Overview of the State Children's Health Insurance Program
Children's health insurance became a subject of national debate early in 1997 when President Clinton and members of Congress began to develop a variety of competing proposals to expand coverage for children. After several months of active discussion and negotiation, Congress enacted the State Children's Health Insurance Program (SCHIP) as part of the Balanced Budget Act of 1997 (P.L. 105-33).
SCHIP was designed to allow states to provide “child health assistance to uninsured, low-income children in an effective and efficient manner that is coordinated with other sources of health benefits coverage for children.” For the purposes of SCHIP, low-income children are generally defined as those whose family incomes are higher than Medicaid eligibility but lower than 200% of poverty (about $32,000 for a family of four).
After October 1, 1997, SCHIP made $24 billion available to states over 5 years, including $20.3 billion for new initiatives based on private insurance coverage and $3.6 billion for Medicaid improvements, such as continuing eligibility for children who were formerly eligible for Supplemental Security Income, and guaranteeing 1 year of Medicaid eligibility. Some analysts suggest that SCHIP funding may be adequate to cover almost 6 million children, but that only about 3 million children will be eligible for SCHIP under current program rules (Ullman et al., 1998).
According to the latest estimates from the Census Bureau, 11 million children are uninsured—1 out of every 7—and most of these children live in low-income working families (Employee Benefits Research Institute, 1997). States may use SCHIP funds to broaden their Medicaid programs, to start up or expand state-sponsored or private insurance programs, or to support a combination of programs. Under SCHIP, states must screen all applicants for Medicaid eligibility and must enroll any eligible children in the Medicaid program. Depending on the source of these data, an estimated 1.6 million to 4.7 million children who are already eligible for Medicaid are not enrolled (Selden et al., 1998; Ullman et al., 1998; Weigers et al., 1998) Thus, coordination between SCHIP and Medicaid programs will be critically important.
The potential for flexibility in SCHIP designs appeals to most states because it gives them the opportunity to provide coverage and services in ways that reflect the state's unique circumstances and characteristics, such as the availability of insurance products
and providers, geographic distribution of uninsured children, and the potential sources of financing, among others.
This flexibility also raises some technical and practical issues. The most fundamental question is this: With so much variation possible, how will we know whether SCHIP is effective?
PURPOSE OF THIS REPORT
This report describes the responsibilities of Congress, the U.S. Department of Health and Human Services (DHHS), and the states in implementing and evaluating SCHIP. The report presents a framework and recommendations for designing systems of accountability for the program as states take a variety of steps to reduce the number of uninsured children. The committee defines systems of accountability as those processes and procedures that provide information for analysis and decision-making and that provide a basis for designing, implementing, evaluating, and improving programs.
The committee strongly supports the flexibility and innovation that are built into the SCHIP legislation, provided there are ways to measure the program's impact on a national basis and to ensure that the funds spent actually improve insurance coverage and health outcomes for children. From the beginning, it will be important to learn where states are heading with their spending and services. Later on, it will be important to be able to identify which program components are effective so that “best practices” can be continued and replicated in other locations and less effective practices can be avoided. Thus, the committee's accountability framework includes steps that can be taken immediately, as well as steps that are needed to build infrastructure, capacities, and systems for a coordinated, longer-term approach.
WHO IS ACCOUNTABLE FOR SCHIP?
What Is Accountability?
In general terms, accountability is the process by which an individual or organization accepts responsibility for an activity and provides information regarding its progress in meeting requirements and expectations. Accountability involves the development and dissemination of information regarding the process, quality, and outcomes of work; the use of fiscal resources; the problems encountered or anticipated; and other activities undertaken to fulfill contractual, fiscal, statutory, professional, or public responsibilities. For a children's health insurance program, accountability refers to responsible spending to expand children's access to affordable, high-quality health care.
Systems of accountability should specify the mechanisms and formats for collecting and transmitting the expected information. These formats may be oral, written, electronic, or in some other standardized technology. The systems also should specify the ways in which feedback on the information will be exchanged, and what kinds of responses might be expected as a result.
Accountability is an interactive process. In other words, accountability should be defined specifically in the context of relationships. Figure 1 portrays the specific relationships through which the committee believes accountability for SCHIP must be established.
