of this report, uncompensated care provided by hospitals has historically been offset in part by Disproportionate Share Hospital (DSH) payments made under Medicaid and Medicare. The Balanced Budget Act of 1997 significantly reduced the amount of DSH funding and also eliminated cost-based reimbursement for community health centers. For these and other reasons discussed in Chapter 4, safety net providers need to change the structure of their services and to identify other financial resources to pay for or to offset the costs of uncompensated care.
Regional Variations In Lack Of Coverage
Figure 2.12 shows the state-by-state variations in the rates of uninsured children. The highest rates (greater than 20 percent) are in central southeastern, south-central, and southwestern states (Mississippi, Louisiana, Oklahoma, Texas, New Mexico, Arizona, and Nevada). The lowest rates (less than 10 percent) are in the northern tier. Moving from east to west, the rates of uninsured children are lowest in Pennsylvania, West Virginia, Ohio, Michigan, Illinois, Wisconsin, Minnesota, North Dakota, South Dakota, Nebraska, Montana, and Washington.
There are tremendous state-to-state variations in the availability of employer-sponsored health
MOST UNINSURED CHILDREN LACK COVERAGE FOR SEVERAL MONTHS
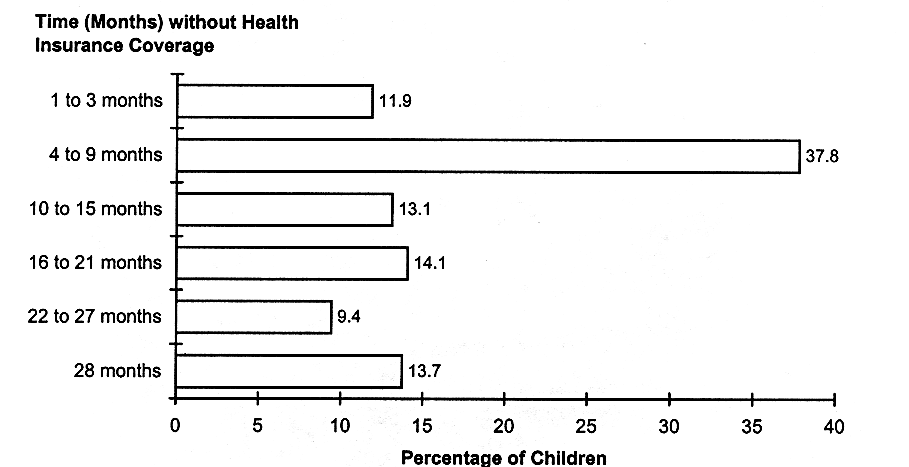
FIGURE 2.11
Percentage of children without health insurance coverage, ages 0-17, by number of consecutive months without coverage, United States, 1992-1994. SOURCE: Bennefield (1996).
