Executive Summary
The National Institutes of Health (NIH) is the leading federal agency supporting research related to improving the nation's health. The scientists and clinicians whom it has helped train and support have consistently been at the forefront of research discoveries that have advanced fundamental knowledge of human biology and of better ways to treat or prevent disease and promote good health. Over the past 50 years, NIH as an institution has played a major role in the explosion of knowledge that has amounted to a revolution in biology.
NIH's success has earned it steadily increasing budgets even when the overall federal budget has been tight, as it has been in recent years. Although the NIH budget for the current fiscal year (1998) is more than $13 billion and both the administration and the U.S. Congress have promised a substantial increase for 1999, it will never be large enough to meet every need or fund every promising lead. Choices must be made and priorities must be set.
Concerns about priority setting in the allocation of NIH research funding come from several sources. First, some members of Congress believe that there should be more of a correlation between the allocation of funding by disease and the distribution of disease burdens and costs in the population. Second, more and more disease-specific interest groups have begun campaigning for increases in NIH funding related to particular diseases. Additionally, many of these groups do not feel that NIH listens or responds to their inputs. Finally, the leadership of the health committees in Congress has become increasingly uncomfortable with intervening in research priority setting at NIH, for example, by mandating specific funding set-asides, new programs or institutions focused on specific diseases, or the use of particular research mechanisms or by trying to
push research advances in specific areas in other ways. For these reasons, this committee has been asked to evaluate the processes for setting priorities at NIH, particularly NIH's mechanisms for obtaining public input and the role of Congress in directing the allocation of funding among areas of research.
In setting priorities, NIH must also adapt to a changing policy environment. Despite having a growing budget, scientific research opportunities have grown even more rapidly, as has awareness of health problems as the population ages and as globalization exposes the U.S. population to emerging or reemerging infectious diseases.
To meet the expectations of the American people and fulfill the agency's mission, NIH's leaders must pursue many objectives. Two of the most important are (1) to identify the public's health needs, reducing the burdens of illness by developing better methods of prevention, diagnosis, treatment, and rehabilitation, and (2) to extend the basic knowledge base to lead to even better methods in the future. These two objectives are complementary and must be pursued with equal intensities if NIH is going to be successful. A third important objective is to communicate to the public and health providers the current state of scientific knowledge and the implications of research advances for improving the nation's health. Box 1 describes some of NIH's constituencies.
|
BOX 1 NIH Constituencies NIH interacts with various external constituencies who have a stake in research priority setting. These include:
|
Identifying the burden of illness, however, is not a straightforward task. As indicated in the NIH booklet ''Setting Research Priorities at the National Institutes of Health" (National Institutes of Health, 1997b) (referred to hereafter as Setting Research Priorities), there are many ways to measure the burden of disease because the problem can be analyzed and interpreted from many different perspectives. These are all relevant because the concept of the burden of disease is very broad.
When applied to illness, the burden includes the heavy load borne by society in providing services to prevent, cure, and care for the sick. It also includes the substantial losses of output to the economy due to disease, disability, and death. The burden on the family in caring for and accommodating a sick member of the household can also be severe. Finally, there is the burden of pain, discomfort, and suffering of each sick person and that of anguish and grief of relatives and friends (Institute of Medicine, 1976:2).
Assessing the burden of disease takes into account the fact that the benefits of past research have not reached everyone, indicated by significant differentials in disease rates and outcomes among different socioeconomic and ethnic groups. Also, about half the nation's health care costs result from unhealthy behaviors and environments, which pose major research challenges. In addition, state-of-the-art screening, diagnostic procedures, and treatments are not reaching everyone, resulting in unnecessary burdens of undetected or poorly treated diseases, and patient and provider knowledge could be improved through education. All of these factors must be weighed and balanced in the priority-setting process.
The committee assessed NIH's priority-setting process in light of the agency's mission and objectives and the changing policy environment. Are the criteria adequate? Is the process for implementing them working? Given the objective of responding to health needs as well as scientific opportunity, in conjunction with the expansion of organized disease-specific interest groups, are the mechanisms for public input adequate, or can they be changed to increase the complementarity between NIH's goals of responding to health needs and scientific opportunity? Can Congress, the holder of the public purse strings, be assured that NIH has a rigorous process for priority setting in which the full range of considerations is taken into account in planning programs and allocating funding?
The committee concludes that NIH's system for setting priorities has generally served NIH and the nation well in supporting research to improve human health, but some changes would strengthen it, especially in mechanisms for exchanging information and concerns with interested individuals and groups. The process by which NIH sets its research priorities should more fully engage the public (i.e., the public should have greater opportunity to learn about and provide input into the priority-setting process) in a process that is led by the director, guided by reasonable criteria, and well informed by robust analyses of health statistics. The process should be open and understandable, include multi-
year strategic planning, and give appropriate consideration to the competing needs of scientific opportunity and disease burden. Effective implementation of such a process would improve public access to the process and limit the need for congressional directives.
