APPENDIX B
NATIONAL INSTITUTES OF HEALTH SUPPORT OF RESEARCH IN DEPARTMENTS OF OBSTETRICS AND GYNECOLOGY*
ROBERT A. WALKINGTON
The National Institutes of Health (NIH) is the major supporter of biomedical research conducted in the nation's universities and medical schools. In 1989, 60 percent of funds for biomedical research in academic institutions came from NIH, compared with 8 percent from private, non-profit sources and 6 percent from industry.1 In medical schools, over 75 percent of funds for sponsored research comes from the federal government, the majority from NIH.2 NIH support in FY 1989 included over $500 million for clinical trials, $245 million to support research training, $90 million for career development awards and $120 million to support beginning researchers.3 Since it is peer reviewed in national competition, NIH support is considered a standard of excellence. For this reason it can be used to leverage other support: from the community, from private sources and from industry.
For more than a decade there has been concern that clinical research is not adequately supported. This is thought in part to be because physician-scientists are relatively unsuccessful in winning NIH peer awards. The following comments are indicative of interwoven concerns.
''Whether for lack of time, expectation of greater funding, more ability to control variables or other reasons, the physician-investigator has turned away from involvement in human research. Obtaining funding for human studies is considered so difficult that many investigators are discouraged and in some instances, bitter."4
"Concerns of insufficient access to research support have been voiced by a variety of individual surgical investigators. Frustrated by a perceived inability to successfully compete for NCI grant support, some surgical oncologists have criticized aspects of the current NCI peer-review mechanisms for awarding grants."5
"It is essential to understand that in 1988 it is effectively impossible for an individual investigator to obtain NIH funding for human investigation."6
"If I leave here (Intramural Program) I will leave research" [because its impossible to get a grant for clinical research].7
"Friedman told the board that clinical investigators do complain that is very difficult to get RO1 grants: 'The perception is that they receive poorer priority scores and inferior funding', he remarked. 'If one looks at...comparisons by program...it's evident, that year by year, there are inferior funding rates for the clinical proposals compared to the preclinical proposals' Friedman stated. 'This does not indicate whether the proposals are good or not'; 'I would argue that some of them are [good]. What we need is [the submission of] more good clinical proposals.'"8
The evidence to support these concerns is mixed. Different studies, using different data bases and or time periods, have produced different results. A study conducted at NIH in the early 1980s showed that between 1976–1981 only 63 percent of clinical applications were approved compared with 74 percent of basic science applications. The study also found that approved clinical applications received poorer priority scores than did those dealing with basic research.9 M.D. applicants in 1985 had a higher disapproval rate (9.1 percent) than Ph.D. applicants (6.8 percent). During the decade 1975–1985, Ph.D.s had consistently slightly better priority scores than M.D.s on competing RO1 applications. 10 Recent NIH data, however, indicate that between 1987 and
1989 M.D.s had slightly higher success rates than Ph.D.s in competing for research-project grants, of which the majority are RO1s.11
A 1986 study indicated that between 1975 and 1985 the number of ROI applications from M.D.s and M.D./Ph.D.s increased by 30 percent, compared with an increase of 83 percent in applications by Ph.D.s. The proportion of new applications submitted by M.D.s dropped from 31 percent of total R01 applications in 1975 to 25 percent in 1986.
There is also concern that the number of physicians in clinical research is declining, though conclusive data are lacking.12,13,14,15, 16,17 Particular concern is expressed over the shortage of physicians involved in patient oriented clinical research. Reasons suggested for the decline include:
-
increasing indebtedness of medical school graduates;
-
increasing difficulty of maintaining competency in both science and medicine;
-
perceived insecurities associated with extramural research funding for clinical investigation;
-
problems associated with financial soundness of academic departments combined with increasing demands for faculty to engage in clinical practice;
-
expectations with less willingness to undergo relative deprivation;
-
the paucity of role models and inadequate mentoring; and
-
curriculum deficiencies in medical schools.18
In addition to the general problems related to NIH support of clinical research and the physician-scientist, specific concerns have been expressed about the paucity of research conducted in departments of OB/GYN. The IOM Planning Committee for the current study concluded that departments of OB/GYN lagged in receiving support from NIH for research and speculated that:
"possible causes related to the politicalization of problems relating to the status of the fetus, lack of organizational focus for reproductive research at NIH, the lack of a national consensus concerning the ethical issues raised by some reproductive research ... there is also the possibility that the absence of OB/GYN presence in the NIH intramural program results in a relative disregard of OB/GYN research."19
NIH support appears to be hindered by three interrelated problems: 1) the quality of the research being proposed 2) the nature of the research, and 3) the
organizational structure and management of NIH in general and with regard to the review of grant proposals. There are a few studies that illuminate the quality of OB/GYN research, or research proposals: In 1986, research grant applications (competing RO1s) from OB/GYN departments had the poorest average priority scores of nine clinical departments studied—a decline from FY 1979 when OB/GYN ranked in the middle (5th of 9) of the clinical departments studied.20 A study focusing on clinical oncology support from the National Cancer Institute showed that between FYs 1980 and 1985 OB/GYN departments had success rates substantially lower than departments of medicine, pediatrics and radiology. While the success rated varied greatly from year to year, for 3 of the 6 years the rate for OB/GYN was substantially lower than that of the other departments. The decline in success rates between 1980 and 1985 was greater for OB/GYN than the three other departments studied.21
A measure of the research intensity of a department is the degree to which faculty are involved in research. A 1989 Association of American Medical Colleges (AAMC) study, analyzed the distribution of full-time faculty of U.S. medical schools who are principal investigators on NIH or Alcohol, Drug Abuse and Mental Health Administration (ADAMHA) research awards by department and degree. The study linked the AAMC Faculty Roster (1988)—with records of NIH and ADAMHA research awards (FY 1987). This linkage allowed awards made to affiliated hospitals to be credited to the appropriate department. OB/GYN departments ranked 11th of 17 clinical departments with 9.8 percent of their faculty being principal investigators, compared with an average of 14 percent for all clinical departments. Examination of the data by the degree of the principal investigator reveals that the discrepancy between OB/GYN and more research intensive departments can be attributed to the M.D. and M.D./Ph.D. faculty. Ph.D.s in OB/GYN departments are principal investigators at a rate above the average for all clinical departments (Ph.D.s in OB/GYN departments ranked 6th of 17 clinical departments; M.D and M.D/Ph.D.s ranked 12th). (Table B-1).22
According to a 1986 survey of academic manpower in OB/GYN departments, almost all the Ph.D. faculty and 61 percent of the M.D. faculty reported involvement in research.23 A survey in 1990 asked faculty to indicate if they spent at least 20 percent of their time in research. Although 92 percent of the Ph.D. faculty indicated that they were so involved, only 38 percent