TABLE 2.6 Number and Percentage of Children Without Health Insurance Coverage, Ages 0-17, by Number of Consecutive Months Without Coverage, United States, 1992-199
|
Time (months) with No Coverage |
Percentage of Total |
Number (in millions) |
|
None (covered full period) |
70.0 |
47.7 |
|
1 to 28 months (uninsured) |
30.0 |
20.4 |
|
1 to 3 months |
11.9 |
2.4 |
|
4 to 9 months |
37.8 |
7.7 |
|
10 to 15 months |
13.1 |
2.7 |
|
16 to 21 months |
14.1 |
2.9 |
|
22 to 27 months |
9.4 |
7.9 |
|
28 months |
13.7 |
2.8 |
|
Total |
100.0 |
68.1 |
|
SOURCE: Bennefield (1996). |
||
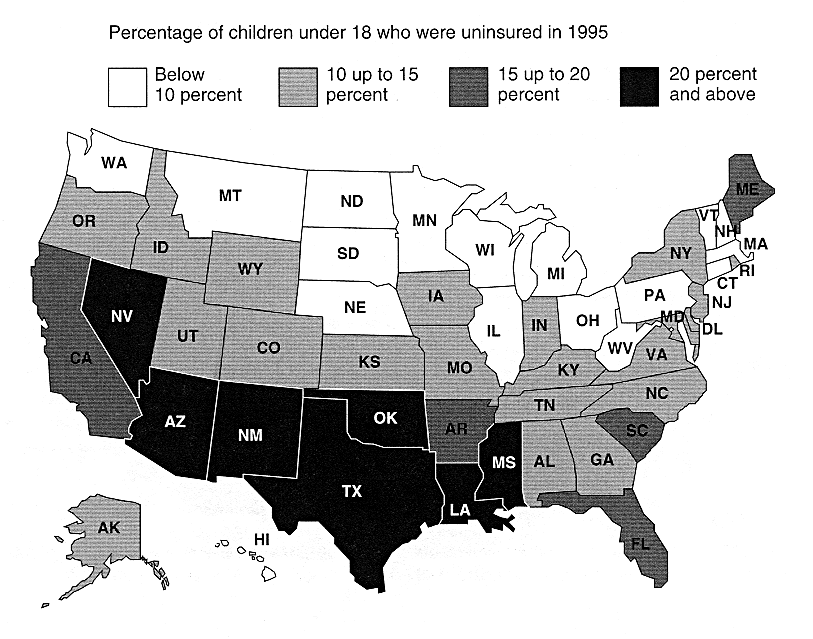
FIGURE 2.12
Distribution of uninsured children by state, 1995.
insurance (NCHS, 1998). Variability occurs because of state and regional differences in the industry and employment base, such as the distribution of large versus small employers, and in the coverage and cost-sharing options they customarily offer (Holahan, 1997). For example, children and adults in the South traditionally have had lower rates of employer-based coverage and correspondingly higher rates of uninsurance.
Another reason for state and regional differences in rates of uninsured children is because of the variability of state experiments with health insurance for children and state participation in Medicaid options. Some states—notably Massachusetts, Minnesota, and Florida—have undertaken successful expansions of children's health insurance coverage. Some private insurance initiatives (e.g., Caring Programs) operate in several states (see discussion in Chapter 6). In other states, however, there has been little or no previous activity in the children's health insurance coverage arena.
The State Children's Health Insurance Program (SCHIP) created under the Balanced Budget Act of 1997 recognized this tremendous variability among the states and built on the variety of approaches already being taken in several states. SCHIP was designed to give states flexibility and choice, and the flexibility appeals to most states. The national patterns of coverage are likely to change as a result of SCHIP, but it is too early to tell whether the states with the highest rates of uninsured children will develop programs that are most successful in expanding insurance coverage.
Summary And Discussion
Trends in Children's Health Insurance Coverage
Employer-based coverage is decreasing more rapidly for children than for adults. Although the percentage of children without coverage remained relatively stable between 1987 and 1995, the absolute number of uninsured children increased, from 8.5 million in 1987 to 9.8 million in 1995. The percentage of uninsured children remained stable over that period primarily because increases in Medicaid enrollments offset declines in employer-based coverage.
Among Medicaid enrollees, young children (ages 0 to 5) are the largest age group (43.6 percent). This suggests that Medicaid expansions to younger children have been effective in reaching them.
Patterns of coverage differ for racial and ethnic minorities. Black and Hispanic children are more likely than white children to lack coverage. Nationally, one of every six black children and one of every four Hispanic children is uninsured. Among white children, 1 of every 10 is uninsured.
Racial and ethnic variations in coverage have important implications for outreach and enrollment strategies for new insurance programs. These strategies should be designed to reach the groups with highest rates of uninsurance, and should be culturally sensitive and culturally appropriate in order to increase the likelihood of participation.