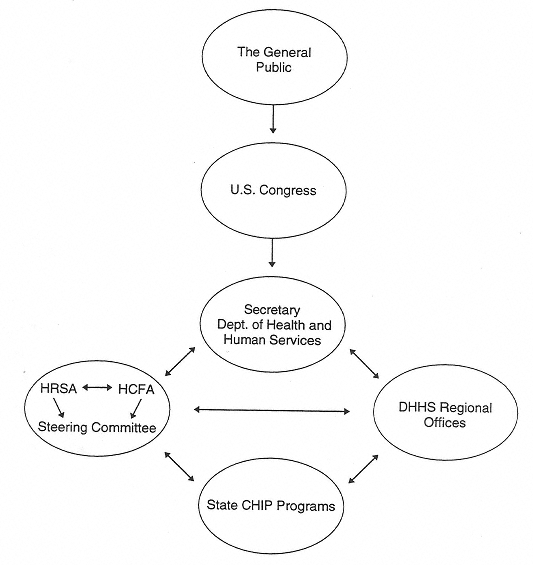
FIGURE 1 Accountability for SCHIP programs. One-way arrows indicate public accountability specified in The Balanced Budget Act of 1997 (P.L. 105-33). Two-way arrows indicate collaborative exchanges of information to ensure accountability for the SCHIP programs.
Congress
Having enacted SCHIP and appropriated $24 billion over 5 years, Congress will oversee DHHS's administration of the program. The legislation requires states to submit written plans to DHHS describing their programs as well as their strategic objectives, performance goals, and performance measures (see Box 1). The legislation also requires the secretary of DHHS to report to Congress on the effectiveness of the state plans by December 31, 2001.
|
BOX 1 Strategic Objectives and Performance Goals Described in the Balanced Budget Act of 1997 States must do the following:
By December 31, 2001, the secretary shall submit a report to the Congress and will make it available to the public. The report will be based on information submitted by the states. The Balanced Budget Act does not further specify the information to be collected, analyzed, or evaluated by the secretary. SOURCE: Based on The Balanced Budget Act of 1997 (P.L. 105-33, Subtitle J, Summary of Provisions, at http://www.house.gov/budget/papers/mainsumm.htm. |
With these legislative requirements, Congress established a basic template for SCHIP accountability. However, the authorizing legislation leaves a great deal of room for interpretation by DHHS and by the states. At this very early stage in the program, it is vitally important to design and develop systems of accountability and to anticipate information and communication needs based on experiences with other programs.
If Congress chooses to gather additional information on SCHIP, it has several of its usual oversight options. For example, it may hold hearings or it may request a study by the U.S. General Accounting Office. After SCHIP has been fully implemented, if it is not developing in the way Congress intended, Congress could amend the statute to change the program or to include additional requirements.
U.S. Department of Health and Human Services
Within DHHS, the Health Care Financing Administration (HCFA) and the Health Resources and Services Administration (HRSA) are leading an interdepartmental steering committee to implement SCHIP. State plans are being submitted to HCFA and are being reviewed by HCFA's national and regional offices in collaboration with HRSA, the Agency for Health Care Policy and Research, the office of the Assistant Secretary for Planning and Evaluation, and other participants on the steering committee.
For several months, DHHS has been actively providing information and technical assistance to states as they develop and implement their SCHIP plans. Activities have included
-
a series of regional conferences in January and February 1998 for state and federal officials, state legislators, providers, and community leaders;
-
written guidance in the form of “dear state” letters on the state plan approval process, financial reporting, outreach and enrollment, cost-sharing, substitution of coverage, public involvement, and other issues;
-
a web site (www.hcfa.gov) containing the “dear state” letters, press releases, names and contact information for agency assistance, and other information; and
-
collaboration with the American Public Human Services Association, the National Governors' Association, the National Conference of State Legislatures, the Association of State and Territorial Health Officials, the National Association of Insurance Commissioners, and other groups.
By late September 1998, 50 plans have been submitted and 41 plans have been approved. Of the 50 plans, 13 are for programs created by states, 27 are for Medicaid expansions, and 10 are combinations of Medicaid and state programs. DHHS has created a standard format to help states provide information that is required by the statute, but the current focus is on start up and enrollment activities. Further decisions and guidance on data and on federal and state accountability systems are still pending.