TABLE B-1: Percentage of Full Time Faculty, in Clinical Departments Who are PIs on NIH/ADMHA Awards (1988)
|
|
Total Full Time Faculty |
Total M.D.s |
||
|
Department |
No. |
%PIs |
No. |
%PIs |
|
Opthalmology |
1,014 |
36.5 |
650 |
25.7 |
|
Neurology |
1,637 |
23.9 |
1,101 |
18.4 |
|
Dermatology |
365 |
22.5 |
291 |
20.0 |
|
Int. Medicine |
13,448 |
19.9 |
10,894 |
17.7 |
|
Pathology |
1,152 |
17.0 |
656 |
13.9 |
|
Public Health |
1,127 |
15.7 |
445 |
10.6 |
|
Other Clinical |
69 |
14.5 |
21 |
19.0 |
|
Otolaryngology |
543 |
14.2 |
296 |
6.4 |
|
Pediatrics |
5,724 |
13.4 |
4,503 |
11.9 |
|
Psychiatry |
5,244 |
12.1 |
2,858 |
8.1 |
|
OB/GYN |
2,265 |
9.8 |
1,687 |
5.9 |
|
Surgery |
5,031 |
9.5 |
4,038 |
7.0 |
|
Radiology |
3,884 |
8.3 |
2,786 |
3.2 |
|
Orthope. Surgery |
730 |
7.8 |
569 |
4.4 |
|
Anesthesiology |
2,649 |
3.5 |
2,186 |
1.6 |
|
Phy. Med/Rehab. |
548 |
1.2 |
341 |
0.9 |
|
Family Medicine |
1,539 |
1.2 |
1,127 |
0.7 |
|
Total/Average |
45,969 |
14.0 |
34,449 |
11.1 |
|
|
Total M.D./ Ph.D.s |
Total Ph.D.s |
||
|
Department |
No. |
%PIs |
No. |
%PIs |
|
Opthalmology |
61 |
39.3 |
245 |
69.4 |
|
Neurology |
148 |
37.8 |
315 |
35.6 |
|
Dermatology |
22 |
40.9 |
43 |
34.9 |
|
Internal Medicine |
875 |
31.1 |
1,261 |
33.9 |
|
Pathology |
122 |
25.4 |
280 |
22.1 |
|
Public Health |
48 |
14.3 |
472 |
25.0 |
|
Other Clinical |
2 |
0.0 |
41 |
12.2 |
|
Otolaryngology |
28 |
25.0 |
171 |
27.5 |
|
Pediatrics |
275 |
28.4 |
614 |
21.8 |
|
Psychiatry |
197 |
18.8 |
1,728 |
20.2 |
|
OB/GYN |
126 |
13.5 |
320 |
32.2 |
|
Surgery |
268 |
17.9 |
540 |
25.9 |
|
Radiology |
169 |
13.6 |
696 |
29.0 |
|
Orthope. Surgery |
23 |
13.0 |
81 |
34.6 |
|
Anesthesiology |
181 |
8.8 |
157 |
22.3 |
|
Phy. Med/Rehab. |
18 |
5.6 |
97 |
6.2 |
|
Family Medicine |
25 |
0.0 |
265 |
6.8 |
|
Total/Average |
2,589 |
24.3 |
7,327 |
26.9 |
|
SOURCE: AAMC Medical School Faculty Roster (1988) linked with IMPAC record of research grants (NIH and ADAMHA) and Contracts (NIH) that received funds during FY 1987. |
||||
of the M.D. faculty were.24 Because of differences in the wording of questions the two surveys are not comparable. Roughly comparable data exist for departments of internal medicine. A study in the early 1980s indicated a more intense involvement in research of physician faculty in departments of internal medicine than in departments of OB/GYN in 1990, with 50 percent of internal medicine faculty with an M.D. degree spending at least 20 percent of their time
engaged in research. Seventy seven percent of the faculty with Ph.D. degree spent at least 10 percent of their time in research.25
Although data are not available on the level of NIH support for research in reproductive issues, or for women's health in general, there are strongly held views about the interest of NIH in those topics. It should be remembered that human embryo research cannot be supported by federal funds. The following comments from letters from chairman of departments of OB/GYN to the IOM committee indicate some concerns:
''Funding has been confused by the political turmoil surrounding sex education, abortion and contraception. Because of this departments must seek funding outside the federal government; pharmaceutical and equipment companies etc. or find clinical income to support research".
"Funding has moved from NIH and NSF to pharmaceutical companies with interests in product development. Some types of clinical research (sohographic studies of the fetus in utero) are impossible to fund through NIH, despite their importance. These studies are conducted with support from clinical income, but not at the standard of peer reviewed funding".
In addition to the political, and ethical ramifications of some areas of OB/GYN research, many OB/GYNs in medical schools believe that NIH lacks interest in reproductive issues and women's health in general. Again, comments from some department chairmen indicate these concerns:
"Lack of NIH commitment to women's health research is evidenced by composition of study sections, no separate institute and few NIH OB/GYNs".
"The governance of NIH is neither responsive nor interested in women's issues. They will only act if they think they can direct funds to other specialties. An example is the lack of representation by chairman of OB/GYN departments in the governing councils of the NIH. The NIH Advisory Committees are comprised of approximately 3,056 individuals; of those only 26 are OB/GYNs yet the most common cause for admission to most acute hospitals are in OB/GYN. I would agree with the GAO that arrogance and indifference summarize the attitude of the NIH towards women's issues and departments of OB/GYN. The NIH is not "national" in that is not representative of
the nation or its health issues, as more than half of the nation are women".
The data and beliefs cited indicate a need to examine more closely what has been happening to OB/GYN departments in the competition for funds, and a need to indicate where one might seek change to improve the outcome.
NIH Support for OB/GYN Research
Overview
"Federal funding of research in academic departments of OB/GYN in the United States has never been substantial and the situation is no different today."26
In FY 1978, the majority of federal support for OB/GYN departments came from the Department of Health, Education and Welfare (DHEW), now the Department of Health and Human Services, with a small amount coming from the Agency for International Development. Of the money from DHEW, over 90 percent came from NIH with small amounts from ADAMHA and the Bureau of Maternal and Child Health. The picture in FY 1989 was similar, with HHS providing the large majority of federal support, and most of that coming from NIH.
Figure B-1 shows total NIH support for OB/GYN departments in both current and constant (1968) dollars. Growth in constant dollars has been modest, from $7 million in 1968 to $12 million in 1989 (71 percent). Between 1968 and 1989 OB/GYN departments slightly increased their share of NIH funds—current dollar support to OB/GYN departments grew by 570 percent while overall NIH research support grew by only approximately 550 percent. Between 1978 and 1989, support to OB/GYN departments increased by approximately 190 percent while overall NIH support grew by approximately 150 percent. The increased support of departments of OB/GYN in the 1980s is actually more impressive than the percentages indicate since the two institutes providing the majority of the support the National Institute of Child Health and Human Development (NICHD) and the National Cancer Institute (NCI) both had budget increases below the NIH average for the decade.
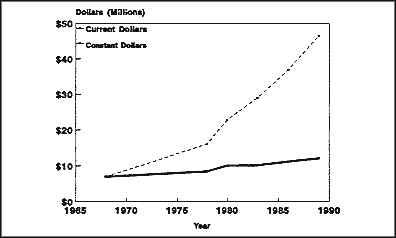
Figure B-1: NIH support of departments of OB/GYN, current and constant (1968) dollars.
SOURCE: Special tabulation by NIH.
OB/GYN departments received a fairly constant share of NIH funds going to medical schools—1.5 percent in 1968, 1.4 percent in 1978 and 1.5 percent in 1989. OB/GYN faculty received approximately 2.7 percent of the NIH/ADAMHA awards to clinical departments.* However, the departments received slightly less than would be expected on the basis of size of faculty, since OB/GYN departments had approximately 3.7 percent of the total full time medical schools faculty and 4.8 percent of the flail time faculty in clinical departments in 1988.
NICHD has been the major NIH supporter of OB/GYN departments, providing 69 percent of support in 1968, falling to 56 pete t in 1978, returning to 69 percent in 1989. Support from the NCI fell from 31 percent in 1978 to 9 percent in 1989, although in 1989 it was still the second largest NIH funder of OB/GYN departments. The National Institute of Allergy & Infectious Diseases (NIAD) increased its support of OB/GYN departments, mostly because of a $1.7 million contract to study prenatal transmission of HIV. The Heart, Lung and Blood Institute (NHLBI) and the Division of Research Resources (DRR) also showed major increases, the latter due largely to a grant and a cooperative agreement with Emory University for "support of animal resources available to all qualified investigators without regard to scientific disciplines or disease orientation." (Table B-2).