Some Concerns About Substitution of Coverage
Evidence is fairly clear that rates of employer-based health insurance coverage for children declined from 1987 to 1995 and that rates of Medicaid enrollment increased for children over the same time period. It is less clear whether the relationship is causal—that is, whether the availability of Medicaid actually caused employers and employees to drop dependent coverage. The available evidence comes from aggregated data reported in national surveys. Because data on specific employer and employee decision making about these issues are not readily available, the survey data are subject to different interpretations.
Many policymakers are concerned that the availability of public insurance through Medicaid or SCHIP will encourage employers and employees to drop their private coverage, also called substitution or crowding-out of coverage (Chollet et al., 1997; Cutler and Gruber 1996, 1997; Dubay and Kenney, 1997). Substitution can take place in one of two ways: (1) An employer that currently provides coverage for children may stop covering dependents or may continue to offer coverage but increase the amount that employees must pay to receive dependent coverage, making it more likely that they will drop the coverage and try to replace it with public insurance; or (2) employees who are already paying a share of the cost of employer-based insurance might stop participating if, for example, they became eligible for new publicly funded programs.
Some researchers suggest that the decline in employer-based coverage is due primarily to the increases in health care costs, making employers less willing to offer coverage or more likely to shift the costs to employees, who in turn are less likely to accept the cost-sharing arrangements because of national declines in average real family incomes (Holahan et al., 1995). Others have suggested that the reductions in employer coverage may be largely attributable to the shift in jobs from the manufacturing sector to the service sector, where insurance is less likely to be offered as a benefit (Newacheck et al., 1995).
These employer trends thus may be occurring independently of expansions in Medicaid or other public programs like it. There does not appear to be any evidence that most employers are familiar with Medicaid program requirements in their states. Nor is there evidence that most people are aware of the Medicaid requirements in their states: in fact, the widespread underenrollment of eligible children in Medicaid would suggest the opposite.
There is evidence, however, that cost-sharing affects consumer health care purchasing decisions. For example, in a recent study of premium levels and participation in state-subsidized health insurance programs, Urban Institute researchers found that when families were charged 1 percent of their income, 57 percent joined a subsidized program; when the charge was 3 percent of income, 35 percent joined; and when the charge was 5 percent of income, only 18 percent joined (Ku and Coughlin, 1997).
Methodological differences across surveys have made it difficult to derive an exact estimate of the extent of crowd-out or coverage replacement (Chollet et al., 1997; Cutler and Gruber, 1996, 1997; Dubay and Kenney, 1997). Among poor children, those up to 200 percent of poverty, there tends to be relatively little substitution of coverage because few are likely to have private coverage in the first place (Dubay and Kenney, 1997). As income levels increase, families are increasingly likely to have private coverage through their employers, and so there is a greater risk of substitution.
States that have already expanded coverage to medium-income families (i.e., up to 400 percent of poverty) have taken several steps, sometimes referred to as firewalls, to reduce incentives to obtain replacement coverage. California and Minnesota use waiting periods to discourage people from moving from a private program to a public one: a child must be uninsured for at least 4 months before an application can be submitted for the new program. Several states have cost-sharing requirements, usually monthly fees charged on a sliding scale starting at 200 percent of the federal poverty level (Children Now, 1997; Chollet et al., 1997). Most state officials believe that these types of measures are effective in deterring crowd-out without preventing eligible individuals from enrolling (Chollet et al., 1997).
Concern about crowd-out was reflected in the structure of the SCHIP legislation. In general, the program was designed to target uninsured children in families with incomes up to 200 percent of poverty. Eligible children are those who are not eligible for Medicaid (whether enrolled or not) and who are not covered by private insurance. Although states are free to design their own enrollment procedures and eligibility criteria, they are required to describe the procedures they will use to prevent substitution of coverage in the state SCHIP plans they submit to the Department of Health and Human Services for approval.