Several child health performance measurement and managed care quality improvement activities have implications for SCHIP, including Bright Futures encounter forms and the National Committee on Quality Assurance's expansion of HEDIS child health measures. In addition, HCFA's Quality Improvement System for Managed Care standards and guidelines are in interim final form as of late September 1998. The challenge for DHHS will be to continue to collaborate with the variety of efforts underway in states and the private sector while also moving forward on defining standardized reporting information for SCHIP.
States
To qualify for their first-year SCHIP allotments, states must submit written plans to HCFA before September 30, 1999. (The original deadline of June 30, 1998, was extended on May 1, 1998, by H.R. 3579). After HCFA approves the plans, they become the states' contracts and serve as the basis for each state's accountability framework for SCHIP.
As of March 17, 1998, 22 states had submitted plans to HCFA for approval, and four plans had been approved—those for Alabama, Colorado, Florida, and South Carolina. HCFA has also encouraged states to submit “mini-plans” that would secure their allotment for up to 3 years, but would also allow them to submit revised plans later on (National Economic Council/Domestic Policy Council, 1998).
In addition to information on eligibility, enrollment, and program coordination, state plans must include information on the scope of services and on methods to ensure the quality and appropriateness of care (see Box 2 and Figure 2).
States vary widely in technical and analytical capacities as well as in their willingness to collect and analyze performance data (Landon et al., 1998; Rosenbaum et al., 1997). Technical problems in the exchange of health care information arise from the variety of software systems used by states, health plans, and other providers, as well as from the cost of new management information systems—which can range from $250,000 to $1 million for a basic administrative system and much higher for a full managed care system (Ciotti and Zodda, 1996).
For example, even though HCFA requires states to collect encounter-level data for Medicaid managed care 1115 waiver demonstrations, some states' information systems will not allow them to merge and analyze eligibility and claims files, which could enable them to analyze access and patterns of care (Epstein, 1997). As large-scale purchasers of private health care coverage for SCHIP enrollees, states must be able to develop specific contract language, define a scope of services within existing resources, and establish performance measures that ensure access and quality of care.
|
BOX 2 Information to Be Included in State SCHIP Plans States must submit a written SCHIP plan to DHHS for approval in order to receive the federal match. The plan must include the following information:
SOURCES: Based on The Balanced Budget Act of 1997 (P.L. 105-33, Subtitle J, Summary of Provisions, at http://www.house.gov/budget/papers/mainsumm.htm and Title XXI Summary from The Balanced Budget Act of 1997, Children's Health Insurance Program by the Health Care Financing Administration at http://www.hcfa.gov/init/kidssum.htm. |
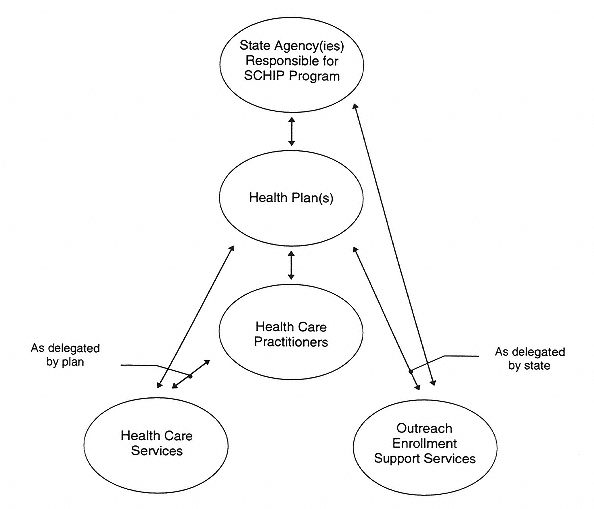
FIGURE 2 Information flows to support accountability relationships within states for SCHIP programs. Arrows indicate information flows and accountability relationship, as specified in state laws, public policies, and contractual agreements.
RECOMMENDATIONS
The recommendations in this report are based on an extensive review of evidence on the relationship between insurance coverage and access to care, as presented in the committee's companion report, America's Children: Health Insurance and Access to Care (IOM, 1998). The recommendations are also based on the following assumptions:
-
New Opportunities. SCHIP offers new opportunities for innovation and flexibility in insurance expansion, for improving existing programs, for increasing children's access to health care, and for developing child-specific performance measures.