TABLE B-2: NIH Support of Departments of OB/GYN By Institute, FYs 1968, 1978, 1989
|
Institute |
1968 |
1978 |
1989 |
|
NICHD |
$4,793,336 |
$8,977,923 |
$32,023,354 |
|
NCI |
823,276 |
4,997,132 |
4,362,099 |
|
NHLBI |
213,314 |
451,276 |
1,859,406 |
|
NIA |
— |
448,292 |
774,409 |
|
NIADDK |
898,441 |
930,580 |
1,656,883 |
|
NIDR |
16,000 |
187,040 |
— |
|
FIC |
10,661 |
77,541 |
55,496 |
|
NIGMS |
73,265 |
59,114 |
389,055 |
|
NIDCDS |
— |
15,200 |
1,013,612 |
|
NIAID |
— |
— |
2,494,911 |
|
DRR |
120,031 |
— |
946,000 |
|
NIEHS |
— |
— |
796,639 |
|
NEI |
— |
— |
161,632 |
|
Total NIH Support |
6,948,324 |
16,144,098 |
46,533,496 |
|
Percent of NIH Support to Medical Schools |
1.5 % |
1.4% |
1.5% |
Table B-3 shows competitive and noncompetitive NIH awards to OB/GYN departments, 1980–1989, by number and type of award (later tables reflect only competitive awards—new or competing continuations). OB/GYN department support more than doubled ($22.8 million to $46.5 million), however, since the size of awards increased, the number of awards increased more modestly. The number of research grants increased, but the number of contracts declined from 11 to 7, although contract dollar support more than doubled. Awards for training grants and fellowships combined fell in both number and dollars. These trends generally reflect the overall NIH experience during the decade.
TABLE B-3: Total NIH Awards to OB/GYN Departments (By Major Type) Thousands of Dollars 1980–1989
|
|
Total Awards |
Research Grants |
Contracts |
|||
|
Year |
No. |
$ |
No. |
$ |
No. |
$ |
|
1980 |
246 |
22,764 |
202 |
20,676 |
11 |
1,373 |
|
1881 |
236 |
26,084 |
212 |
24,444 |
8 |
1,256 |
|
1982 |
232 |
26,009 |
203 |
23,871 |
9 |
1,601 |
|
1983 |
233 |
28,978 |
200 |
25,792 |
13 |
2,713 |
|
1984 |
251 |
33,479 |
222 |
29,869 |
11 |
3,112 |
|
1985 |
246 |
36,415 |
222 |
33,383 |
9 |
2,525 |
|
1986 |
256 |
36,947 |
222 |
34,563 |
10 |
1,694 |
|
1987 |
275 |
41,902 |
250 |
39,493 |
9 |
1,943 |
|
1988 |
272 |
45,454 |
247 |
44,602 |
9 |
3,184 |
|
1989 |
258 |
46,533 |
235 |
42,678 |
7 |
3,229 |
|
|
Training Grants |
Fellowships |
||
|
Year |
No. |
$ |
No. |
$ |
|
1980 |
7 |
338 |
26 |
377 |
|
1881 |
6 |
236 |
10 |
148 |
|
1982 |
5 |
246 |
15 |
291 |
|
1983 |
4 |
200 |
16 |
268 |
|
1984 |
4 |
21 |
14 |
278 |
|
1985 |
4 |
270 |
11 |
237 |
|
1986 |
4 |
247 |
20 |
443 |
|
1987 |
3 |
185 |
13 |
280 |
|
1988 |
7 |
445 |
9 |
222 |
|
1989 |
7 |
371 |
9 |
255 |
The number of OB/GYN departments receiving awards fluctuated slightly, and in 1989 was three fewer than in 1980. There was little change in the distribution of awards (number and dollars) among OB/GYN departments between 1980 and 1989 (Table B-4), with ten departments receiving approximately 50 percent of the funds and 40 percent of awards. In 1989 only 4 departments had more than 10 awards while 15 had only one award, 17 had two awards and 9 had three awards. This distribution is similar to, but somewhat more concentrate than, the distribution of total NIH funds: 20 medical schools received 50 percent of NIH extramural funds going to medical schools in FY 1989. This concentration of research in a relatively small number of institutions highlights the difficulty of developing new and successful research efforts in part because of the limited number of locations that are suitable for expanded research training.
TABLE B-4: Total NIH Awards to OB/GYN Departments and Awards to Top Ten Departments, Thousands of Dollars, 1980–1989
|
Year |
No. of Depts. w/ Awards |
Total Awards |
Awards to Top Ten |
||||
|
|
|
No. |
$ |
No. |
% |
$ |
% |
|
1980 |
70 |
246 |
22,764 |
102 |
41 |
11,400 |
50 |
|
1981 |
69 |
236 |
26,084 |
88 |
37 |
12,865 |
49 |
|
1982 |
69 |
232 |
26,009 |
81 |
35 |
12,511 |
48 |
|
1983 |
71 |
233 |
28,978 |
82 |
35 |
13,439 |
46 |
|
1984 |
72 |
251 |
33,479 |
95 |
38 |
15,550 |
46 |
|
1985 |
69 |
246 |
36,415 |
100 |
41 |
17,661 |
48 |
|
1986 |
69 |
256 |
36,974 |
97 |
38 |
17,985 |
49 |
|
1987 |
70 |
275 |
41,902 |
99 |
36 |
20,153 |
48 |
|
1988 |
69 |
272 |
45,454 |
110 |
40 |
21,341 |
47 |
|
1989 |
67 |
258 |
46,533 |
102 |
40 |
24,856 |
53 |
The past decade has seen little change in which departments of OB/GYNs received the majority of NIH awards. Of the departments ranked in the top 10 in 1980, 8 were in the top ten in 1989 (and one was 11th). Only one of departments in the top 10 in 1980 dropped significantly in the ranking—that department was in the top 10 for the first 5 years of the decade but subsequently fell to 24th place. A total of only 15 departments were ranked in the top 10 during the decade.*
While the number of applications from departments of OB/GYN fluctuated from year to year, applications from M.D.s decreased. The number of applications from Ph.D.s increased. Ph.D.s also achieved a higher success rate than M.D.s (Table B-5).
TABLE B-5: Success Rates of Competing Applications from OB/GYN Departments by Degree of Principal Investigator, 1980–1989
|
Number of Year |
Applications |
Awards |
Success Rate |
|
All Applications |
|||
|
1980 |
216 |
82 |
38.0% |
|
1981 |
247 |
54 |
21.9 |
|
1982 |
242 |
68 |
28.1 |
|
1983 |
227 |
63 |
27.7 |
|
1984 |
308 |
88 |
28,6 |
|
1985 |
322 |
66 |
20.5 |
|
1986 |
331 |
83 |
25.1 |
|
1987 |
259 |
76 |
29.3 |
|
1988 |
268 |
74 |
27.6 |
|
1989 |
249 |
52 |
21.0 |
|
Total |
2,669 |
706 |
26.5 |
|
M.D. Applications |
|||
|
1980 |
87 |
33 |
37.9% |
|
1981 |
115 |
17 |
17.7 |
|
1982 |
96 |
27 |
28.1 |
|
1983 |
79 |
11 |
13.9 |
|
1984 |
122 |
42 |
34.4 |
|
1985 |
124 |
19 |
15.3 |
|
1986 |
123 |
24 |
19.5 |
|
1987 |
102 |
27 |
26.5 |
|
1988 |
101 |
33 |
32.7 |
|
1989 |
64 |
12 |
18.7 |
|
Total |
1,013 |
245 |
24.2 |
|
Number of Year |
Applications |
Awards |
Success Rate |
|
Ph.D. Applications |
|||
|
1980 |
110 |
42 |
38.2% |
|
1981 |
115 |
33 |
28.7 |
|
1982 |
130 |
38 |
29.2 |
|
1983 |
133 |
46 |
34.6 |
|
1984 |
166 |
42 |
25.3 |
|
1985 |
177 |
43 |
24.3 |
|
1986 |
178 |
50 |
28.1 |
|
1987 |
145 |
48 |
33.1 |
|
1988 |
152 |
38 |
25.0 |
|
1989 |
167 |
36 |
21.5 |
|
Total |
1,473 |
416 |
28.2 |
Support by Institute
As noted earlier, support for departments of OB/GYN comes mainly from a few NIH institutes, with NICHD providing the majority of such support. Slightly more than a quarter of all competing applications from departments of OB/GYN were awarded support. Applications to NIDDK had the highest ess rate with 28.9 percent of approved applications funded. Applications to NICHD and NCI (nearly 85 percent of total OB/GYN applications) had success rates of 26.7 and 24.9 respectively. Applications from departments of OB/GYN to NHLBI and NIAID were less successful in winning awards (Table B-6). No trend in success rates by institute over the decade was discernible.
