8
Live Smart Texas Panel Presentation
Deanna Hoelscher, Director of the Michael & Susan Dell Center for Advancement of Healthy Living and Co-chair of the Live Smart Texas Coalition, described the structure and functions of the Live Smart Texas Coalition. Live Smart Texas was initiated in an effort to bring funding from The Robert Wood Johnson Foundation to the state of Texas. Today, Live Smart Texas is a coalition of more than 80 statewide partners, including state agencies, policy institutes, community organizations, and advocacy groups, with a shared policy agenda of preventing obesity throughout the life cycle. At its inception, the partners defined a collaborative research agenda centered on obesity prevention efforts and the development of resources to build infrastructure and capacity within all communities.
The full Live Smart Texas Coalition is overseen by a 15-member steering committee, with six ancillary working committees covering obesity leadership, policy and environmental change, programs and interventions, prevention research, instruments and protocols, and data (Figure 8-1). Each of the partners serves a unique function for the group, including providing resources, advocacy, and research. In addition to the working committees, the collaborative has a communications committee and a special projects arm. Box 8-1 lists the current projects of Live Smart Texas.
Hoelscher explained that advocacy within Live Smart Texas is carried out by Partnership for a Healthy Texas. This partnership was formed in 2006 when more than 20 organizations banded together with the common goal of working with the Texas legislature to develop and promote policies that would prevent obesity in the state. The partnership has grown to include roughly 60 organizations and advisors with a common voice. The
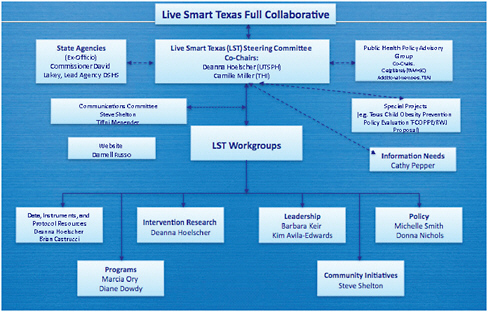
FIGURE 8-1 Live Smart Texas organizational chart, as presented by Hoelscher
|
BOX 8-1 Current Projects of the Live Smart Texas Coalition Texas Childhood Obesity Prevention Policy Evaluation (T-COPPE)
Obesity Surveys
Live Smart Texas Website
|
guiding principles of Partnership for a Healthy Texas are similar to those of Live Smart Texas:
-
Encourage collaboration among all interested parties in reducing obesity.
-
Inform policy makers about the consequences of obesity.
-
Promote evidence-based strategies at multiple levels: individual, family, community, and policy.
-
Serve as a resource for people interested in addressing obesity prevention and treatment.
In 2007, the Partnership succeeded in getting the legislature to pass five of six priority initiatives. The Partnership has identified six priorities for the 2009 legislative session:
-
Support implementation of coordinated school health.
-
Improve nutrition education and access to healthy foods.
-
Strengthen physical education in schools and communities to reflect best practice.
-
Promote worksite wellness programs.
-
Support comprehensive evidence-based programs at the community level that will have an impact on obesity.
-
Monitor the Texas Department of Agriculture’s Sunset Review Process to strengthen implementation of nutrition policy.
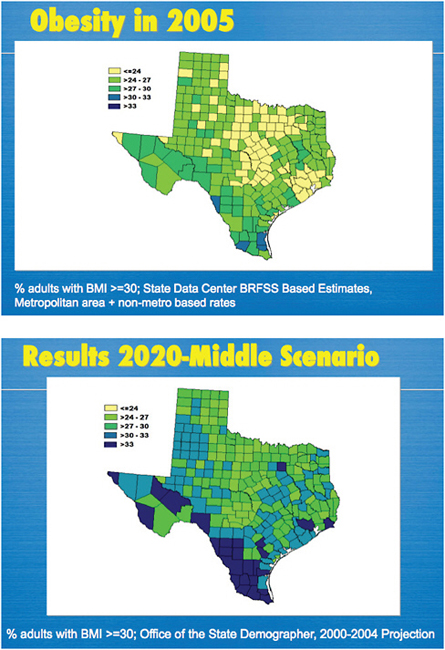
The research component of Live Smart Texas is currently fulfilled by the Texas Childhood Obesity Prevention Policy Evaluation (T-COPPE) and the Texas obesity projections made by State Epidemiologist Vincent Fonseca, data that were released in January 2009 by the Office of the State Demographer, the Office of the State Epidemiologist, Methodist Healthcare Ministries, and the Texas Health Institute. These projections were developed through a collaborative effort between the state epidemiologist and the Office of the State Demographer, using a conservative methodology to predict increasing obesity rates in the state. These predictions used actual data from the Behavioral Risk Factor Surveillance System for 2005–2007 as a baseline, taking into account demographic changes, recent patterns of observed weight change due to aging, and recent patterns of increasing obesity among younger adults to project future obesity rates. As discussed previously, the resulting projections show that, unless preventive measures are taken, the number of obese Texans will surge to 15 million by 2040, representing 43 percent of the state’s adult population (Figure 8-2).
Fonseca stressed that very conservative data and methods were used to generate these projections so as to err on the low side. He also noted that
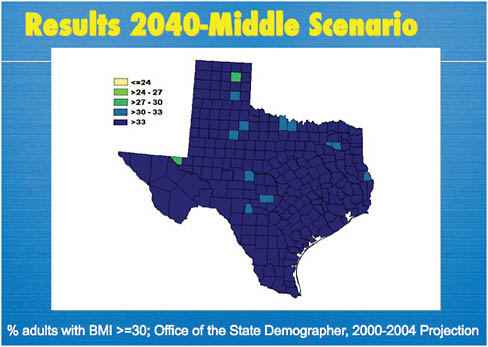
he and his colleagues had oversampled the border communities that face greater health risks due to poor nutrition, as well as major metropolitan areas with dense populations.
Discussions with the panel revealed several challenges faced by the Live Smart Texas Coalition. According to Donna Nichols, “To have a coalition this size takes a lot of feeding and watering…. When it gets really tough and there is gnashing of teeth and pulling of hair, you have to rely back on your guiding principles to say, ‘Yes, this is what we believe in.’” Klaus Madsen, Vice President of Programs, Texas Health Institute, noted that the coalition went through a phase in which it was closely allied with the State Health Officer, but this relationship changed following governmental reorganization. He stated, “One of the lessons learned is that sometimes, it is important to have people outside of governmental public health to drive a public health coalition, because [of the] ebbs and flows” that can occur with such changes in governmental leadership.
Michelle Smith, Chair, Partnership for a Healthy Texas, suggested that when working with policy makers, it is important to present statistics illustrating the scope of the problem of interest and how those statistics pertain to constituents. She also stressed how narrow the policy window can be
and therefore how important it is to move quickly to advance an agenda with policy makers.
Fonseca followed up on Smith’s points by noting that it is difficult to achieve health initiatives for children in all communities through state efforts alone. His perspective suggests that obesity prevention might be more successful in a state if the federal government instituted national mandates, such as nutritional updates to the National School Lunch and Breakfast Programs, improvements to the Food Stamp and WIC Programs, and better food and menu labels. He added that this approach might also be a more cost-effective way of reducing obesity than implementing interventions that require local financial or human resources. For example, mandating that schools offer nonfat or 1 percent milk instead of 2 percent milk would shave roughly 20 calories off of every carton of milk children drink at no cost to schools.