-
Accountability for Public Funding. The $24 billion in federal funds allocated for SCHIP and Medicaid improvements represents a significant national commitment to insurance expansion for children. This commitment should be monitored to ensure that the legislation's goals are fulfilled.
-
Need for Sustained Efforts. Although SCHIP will help to reduce the number of uninsured children, millions of children will remain uninsured or underinsured even assuming its full implementation. To guide future insurance expansions, careful evaluation of the multitude of state approaches used under SCHIP will be essential.
CONGRESSIONAL ACCOUNTABILITY FOR SCHIP
1. Congress should take immediate action to ensure that funding is adequate to evaluate SCHIP's impact.
Congress provided a basic template for SCHIP accountability systems by requiring states to set strategic objectives and performance goals and to collect performance data as part of their SCHIP plans, and by requiring the Secretary of DHHS to report to Congress by December 2001 on the effectiveness of the state plans (see Box 1). The commitment to using performance data is a critical component of any long-term accountability system (Congressional Budget Office, 1993).
The committee is concerned that existing federal and state information systems, data sources, and analytical capacities may not be adequate to accomplish the ongoing evaluation and monitoring of child health insurance coverage, access, utilization, and outcomes that are required by the SCHIP legislation. For example, recent experience with welfare reform shows that new programs need adequate resources to be able to make initial procedural and programmatic adjustments (GAO, 1998a,b).
To protect the national investment in SCHIP, the committee urges Congress to take the necessary steps to ensure that the resources and strategies needed to evaluate the impact of SCHIP are adequate at the state and federal levels.
-
The leadership of key committees should periodically ensure that DHHS has adequate resources to implement its responsibilities under SCHIP.
-
Key committees should designate staff members who would keep in contact on an informal basis with DHHS staff to ensure that SCHIP accountability systems have adequate resources and support.
FEDERAL GOVERNMENT ACCOUNTABILITY FOR SCHIP
Performance Monitoring for SCHIP
2. DHHS must establish a performance monitoring system for SCHIP in collaboration with agencies from other levels of government and with private organizations.
DHHS should involve states, local governments, health plans, national organizations, and private foundations active in health care in a national effort to evaluate the impact of SCHIP. This effort should be coordinated with ongoing performance monitoring activities concerned with public health, mental health and substance abuse treatment and preven-
tion, education, disabilities, and other programs and activities involving children and families, especially low-income working families.
The collaboration should involve the design and support of measurement methods and strategies and the development of technical and analytical capacities in the states, including financial and technical support for designing and implementing new information systems. State governments and state and local private foundations should assist the national effort by supporting statewide and local evaluations and by helping to develop systems to disseminate information and stimulate action in the states and in local communities.
a. DHHS should designate an interdepartmental task force to coordinate, implement, and oversee a performance monitoring system for SCHIP.
The task force should develop a strategic plan that sets clear, realistic priorities for SCHIP in the short term (1998–2000) and for the mid-phase (2001–2003). The plan should identify what can be learned from different SCHIP approaches over the long-term, including the net increase in the number of insured children under different SCHIP program approaches; effective strategies for coordination of SCHIP with Medicaid and other state and community-based programs; and likely effects on SCHIP children's health status. This strategic plan should be made available to the public.
The task force could include the key staff who were involved with the DHHS Steering Committee for SCHIP during its design phase. The task force should continue to develop relationships with stakeholder groups in state and local governments, as well as with foundations.
b. A well-chosen set of basic performance measures is needed to provide comparable information for all SCHIP programs.
Currently, states vary widely in their use of information systems, analytical and technical capacities, and measurement approaches. Without a minimum set of comparable data, it will be difficult to establish baseline information and to track changes in the number of uninsured children; to evaluate disparities in health status; to compare the scope of services in different programs, utilization data for different groups, and the quality of care in different health plans; and to collect other information essential for evaluating the success of SCHIP across states.
The field of performance measurement is continually improving and is moving toward more outcome-oriented, population-specific, and evidence-based measures. In addition to the technical difficulty and expense of developing and implementing new accountability systems, a major challenge and tension in this evolving field is how to strike a balance between the desire for comparable information and the resistance to public comparisons and judgments. For example, states are accustomed to financial reporting for federal programs but may be less willing to collect programmatic data that can be used for monitoring or for purposes of cross-state comparisons.