TABLE B-6: NIH Competing Applications from OB/GYN Departments by Funding Institute, 1980–1989
|
Number of Institute |
Number of Applications |
Number Awarded |
Percent Awarded |
|
NICHD |
1,759 |
469 |
26.7 |
|
NCI |
457 |
114 |
24.9 |
|
NHLBI |
110 |
18 |
16.4 |
|
NIAID |
49 |
6 |
12.2 |
|
All Other |
211 |
75 |
35.6 |
|
Decade Total |
2,669 |
706 |
26.5 |
Support by Review Group
Each application submitted to NIH is assigned to an Initial Review Group (IRG) to be assessed for scientific merit and assigned a priority score if recommended for approval. Applications recommended for approval by the IRGs axe then reviewed by an institute's National Advisory Council and considered for funding. Funding is based primarily on the score assigned by the IRG but consideration is also given to the amount of money available for extramural research and the contributions the proposed activity would make to advancing the mission and programs of the institute.
Although there are a large number of IRGs, a small number of them review the majority of applications submitted by OB/GYN departments. In 1989, for example, 54 IRGs reviewed applications submitted by OB/GYN departments, 27 received only one application and another 11 received only two or three applications. On the other hand, four IRGs, Biochemical Endocrinology, Human Embryology and Development, Reproductive Biology and Reproductive Endocrinology (created in 1985) together received 50 percent of all competing applications from OB/GYN departments during the past decade. In 1989 these four IRGs reviewed 125 out of the 247 applications submitted, with Reproductive Biology reviewing the largest number.
Table B-7 shows the success rates (number of awards divided by number of applications) for applications from OB/GYN departments sent to the four IRGs which review the greatest number of applications from OB/GYN departments. Applications from OB/GYN departments reviewed by the
Biochemical Endocrinology and Reproductive Biology study sections had the highest success rates of the four. Although success rates varied from year to year, in general OB/GYN departments experienced a slight decline in sucks rates in the second half of the decade. The three IRGs that were active for the entire decade (Reproductive Endocrinology was created in 1985) all saw their workload from departments OB/GYN increase in the middle of the decade and then decrease to the previous level or slightly lower in the last several years.
OB/GYN Departments Compared with Other Clinical Departments
Another way to assess the success of OB/GYN departments in the competition for NIH funds is to compare them with other clinical departments. Medicine, the largest clinical department, was chosen for comparison with OB/GYN because it is a recognized leader in clinical research; pediatrics, because it ''shares'' an institute with OB/GYN and because of its numerous interrelationships with OB/GYN; surgery was chosen because of its emphasis on technique; and radiology because it is closer to OB/GYN in faculty size than the other clinical departments, and because it is similar to OB/GYN in terms of percent of faculty who were principal investigators on NIH/ADAMHA grants. Data on grant applications from urology departments are not available. Data on two surgical subspecialties which would have provided interesting comparisons, orthopedics and otolaryngology, were available but the number of full time faculty and grants submitted were too small for analysis.
TABLE B-7: NIH Competing Applications from OB/GYN Departments, Success Rates by Selected IRGS, 1980–1989
|
Year |
Submitted |
Awarded |
Success Rate |
Success Rate of OB/GYN in All IRGs |
|
Reproductive Biology |
||||
|
1980 |
40 |
14 |
34.1% |
37.8% |
|
1981 |
49 |
17 |
34.0 |
21.8 |
|
1982 |
50 |
15 |
30.0 |
27.8 |
|
1983 |
52 |
17 |
32.7 |
27.6 |
|
1984 |
61 |
15 |
24.6 |
28.1 |
|
1985 |
59 |
15 |
25.4 |
20.2 |
|
1986 |
43 |
12 |
27.9 |
25.2 |
|
1987 |
41 |
14 |
32.6 |
28.7 |
|
1988 |
44 |
12 |
27.3 |
27.6 |
|
1989 |
40 |
6 |
15.0 |
20.9 |
|
Total |
479 |
137 |
28.6 |
|
|
Reproductive Endocrinology |
||||
|
1985 |
12 |
0 |
0.0% |
20.2% |
|
1986 |
21 |
9 |
42.9 |
25.2 |
|
1987 |
26 |
5 |
19.2 |
28.7 |
|
1988 |
24 |
5 |
20.8 |
27.6 |
|
1989 |
26 |
4 |
15.4 |
20.9 |
|
Total |
109 |
23 |
21.0 |
26.2 |
|
Year |
Submitted |
Awarded |
Success Rate |
Success of OB/GYN ins Rate All IRGs |
|
Biochemical Endocrinology |
||||
|
1980 |
31 |
13 |
41.9% |
37.8% |
|
1981 |
36 |
11 |
36.1 |
21.8 |
|
1982 |
54 |
18 |
33.3 |
27.8 |
|
1983 |
35 |
13 |
37.1 |
27.6 |
|
1984 |
51 |
10 |
19.6 |
28.1 |
|
1985 |
44 |
13 |
28.3 |
20.2 |
|
1986 |
35 |
10 |
28.6 |
25.2 |
|
1987 |
34 |
10 |
29.4 |
28.7 |
|
1988 |
25 |
5 |
20.0 |
27.6 |
|
1989 |
25 |
6 |
24.0 |
20.9 |
|
Total |
370 |
111 |
30.0 |
26.2 |
|
Human Embryology and Development |
||||
|
1980 |
34 |
11 |
32.4% |
37.8% |
|
1981 |
28 |
3 |
10.7 |
21.8 |
|
1982 |
29 |
1 |
3.4 |
27.8 |
|
1983 |
34 |
2 |
5.9 |
27.6 |
|
1984 |
33 |
17 |
47.2 |
28.1 |
|
1985 |
48 |
6 |
12.5 |
20.2 |
|
1986 |
27 |
5 |
18.5 |
25.2 |
|
1987 |
26 |
9 |
33.3 |
28.7 |
|
1988 |
29 |
8 |
27.6 |
27.6 |
|
1989 |
29 |
6 |
20.7 |
20.9 |
|
Total |
317 |
68 |
21.5 |
26.2 |
In reviewing the comparisons among departments it is important to remember the relative sizes of the departments (Table B-8). Internal medicine had nearly six times as many full time faculty in 1988 as OB/GYN, while pediatrics and surgery had more than twice as many as OB/GYN. Radiology departments had almost twice as many full-time faculty as departments of OB/GYN.
TABLE B-8: Full Time Faculty and Competing Applications, Selected Clinical Departments, 1980–1989
|
|
Full Time Faculty 1988 |
Competing Applications 1980–1989 |
||
|
Department |
Number |
Percent |
Number |
Percent |
|
OB/GYN |
2,265 |
7 |
2,667 |
6 |
|
Pediatrics |
5,724 |
19 |
6,801 |
15 |
|
Radiology |
3,884 |
13 |
3,325 |
7 |
|
Surgery |
5,031 |
17 |
6,117 |
13 |
|
Medicine |
13,448 |
44 |
27,238 |
59 |
|
Total |
30,352 |
100 |
46,148 |
100 |
Departments of internal medicine submitted a disproportionately large number of applications (59 percent of the total with 44 percent of faculty). Applications from OB/GYN, pediatrics and surgery are roughly proportionate to their faculty size, and radiology is underrepresented relative to faculty size.*
OB/GYN departments had significantly lower success rate for the decade than internal medicine, pediatrics or radiology. While the success rate for surgery was also higher than OB/GYN the difference was not statistically significant (Table B-9). Data suggest that weakness in the success rates of OB/GYN departments became more acute in the second half of the decade.