A recent study by the Urban Institute estimates that only about 2.9 million uninsured children will meet the income eligibility criteria set by SCHIP, and that the available funds could insure a total of nearly 6 million children (Ullman et al., 1998). In other words, there may be enough money in the SCHIP program to insure almost twice as many children as are eligible under the current program rules, and states may have difficulty finding enough eligible children to draw down their full federal allotments. For this and other reasons, the committee urges states to develop systems of accountability that will help to enroll as many eligible children as possible, track changes in enrollment and utilization patterns, and collect and analyze other information that will help to assess the impact of SCHIP over time (IOM, 1998).
References
Bennefield RL. 1996. Who Loses Coverage and for How Long? Current Population Reports P70-54. Washington, DC: Bureau of the Census, U.S. Department of Commerce.
Bureau of the Census. 1995. Current Population Survey 1995. Washington, DC: U.S. Department of Commerce.
Children Now. 1997. California's Working Families and Their Uninsured Children: A Big Problem With an Affordable Solution. Oakland, CA: Children Now.
Chollet DJ, Birnbaum ML, Sherman MJ. 1997. Deterring Crowd-Out in Public Insurance Programs: State Policies and Experience. Washington, DC: Alpha Center. [http://www.ac.org/]
Cutler D, Gruber J. 1997. Medicaid and Private Insurance: Evidence and Implications. Health Affairs 16(1):194-200.
Cutler D, Gruber J. 1996. Does Public Insurance Crowd out Private Insurance? Quarterly Journal of Economics 111:391-430.
Dubay L, Kenney G. 1997. Lessons from the Medicaid Expansions for Children and Pregnant Women: Implications for Current Policy. Statement for Hearing on Children's Access to Health Coverage, Subcommittee on Health, U.S. House Committee on Ways and Means, April 8, 1997. [http://www.urban.org/TESTIMON/dubay.html]
EBRI (Employee Benefit Research Institute). 1997. Special tabulations from the Bureau of the Census Current Population Survey prepared for the Institute of Medicine Committee on Children, Health Insurance, and Access to Care. Washington, DC: EBRI.
Holahan J. 1997. Expanding Insurance Coverage for Children. Washington, DC: Urban Institute.
IOM (Institute of Medicine). 1993. Employment and Health Benefits: A Connection at Risk. Washington, DC: National Academy Press.
IOM. 1998. Systems of Accountability: Implementing Children's Health Insurance Programs. Washington, DC: National Academy Press.
Ku L, Coughlin TA. 1997. The Use of Sliding Scale Premiums in Subsidized Insurance Programs. Washington, DC: Urban Institute. [http://www.urban.org/entitlements/premium.htm]
NCHS (National Center for Health Statistics). 1998. Employer-Sponsored Health Insurance: State and National Estimates. Rockville, MD: Centers for Disease Control and Prevention. [http://www.cdc.gov.nchswww/]
Newacheck PW, Hughes DC, Cisternas M. 1995. Children and Health Insurance: An Overview of Recent Trends. Health Affairs 14(1):244-254.
Newacheck PW, Hughes DC, Stoddard JJ. 1996. Children's Access to Care: Differences by Race, Income, and Insurance Status. Pediatrics 97(1):26-32.
Nichols LM, Blumberg LJ, Acs GP, Uccello CE, Marsteller JA. 1997. Small Employers: Their Diversity and Health Insurance. Washington, DC: Urban Institute. [http://www.urban.org/health/smemployers.htm]
Schieber GJ, Poullier JP. 1989. Overview of International Comparisons of Health Care Expenditures. Pp. 1-7 in Health Care Financing Review Annual Supplement 1989.
Ullman F, Bruen B, Holahan J. 1998. The State Children's Health Insurance Program: A Look at the Numbers. Washington, DC: Urban Institute. [http://www.urban.org]
Weigers ME, Weinick RM, Cohen JW. 1998. Children's Health, 1996. MEPS Chartbook No. 1. Rockville, MD: Agency for Health Care Policy and Research.





