The set of SCHIP performance measures should anticipate and incorporate future developments in the science and technology of performance measurement. Unless the existing resources are increased, the set of measures should be relatively small, should not be too burdensome or expensive to implement, and should be based on existing systems wherever possible. In addition to this minimum data set, states also should be encouraged to collect more extensive information as described in their state plans.
c. The interdepartmental task force should coordinate its activities with representatives of the technical and analytical infrastructure being developed at state and federal levels to evaluate welfare reform and other recent health insurance legislation.
When DHHS became responsible for SCHIP, it was already in the process of implementing two other major pieces of recent legislation: the Personal Responsibility and Work Opportunity Reconciliation Act of 1996 (welfare reform), and the administrative simplification provisions of the Health Insurance Portability and Accountability Act (HIPAA). Due to technical difficulties, competing agency demands within the existing staffing levels, and the need for public involvement and commentary, DHHS missed its statutory deadline for implementing a high-performance bonus program under welfare reform (GAO, 1998a) and is behind schedule in issuing its national data standards for HIPAA.
These challenges in implementing the requirements of welfare reform and HIPAA may be important lessons for SCHIP. The last decade of experience on the implementation and oversight of Medicaid managed care, including the issues associated with state contracting with managed care plans under Medicaid, also may be instructive for SCHIP. The committee encourages DHHS to continue to strengthen its interdepartmental communications, to make the most efficient use of existing resources, and to learn from recent experience in other areas.
d. A new, rapid turnaround survey is needed to track key indicators of SCHIP performance at the state level.
An initial survey should be implemented quickly to provide a baseline for measuring changes in children's insurance coverage, enrollment, and utilization. A more comprehensive survey should be repeated on an ongoing basis to monitor changes in children's health status and well-being after states implement their SCHIP programs.
Children's Health Indicators
3. DHHS must develop systems that improve the availability of national and state-level information on children's insurance coverage, access, utilization, satisfaction, health status, and outcomes, particularly for children with special health care needs.
The major national health surveys, including the National Health Interview Survey (NHIS) and the Medical Expenditure Panel Survey, can provide national and regional data on insurance coverage, utilization, and health status. However, these surveys do not provide state-level data for most states, and the data they do provide are not always current. For example, the last child health supplement to the NHIS was conducted in 1988. Additional resources may be necessary to develop and improve these data collection systems.
-
DHHS should increase the sample size of the NHIS to permit state-level estimates and evaluations. Supplements on child health and well-being should be conducted every 3 years.
-
DHHS should continue to support and encourage efforts to develop and improve indicators of children's health status and outcomes, including indicators for children with special health care needs.
DHHS has undertaken several exemplary activities in quality measurement. These include department-wide collaborative efforts with the National Committee for Quality Assurance; HCFA's testing of outcome measures developed by the Foundation for Accountability and development of the Quality Improvement System for Managed Care; and the Agency for Health Care Policy and Research's support of the Consumer Assessment of Health Plans Survey.
However, most measures being tested are not child-specific, and current children's health and functional status indicators are inadequate, especially for children with special health care needs. For the most part, existing measures lack the sensitivity and specificity needed to track changes in children's health status and treatment outcomes over time. The committee urges the sponsoring and participating organizations to increase their commitment to developing child-specific and age-appropriate measures.
STATE ACCOUNTABILITY FOR SCHIP
Designing Accountability Systems
4. States should begin immediately to design and implement systems to produce meaningful information on SCHIP's effects.
Information should be collected to provide evaluative data on the impact of SCHIP on children's insurance coverage, access, utilization, satisfaction, health status, and outcomes, particularly for children with special health care needs.
To the maximum extent possible, information systems to track SCHIP should be developed at the same time the programs are being designed and implemented. Without coordinated guidance and planning for state-level accountability systems, opportunities may inadvertently be missed. For example, a state with streamlined enrollment forms may choose not to ask about prior insurance status, race/ethnicity, or other information that could be extremely useful to the state later on in determining overall program impact as well as SCHIP penetration with particular subgroups.
Regardless of which state agency takes the lead during the planning process, each state will need to identify the responsible parties and strategies for SCHIP implementation and for technical assistance in developing statewide accountability systems. At a minimum, states will need to specify the agencies and individuals responsible for providing public information about SCHIP; for developing tools and incentives for provider and health plan participation; for evaluating program impact; and for making timely adjustments and modifications to the enrollment process, information and tracking systems, and other administrative components of the program.