TABLE B-9: Success Rates of Competing Applications from Selected Clinical Departments Overall and by Degree of Principal Investigator, 1980–1989
|
Department |
Number of Applications |
No. of Awards |
Success Rate |
|
All Applications |
|||
|
OB/GYN |
2,669 |
706 |
26.5% |
|
Medicine |
27,240 |
10,242 |
37.6* |
|
Pediatrics |
6,801 |
2,105 |
31.0* |
|
Radiology |
3,335 |
1,111 |
33.4* |
|
Surgery |
6,117 |
1,742 |
28.5 |
|
Total |
46,148 |
15,866 |
34.4 |
|
M.D. |
|||
|
OB/GYN |
1,013 |
245 |
24.2% |
|
Medicine |
17,684 |
6,962 |
39.4* |
|
Pediatrics |
4,327 |
1,134 |
37.7* |
|
Radiology |
920 |
278 |
30.2* |
|
Surgery |
3,522 |
1,059 |
30.1* |
|
Total |
27,466 |
9,956 |
36.3 |
|
Ph.D. |
|||
|
OB/GYN |
1,473 |
416 |
28.2% |
|
Medicine |
7,126 |
2,428 |
34.1* |
|
Pediatrics |
1,794 |
478 |
26.7 |
|
Radiology |
2,127 |
745 |
35.0* |
|
Surgery |
2,038 |
547 |
26.9 |
|
Total |
14,558 |
4,614 |
31.7 |
|
* Significant at 95% confidence level when compared with OB/GYN |
|||
Degree of Principal Investigator
The pattern changes if we look at performance by degree of the principal investigator. Table B-10 displays the percentage of full time faculty that are M.D.s and the percentage of grant applications from their departments that they submitted. Most full time faculty have the M.D. degree (ranging from 72 percent in radiology to 81 percent in medicine). M.D.s in departments of internal medicine, pediatrics and surgery, submitted between 58 percent and 65 percent of applications from their departments, while only 28 percent of the applications from radiology and 38 percent of the applications from OB/GYN came from M.D.s. Internal medicine was the only department, at to show an increase in the percentage of applications by M.D.s between 1980 and 1989 decade. During that period M.D.s in OB/GYN had the lowest success rates and the fewest awards among the five departments. Internal medicine did significantly better that the other departments in every year while there was some annual variation among the other departments. OB/GYN was at or near the bottom in most years of the decade.
TABLE B-10: Percent of Total Faculty that are M.D.s Compared with Percentage of Grant Applications to NIH Submitted by M.D. s, Selected Clinical Departments, 1980–1989
|
Department |
M.D.s as Percent of Full Time Faculty |
M.D. Grant Applications as Percent of Department's Applications |
|
OB/GYN |
74 |
38 |
|
Pediatrics |
79 |
64 |
|
Radiology |
72 |
28 |
|
Surgery |
80 |
58 |
|
Internal Med. |
81 |
65 |
The picture with regard to applications submitted by Ph.D.s is different (Table B-9). Ph.D.s, in OB/GYN departments were more competitive than their M.D. colleagues in the department and their approval rate trailed only Ph.Ds in
medicine and radiology. Between 1980 and 1989, the number of applications from Ph.D.s and their approval rates increased in all five departments.
Investigator Initiated Research (RO1s)
The NIH supports a wide variety of research and research training activities. However, the core of NIH research support is the investigator initiated research grant, the RO1. The RO1 is intended "...to support a discrete, specific project in an area representing the insterests and competencies of the principal investigator." The majority of NIH awards are for RO1s—in 1989 they constituted 62 percent of all research grants. Of the five depots analyzed, departments of medicine submitted the largest number of RO1 applications, had the most approved and funded and had the highest success rates in the period 1980 to 1989 (Table B-11). The differences in success rates for the decade between OB/GYN and medicine and radiology were statistically significant. Again, applications for RO1s from OB/GYN departments declined in competitiveness during the later years of the decade.
TABLE B-11: Success Rates of RO1 Applications, Selected Clinical Departments, 1980–1989
|
Department |
Number of Applications |
No. of Awards |
Success Rate |
|
All Applications |
|||
|
OB/GYN |
1,954 |
458 |
23.4 % |
|
Internal Medicine |
16,336 |
5,145 |
31.5* |
|
Pediatrics |
4,369 |
1,106 |
25.3 |
|
Radiology |
2,538 |
771 |
30.4* |
|
Surgery |
4,258 |
1,044 |
24.5 |
|
Total |
29,455 |
8,524 |
28.9 |
|
Department |
Number of Applications |
No. of Awards |
Success Rate |
|
M.D. |
|||
|
OB/GYN |
628 |
112 |
17.8% |
|
Internal Medicine |
10,146 |
3,313 |
32.7* |
|
Pediatrics |
2,676 |
694 |
26.0* |
|
Radiology |
625 |
155 |
24.8* |
|
Surgery |
2,216 |
550 |
24.8* |
|
Total |
16,291 |
4,824 |
29.6 |
|
Ph.D. |
|||
|
OB/GYN |
1,190 |
314 |
26.4% |
|
Internal Medicine |
4,620 |
1,367 |
29.6* |
|
Pediatrics |
1,247 |
291 |
23.3 |
|
Radiology |
1,682 |
556 |
33.1* |
|
Surgery |
1,645 |
416 |
25.3 |
|
Total |
10,384 |
2,944 |
28.4 |
|
* Significant at 95% confidence level when compared with OB/GYN. |
|||
Most RO1s from departments of internal medicine and pediatrics were submitted by M.D.s, while in radiology and OB/GYN most RO1s were submitted by Ph.D.s. The situation in surgery was different. Between 1980 and 1989, 58 percent of RO1s were submitted by M.D.s. However, towards the end of the 1980s the percentage of applications from M.D.s fell, and, there was a modest increase in the percentage of applications submitted by Ph.D.s.
Between 1980 and 1989, OB/GYN departments experienced a comparatively low success rate (Table B-11)—the differences between OB/GYN and the other four departments were statistically significant. However, Ph.D.s from
departments of OB/GYN experienced a success rate in the middle of the five departments, significantly below internal medicine and radiology, and above pediatrics and surgery (not statistically significant). Data suggest a modest deterioration in the competitiveness of OB/GYN departments in the second half of the decade.
NIH Support for OB/GYN Research Training
Fellowships and Institutional Training Awards
NIH has supported research training for many years and while the magnitude of such support has declined since the 1960s it is still a major focus of NIH effort. In FY 1989, funds for research training totaled $262 million, or 4.3 percent of the total extramural program. This compares with FY 1980 when funding totaled $182.8 million, or 6.6 percent of the extramural budget. Training support is in the form of fellowships which NIH awards directly to individuals, and training grants which NIH awards to institutions which in turn select individuals as trainees. In FY 1989, NIH directly and through training grants supported approximately 11,500 individuals in research training, slightly less than half at the post-doctoral level. Post-doctoral awards were divided between M.D.s, 2,582 (48 percent) and Ph.D.s 2,787 (52 percent). Over the decade (1980 to 1989) the number of M.D.s supported increased from 2,100 to nearly 2,600 per year while the number of Ph.D.s declined from 3,600 annually to 2,800.
Table B-12 provides information on training grant and fellowship applications from five clinical departments. The departments differed markedly in the degrees of their trainees and fellows. While between 1980 and 1989 three quarters of the applications from surgery and two thirds of those from medicine and pediatrics were submitted by M.D.s, in radiology only 35 percent and in OB/GYN only 28 percent were from M.D.s. There was little difference among the five departments in success rates for training (T and F) grants between 1980 and 1989, but because of the small numbers of applications and grants it is hard to draw conclusions.