CRITERIA FOR PRIORITY SETTING
The committee reviewed the major criteria that NIH uses in its overall priority setting. These criteria were explicitly laid out in Setting Research Priorities, and the committee concluded that they are generally reasonable and useful both for allocating research resources and for enabling organized interest groups, members of Congress, and members of the public to understand and evaluate NIH's program. The criteria are
- public health needs,
- scientific quality of the research,
- potential for scientific progress (the existence of promising pathways and qualified investigators),
- portfolio diversification along the broad and expanding frontiers of research, and
- adequate support of infrastructure (human capital, equipment and instrumentation, and facilities).
The committee wants to be sure, however, that the conceptualization of the first criterion, public health needs, be broadened beyond the medical model implied in the discussion of the criterion in the booklet to include the preservation and maintenance of health and function.
Recommendation 1. The committee generally supports the criteria that NIH uses for priority setting and recommends that NIH continue to use these criteria in a balanced way to cover the full spectrum of research related to human health.
To enhance the legitimacy of and support for its priority-setting and resource allocation processes, NIH should work to increase the level of understanding of its criteria by the general public and of how they are implemented and should engage in regular evaluations of how the criteria are used and of their impacts. The Setting Research Priorities booklet and other documents are not as effective at gaining public understanding as they could be, for example, in informing citizens who are concerned about health and particular diseases about how they can become involved (an issue addressed more fully below in the section Mechanisms for Public Input).
Recommendation 2. NIH should make clear its mechanisms for implementing its criteria for setting priorities and should evaluate their use and effectiveness.
The committee found that some of the information needed for priority setting, especially data on disease burden and costs, is obtained rather informally and concluded that NIH should be more systematic in obtaining and analyzing such data. It should be kept in mind, however, that there is no simple metric for the use of these data, and the relationship between such data and allocations of research funding will not be simple because health problems are not equally ripe for research advances.
Recommendation 3. In setting priorities, NIH should strengthen its analysis and use of health data, such as burdens and costs of diseases, and of data on the impact of research on the health of the public.
Individuals and groups concerned about specific health problems or health research often use NIH-generated data on spending by specific disease or area of research to assess the overall research portfolio. The data are not of the quality that they could be, however, and NIH should work to improve the data and to better explain the data to the public. Calculations of spending by disease should include not only all research directly related to the disease but also research projects on fundamental areas indirectly related to that disease. Users of the data should know that such calculations reflect the best estimates of all NIH spending in particular areas and that fundamental science is essential to understanding the etiology and progression of disease.
NIH should also collect and analyze data on health research spending by others, such as other federal agencies, industry, nonprofit health organizations that fund research, foundations, or other countries. This should help identify gaps, overlaps, and opportunities for joint efforts and ensure that NIH invests wisely in areas and approaches that no one else is funding, provides the appropriate coordination, and supports the training of personnel and the other infrastructure needed in the national research enterprise.
Recommendation 4. NIH should improve the quality and analysis of its data on funding by disease and should include both direct and related expenditures.
PRIORITY-SETTING PROCESSES
Priority setting is decentralized at NIH, which is appropriate for a research organization in which those closest to a problem are in the best position to de-
cide on approaches and in which expertise is highly specialized. The priority setting processes also vary from institute to institute and from area to area within institutes. Some such variation is appropriate, because the institutes vary in their missions, histories, leadership, sizes, and complexities. The committee did find that some institutes and programs have priority-setting processes that incorporate a broader range of inputs and views, including those of nonresearchers and nonclinicians.
More recently, NIH has been making decisions on priorities and funding allocations that are more centralized than in the past; that is, NIH is looking across traditionally independent institutes and centers and focusing on certain crosscutting needs and opportunities where joint or unified action is desirable. This trend stems from the growing realization that common biological processes underlie diseases that were previously seen as different or that important diseases and other health problems are more complex than was previously thought, affect more organs and processes than was previously realized, and happen to be addressed in more than one institute.
The committee concluded that the Office of the Director of NIH needs an increased capacity to analyze such crosscutting needs and opportunities and to interact with the public (the latter process-related issue is addressed separately below). Improvement requires a more central role for the NIH director and more uniformity in the data and analyses presented to the Office of the Director.
Recommendation 5. In exercising the overall authority to oversee and coordinate the priority-setting process, the NIH director should receive from the directors of all of the institutes and centers multiyear strategic plans, including budget scenarios, in a standard format on an annual basis.
In any organization, change toward centralization raises concerns about accountability. As the authority of the director is strengthened, greater accountability of the director's office could be achieved through a strengthened Advisory Committee to the Director, one that is more actively engaged in the NIH priority-setting process and that has a broader base of membership, especially among its public members.