Public Information
5. Information on SCHIP should be made available by states to the public and should be meaningful in evaluating the program's performance.
The committee recognizes the technical and procedural difficulties inherent in developing systems that can produce useful, comparable information and that can track developments and changes in performance over time. However, the demand for better information on the delivery and outcomes of health care is increasing among policymakers, providers, and consumers (IOM, 1997; Roper and Cutler, 1998). Many states are already beginning to benchmark the performance of a variety of public programs (National Academy of Public Administration, 1998; Southern Growth Policies Board, 1995), and are disseminating “best practices” models so they can learn from each other's experiences (National Governor's Association, 1998). However, few existing programs that serve children are being systematically evaluated.
SCHIP can stimulate the development of new sources of useful information on the quality and types of care provided to children. Because SCHIP is a public program, information about the program should be made available to the public to hold policymakers accountable and to ensure that the funds are spent appropriately. Information also should be made available to practitioners for quality improvement purposes and to researchers for analysis. A coordinated effort should be made to collect and analyze these SCHIP data nationally to provide an ongoing, comprehensive tracking of efforts to insure children and improve their health.
Data Collection and Performance Reporting
6. As much as possible, states should delegate the collection and synthesis of SCHIP information to contracted health plans or provider groups, with requirements for independent auditing of these data.
States often lack the financial resources, trained administrative and technical staff, and information systems required to monitor the quality of care purchased from managed care organizations (GAO, 1997; Howell, 1996; IOM, 1988; Landon et al., 1998; Zuckerman et al., 1997). In contrast, many managed care organizations are experienced in reporting information on performance to employers, other large-scale purchasers, and accreditation organizations.
Contracts are the basis for defining the business and accountability relationship between purchasers and providers. States vary in the degree to which they specify performance standards in contracts and establish and apply sanctions in contracts for Medicaid managed care providers (Rosenbaum et al., 1997). Recent experience with Medicaid managed care suggests that state-level expertise and technical capacity are necessary components in monitoring the quality and effectiveness of managed care. Similar challenges may arise with SCHIP, particularly in states with less managed care experience.
Therefore, the committee believes that state contracts with health plans or provider groups should clearly specify their responsibilities for analyzing, synthesizing, and reporting SCHIP data to states. Contracts should also specify the measures, format, timeline, and incentives or penalties associated with reporting, as well as requirements for independent audits. Once states have received data and information, they should exercise their
oversight responsibilities through technical and analytical procedures to ensure the quality and completeness of the information. Ultimately, states are accountable and responsible for fulfilling their public obligations through analyzing and evaluating the data produced by the participants in publicly supported programs.
Performance Incentives and Rewards
7. States should set conditions of participation in SCHIP, experiment with a variety of incentives to reward health plans for their performance, and develop the technical and analytical capacity to evaluate the impact of incentives on health plan performance.
Performance reporting using standardized measures is critical—necessary although not sufficient alone—to the implementation of systems of accountability. Many private purchasers and purchaser coalitions have seen costs, satisfaction and utilization patterns, or both improve as a result of using performance reporting and related tools and incentives (Hanchak et al., 1996). In contrast, few state agencies now require standardized reporting or link performance to conditions of participation or compensation, and performance-based incentives can be difficult to implement (GAO, 1998a; IOM, 1997).
Performance reporting must be accompanied by one or more of the following reinforcements: (a) dissemination of information on performance to providers, consumers, state agencies, or others who are in a position to influence the reporting entity; (b) the application of conditions of participation (i.e., thresholds of contracting); or (c) the provision of variable compensation (i.e., linking reimbursement to performance). For example, states may choose to provide additional compensation for every child who receives age-appropriate immunizations on a recommended schedule.
States may benefit from developing collaborative relationships with purchaser coalitions to identify and test incentives tied to health plan performance. These partnerships and incentives may help to address inherent problems in SCHIP, such as limitations on the amount that can be spent on information systems and other administrative expenses.
CONCLUSION
SCHIP is historic, innovative, and rapidly evolving. It offers an unprecedented opportunity to move from the traditional monitoring and compliance models of health care, which focus on financial performance, to a quality improvement model that fulfills the intent of the SCHIP legislation: to provide insurance coverage for uninsured children, to improve their access to high-quality health care services, and, ultimately, to improve their health.