TABLE B-12: Success Rates of Traineeships, Fellowships and Career Development Award Applications, Selected Clinical Departments, 1980–1989
|
Trainees/Fellowships (T/F) |
Career Development (K) |
|||||
|
Department |
No. Applications |
No. of Awards |
Success Rate |
No. Applications |
No. of Awards |
Success Rate |
|
All Applications |
||||||
|
OB/GYN |
194 |
84 |
43.3% |
69 |
21 |
30.4% |
|
Medicine |
3,613 |
1,777 |
49.2 |
1,738 |
729 |
42.0 |
|
Pediatrics |
671 |
265 |
39.5 |
445 |
177 |
39.8 |
|
Radiology |
192 |
86 |
44.8 |
66 |
20 |
30.3 |
|
Surgery |
564 |
207 |
36.7 |
200 |
66 |
33.0 |
|
Total |
5,234 |
2,419 |
46.2 |
2,518 |
1,013 |
40.2 |
|
M.D.s |
||||||
|
OB/GYN |
56 |
24 |
42.9% |
52 |
18 |
34.6% |
|
Medicine |
2,316 |
1,001 |
43.2 |
1,412 |
620 |
43.9 |
|
Pediatries |
425 |
172 |
40.5 |
343 |
137 |
39.9 |
|
Radiology |
68 |
28 |
41.2 |
43 |
12 |
27.9 |
|
Surgery |
406 |
151 |
32.5 |
151 |
53 |
35.1 |
|
Total |
3,271 |
1,376 |
40.4 |
2,001 |
840 |
42.0 |
In addition to research training, NIH supports the renewal of the biomedical research community through a number of career development programs. Total funding for these programs was $90 million in 1989, nearly double the 1980 level of $47.5 million. However, as a portion of the extramural budget, career development support fell from 1.7 percent in 1980 to 1.5 percent in 1989. In 1980 all career development awards were made to individuals; however, since 1984 a few institutional awards, each of which generally supports several individuals, have been made. Individual awards continue to predominate
absorbing over 90 percent of the funding to career development with roughly 1,200 awards per year. There were three institutional program awards in 1984. These increased to 21 during the last three years of the decade.
While the total number of researchers receiving career development awards has been relatively constant between 1980 and 1989, there has been a change in the mix of researchers. In 1980, 495 M.D.s and 736 Ph.D.s received individual career development awards. By 1989 the number of individual awards to M.D.s had risen to 873 and the number of awards to Ph.D.s had declined to 350. In addition in 1985 there were 9 institutional program grants which made multiple awards to physicians (there was no equivalent program for Ph.D.s). In 1989 12 institutional awards were made to support M.D.s.
Changes in the career development programs have occurred. The program of modified research career development awards (K04s), which supported the majority of Ph.D.s, was reduced. A major expansion of the program for clinical investigators designed to develop skills in clinical research (K08s) took place. Two new programs for physician scientists, K11 and K12 (one individual and one institutional) were created. These physician scientist awards, unlike the clinical investigator awards, are designed to support newly trained clinicians in the ''development of independent research skills and experience in a fundamental science''. For the institutional (program) awards this experience is to be developed "within the frame work of an interdisciplinary research and development program."
Applications from OB/GYN departments for career development awards experienced success rates comparable to the other four departments, but departments of OB/GYN submitted few applications (Table B-12). Between 1980 and 1989, OB/GYN departments moved from the lowest success rate of the five departments to the highest success rate, both overall and for M.D.s. Unlike training grants and fellowships, most career development award applications from all five departments were submitted by M.D.s—ranging from 65 percent in radiology to 81 percent in medicine, with OB/GYN, surgery and pediatrics having approximately three quarters of their applications from M.D.s.
Departments of OB/GYN averaged only two competitive career development awards per year between 1980 and 1989. Awards to M.D.s increased during the 1980s, while support of Ph.D.s decreased. The number of individuals supported in the last three years is larger than the number of awards because the NIH data system counts the K-12 award for the Reproductive Scientist Development Program (which supports three scientists) as a single recipient. The number of Modified Research Career Develop net Awards (K04s) declined during the decade while the number of Clinical Investigator Awards (K08s) and Physician Scientist Awards (K11) in departments of OB/GYN increased. Over
the past six years more than two thirds of the awards have been either K08s or K11 (in approximately equal numbers).
Number of Individuals in Departments of OB/GYN with NIH Training Support
It is difficult to determine the number of people in departments of OB/GYN whose research training has been helped by NIH support. While NIH codes data on the recipients of traineeships and fellowships on its records, and also has data on career development awards, those at NIH most familiar with these data files do not consider them to be reliable. However, by using several different files and source some approximate numbers can be generated: Physicians m OB/GYN departments received 18 competing career development awards between 1980 and 1989 (individuals normally receive support for two to four years). In addition to individual awards there was one institutional K award during the decade, thus roughly 20 OB/GYN M.D.s were supported by NIH career development awards. In addition, nine individual physicians in OB/GYN departments received National Research Service Fellowships directly from NIH and eight OB/GYN departments received training grants from NIH. While it is not possible to determine how many individual M.D.s received support under the institutional awards, it is generally believed that most of the programs were small. This, coupled with the fact that four of the eight institutional grants were made in FY 1988 for awards to begin in FY 1989, make it unlikely that more than 20 to 25 individuals received support under the training program during the decade of the 1980s. Adding together the career development "K" awards (seventeen individuals, one institutional award) and the research training awards (nine individual fellowships and eight training grants under the National Research Service Awards Program) it is likely that approximately fifty OB/GYNs received research training from NIH during the decade of the 1980s.
Beginning Research Awards
To help new biomedical researchers develop from working under a mentor to independence, NIH uses the R-29 grant, the First Independent Research Support and Transition (FIRST). These grants are designed "... to underwrite the first independent investigative efforts of an individual; to provide a reasonable opportunity to demonstrate creativity, productivity, and further promise and to help in the transition to traditional types of NIH research project
grants".27 The grants are for 5 years, are not renewable, are limited to $350,000 in total and $100,000 in a single year.
The R-29 (FIRST grants) replaced similar R-23 grants in the mid 1980s, therefore departmental comparisons below include both types of awards. In 1989, 1,711 R-29 awards were made in the amount of approximately $152 million. This represents an increase from 0.8 percent of the NIH extramural research budget in 1980 ($20 million) to 2.7 percent in 1989.
Like several other grant mechanisms, OB/GYN and radiology made little use of R-23 and R-29 grants between 1980 and 1989. OB/GYN submitted few applications and had low success rates, which declined during the second five years of the decade. OB/GYN had the lowest success rate of the five departments for both the periods, 1980–1984 and 1985–1989 (Table B-13). The number of applications from M.D.s, presents a similar picture to that for traineeships and fellowships, although it is not as extreme. Over half of the R23/R29 grants from departments of pediatrics, medicine and surgery came from M.D.s, while only 31 percent of those from OB/GYN departments and 13 percent of those from radiology were from M.D.s. M.D.s from OB/GYN had success rates significantly lower than any of the comparison departments.
Institutional Grants
In addition to individual awards, NIH supports larger multi-project research efforts. The two most important are program projects (P01s) and research centers, a generic term which includes a number of different types of centers-specialized, core, comprehensive, animal, and general clinical research centers.
Program project grants (PO1s) are broad-based, long term multidisciplinary research activities organized around a basic theme. The individual sub-parts or components '...must have scientific merit and essential elements of unity and interdependence that constitute a system of research activities and projects directed toward the overall goal of the program". These grants involve large numbers of researchers and in addition to supporting the interrelated research projects can also support both basic resources and clinical components used by the overall group. The number of program project grants awarded and funding rose in the past decade. The number of awards increased from 535 to 793 and funding increased from $297.5 million to $683 million. While few in number, compared for example to RO1s, they are the second largest grant in terms of funding.
TABLE B-13: Success Rates of R23 and R29 Applications, Selected Clinical Departments, 1980–1989
|
Department |
Number of Applications |
No. of Awards |
Success Rate |
|
All Applications |
|||
|
OB/GYN |
165 |
29 |
17.6% |
|
Medicine |
1,909 |
652 |
34.2* |
|
Pediatrics |
607 |
189 |
31.1* |
|
Radiology |
181 |
68 |
37.6* |
|
Surgery |
411 |
122 |
29.7* |
|
Total |
3,273 |
1,060 |
32.4 |
|
M.D.s |
|||
|
OB/GYN |
51 |
4 |
7.8% |
|
Medicine |
1,024 |
345 |
33.7* |
|
Pediatrics |
344 |
114 |
33.1* |
|
Radiology |
23 |
7 |
30.4* |
|
Surgery |
213 |
60 |
28.2* |
|
Total |
1,655 |
530 |
32.0 |
|
* Significant at 95 % confidence level when compared with OB/GYN. |
|||
Between 1980 and 1989 OB/GYN departments were relatively successful in the competition for program project grants (P01), with success rates failing approximately in the middle of the five comparison departments (Table B-14). The number of applications from each department is small and none of the differences between OB/GYN and the other four departments is statistically significant. With the exception of an increase in the number of applications from departments of medicine there are no discernable trends over the decade. In fact the most significant fact about OB/GYN performance with regard to P01s is the small number of applications—on average less than 3 per year and a total for the decade of only 28. This is only a quarter of the number submitted by
radiology, the department with the next fewest applications. Since program project grants are only awarded to institutions with developed research programs, the small amber of applications may indicate that few OB/GYN departments believe they have the research programs that would allow them to compete successfully.