Recommendation 6. The director of NIH should increase the involvement of the Advisory Committee to the Director in the priority setting process. The diversity of the committee's membership should be increased, particularly with respect to its public members.
MECHANISMS FOR PUBLIC INPUT
Although a major criterion in research priority setting is public health needs, the committee found that NIH's interaction with various kinds of publics is generally weak compared with NIH's interaction with the research community. This is especially true for the Office of the Director of NIH, which does not have adequate channels through which members of the public can express their concerns to NIH or through which they can receive information about the broad scope of effort being made in the fields with which they are concerned.
This structural weakness has important implications: first, because patient advocacy groups have become better organized and more proactive on behalf of their interests and have greatly increased their appeals to Congress to intervene to adjust NIH research priorities; second, because congressional leaders have expressed a strong desire to avoid mandates and earmarks in favor of particular diseases and to let NIH set research priorities; and third, because the NIH director has increased his role in priority setting (partly by exercising additional authorities granted to him by Congress). This confluence of events highlights the need for improved communication between the public and NIH.
NIH should engage the public to a greater extent in informing the process by which NIH sets its research priorities. The following three recommendations are intended to provide the public with more opportunities to present their views regarding research needs and to receive information about research and the priority-setting process at NIH.
Recommendation 7. NIH should establish an Office of Public Liaison in the Office of the Director and, where offices performing such a function are not already in place, in each institute. These offices should document, in a standard format, their public outreach, input, and response mechanisms. The director's Office of Public Liaison should review and evaluate these mechanisms and identify best practices.
The Offices of Public Liaison are meant to serve several purposes: (1) they provide an easily identifiable point of contact for individuals and groups who have an interest or concern; (2) they are a place where members of Congress can refer constituents who want to obtain information or to raise concerns; and (3) they conduct an active program of outreach to and interaction with constituency groups. The NIH director's Office of Public Liaison will oversee and coordinate the institutes' Offices of Public Liaison, serve as a point of contact for individuals or groups who are dealing with crosscutting issues or who do not have a specific institute to contact, and staff the Director's Council of Public Representatives (discussed below).
Recommendation 8. The director of NIH should establish and appropriately staff a Director's Council of Public Representatives, chaired by the NIH director, to facilitate interactions between NIH and the general public.
The Director's Council of Public Representatives—an advisory group made up of citizens who are either patients, family members of patients, or advocates for patients—serves to elevate public input into the priority-setting process to the highest level of NIH in a systematic and periodic manner. Importantly, the Council will not set priorities regarding the NIH budget or its research programs. That is, it is not intended to serve as a forum for advocacy groups to lobby the NIH director for research dollars. Rather, it is intended to serve as a mechanism for NIH to receive valuable and thoughtful perspectives on its research programs from those who are in some way affected by disease and disability and who are therefore advocates for a healthy NIH and for NIH to provide information about its research and priority-setting process as part of a two-way exchange of information.
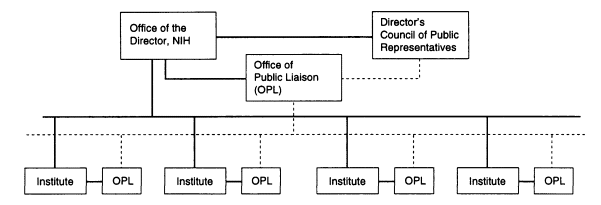
Together with the Offices of Public Liaison, the Director's Council of Public Representatives would permit continual interaction between NIH and the public. The Council would allow the NIH director to hear periodically from representatives of a spectrum of interest groups; the Offices of Public Liaison, which would be staff offices that function on a daily basis, unlike the Council, would provide information to and receive input from interested groups and congressional offices and would staff the Council in the Office of the Director. Figure 1 shows the proposed placement of the Offices of Public Liaison and the Director's Council of Public Representatives within the current organization at NIH.
Recommendation 9. The public membership of NIH policy and program advisory groups should be selected to represent a broad range of public constituencies.
NIH has long-standing mechanisms by which to include public or lay members on top-level advisory bodies. In the institutes, these councils provide advice and guidance on their research programs and funding decisions by providing the second layer of review (the first being peer review through the study sections). Thus, public representatives play a role in the priority-setting process and provide advice on funding decisions. NIH also reserves slots for public members on the Advisory Committee to the Director. It does not appear, however, that advocates for patients or special populations are regularly considered for these advisory committee memberships, despite numerous examples of cases in which such arrangements have been constructive and positive. Not using this mechanism to receive public input is a missed opportunity and has resulted in the perception of some groups that NIH does not encourage public input at the highest levels of its advisory processes.