REFERENCES
Congressional Budget Office (CBO). 1993. Using Performance Measures in the Federal Budget Process. Washington, DC: CBO.
Ciotti V, Zodda F. 1996. Selecting Managed Care Information Systems. Healthcare Financial Management June, 35–40.
Employee Benefits Research Institute (EBRI). 1997. Special tabulations from the Bureau of the Census, Current Population Survey, prepared for the Institute of Medicine Committee on Children, Health Insurance, and Access to Care. Washington, DC: EBRI.
Epstein AM. 1997. Medicaid Managed Care and High-Quality: Can We Have Both? Journal of the American Medical Association 278(19):1617–1621.
GAO (U.S. General Accounting Office). 1997. Medicaid Managed Care Accountability (Pub. No. GAO/HEHS-97-86). Washington, DC: GAO.
GAO. 1998a. Medicaid: Early Implications of Welfare Reform for Beneficiaries and States (Pub. No. GAO/HEHS-98-62). Washington, DC: GAO.
GAO. 1998b. Welfare Reform: HHS's Progress in Implementing Its Responsibilities (Pub. No. GAO/HEHS-98-44). Washington, DC: GAO.
Hanchak NA, Schlackman N, Harmon-Weiss S. 1996. U.S. Healthcare's Quality-Based Compensation Model. Health Care Financing Review 17(3):143–159.
Howell EM. 1996. Medicaid Managed Care Encounter Data: What, Why, and Where Next? Health Care Financing Review 17(4):87–95.
Institute of Medicine (IOM). 1988. The Future of Public Health. Washington, DC: National Academy Press.
IOM. 1997. Managing Managed Care: Quality Improvement in Behavioral Health. Washington, DC: National Academy Press.
IOM. 1998. America's Children: Health Insurance and Access to Care. Washington, DC: National Academy Press.
Landon BE, Tobias C, Epstein AE. 1998. Quality Management by State Medicaid Agencies Converting to Managed Care: Plans and Current Practice. Journal of the American Medical Association 279(3):211–216.
Lefton R. 1997. Aligning Incentives Using Risk-Sharing Arrangements. Healthcare Financial Management. February, 50–57.
National Academy of Public Administration. 1998. Alliance for Redesigning Government [WWW document]. URL http://www.alliance.napawash.org (accessed April 13, 1998).
National Economic Council/Domestic Policy Council. Implementation of the Children's Health Insurance Program [WWW Document]. Washington, DC: The White House. URL http://www.hcfa.gov/init/wh-chip5.htm (accessed May 22 1998).
National Governors Association. 1998. Promising Practices to Improve Results for Young Children [WWW document]. URL http://www.nga.org/PromisingPractices/default.htm (accessed April 28, 1998).
Roper WL, Cutler CM. 1998. Health Plan Accountability and Reporting: Issues and Challenges. Health Affairs 17(2):152–155.
Rosenbaum S, Shin P, Smith BM, Wehr E, Borzi PC, et al. KA Johnson, Ed. 1997. Negotiating the New Health System: A Nationwide Study of Medicaid Managed Care Contracts. Washington, DC: The George Washington University Center for Health Policy Research.
Selden TM, Banthin JS, Cohen JW. 1998. Medicaid's Problem Children: Eligible but Not Enrolled. Health Affairs 17(3):192–200.
Southern Growth Policies Board. 1995. Measure by Measure: Benchmarking and Performance Measurement in the South [WWW document]. URL http://alliance.napawash.org (accessed March 9, 1998).
Ullman F, Bruen B, Holahan J. 1998. The State Children's Health Insurance Program: A Look at the Numbers. Occasional Paper Number 4. Washington, DC: Urban Institute.
Weigers ME, Weinick RM, Cohen JW. 1998. Children's Health, 1996. MEPS Chartbook No. 1. (AHCPR Pub. No. 98-0008). Rockville, MD: Agency for Health Care Policy and Research.
Zuckerman S, Evans A, Holahan J. 1997. Questions for States as They Turn to Medicaid Managed Care [WWW document]. URL http://newfederalism.urban.org/html/anf_all.htm (accessed April 24, 1998).