Research center grants together are the third largest grant activity in terms of dollars awarded. While there are 10 different types of center grants, the two largest are the specialized (P50) and the core (P30) which between them accounted for approximately 60 percent of the number and 57 percent of the dollars for center grants in 1989. The core grants (P30s) are designed to provide "... shared resources and facilities for categorical research by a number of investigators from different disciplines who provide a multidisciplinary approach to a joint research effort or from the same discipline who focus on a common research problem".28 Specialized centers (P50s), on the other hand, not only provide supportive ancillary activities but also provide support for an overall set of research activities to mount "... a multidisciplinary attack on a specific disease entity or biomedical problem area.29 These latter grants are similar to program project grants except that awards are usually based on specific announcements from an NIH institute or division and are more closely monitored by NIH. The number of new center grants NIH can award is limited by Congress which also earmarks some specific center programs to receive awards. In some years in the 1980s, congressional floors on the number of RO1s reduced the number of center grants made by NIH.
OB/GYN departments were competitive for P30 and P50 grants, having had the highest success rate of any of the five departments between 1980 and 1989. However OB/GYN departments submitted on average only three applications per year (Table B-14). Of the five departments only departments of medicine made major use of center grants, submitting 71 percent of applications during the decade. Like program project grants (P01s) center grants are difficult to obtain. In general such grants go only to institutions with a successful research track record.
TABLE B-14: Success Rates of Program Project and Center Grant Applications, Selected Clinical Departments, 1980–1989
|
Department |
Number of Applications |
No. of Awards |
Success Rate |
|
PO1s |
|||
|
OB/GYN |
28 |
13 |
46.4% |
|
Medicine |
646 |
336 |
52.0 |
|
Pediatrics |
121 |
57 |
47.1 |
|
Radiology |
100 |
47 |
47.0 |
|
Surgery |
140 |
65 |
46.4 |
|
Total |
1,035 |
518 |
50.0 |
|
P30s – P50s |
|||
|
OB/GYN |
33 |
24 |
72.7% |
|
Medicine |
601 |
334 |
55.6 |
|
Pediatrics |
111 |
54 |
48.6 |
|
Radiology |
9 |
5 |
55.5 |
|
Surgery |
90 |
47 |
52.2 |
|
Total |
844 |
464 |
55.0 |
Summary of NIH Support of Departments of OB/GYN
The previous sections presented information on NIH support of OB/GYN department research and research training activities. In this section the main points are summarized.
On the positive side, between 1980 and 1989 the increase in funding of OB/GYN departments exceeded the NIH increase in funding of all clinical departments. The percentage of NIH support to medical schools received by OB/GYN departments remained relatively constant since the late 1960s, at about 1.5 percent of the total. However, by one measure OB/GYN wins less
than its share of funding—with about 4.8 percent of full-time faculty in clinical departments of medical schools OB/GYN receives only about 2.7 percent of the funds awarded by NIH/ADAMHA to clinical departments.
While there is no evidence that the ability of OB/GYN departments to compete for NIH support seriously deteriorated between 1980 and 1989, there is a reason to be concerned about several aspects including the low level of NIH funding compared to some other departments, and the competitive state of physician investigators in OB/GYN department.
NICHD has been, and continues to be, the major supporter of OB/GYN departments, providing nearly 70 percent of NIH funds to the departments in 1989. NCI is the second largest supporter, however, its contribution declined from approximately 30 percent in 1978 to less than 10 percent in 1989. No other institute provides as much as 5 percent of the total funding for OB/GYN departments.
The total number of NIH awards to departments of OB/GYN varied from year to year between 1980 and 1989, but was slightly higher in 1989 than in 1980. The increase was in research grants (primarily RO1s), and a slight decline occurred in the number of traineeships, fellowships and research contracts awarded. The number of OB/GYN departments receiving NIH awards in any one year ranged from a high of 72 (in 1984) to a low of 67 (in 1989).
It is important to remember that while the mix of M.D.s to Ph.D.s was similar in the five departments we analyzed, the mix of grant applications was not. M.D.s in the departments of internal medicine, pediatrics and surgery submitted between 58 percent and 65 percent of the departments' grant applications, and the proportion increased through the 1980s. M.D.s in departments of radiology submitted 28 percent, and those in departments of OB/GYN submitted 38 percent. M.D.s from departments OB/GYN and radiology had the fewest applications of the five departments, and for the decade OB/GYN departments had the lowest success rate. Ph.D.s from OB/GYN departments fared better, with a success rate that put them in the middle of the five departments analyzed.
The picture with regard to RO1s is similar. Between 1980 and 1989, applications from OB/GYN departments had the lowest success rates (the differences in success rates between departments of OB/GYN and internal medicine and radiology were statistically significant). The success rate of RO1 applications submitted by M.D.s from OB/GYN departments were significantly lower than submissions by M.D.s in the four other departments. Ph.D.s in OB/GYN departments had a success rate below that of internal medicine and radiology and above that of pediatrics and surgery. The differences between Ph.D.s from departments of OB/GYN and Ph.D.s from departments of internal
medicine and radiology were statistically significant. The competitive position of the Ph.Ds from OB/GYN declined during the later years of the decade.
OB/GYN departments were more successful in obtaining training grants and fellowships. While none of the differences are statistically significant, OB/GYN was the most successful of the five departments with regard to awards for training grants to M.D.s during the period 1980–1984. The success rate declined during the second 5 years of the decade both absolutely and relative to the other departments. A smaller percentage of the trainees in OB/GYN and radiology are M.D.s, compared with internal medicine, surgery, or pediatrics.
The success rate of OB/GYN departments in winning career development awards improved during the second half of the decade rising from the lowest to the highest success rate among the five departments analyzed. This pattern holds both for all career development awards and for those going to M.D.s. However OB/GYN department M.D.s only submitted a total of 52 applications for career development awards in the 1980s.
Both M.D.s and Ph.D.s from OB/GYN departments have been relatively unsuccessful in obtaining R-29 (FIRST) awards. Moreover, M.D.s submitted few applications (51 from departments of OB/GYN compared with 1,024 from departments of internal medicine).
By contrast OB/GYN departments have been relatively successful in obtaining both program-project grants and center grants but submitted few such applications—on average three program-projects and three center grant applications a year between 1980 and 1989. This dearth of applications may reflect both the amount of effort required to develop these applications and the fact that NIH staff will, on occasion, discourage applications from clearly noncompetitive institutions.
NIH Administration and Structure
Two kinds of problems effect NIH support of research in departments of OB/GYN. One pertains to research grants submitted by M.D.s, particularly RO1s and R29s, which have a relatively low success rate. The second relates to program-project grants, center grants, career development grants, and to some degree fellowships, for which the problem is not success in obtaining funding but rather the fact that M.D.s from OB/GYN departments submit very few applications.
This review is not able to determine the reasons for the low success rates and, in some programs, low application rates. The causes could be quality of
the research being proposed, the substance of the research (reproductive research and research into issues concerning women's health) or the nature of the review and the composition of the review committees. Most RO1s are reviewed in the individual study sections of the Division of Research Grants. A few RO1s, usually in response to specific announcements, may be reviewed by groups set up by the supporting institute. Of more than 50 members of the four initial review groups which together review approximately 50 percent of the applications submitted by OB/GYN departments only three list OB/GYN as a primary area of expertise and only four others listed another clinical area.
This review of data pertaining to applications for funding from departments of OB/GYN does not shed light on the concern that there are characteristics of NIH that create barriers to adequate funding of OB/GYN research and women's health issues in general. These characteristics include:
-
A paucity of women at high levels in NIH.
-
The lack of a women's (or OB/GYN focused) institute.
-
Lack of an OB/GYN intramural program.