These recommendations are not intended to replace the existing criteria for priority setting. They are intended to enhance and reinforce existing NIH mechanisms through which the voices of the public can be heard in a constructive and open manner. The committee believes that public input, which has been important in sustaining the growth and stature of NIH, is an important component of the priority-setting process and, if used wisely by NIH when setting research priorities, will make for a stronger and more responsive NIH. It also believes that although implementation of these recommendations will not supersede or remove the potential for appeals to Congress, their enactment will reduce the need for such appeals.
The new organizational mechanisms proposed to improve public input have the potential to increase, in the short term, organizational costs and complexity. In the long run, however, the committee believes that the contribution made by these offices and the Council will prove to be cost-effective in terms of carrying out NIH's mission to improve health through research and will contribute to overall goodwill on the part of the public and Congress toward NIH.
CONGRESSIONAL ROLE
Congress has always taken a special interest in NIH and has usually provided for larger budgets than administrations request. Congress has also often directed NIH in fairly specific ways, requiring the establishment of research programs, setting aside specific amounts of funding for research on designated problems, mandating the creation of research centers, institutes, or other specific mechanisms, and so forth.
Congress has the authority and the responsibility to intervene if it thinks that NIH is neglecting an opportunity or is not responsive to a need. Members of Congress recognize that it would be better for NIH to make the detailed decisions on how to approach problems.
The committee believes that if NIH revises its priority-setting system in the ways recommended above, Congress will be more likely to grant NIH (which, it is hoped, will be informed by stronger public input) the primary role in setting its research priorities. The text of the report includes some guidelines first offered by an Institute of Medicine committee in 1984 for Congress to use in deciding whether to mandate major organizational changes.
Recommendation 10. The U.S. Congress should use its authority to mandate specific research programs, establish levels of funding for them, and implement new organizational entities only when other approaches have proven inadequate. NIH should provide Congress with analyses of how NIH is responding to requests for such major changes and whether these requests can be addressed within existing mechanisms.
If NIH is to have more autonomy in organizing and managing its research programs, it is incumbent on the agency to engage in periodic reviews of its organizational structure and planning and budgeting systems and to explain the results to Congress and the public.
Recommendation 11. The director of NIH should periodically review and report on the organizational structure of NIH, in light of changes in science and the health needs of the public.
The committee questions whether NIH, especially the Office of the Director, has adequate resources to operate an effective priority-setting system. Providing the Office of the Director of NIH with adequate resources for analysis and interface with the public would make research priority setting more effective.
Recommendation 12. Congress should adjust the levels of funding for research management and support so that NIH can implement improvements in the priority-setting process, including stronger analytical, planning, and public interface capacities.
|
BOX 2 The Committee's Recommendations Criteria for Priority Setting Recommendation 1. The committee generally supports the criteria that NIH uses for priority setting and recommends that NIH continue to use these criteria in a balanced way to cover the full spectrum of research related to human health. Recommendation 2. NIH should make clear its mechanisms for implementing its criteria for setting priorities and should evaluate their use and effectiveness. Recommendation 3. In setting priorities, NIH should strengthen its analysis and use of health data, such as burdens and costs of diseases, and of data on the impact of research on the health of the public. Recommendation 4. NIH should improve the quality and analysis of its data on funding by disease and should include both direct and related expenditures. Priority-Setting Processes Recommendation 5. In exercising the overall authority to oversee and coordinate the priority-setting process, the NIH director should receive from the directors of all of the institutes and centers multiyear strategic plans, including budget scenarios, in a standard format on an annual basis. |
|
Recommendation 6. The director of NIH should increase the involvement of the Advisory Committee to the Director in the priority-setting process. The diversity of the committee's membership should be increased. particularly with respect to its public members. Mechanisms for Public Input NIH should engage the public to a greater extent in informing the process by which NIH sets its research priorities, as illustrated by the following: Recommendation 7. NIH should establish an Office of Public Liaison in the Office of the Director and. where offices performing such a function are not already in place, in each institute. These offices should document. in a standard format. their public outreach, input, and response mechanisms. The director's Office of Public Liaison should review and evaluate these mechanisms and identify best practices. Recommendation 8. The director of NIH should establish and appropriately staff a Director's Council of Public Representatives. chaired by the NIH director, to facilitate interactions between NIH and the general public. Recommendation 9. The public membership of NIH policy and program advisory groups should be selected to represent a broad range of public constituencies. Congressional Action Recommendation 10. The U.S. Congress should use its authority to mandate specific research programs, establish levels of funding for them, and implement new organizational entities only when other approaches have proven inadequate. NIH should provide Congress with analyses of how NIH is responding to requests for such major changes and whether these requests can be addressed within existing mechanisms. Recommendation 11. The director of NIH should periodically review and report on the organizational structure of NIH. in light of changes in science and the health needs of the public. Recommendation 12. Congress should adjust the levels of funding for research management and support so that NIH can implement improvements in the priority-setting process, including stronger analytical. planning, and public interface capacities. |