-
The pediatric orientation of NICHD's leadership.
Moreover, the budgets of the two institutes that are the major funders of OB/GYN research have not grown as fast as the total NIH budget. For 8 of the 10 years between 1980–1989, NICHD had award rates for research grants below the NIH average. In 1989, 12 of the 14 institutes and other awarding units had award rates higher than NICHD. While the impact of these factors on the funding of OB/GYN is impossible to quantify, conversations with NIH staff and others indicate that some could be important.
The question of why there is no OB/GYN intramural program at NIH has been asked for some years—the answers most often heard are that obstetric patient accrual would be difficult, the range of ancillary services needed would be hard to support and OB/GYNs will not work for low federal pay. While its not clear if, or how, the lack of intramural OB/GYN affects extramural OB/GYN research, some people claim that it leads to a lack of internal advocates for OB/GYN and that NIH staff dealing with OB/GYN grants feel isolated. Moreover, since the OB/GYN research community is the NIH "client" contact between NIH staff and the investigators cannot achieve the informal collegial relationship needed to generate creative thinking and ongoing excitement about the discipline. However, as a result of Congressional pressure, NICHD is planning to establish an intramural gynecological research section on campus. They are recruiting for an individual certified in gynecology to head the research program, direct its clinical consultative service and its
endocrinology fellowship program. NCI has also indicated a willingness to meet with leaders in academic gynecology to discuss the possibility of establishing a gynecology branch as well as increasing support for research in gynecological oncology.
Whether it would be helpful for OB/GYN or women's health to have an institute devoted to the discipline is debatable. It is argued that relying on an institute whose primary mission is children and development relegates OB/GYN to a secondary position. This is reinforce by the tradition of having a pediatrician direct the institute. Moreover, there is a lack of visibility and organizational identification that might attract the attention of Congress to issues in OB/GYN, and allow an NIH intramural constituency to systematically develop programs. On the other hand, it is argued that a women's or OB/GYN institute would relieve the existing funders (NICHD, NCI, NIA, etc.) of the obligation to pursue OB/GYN questions, and would create a "ghetto" for OB/GYN and women's issues. In the light of ongoing developments concerning issues in women's health, such as the establishment of the Office of Research on Women's Health, and with NIH in the process of generating a research agenda for women's health, there may exist now an impetus at NIH that will allow OB/GYN and other women's health research to flourish.
Actions and Further Analysis Needed to Improve NIH Support of OB/GYN Research
-
Study is needed to examine charges that clinical research does not receive a fair scientific review at NIH.
-
The charters of the study sections that review the majority of OB/GYN applications, their composition and the applications reviewed should be analyzed to determine whether there are problems with the composition of membership.
-
OB/GYN academic leaders should review the career development award (Ks) and the FIRST grants (R29) to determine if there axe features of the programs that are discouraging OB/GYN participation. If such features axe found, they should meet with appropriate NIH leaders to encourage necessary changes. NIH institutes have a great range of options in how programs are structured and which mechanisms are used.
-
It is appropriate that representatives of gynecological oncology continue to meet with NCI leadership given the institutes's decreasing support for OB/GYN research over the past decade. Given the range of women's health issues that axe the responsibility of NIA and its relatively low level of support
-
for OB/GYN research, it might also be appropriate for OB/GYN leaders to meet with representatives of that institute.
The creation of the Office of Research on Women's Health is a positive step, and the office can play an important role as a coordinator, advocate and honest broker. It will also play a role in creating a research agenda and in monitoring the responsiveness of NIH to women's health needs. However, the major strength of NIH is in its individual institutes and increased support for OB/GYN can only come from increased awareness and support from the individual institutes.
References
1. National Institutes of Health. NIH Data Book, 1990. NIH Publication No. 90–1261. September. Bethesda, Maryland.
2. Association of American Medical Colleges. 1988–1989. U.S. Medical School Finance Section for Operation Studies, July 1990. Washington, D.C.: Association of American Medical Colleges.
3. National Institutes of Health. NIH. Data Book 1990.
4. Sherman, Barry, and Myron Genel. 1983. Human Investigation in the 1980s: Themes from the Scottsdale Conference, Clinical Research 31:570–571.
5. Avis, Frederick P., Ellenberg, S. and Friedman, M. 1988. Surgical Oncology Research. Annals of Surgery. 207(3) 262–268.
6. Sherman, Barry. 1988. Position Paper Prepared for Institute of Medicine Committee. Resources for Clinical Investigation.
7. Personal Interview, 1990.
8. Health Policy and Biomedical Research News of the Week. 1990. ''Blue Sheet'', Vol. 33, No.50. December 17.
9. Cuca, J. A. 1990. Scientific, Social and Other Factors in the Evaluation of Applications for NIH Research Grants. Ph.D. Dissertation. The Catholic University of America, Washington, D.C.
10. National Institutes of Health. 1986. Peer Review Trends 1976–1985. Division of Research Grants. Bethesda, Maryland.
11. National Institutes of Health. 1990. Extramural Trends. FY 1980–1989. Division of Research Grants. Bethesda, Maryland.
12. Arias, I.M. 1989. Training Basic Scientists to Bridge the Gap Between Basic Science and Its Application to Human Disease. New England Journal of Medicine, 321:972–974.
13. Healy, B. H. 1988. Innovators for the 21st Century: Will we Face a Crisis in Biomedical Research Brainpower. NEJM. 319:1058–1064.
14. Healy, B. H. 1989. The Human Factor at the Endless Frontier. Circulation. 79:959–965.
15. Kelley, W. N. 1985. Personnel Needs for Clinical Research: Role of the Clinical Investigator. Clinical Research 33:100–104.
16. Kelley, W. N. 1988. Are We About to Enter the Golden Era of Clinical Investigation? Journal of Laboratory and Clinical Medicine 111(4):365–370.
17. Wyngaarden, J. 1981. The Clinical Investigator as an Endangered Species. Bull New York Academic Medicine. 57(6):415–426.
18. Smith, Lloyd H. Jr. 1989. Training of Physician Scientists. Background Paper for National Research Council, Committee on Biomedical and Behavioral Personnel. Washington, D.C. National Academy Press.
19. Institute of Medicine. 1989. Research Capabilities of Academic Departments of Obstetrics and Gynecology: Report of a planning Committee. Washington, D.C.
20. National Institutes of Health. 1988. Peer Review Trends. 1976–1985. Division of Research Grants. Bethesda, Maryland.
21. Avis, Fredrick P., Ellenberg, S. and Friedman, M. 1988. Surgical Oncology Research. Annals of Surgery. 207(3)262–268.
22. Association of American Medical Colleges. 1989. Distribution of Full Time Faculty at U.S. Medical Schools who are Principal Investigators by Department. A series of tables prepared for the National Institutes of Health. Washington, D.C.
23. Pearse, Warren H., et al. 1986. Obstetric and Gynecological Manpower. Obstetrics and Gynecology. Vol. 70, No.3. Part 1. September, 1987.
24. Pearse, Warren H., et.al. Trends in Obstetric and Gynecological Academic Manpower and Research 1977–1990. (In press 1991)
25. Gentile, Nancy O., et.al. 1987. Research Activity of Full Tune Faculty in Departments of Medicine. Washington, D.C. Association of Professors of Medicine and Association of American Medical Colleges.
26. Kretchmer, Norman. 1980. The Support of Academic Obstetrics: The Public Sector in the Current Status and Future of Academic Obstetrics. Edited by John Bowers and Elizabeth Purcell. 1980. New York, NY: Josiah Macy, Jr. Foundation.
27. Association of American Medical Colleges. U.S. Medical School Finance 1988–1989. Section for Operational Studies, July 1990. Washington, D.C.: Association of American Medical Colleges.
28. National Institutes of Health. 1989. Orientation Handbook for Members of Scientific Review Group. Division of Research Grants. Bethesda, Maryland.
29. National Institutes of Health. 1989. Activity Codes, Organizational Codes, and Definitions Used in Extramural Programs. Division of Research Grants. Bethesda, Maryland.






































